- Codeine
-
Codeine 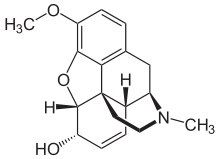
Systematic (IUPAC) name (5α,6α)-7,8-didehydro-4,5-epoxy-3-methoxy-17-methylmorphinan-6-ol Clinical data AHFS/Drugs.com monograph MedlinePlus a682065 Pregnancy cat. ? Legal status Controlled (S8) (AU) Schedule I (CA) ? (UK) Schedule II (US) Dependence liability Low - Moderate Routes oral, intra-rectally, SC, IM Pharmacokinetic data Bioavailability ~90% Oral Metabolism Hepatic, via CYP2D6 (Cytochrome P450 2D6)[1] Half-life 2.5–3 h Identifiers CAS number 76-57-3 
ATC code R05DA04 N02AA59 PubChem CID 5284371 IUPHAR ligand 1673 DrugBank APRD00120 ChemSpider 4447447 
UNII Q830PW7520 
KEGG C06174 
ChEBI CHEBI:16714 
ChEMBL CHEMBL485 
Chemical data Formula C18H21NO3 Mol. mass 299.364 g/mol SMILES eMolecules & PubChem  (what is this?) (verify)
(what is this?) (verify)Codeine or 3-methylmorphine (a natural isomer of methylated morphine, the other being the semi-synthetic 6-methylmorphine) is an opiate used for its analgesic, antitussive, and antidiarrheal properties. Codeine is the second-most predominant alkaloid in opium, at up to three percent; it is much more prevalent in the Iranian poppy (Papaver bractreatum), and codeine is extracted from this species in some places although the below-mentioned morphine methylation process is still much more common. It is considered the prototype of the weak to midrange opioids (tramadol, dextropropoxyphene, dihydrocodeine, hydrocodone, oxycodone).
Contents
Medical uses
Codeine is used to treat mild to moderate pain and to relieve cough.[2] Codeine is also occasionally used to treat diarrhea, although loperamide (which is available OTC for milder diarrhea), diphenoxylate, paregoric or even laudanum (also known as Tincture of Opium) are more frequently used to treat severe diarrhea.[3]
Formulations
Codeine is marketed as both a single-ingredient drug and in combination preparations with the analgesic acetaminophen (paracetamol), as co-codamol, paracod, panadeine, Paramol or the Tylenol With Codeine series (e.g., Tylenol 3 and 4 tablets and elixir); with the analgesic acetylsalicylic acid (aspirin), as co-codaprin; or with the NSAID (non-steroidal anti-inflammatory drug) ibuprofen, as Nurofen Plus. These combinations provide greater pain relief than either agent alone (drug synergy). Codeine is also commonly marketed in products containing codeine with other pain killers or muscle relaxers, as well as codeine mixed with phenacetin (Emprazil With Codeine No. 1, 2, 3, and 4), naproxen, indomethacin, diclofenac and others as well as more complex mixtures including such mixtures as aspirin + paracetamol + codeine ± caffeine ± antihistamines and other agents such as those mentioned above.
Codeine-only products can be obtained with a prescription as a time release tablet (e.g., Codeine Contin 100 mg and Perduretas 50 mg). Codeine is also marketed in cough syrups with zero to a half-dozen other active ingredients, and a linctus (e.g., Paveral) for all of the uses for which codeine is indicated.
Injectable codeine is available for subcutaneous or intramuscular injection; intravenous injection can cause a serious reaction that can progress to anaphylaxis. Codeine suppositories are also marketed in some countries.
Adverse effects
Common effects other than analgesia associated with the use of codeine include euphoria, itching, nausea, vomiting, drowsiness, dry mouth, miosis, orthostatic hypotension, urinary retention, depression, constipation and coughing (which is a paradoxical symptom).[4] Some people may also have an allergic reaction to codeine, such as the swelling of skin and rashes.[5] Erectile dysfunction and diminished libido can be a longer-term effect (years to decades) of many narcotic analgesics due to development of central hypogonadism; this appears to be especially common in individuals with significant melanin deficiencies, as the hormones tied to melanin production affect the absorption and conversion of these analgesics into progesterone. [6] Additionally, the haplotypes of about 48% of the indigenous population of Great Britain aggravate the condition, as the E647 sequence underwent epigenetic degradation and became a pseudogene. The chance of vulnerability is doubled for males, as the critical sequence is located on the X chromosome.[7]
Codeine and morphine as well as opium were used for control of diabetes until relatively recently, and still are in rare cases in some countries, and the hypoglycaemic effect of codeine, although usually weaker than that of morphine, diamorphine, or hydromorphone, can lead to cravings for sugar.
Tolerance to many of the effects of codeine develops with prolonged use, including therapeutic effects. The rate at which this occurs develops at different rates for different effects, with tolerance to the constipation-inducing effects developing particularly slowly for instance.
A potentially serious adverse drug reaction, as with other opioids, is respiratory depression. This depression is dose-related and is the mechanism for the potentially fatal consequences of overdose. As codeine is metabolized to morphine, morphine can be passed through breast milk in potentially lethal amounts, fatally depressing the respiration of a breastfed baby.[8][9]
Withdrawal and dependence
As with other opiate-based pain killers, chronic use of codeine can cause physical dependence. When physical dependence has developed, withdrawal symptoms may occur if a person suddenly stops the medication. Withdrawal symptoms include: drug craving, runny nose, yawning, sweating, insomnia, weakness, stomach cramps, nausea, vomiting, diarrhea, muscle spasms, chills, irritability, and pain. To minimize withdrawal symptoms, long-term users should gradually reduce their codeine medication under the supervision of a healthcare professional.[10] A support group called Codeine Free exists to help people who have found themselves dependent on codeine.
Pharmacology
Codeine was once considered to be a morphine prodrug, since it was thought that its analgesia was due in large part to its O-demethylation to the much more powerful opiate, morphine. However, more recent research shows that 80% of codeine is conjugated with glucuronic acid to codeine-6-glucuronide (C6G), which is the metabolite that is most responsible for codeine's analgesia. Only 5% of the dose is O-demethylated to morphine, which in turn is immediately glucuronidated at the 3- and 6-position and excreted renally.[11][12] A portion (~ 15%) of the codeine is N-demethylized to norcodeine.[13] So analgesia of codeine does not depend on the formation of morphine, as previously thought.[11] It is less potent than morphine and has a correspondingly lower dependence-liability than morphine.[14] Like all opioids, continued use of codeine induces physical dependence and can be psychologically addictive. However, due to its low potency, the withdrawal symptoms are relatively mild compared to closely related opioids such as hydrocodone and oxycodone. As such, codeine has a lower physical dependence liability than most other opioids.[15]
A dose of approximately 200 mg (oral) of codeine must be administered to give analgesia approximately equivalent to 30 mg (oral) of morphine (Rossi, 2004). However, codeine in general isn't used in single doses greater than 60 mg (and no more than 240 mg in 24 hours).[16][17] When analgesia beyond 60 mg of codeine is required, stronger opioids such as hydrocodone or oxycodone are utilized.[18] When used to relieve dry coughs, codeine is used in doses ranging from 5-15 mg and is usually mixed as a syrup with other drugs such as promethazine[19] which is an antihistamine with strong sedative activity (some formulations come with different types of antihistamines),[20] guaifenesin which is an expectorant,[21] and other drugs. When codeine isn't effective in relieving stronger dry coughs, then the opioid hydrocodone is used instead.
Codeine is metabolized to C6G by uridine diphosphate glucuronosyl transferase UGT2B7, and, since only about 5% of codeine is metabolized by cytochrome P450 CYP2D6, the current evidence is that codeine-6-glucuronide (C6G) is the primary active compound.[22] Claims about the supposed "ceiling effect" of codeine doses seemed to rest on the assumption that high doses of codeine saturated CYP2D6, which prevented further conversion of codeine to morphine, which is simply incorrect since we now know that codeine-6-glucuronide (C6G) is the main metabolite responsible for codeine's analgesia.[11] There is also no evidence that CYP2D6 inhibition is useful in treating codeine dependence,[23] though the metabolism of codeine to morphine (and hence further metabolism to glucuronide morphine conjugates) does have an effect on the abuse potential of codeine.[24] However, CYP2D6 has been implicated in the toxicity and death of neonates when codeine is administered to lactating mothers, particularly those with increased 2D6 activity ("ultra-rapid" metabolisers).[25][26]
Pharmacokinetics
The conversion of codeine to morphine occurs in the liver and is catalysed by the cytochrome P450 enzyme CYP2D6. CYP3A4 produces norcodeine and UGT2B7 conjugates codeine, norcodeine, and morphine to the corresponding 3- and 6- glucuronides. Approximately 6–10% of the Caucasian population, 2% of Asians, and 1% of Arabs[27] are "poor metabolizers"; they have little CYP2D6, and codeine is less effective for analgesia in these patients (Rossi, 2004). Srinivasan, Wielbo and Tebbett speculate that codeine-6-glucuronide is responsible for a large percentage of the analgesia of codeine, and, thus, these patients should experience some analgesia.[12] Many of the adverse effects will still be experienced in poor metabolizers. Conversely, 0.5-2% of the population are "extensive metabolizers"; multiple copies of the gene for 2D6 produce high levels of CYP2D6 and will metabolize drugs through that pathway more quickly than others.
Some medications are CYP2D6 inhibitors and reduce or even completely block the conversion of codeine to morphine. The most well-known of these are two of the selective serotonin reuptake inhibitors, paroxetine (Paxil) and fluoxetine (Prozac) as well as the antihistamine diphenhydramine and the antidepressant, buproprion (Wellbutrin, also known as Zyban). Other drugs, such as rifampicin and dexamethasone, induce CYP450 isozymes and thus increase the conversion rate.
Since codeine is a prodrug, metabolism differences have the opposite effect. Thus an extensive metabolizer may have adverse effects from a rapid buildup of codeine metabolites while a poor metabolizer may get little or no pain relief. CYP2D6 is dysfunctional in 7% of white and black Americans, resulting in reduced metabolism of codeine. Other individuals may have two or more copies of the CYP2D6 gene, resulting in rapid metabolism of the target drug. CYP2D6 metabolizes and activates codeine into morphine, which then undergoes glucuronidation. Life-threatening intoxication, including respiratory depression requiring intubation, can develop over a matter of days in patients who have multiple functional alleles of CYP2D6, resulting in ultra-rapid metabolism of opioids such as codeine into morphine.[28][29][30]
The active metabolites of codeine, notably morphine, exert their effects by binding to and activating the μ-opioid receptor.
Relation to other opiates
Codeine is the starting material and prototype of a large class of mainly mild to moderately strong opioids such as hydrocodone (1920 in Germany), oxycodone (1916 in Germany), dihydrocodeine (1908 in Germany), and its derivatives such as nicocodeine (1956 in Austria). Other series of codeine derivatives include isocodeine and its derivatives, which were developed in Germany starting around 1920. As an analgesic, codeine compares moderately to other opiates. Related to codeine in other ways are codoxime, thebacon, Codeine-N-Oxide (Genocodeine), related to the nitrogen morphine derivatives as is codeine methobromide, and heterocodeine, which is a drug six times stronger than morphine and 72 times stronger than codeine due to a small re-arrangement of the molecule, viz. moving the methyl group from the 3 to the 6 position on the morphine carbon skeleton. Drugs bearing resemblance to codeine in effects due to close structural relationship are variations on the methyl groups at the 3 position including ethylmorphine a.k.a. codethyline (Dionine) and benzylmorphine (Peronine). While having no narcotic effects of its own, the important opioid precursor thebaine differs from codeine only slightly in structure. Pseudocodeine and some other similar alkaloids not currently used in medicine are found in trace amounts in opium as well.
History
Codeine, or 3-methylmorphine, is an alkaloid found in the opium poppy, Papaver somniferum var. album, a plant in the papaveraceae family. Opium poppy has been cultivated and utilized throughout human history for a variety of medicinal (analgesic, anti-tussive and anti-diarrheal) and hypnotic properties linked to the diversity of its active components, which include morphine, codeine and papaverine.
Codeine is found in concentrations of 0.9 to 3.0 per cent in opium prepared by the latex method from unripe pods of Papaver somniferum. The name codeine is derived from the Greek word kodeia (κώδεια) for "poppy head". The relative proportion of codeine to morphine, the most common opium alkaloid at 4 to 23 per cent, tends to be somewhat higher in the poppy straw method of preparing opium alkaloids.
Until the beginning of the 19th century, raw opium was used in diverse preparations known as laudanum (see Thomas de Quincey's "Confessions of an English Opium-Eater", 1821) and paregoric elixirs, a number of which were popular in England since the beginning of the 18th century; the original preparation seems to have been elaborated in Leiden, the Netherlands around 1715 by a chemist named Lemort; in 1721 the London Pharmocopeia mentions an Elixir Asthmaticum, replaced by the term Elixir Paregoricum ("pain soother") in 1746.
The progressive isolation of opium's several active components opened the path to improved selectivity and safety of the opiates-based pharmacopeia.
Morphine had already been isolated in Germany by German pharmacist Friedrich Sertürner in 1804.[31] Codeine was first isolated decades later in 1832 in France by Pierre Robiquet, a French chemist and pharmacist already famous for the discovery of alizarin, the most widespread red dye, while working on refined morphine extraction processes. This paved the way for the elaboration of a new generation of safer, codeine-based specific antitussive and antidiarrheal formulations.
Codeine is currently the most widely-used opiate in the world,[17][32] and is one of the most commonly used drugs overall according to numerous reports by organizations including the World Health Organization and its League of Nations predecessor agency. It is one of the most effective orally administered opioid analgesics and has a wide safety margin. Its strength ranges from 8 to 12 percent of morphine in most people; differences in metabolism can change this figure as can other medications, depending on its route of administration.
While codeine can be directly extracted from opium, its original source, most codeine is synthesized from the much more abundant morphine through the process of O-methylation.[32][33]
By 1972, the effects of the Nixon War On Drugs had caused across-the-board shortages of illicit and licit opiates because of a scarcity of natural opium, poppy straw, and other sources of opium alkaloids, and the geopolitical situation was growing difficult for the United States. After a large percentage of the opium and morphine in the US National Stockpile of Strategic & Critical Materials was tapped in order to ease severe shortages of medicinal opiates — the codeine-based antitussives in particular — in late 1973, researchers were tasked with finding a way to synthesize codeine and its derivatives. They quickly succeeded using petroleum or coal tar and a process developed at the United States' National Institutes of Health.
Numerous codeine salts have been prepared since the drug was discovered. The most commonly used are the hydrochloride (freebase conversion ratio 0.805), phosphate (0.736), sulphate (0.859), and citrate (0.842). Others include a salicylate NSAID, codeine salicylate (0.686), and at least four codeine-based barbiturates, the cyclohexenylethylbarbiturate (0.559), cyclopentenylallylbarbiturate (0.561), diallylbarbiturate (0.561), and diethylbarbiturate (0.619).
Recreational use
Codeine can be used as a recreational drug.
In some countries, cough syrups and tablets containing codeine are available without prescription; some potential recreational users are reported to buy codeine from multiple pharmacies so as not to arouse suspicion. A heroin addict may use codeine to ward off the effects of a withdrawal.[34]
Codeine is also available in conjunction with the anti-nausea medication promethazine in the form of a syrup. Brand named as Phenergan with Codeine or in generic form as promethazine with codeine. Called 'syrup', this medication is quickly becoming one of the most commonly misused codeine preparations.[35]
Codeine is also demethylated by reaction with pyridine to illicitly synthesize morphine, which can then be acetylated to make heroin (diacetylmorphine). Pyridine is toxic and possibly carcinogenic, so morphine illicitly produced in this manner (and potentially contaminated with pyridine) may be particularly harmful.[36] Codeine can also be turned into α-chlorocodide, which is used in the clandestine synthesis of desomorphine (Permonid).
Detection
Codeine and/or its major metabolites may be quantitated in blood, plasma or urine to monitor therapy, confirm a diagnosis of poisoning or assist in a medicolegal death investigation. Drug abuse screening programs generally test urine, hair, sweat or oral fluid. Many commercial opiate screening tests directed at morphine cross-react appreciably with codeine and its metabolites, but chromatographic techniques can easily distinguish codeine from other opiates and opioids. It is important to note that codeine usage results in significant amounts of morphine as an excretion product. Furthermore, heroin contains codeine (or acetylcodeine) as an impurity and its use will result in excretion of small amounts of codeine. Poppy seed foods represent yet another source of low levels of codeine in one's biofluids. Blood or plasma codeine concentrations are typically in the 50–300 µg/L range in persons taking the drug therapeutically, 700–7000 µg/L in chronic users and 1000–10,000 µg/L in cases of acute fatal overdosage.[37][38][39]
Legal status
In Australia, Canada, New Zealand, Romania, Sweden, the United Kingdom, the United States, and many other countries, codeine is regulated under various narcotic control laws. In some countries it is available without prescription in combination preparations from licensed pharmacists in doses up to 15 mg/tablet in Australia, New Zealand, Poland, Romania (Codamin), and Costa Rica, 12.8 mg/tablet in the UK, 10 mg/tablet in Russia and Israel and 8 mg/tablet in Canada and Estonia.[citation needed]
Australia
In Australia, codeine preparations must be sold only at a pharmacy. The item is given over the counter, no prescriptions. The strongest available over the counter preparation containing codeine has 15 mg (with paracetamol, brand name Panadeine Extra); anything stronger requires a prescription.[40]
Denmark
In Denmark, codeine preparations must be sold only at a pharmacy. The item is given over the counter, no prescriptions. The strongest available over the counter preparation containing codeine has 9.6 mg (with aspirin, brand name Kodimagnyl); anything stronger requires a prescription.
France
In France, most preparations containing codeine do not require a doctor's prescription. Example products containing codeine include Néocodeion (cough pills), Codoliprane (codeine with paracetamol), Prontalgine and Migralgine (codeine, paracetamol and caffeine).[41]
Germany, Switzerland and Austria
Codeine is listed under the Betäubungsmittelgesetz in Germany and the similarly named narcotics and controlled substances law in Switzerland. In Austria, the drug is listed under the Suchtmittelgesetz in categories corresponding to their classification under the Single Convention on Narcotic Drugs. Dispensing of products containing codeine and similar drugs (dihydrocodeine, nicocodeine, benzylmorphine, ethylmorphine etc.), in general, require a prescription order from a doctor or the discretion of the pharmacist. Municipal and provincial regulations may impact availability, in particular in Austria and Switzerland, which allows cities and provinces to regulate the selling of the least-regulated schedule of the SMG/BtMG; and, of course, individual chemists' shops can opt out of providing them or imposing volume, frequency, or single-purchase limitations and other things of the same store. Plain codeine hydrochloride tablets (which in the USA would share CSA Schedule II with drugs like morphine, cocaine, hydromorphone, and bezitramide) as well as other non-injectable forms of codeine and its midrange derivatives can be dispensed in this way; the same goes for most chemical classes of benzodiazepines, the majority of non-barbiturate sedative/hypnotics, and at least a handful of barbiturates.
Title 76 of the Schengen treaty has made it possible for countries within the signatory states to import and export drugs with various provisos, recording and ordering requirements, and various other rules.
Greece
Codeine is classed as an illegal drug in Greece, and individuals possessing it could conceivably be arrested, even if they were legitimately prescribed it in another country.[42]
Hong Kong
In Hong Kong, codeine is regulated under Schedule 1 of Hong Kong's Chapter 134 Dangerous Drugs Ordinance. It can be used legally only by health professionals and for university research purposes. The substance can be given by pharmacists under a prescription. Anyone who supplies the substance without prescription can be fined $10,000 (HKD). The maximum penalty for trafficking or manufacturing the substance is a $5,000,000 (HKD) fine and life imprisonment. Possession of the substance for consumption without license from the Department of Health is illegal with a $1,000,000 (HKD) fine and/or 7 years of jail time.
However, codeine is available without prescription from licensed pharmacists in doses up to 0.1% (5 mg/5ml) according to Hong Kong "Dangerous Drugs Ordinance".
Iceland
Preparations of paracetamol and codeine require a prescription in Iceland. These tablets are known as Parkódín.
Ireland
In the Republic of Ireland, new regulations came into effect on August 1, 2010[43] concerning codeine, due to worries about the overuse of the drug. Codeine remains a non-prescriptive, over-the-counter drug, but codeine products must be out of the view of the public to facilitate the legislative requirement that these products “are not accessible to the public for self-selection”.[44] In practice, this means customers must ask pharmacists for the product containing codeine in name, and the pharmacist makes a judgement whether it is suitable for the patient to be using codeine, and that patients are fully advised of the correct use of these products.[45]
Italy
Codeine tablets or preparations require a prescription in Italy. A preparation of paracetamol and codeine is available in Italy as CoEfferalgan.
Japan
Codeine and similar mid-level centrally acting agents in combination with non-opioid analgesics, antihistamines, vitamins, inert GI agents like kaolin & pectin, mild laxatives, antacids, and herbal preparations, can be purchased over the counter, with 10 mg being the ceiling for OTC dispensing. This is also true of ethylmorphine and dihydrocodeine, and also diphenoxylate, some weak relatives of the thiambutene opioid family.
North America
Narcotic content numbers
Narcotic content number in the US names of codeine tablets and combination products like Tylenol With Codeine No. 3, Emprin With Codeine No. 4, and pure codeine tablets are as follows: No. 1 - 7½ or 8 mg (1/8 grain), No. 2 - 15 or 16 mg (1/4 grain), No. 3 - 30 or 32 mg (1/2 grain), No. 4 - 60 or 64 mg (1 grain). The Canadian "Frosst 222"[46] series is identical to the above list: "222" contains 8 mg codeine, "282" 15 mg, "292" 30 mg, and "293" 60 mg. This system, which is also used at present in the trade names of some dihydrocodeine and ethylmorphine products both in and outside of North America, was inaugurated with the Pure Food and Drug Act of 1906 and related legislation and refined since.
Equivalent scales for labeling stronger opioids such as diacetylmorphine (heroin), morphine, opium salts mixtures, and others were in common use in the past, and on occasion one can find past references to brand names for hydrocodone (invented 1920, introduced in US 1943), hydromorphone (invented 1924), oxycodone (invented 1916), paregoric and similar drugs containing narcotic content numbers. For example. from circa 1900 to 1925, the most common cough medicine was terpin hydrate With Heroin Elixir No. 2.
Contrary to the advertising matter of some pharmacies, 60 mg is No. 4, not No. 6, and tablets with 45 mg of codeine are not No. 4 and would in all likelihood be classified as No. 3½ under that system. Whether the scale goes to No. 5 and higher is moot at this point, as in the United States and Canada single-dose-unit concentrations of more than 64 mg are not manufactured. The United States Controlled Substances Act of 1970 does place dosage unit strengths of 90 mg of codeine and higher in Schedule II, even if mixed with another active ingredient. Oral tablets, hypodermic tablets, liquid forms, and capsules of less common doses are available in some cases the equivalent dihydrocodeine, dionine, benzylmorphine, and opium dosages were previously available in North America (and in most cases still are in other countries, particularly the 45 mg paracetamol/codeine and 50 and 100 mg single-ingredient codeine tablets).
Canada
In Canada, codeine preparations must be sold only at a pharmacy and be either behind the dispensing counter (or elsewhere, like in a back room) or on shelves in an area of the store that can be seen from the dispensing counter. Further, codeine can be sold over the counter only in combination with two or more ingredients, which has resulted in the prevalence of co-codaprin (or "AC&C"), which contains acetylsalicylic acid (ASA), codeine, and caffeine, and similar combinations using acetaminophen (paracetamol) rather than acetylsalicylic acid (aspirin). Caffeine, being a stimulant, tends to offset the sedative effects of codeine. It also can increase the effectiveness and absorption rate of analgesics in some circumstances.[47] Co-codaprin containing 8 mg codeine is often requested and sold as "Frosst 222" at pharmacies, where it is generally available over the counter. Formulations containing more than 8 mg of codeine are available by prescription only.
United States
In the United States, codeine is regulated by the Controlled Substances Act. It is a Schedule II controlled substance for pain-relief products containing codeine alone or more than 90 mg per dosage unit. Tablets of codeine in combination with aspirin or acetaminophen (paracetamol/Tylenol) made for pain relief are listed as Schedule III; and cough syrups are Schedule III or V, depending on formula. The acetaminophen/codeine pain-relief elixir (trade name Tylenol Elixir with Codeine) is a Schedule V controlled substance.[48]
Preparations for cough or diarrhea containing small amounts of codeine in combination with two or more other active ingredients are Schedule V in the US, and in some states may be dispensed in amounts up to 4 fl. oz. per 48 hours (one or two states set the limit at 4 fl. oz. per 72 hours) without a prescription. Schedule V specifically consigns the product to state and local regulation beyond certain required record-keeping requirements (a dispensary log must be maintained for two years in a ledger from which pages cannot easily be removed and/or are pre-numbered, and the pharmacist must ask for photo identification) and also maintain controlled substances in the closed system at the root of the régime intended by the Controlled Substances Act of 1970; the codeine in these products was a Schedule II substance when the company making the Schedule V product acquired it for mixing up the end-product.
In locales where dilute codeine preparations are non-prescription, anywhere from very few to perhaps a moderate percentage of pharmacists will sell these preparations without a prescription. However, many states have their own laws that do require a prescription for Schedule V drugs. The December 2008 issue of The Bulletin of the National Codeine OTC Lobby (Vol. XVIII, No. 4) listed 12 states with some kind of OTC access to codeine, noting that small independent pharmacies are the most likely to have it. This situation is roughly equivalent to that in February 1991, when the aforementioned organisation undertook its first comprehensive study of Schedule V and overall codeine, dihydrocodeine, ethylmorphine, and hydrocodone availability.
Other drugs that are present in Schedule V narcotic preparations like the codeine syrups are ethylmorphine and dihydrocodeine. Paregoric and hydrocodone were transferred to Schedule III from Schedule V even if the preparation contains two or more other active ingredients, and diphenoxylate is usually covered by state prescription laws even though this relative of pethidine is a Schedule V substance when adulterated with atropine to prevent abuse.
Around the world, codeine is, contingent on its concentration, a Schedule II and IV drug under the Single Convention on Narcotic Drugs.[49]
Spain
Codeine tablets or preparations require a prescription in Spain although it's often not enforced and many pharmacies will sell codeine products without the requirement of a prescription.[citation needed]
Turkey
Codeine is available by a doctor's prescription. It is still possible to find some pharmacies who sell codeine without any prescription. In big cities, pharmacies often don't sell the drug at all. For OTC codeine containing combinations, the choice is up to the pharmacist.[citation needed]
United Kingdom
In the United Kingdom, higher-strength codeine formulations - such as 30/500 co-codamol, where 30 mg of codeine phosphate is combined with 500 mg paracetamol - are prescription-only medicines (POM). Lower-strength combinations, such as 8/500 (various brands) or 12.8/500 (Panadol Ultra, Solpadeine MAX and others) are available as pharmacy supervised ("behind the counter") medicines. Codeine is also available combined with Ibuprofen; a common formulation is 12.8 mg codeine alongside 200 mg Ibuprofen. It is also available 'behind the counter' with aspirin in doses of 8 mg codeine phosphate and 500mg aspirin (Codis). Codeine Linctus of 15 mg per 5ml is also available behind the counter at some pharmacies, although a purchaser would have to request it specifically from the pharmacist. Intramuscular injection of codeine is a controlled drug under the Misuse of Drugs Act 1971.[citation needed]
References
- ^ Shen H, He MM, Liu H, et al (August 2007). "Comparative metabolic capabilities and inhibitory profiles of CYP2D6.1, CYP2D6.10, and CYP2D6.17". Drug Metab. Dispos. 35 (8): 1292–300. doi:10.1124/dmd.107.015354. PMID 17470523.
- ^ "Codeine". The American Society of Health-System Pharmacists. http://www.drugs.com/monograph/codeine.html. Retrieved 3 April 2011.
- ^ Stefano Guandalini; Haleh Vaziri (November 8 2010). Diarrhea: Diagnostic and Therapeutic Advances. New York, USA: Humana Press. p. 452. ISBN 1607611821. http://books.google.com/?id=BstHGdtpb9AC&printsec=frontcover&dq=Diarrhea:+Diagnostic+and+Therapeutic+Advances#v=onepage&q&f=false.
- ^ Australian Medicines Handbook (2004). Rossi S. ed. Australian Medicines Handbook. Adelaide: Australian Medicines Handbook. ISBN 978-0-9757919-2-9. OCLC 224913182 224831213 224913182.
- ^ Codeine Information from Drugs.com
- ^ Advanced Hormone Physiology
- ^ Busch and Grenfield, et al.
- ^ CTV News, Codeine use while breastfeeding may be dangerous, Wed. Aug. 20 2008 9:42 PM ET.
- ^ Koren G, Cairns J, Chitayat D, Gaedigk A, Leeder SJ (August 2006). "Pharmacogenetics of morphine poisoning in a breastfed neonate of a codeine-prescribed mother". Lancet 368 (9536): 704. doi:10.1016/S0140-6736(06)69255-6. PMID 16920476.
- ^ Alberta Health Services; AADAC (April 16, 2007). "The ABCs - Codeine and Other Opioid Painkillers". Alberta Alcohol and Drug Abuse Commission. http://www.aadac.com/87_436.asp. Retrieved Sep 12 2008.
- ^ a b c Vree TB, van Dongen RT, Koopman-Kimenai PM (2000). "Codeine analgesia is due to codeine-6-glucuronide, not morphine". Int. J. Clin. Practa. 54 (6): 395–8. PMID 11092114.
- ^ a b Srinivasan V, Wielbo D, Tebbett IR (1997). "Analgesic effects of codeine-6-glucuronide after intravenous administration". European Journal of Pain 1 (3): 185–90. doi:10.1016/S1090-3801(97)90103-8. PMID 15102399.
- ^ Dr. Nalini Vadivelu MD; Dr. Richard D. Urman MD; Dr. Roberta L. Hines MD (March 3 2011). Essentials of Pain Management. New York, USA: Springer Science. p. 649. ISBN 0387875786. http://books.google.com/?id=rFLLYkCg-FsC&printsec=frontcover&dq=Essentials+of+Pain+Management+By+Nalini+Vadivelu#v=onepage&q&f=false.
- ^ [nzic.org.nz/ChemProcesses/biotech/12C.pdf Opiate Chemistry and Metabolism]
- ^ Dr.Marcus F. Kuntze, MD; Dr. Franz Muller-Spahn, MD; Dieter Ladewig; Alex H. Bullinger (March 2003). Basic and clinical science of opioid addiction. New York, USA: S Karger Pub). pp. 72. ISBN 3805575041. http://books.google.com/?id=ukVA-JaFR_gC&printsec=frontcover&dq=Basic+and+clinical+science+of+opioid+addiction#v=onepage&q&f=false.
- ^ APAP/CODEINE 650/30 mg
- ^ a b Opiates.com - Codeine
- ^ Pain Management
- ^ Drugs.com - Promethazine w/ Codeine
- ^ Drugs.com - Codeine w/ Diphenhydramine & Phenylephrine
- ^ Drugs.com - Codeine w/ Guaifenesin
- ^ Armstrong SC, Cozza KL (2003). "Pharmacokinetic drug interactions of morphine, codeine, and their derivatives: theory and clinical reality, Part II". Psychosomatics 44 (6): 515–20. doi:10.1176/appi.psy.44.6.515. PMID 14597688.
- ^ Fernandes LC, Kilicarslan T, Kaplan HL, Tyndale RF, Sellers EM, Romach MK (June 2002). "Treatment of codeine dependence with inhibitors of cytochrome P450 2D6". J Clin Psychopharmacol 22 (3): 326–9. doi:10.1097/00004714-200206000-00014. PMID 12006904.
- ^ Kathiramalainathan K, Kaplan HL, Romach MK, et al. (2000). "Inhibition of cytochrome P450 2D6 modifies codeine abuse liability". J Clin Psychopharmacol 20 (4): 435–44. doi:10.1097/00004714-200008000-00008. ISBN 0000800000008. PMID 10917405.
- ^ Koren G, Cairns J, Chitayat D, Gaedigk A, Leeder SJ (2006). "Pharmacogenetics of morphine poisoning in a breastfed neonate of a codeine-prescribed mother". Lancet 368 (9536): 704. doi:10.1016/S0140-6736(06)69255-6. PMID 16920476.
- ^ Willmann S, Edginton AN, Coboeken K, Ahr G, Lippert J (2009). "Risk to the Breast-Fed Neonate From Codeine Treatment to the Mother: A Quantitative Mechanistic Modeling Study". Clinical Pharmacology & Therapeutics 86 (6): 634–43. doi:10.1038/clpt.2009.151.
- ^ "Codeine Information - Facts - Codeine". http://codeine.50g.com/info/codeine.html. Retrieved 2007-07-16.
- ^ Lurcott G (1998). "The effects of the genetic absence and inhibition of CYP2D6 on the metabolism of codeine and its derivatives, hydrocodone and oxycodone". Anesth Prog 45 (4): 154–6. PMC 2148980. PMID 10483388. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=2148980.
- ^ Gasche Y, Daali Y, Fathi M, et al. (December 2004). "Codeine intoxication associated with ultrarapid CYP2D6 metabolism". N. Engl. J. Med. 351 (27): 2827–31. doi:10.1056/NEJMoa041888. PMID 15625333.
- ^ Caraco Y (December 2004). "Genes and the response to drugs". N. Engl. J. Med. 351 (27): 2867–9. doi:10.1056/NEJMe048278. PMID 15625340.
- ^ Andreas Luch (2009). Molecular, clinical and environmental toxicology. Springer. p. 20. ISBN 3764383356. http://books.google.com/?id=MtOiLVWBn8cC&pg=PA20.
- ^ a b Science Daily (March 2010) - "Unlocking the Opium Poppy's Biggest Secret: Genes That Make Codeine, Morphine"
- ^ Elmhurt College - Narcotic Analgesic Drugs
- ^ Boekhout van Solinge, Tim (1996). "7. La politique de soins des années quatre-vingt-dix" (in French). L'héroïne, la cocaïne et le crack en France. Trafic, usage et politique. Amsterdam: CEDRO Centrum voor Drugsonderzoek, Universiteit van Amsterdam. pp. 247–262. http://www.cedro-uva.org/lib/boekhout.heroine.fr.7.html.
- ^ Leinwand, Donna (2006-10-18). "DEA warns of soft drink-cough syrup mix". USA Today. http://www.usatoday.com/news/nation/2006-10-18-lean_x.htm?csp=34. Retrieved 2006-10-23.
- ^ Hogshire, Jim (June 1999). Pills-A-Go-Go: A Fiendish Investigation into Pill Marketing, Art, History & Consumption. Los Angeles: Feral House. pp. 216–223. ISBN 978-0-922915-53-8.
- ^ Thevis M, Opfermann G, Schänzer W (2003). "Urinary concentrations of morphine and codeine after consumption of poppy seeds". J. Anal. Toxicol. 27 (1): 53–6. PMID 12587685.
- ^ Cone EJ, Welch P, Paul BD, Mitchell JM (1991). "Forensic drug testing for opiates, III. Urinary excretion rates of morphine and codeine following codeine administration". J. Anal. Toxicol. 15 (4): 161–6. PMID 1943064.
- ^ Baselt, R. (2008). Disposition of Toxic Drugs and Chemicals in Man (8th ed.). Foster City CA: Biomedical Publications. pp. 355–360.
- ^ "Codeine crackdown comes into effect". ABC.net.au. http://www.abc.net.au/news/stories/2010/05/01/2887640.htm. Retrieved 2010-11-22.
- ^ "vital list of codein". vidal.com. http://www.vidal.fr/Substance/codeine-1039.htm. Retrieved 2011-01-12.
- ^ "Pharmacies in Greece". About.com. http://gogreece.about.com/od/planagreattriptogreece/a/greecepharmacy_2.htm. Retrieved 2009-10-10.
- ^ The Irish Times
- ^ Office of The Attorney General, Regulation 5(1)(e) of the Regulation of Retail Pharmacy Businesses Regulations 2008 (S.I. 488 of 2008)
- ^ [www.thepsi.ie/Libraries/Consultations/Draft_Codeine_Guidelines.sflb.ashx Pharmaceutical Society of Ireland]
- ^ Business and History - Merck Frosst Canada Inc. | Western Libraries
- ^ "Headache Triggers: Caffeine". WebMD. June 2004. http://www.webmd.com/content/article/46/1826_50681.htm. Retrieved 2007-03-23.
- ^ Valeant Pharmaceuticals. "Prescribing Information for Capital with Codeine (acetaminophen with codeine) showing Schedule V designation" (PDF). http://www.valeant.com/fileRepository/products/PI/Capital_with_Codeine_Suspension_120mg_PI_Aug04.pdf. Retrieved 2011-02-25.
- ^ International Narcotics Control Board. "List of Narcotic Drugs under International Control" (PDF). http://www.incb.org/pdf/e/list/46thedition.pdf. Retrieved 2006-05-24.
Analgesics (N02A, N02B) Opioids
See also: Opioids templateOpium & alkaloids thereofSemi-synthetic opium
derivativesSynthetic opioidsAlphaprodine • Anileridine • Butorphanol • Dextromoramide • Dextropropoxyphene • Dezocine • Fentanyl • Ketobemidone • Levorphanol • Methadone • Meptazinol • Nalbuphine • Pentazocine • Propoxyphene • Propiram • Pethidine • Phenazocine • Piminodine • Piritramide • Tapentadol • Tilidine • Tramadol
Pyrazolones Cannabinoids Anilides Non-steroidal
anti-inflammatories
See also: NSAIDs templatePropionic acid classFenoprofen • Flurbiprofen • Ibuprofen# • Ketoprofen • Naproxen • Oxaprozin
Oxicam classAcetic acid classDiclofenac • Indometacin • Ketorolac • Nabumetone • Sulindac • Tolmetin
Celecoxib • Rofecoxib • Valdecoxib • Parecoxib • Lumiracoxib
Anthranilic acid
(fenamate) classMeclofenamate • Mefenamic acid
SalicylatesAspirin (Acetylsalicylic acid)# • Benorylate • Diflunisal • Ethenzamide • Magnesium salicylate • Salicin • Salicylamide • Salsalate • Trisalate • Wintergreen (Methyl salicylate)
Atypical, adjuvant and potentiators,
Metabolic agents and miscellaneousAmitryptiline • Befiradol • Bicifadine • Carisoprodol • Camphor • Cimetidine • Clonidine • Chlorzoxazone • Cyclobenzaprine • Duloxetine • Esreboxetine • Flupirtine • Gabapentin • Glafenine • Hydroxyzine • Ketamine • Menthol • Mephenoxalone • Methocarbamol • Nefopam • Orphenadrine • Pregabalin • Proglumide • Scopolamine • Tebanicline • Trazodone • Gabapentin enacarbil • ZiconotideAntidiarrheals, intestinal anti-inflammatory/anti-infective agents (A07) Rehydration Intestinal anti-infectives Antibiotics (Neomycin, Nystatin, Natamycin, Streptomycin, Polymyxin B, Paromomycin, Amphotericin B, Kanamycin, Vancomycin, Colistin, Rifaximin)
Sulfonamides (Phthalylsulfathiazole, Sulfaguanidine, Succinylsulfathiazole)
Nitrofuran (Nifuroxazide, Nifurzide)
Arsenical (Acetarsol)
Oxyquinoline (Broxyquinoline)Intestinal adsorbents Antipropulsives (opioids) Opium Tincture (Laudanum) • Codeine • Morphine • Camphorated Opium Tincture (Paregoric)
crosses BBB: Diphenoxylate (Diphenoxylate/atropine) • Difenoxin
does not cross BBB: LoperamideIntestinal anti-inflammatory agents corticosteroids acting locally (Prednisolone, Hydrocortisone, Prednisone, Betamethasone, Tixocortol, Budesonide, Beclometasone)
antiallergic agents, excluding corticosteroids (Cromoglicic acid)
aminosalicylic acid and similar agents (Sulfasalazine, Mesalazine, Olsalazine, Balsalazide)Antidiarrheal micro-organisms Other antidiarrheals Cough and cold preparations (R05) Expectorants Mucolytics Acetylcysteine • Ambroxol • Bromhexine • Carbocisteine • Domiodol • Dornase alfa • Eprazinone • Erdosteine • Letosteine • Mesna • Neltenexine • Sobrerol • Stepronin • TioproninCough suppressants Acetyldihydrocodeine • Benzylmorphine • Codeine • Dextromethorphan • Diacetylmorphine • Dihydrocodeine • Dimemorfan • Droxypropine • Ethylmorphine • Hydrocodone • Hydromorphone • Isoaminile • Laudanum • Levomethadone • Levopropoxyphene • Methadone • Nicocodeine • Nicodicodeine • Normethadone • Noscapine • Pholcodine • Thebacon • Tipepidine • ZipeprolOtherBenzonatate • Benproperine • Bibenzonium bromide • Butamirate • Clobutinol • Clofedanol • Cloperastine • Diphenhydramine • Dibunate • Dimethoxanate • Dropropizine • Fedrilate • Glaucine • Levodropropizine • Meprotixol • Morclofone • Nepinalone • Oxolamine • Oxeladin • Pentoxyverine • Pipazetate • Prenoxdiazine • PiperidioneCategories:- French inventions
- Antitussives
- Antidiarrhoeals
- Natural opium alkaloids
- World Health Organization essential medicines
- Phenol ethers
- Morphinans
- Alkenes
- Opiates
- Prodrugs
Wikimedia Foundation. 2010.
