- Myocardial infarction
-
"Heart attack" redirects here. For other uses, see Heart attack (disambiguation).
Myocardial infarction Classification and external resources 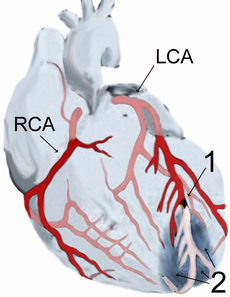
Diagram of a myocardial infarction (2) of the tip of the anterior wall of the heart (an apical infarct) after occlusion (1) of a branch of the left coronary artery (LCA), right coronary artery = RCA.ICD-10 I21-I22 ICD-9 410 DiseasesDB 8664 MedlinePlus 000195 eMedicine med/1567 emerg/327 ped/2520 MeSH D009203 Myocardial infarction (MI) or acute myocardial infarction (AMI), commonly known as a heart attack, results from the interruption of blood supply to a part of the heart, causing heart cells to die. This is most commonly due to occlusion (blockage) of a coronary artery following the rupture of a vulnerable atherosclerotic plaque, which is an unstable collection of lipids (cholesterol and fatty acids) and white blood cells (especially macrophages) in the wall of an artery. The resulting ischemia (restriction in blood supply) and ensuing oxygen shortage, if left untreated for a sufficient period of time, can cause damage or death (infarction) of heart muscle tissue (myocardium).
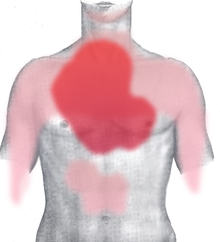
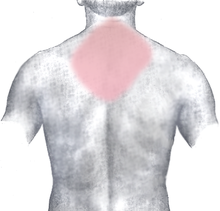
Classical symptoms of acute myocardial infarction include sudden chest pain (typically radiating to the left arm or left side of the neck), shortness of breath, nausea, vomiting, palpitations, sweating, and anxiety (often described as a sense of impending doom).[1] Women may experience fewer typical symptoms than men, most commonly shortness of breath, weakness, a feeling of indigestion, and fatigue.[2] Approximately one quarter of all myocardial infarctions are "silent", that is without chest pain or other symptoms.
Among the diagnostic tests available to detect heart muscle damage are an electrocardiogram (ECG), echocardiography, cardiac MRI and various blood tests. The most often used blood markers are the creatine kinase-MB (CK-MB) fraction and the troponin levels. Immediate treatment for suspected acute myocardial infarction includes oxygen, aspirin, and sublingual nitroglycerin.[3]
Most cases of STEMI (ST elevation MI) are treated with thrombolysis or percutaneous coronary intervention (PCI). NSTEMI (non-ST elevation MI) should be managed with medication, although PCI is often performed during hospital admission. In people who have multiple blockages and who are relatively stable, or in a few emergency cases, bypass surgery may be an option, especially in diabetics.
Heart attacks are the leading cause of death for both men and women worldwide.[4] Important risk factors are previous cardiovascular disease, older age, tobacco smoking, high blood levels of certain lipids (triglycerides, low-density lipoprotein) and low levels of high density lipoprotein (HDL), diabetes, high blood pressure, obesity, chronic kidney disease, heart failure, excessive alcohol consumption, the abuse of certain drugs (such as cocaine and methamphetamine), and chronic high stress levels.[5][6]
Contents
Classification
There are two basic types of acute myocardial infarction:
- Transmural: associated with atherosclerosis involving major coronary artery. It can be subclassified into anterior, posterior, inferior, lateral or septal. Transmural infarcts extend through the whole thickness of the heart muscle and are usually a result of complete occlusion of the area's blood supply.[7]
- Subendocardial: involving a small area in the subendocardial wall of the left ventricle, ventricular septum, or papillary muscles. Subendocardial infarcts are thought to be a result of locally decreased blood supply, possibly from a narrowing of the coronary arteries. The subendocardial area is farthest from the heart's blood supply and is more susceptible to this type of pathology.[7]
Clinically, a myocardial infarction can be further subclassified into a ST elevation MI (STEMI) versus a non-ST elevation MI (non-STEMI) based on ECG changes.[8]
The phrase "heart attack" is sometimes used incorrectly to describe sudden cardiac death, which may or may not be the result of acute myocardial infarction. A heart attack is different from, but can be the cause of cardiac arrest, which is the stopping of the heartbeat, and cardiac arrhythmia, an abnormal heartbeat. It is also distinct from heart failure, in which the pumping action of the heart is impaired; severe myocardial infarction may lead to heart failure, but not necessarily.[citation needed]
A 2007 consensus document classifies myocardial infarction into five main types:[9]
- Type 1 – Spontaneous myocardial infarction related to ischaemia due to a primary coronary event such as plaque erosion and/or rupture, fissuring, or dissection
- Type 2 – Myocardial infarction secondary to ischaemia due to either increased oxygen demand or decreased supply, e.g. coronary artery spasm, coronary embolism, anaemia, arrhythmias, hypertension, or hypotension
- Type 3 – Sudden unexpected cardiac death, including cardiac arrest, often with symptoms suggestive of myocardial ischaemia, accompanied by presumably new ST elevation, or new LBBB, or evidence of fresh thrombus in a coronary artery by angiography and/or at autopsy, but death occurring before blood samples could be obtained, or at a time before the appearance of cardiac biomarkers in the blood
- Type 4 – Associated with coronary angioplasty or stents:
- Type 4a – Myocardial infarction associated with PCI
- Type 4b – Myocardial infarction associated with stent thrombosis as documented by angiography or at autopsy
- Type 5 – Myocardial infarction associated with CABG
Signs and symptoms
The onset of symptoms in myocardial infarction (MI) is usually gradual, over several minutes, and rarely instantaneous.[10] Chest pain is the most common symptom of acute myocardial infarction and is often described as a sensation of tightness, pressure, or squeezing. Chest pain due to ischemia (a lack of blood and hence oxygen supply) of the heart muscle is termed angina pectoris. Pain radiates most often to the left arm, but may also radiate to the lower jaw, neck, right arm,[not in citation given] back, and epigastrium, where it may mimic heartburn. Levine's sign, in which the patient localizes the chest pain by clenching their fist over the sternum, has classically been thought to be predictive of cardiac chest pain, although a prospective observational study showed that it had a poor positive predictive value.[11]
Shortness of breath (dyspnea) occurs when the damage to the heart limits the output of the left ventricle, causing left ventricular failure and consequent pulmonary edema. Other symptoms include diaphoresis (an excessive form of sweating),[1] weakness, light-headedness, nausea, vomiting, and palpitations. These symptoms are likely induced by a massive surge of catecholamines from the sympathetic nervous system[12] which occurs in response to pain and the hemodynamic abnormalities that result from cardiac dysfunction. Loss of consciousness (due to inadequate cerebral perfusion and cardiogenic shock) and sudden death (frequently due to the development of ventricular fibrillation) can occur in myocardial infarctions.[citation needed]
Women and older patients report atypical symptoms more frequently than their male and younger counterparts.[13] Women also report more numerous symptoms compared with men (2.6 on average vs 1.8 symptoms in men).[13] The most common symptoms of MI in women include dyspnea (shortness of breath), weakness, and fatigue. Fatigue, sleep disturbances, and dyspnea have been reported as frequently occurring symptoms which may manifest as long as one month before the actual clinically manifested ischemic event. In women, chest pain may be less predictive of coronary ischemia than in men.[14]
Approximately one fourth of all myocardial infarctions are silent, without chest pain or other symptoms.[15] These cases can be discovered later on electrocardiograms, using blood enzyme tests or at autopsy without a prior history of related complaints. A silent course is more common in the elderly, in patients with diabetes mellitus[16] and after heart transplantation, probably because the donor heart is not fully innervated by the nervous system of the recipient.[17] In diabetics, differences in pain threshold, autonomic neuropathy, and psychological factors have been cited as possible explanations for the lack of symptoms.[16]
Any group of symptoms compatible with a sudden interruption of the blood flow to the heart are called an acute coronary syndrome.[18]
The differential diagnosis includes other catastrophic causes of chest pain, such as pulmonary embolism, aortic dissection, pericardial effusion causing cardiac tamponade, tension pneumothorax, and esophageal rupture. Other non-catastrophic differentials include gastroesophageal reflux and Tietze's syndrome.[19]
Causes
Heart attack rates are higher in association with intense exertion, be it psychological stress or physical exertion, especially if the exertion is more intense than the individual usually performs.[20] Quantitatively, the period of intense exercise and subsequent recovery is associated with about a 6-fold higher myocardial infarction rate (compared with other more relaxed time frames) for people who are physically very fit.[20] For those in poor physical condition, the rate differential is over 35-fold higher.[20] One observed mechanism for this phenomenon is the increased arterial pulse pressure stretching and relaxation of arteries with each heart beat which, as has been observed with intravascular ultrasound, increases mechanical "shear stress" on atheromas and the likelihood of plaque rupture.[20]
Acute severe infection, such as pneumonia, can trigger myocardial infarction. A more controversial link is that between Chlamydophila pneumoniae infection and atherosclerosis.[21] While this intracellular organism has been demonstrated in atherosclerotic plaques, evidence is inconclusive as to whether it can be considered a causative factor.[21] Treatment with antibiotics in patients with proven atherosclerosis has not demonstrated a decreased risk of heart attacks or other coronary vascular diseases.[22]
There is an association of an increased incidence of a heart attack in the morning hours, more specifically around 9 a.m.[23][24][25] Some investigators have noticed that the ability of platelets to aggregate varies according to a circadian rhythm, although they have not proven causation.[26]
Risk factors
Risk factors for atherosclerosis are generally risk factors for myocardial infarction:[citation needed]
- Diabetes (with or without insulin resistance) – the single most important risk factor for ischaemic heart disease (IHD)
- Tobacco smoking
- Air pollution[27]
- Hypercholesterolemia (more accurately hyperlipoproteinemia, especially high low density lipoprotein and low high density lipoprotein)
- Low HDL
- High Triglycerides
- High blood pressure
- Family history of ischaemic heart disease (IHD)
- Obesity[28] (defined by a body mass index of more than 30 kg/m², or alternatively by waist circumference or waist-hip ratio).
- Age — Men acquire an independent risk factor at age 45, Women acquire an independent risk factor at age 55; in addition individuals acquire another independent risk factor if they have a first-degree male relative (brother, father) who suffered a coronary vascular event at or before age 55. Another independent risk factor is acquired if one has a first-degree female relative (mother, sister) who suffered a coronary vascular event at age 65 or younger.
- Hyperhomocysteinemia (high homocysteine, a toxic blood amino acid that is elevated when intakes of vitamins B2, B6, B12 and folic acid are insufficient)
- Stress — Occupations with high stress index are known to have susceptibility for atherosclerosis
- Alcohol — Studies show that prolonged exposure to high quantities of alcohol can increase the risk of heart attack
- Males are more at risk than females.[20]
Many of these risk factors are modifiable, so many heart attacks can be prevented by maintaining a healthier lifestyle. Physical activity, for example, is associated with a lower risk profile.[29] Non-modifiable risk factors include age, sex, and family history of an early heart attack (before the age of 60), which is thought of as reflecting a genetic predisposition.[20]
Socioeconomic factors such as a shorter education and lower income (particularly in women), and unmarried cohabitation are also correlated with a higher risk of MI.[30] To understand epidemiological study results, it's important to note that many factors associated with MI mediate their risk via other factors. For example, the effect of education is partially based on its effect on income and marital status.[30]
Women who use combined oral contraceptive pills have a modestly increased risk of myocardial infarction, especially in the presence of other risk factors, such as smoking.[31]
Inflammation is known to be an important step in the process of atherosclerotic plaque formation.[32] C-reactive protein (CRP) is a sensitive but non-specific marker for inflammation. Elevated CRP blood levels, especially measured with high sensitivity assays, can predict the risk of MI, as well as stroke and development of diabetes.[32] Moreover, some drugs for MI might also reduce CRP levels.[32] The use of high sensitivity CRP assays as a means of screening the general population is advised against, but it may be used optionally at the physician's discretion, in patients who already present with other risk factors or known coronary artery disease.[33] Whether CRP plays a direct role in atherosclerosis remains uncertain.[32]
Inflammation in periodontal disease may be linked to coronary heart disease, and since periodontitis is very common, this could have great consequences for public health.[34] Serological studies measuring antibody levels against typical periodontitis-causing bacteria found that such antibodies were more present in subjects with coronary heart disease.[35] Periodontitis tends to increase blood levels of CRP, fibrinogen and cytokines;[36] thus, periodontitis may mediate its effect on MI risk via other risk factors.[37] Preclinical research suggests that periodontal bacteria can promote aggregation of platelets and promote the formation of foam cells.[38][39] A role for specific periodontal bacteria has been suggested but remains to be established.[40] There is some evidence that influenza may trigger an acute myocardial infarction.[41]
Baldness, hair greying, a diagonal earlobe crease (Frank's sign[42]) and possibly other skin features have been suggested as independent risk factors for MI.[43] Their role remains controversial; a common denominator of these signs and the risk of MI is supposed, possibly genetic.[44]
Calcium deposition is another part of atherosclerotic plaque formation. Calcium deposits in the coronary arteries can be detected with CT scans. Several studies have shown that coronary calcium can provide predictive information beyond that of classical risk factors.[45][46][47]
The European Society of Cardiology and the European Association for Cardiovascular Prevention and Rehabilitation have developed an interactive tool for prediction and managing the risk of heart attack and stroke in Europe. HeartScore is aimed at supporting clinicians in optimising individual cardiovascular risk reduction. The Heartscore Programme is available in 12 languages and offers web based or PC version.[48]
Pathophysiology
See also: Acute coronary syndrome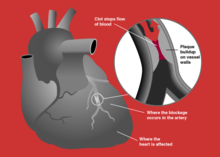 A myocardial infarction occurs when an atherosclerotic plaque slowly builds up in the inner lining of a coronary artery and then suddenly ruptures, causing catastrophic thrombus formation, totally occluding the artery and preventing blood flow downstream.
A myocardial infarction occurs when an atherosclerotic plaque slowly builds up in the inner lining of a coronary artery and then suddenly ruptures, causing catastrophic thrombus formation, totally occluding the artery and preventing blood flow downstream.
Acute myocardial infarction refers to two subtypes of acute coronary syndrome, namely non-ST-elevated myocardial infarction and ST-elevated myocardial infarction, which are most frequently (but not always) a manifestation of coronary artery disease.[8] The most common triggering event is the disruption of an atherosclerotic plaque in an epicardial coronary artery, which leads to a clotting cascade, sometimes resulting in total occlusion of the artery.[49][50] Atherosclerosis is the gradual buildup of cholesterol and fibrous tissue in plaques in the wall of arteries (in this case, the coronary arteries), typically over decades.[51] Blood stream column irregularities visible on angiography reflect artery lumen narrowing as a result of decades of advancing atherosclerosis.[52] Plaques can become unstable, rupture, and additionally promote a thrombus (blood clot) that occludes the artery; this can occur in minutes. When a severe enough plaque rupture occurs in the coronary vasculature, it leads to myocardial infarction (necrosis of downstream myocardium).[49][50]
If impaired blood flow to the heart lasts long enough, it triggers a process called the ischemic cascade; the heart cells in the territory of the occluded coronary artery die (chiefly through necrosis) and do not grow back. A collagen scar forms in its place. Recent studies indicate that another form of cell death called apoptosis also plays a role in the process of tissue damage subsequent to myocardial infarction.[53] As a result, the patient's heart will be permanently damaged. This myocardial scarring also puts the patient at risk for potentially life threatening arrhythmias, and may result in the formation of a ventricular aneurysm that can rupture with catastrophic consequences.
Injured heart tissue conducts electrical impulses more slowly than normal heart tissue. The difference in conduction velocity between injured and uninjured tissue can trigger re-entry or a feedback loop that is believed to be the cause of many lethal arrhythmias. The most serious of these arrhythmias is ventricular fibrillation (V-Fib/VF), an extremely fast and chaotic heart rhythm that is the leading cause of sudden cardiac death. Another life threatening arrhythmia is ventricular tachycardia (V-Tach/VT), which may or may not cause sudden cardiac death. However, ventricular tachycardia usually results in rapid heart rates that prevent the heart from pumping blood effectively. Cardiac output and blood pressure may fall to dangerous levels, which can lead to further coronary ischemia and extension of the infarct.
The cardiac defibrillator is a device that was specifically designed to terminate these potentially fatal arrhythmias. The device works by delivering an electrical shock to the patient in order to depolarize a critical mass of the heart muscle, in effect "rebooting" the heart. This therapy is time dependent, and the odds of successful defibrillation decline rapidly after the onset of cardiopulmonary arrest.
Diagnosis
Main article: Myocardial infarction diagnosisThe diagnosis of myocardial infarction can be made after assessing patient's complaints and physical status. ECG changes, coronary angiogram and levels of cardiac markers help to confirm the diagnosis. ECG gives valuable clues to identify the site of myocardial damage while coronary angiogram allows visualization of narrowing or obstructions in the heart vessels.[54] At autopsy, a pathologist can diagnose a myocardial infarction based on anatomopathological findings.
A chest radiograph and routine blood tests may indicate complications or precipitating causes and are often performed upon arrival to an emergency department. New regional wall motion abnormalities on an echocardiogram are also suggestive of a myocardial infarction. Echo may be performed in equivocal cases by the on-call cardiologist.[55] In stable patients whose symptoms have resolved by the time of evaluation, Technetium (99mTc) sestamibi (i.e. a "MIBI scan") or thallium-201 chloride can be used in nuclear medicine to visualize areas of reduced blood flow in conjunction with physiologic or pharmocologic stress.[55][56] Thallium may also be used to determine viability of tissue, distinguishing whether non-functional myocardium is actually dead or merely in a state of hibernation or of being stunned.[57]
WHO criteria[58] formulated in 1979 have classically been used to diagnose MI; a patient is diagnosed with myocardial infarction if two (probable) or three (definite) of the following criteria are satisfied:
- Clinical history of ischaemic type chest pain lasting for more than 20 minutes
- Changes in serial ECG tracings
- Rise and fall of serum cardiac biomarkers such as creatine kinase-MB fraction and troponin
The WHO criteria were refined in 2000 to give more prominence to cardiac biomarkers.[59] According to the new guidelines, a cardiac troponin rise accompanied by either typical symptoms, pathological Q waves, ST elevation or depression or coronary intervention are diagnostic of MI.
Prevention
The risk of a recurrent myocardial infarction decreases with strict blood pressure management and lifestyle changes, chiefly smoking cessation, regular exercise, a sensible diet for those with heart disease, and limitation of alcohol intake. People are usually commenced on several long-term medications post-MI, with the aim of preventing secondary cardiovascular events such as further myocardial infarctions, congestive heart failure or cerebrovascular accident (CVA). Unless contraindicated, such medications may include:[60][61]
- Antiplatelet drug therapy such as aspirin and/or clopidogrel should be continued to reduce the risk of plaque rupture and recurrent myocardial infarction. Aspirin is first-line, owing to its low cost and comparable efficacy, with clopidogrel reserved for patients intolerant of aspirin. The combination of clopidogrel and aspirin may further reduce risk of cardiovascular events, however the risk of hemorrhage is increased.[62]
- Beta blocker therapy such as metoprolol or carvedilol should be commenced.[63] These have been particularly beneficial in high-risk patients such as those with left ventricular dysfunction and/or continuing cardiac ischaemia.[64] β-Blockers decrease mortality and morbidity. They also improve symptoms of cardiac ischemia in NSTEMI.
- ACE inhibitor therapy should be commenced 24–48 hours post-MI in hemodynamically-stable patients, particularly in patients with a history of MI, diabetes mellitus, hypertension, anterior location of infarct (as assessed by ECG), and/or evidence of left ventricular dysfunction. ACE inhibitors reduce mortality, the development of heart failure, and decrease ventricular remodelling post-MI.[65]
- Statin therapy has been shown to reduce mortality and morbidity post-MI.[66][67] The effects of statins may be more than their LDL lowering effects. The general consensus is that statins have plaque stabilization and multiple other ("pleiotropic") effects that may prevent myocardial infarction in addition to their effects on blood lipids.[68]
- The aldosterone antagonist agent eplerenone has been shown to further reduce risk of cardiovascular death post-MI in patients with heart failure and left ventricular dysfunction, when used in conjunction with standard therapies above.[69] Spironolactone is another option that is sometimes preferable to eplerenone due to cost.
- Evidence supports the consumption of polyunsaturated fats instead of saturated fats as a measure of decreasing coronary heart disease.[70] Omega-3 fatty acids, commonly found in fish, have been shown to reduce mortality post-MI.[71] While the mechanism by which these fatty acids decrease mortality is unknown, it has been postulated that the survival benefit is due to electrical stabilization and the prevention of ventricular fibrillation.[72] However, further studies in a high-risk subset have not shown a clear-cut decrease in potentially fatal arrhythmias due to omega-3 fatty acids.[73][74]
Blood donation may reduce the risk of heart disease for men,[75] but the link has not been firmly established.
A Cochrane review found that giving heparin to people who have heart conditions like unstable angina and some forms of heart attacks reduces the risk of having another heart attack. However, heparin also increases the chance of suffering from minor bleeding.[76]
Management
Main article: Myocardial infarction managementAn MI is a medical emergency which requires immediate medical attention. Treatment attempts to salvage as much myocardium as possible and to prevent further complications, thus the phrase "time is muscle".[77] Oxygen, aspirin, and nitroglycerin may be administered. Morphine was classically used if nitroglycerin was not effective; however, it may increase mortality in the setting of NSTEMI.[78] A 2009 and 2010 review of high flow oxygen in myocardial infarction found increased mortality and infarct size, calling into question the recommendation about its routine use.[79][80] Other analgesics such as nitrous oxide are of unknown benefit.[81] Percutaneous coronary intervention (PCI) or fibrinolysis are recommended in those with an STEMI.
Prognosis
The prognosis post myocardial infarction varies greatly, depending on a person's health, the extent of the heart damage and the treatment given. For the period 2005–2008 in the United States the median mortality at 30 days was 16.6% with a range from 10.9% to 24.9% depending on the hospital.[82] Using variables available in the emergency room, people with a higher risk of adverse outcome can be identified. One study found that 0.4% of patients with a low risk profile died after 90 days, whereas in high risk people it was 21.1%.[83]
Some of the more reproduced risk stratifying factors include: age, hemodynamic parameters (such as heart failure, cardiac arrest on admission, systolic blood pressure, or Killip class of two or greater), ST-segment deviation, diabetes, serum creatinine, peripheral vascular disease and elevation of cardiac markers.[83][84][85] Assessment of left ventricular ejection fraction may increase the predictive power.[86] The prognostic importance of Q-waves is debated.[87] Prognosis is significantly worsened if a mechanical complication such as papillary muscle or myocardial free wall rupture occur.[88] Morbidity and mortality from myocardial infarction has improved over the years due to better treatment.[89]
Complications
Main article: Myocardial infarction complicationsComplications may occur immediately following the heart attack (in the acute phase), or may need time to develop (a chronic problem). Acute complications may include heart failure if the damaged heart is no longer able to adequately pump blood around the body; aneurysm or rupture of the myocardium; mitral regurgitation, particularly if the infarction causes dysfunction of the papillary muscle; and arrhythmias, such as ventricular fibrillation, ventricular tachycardia, atrial fibrillation and heart block. Longer-term complications include heart failure, atrial fibrillation, and the increased risk of a second myocardial infarction.
Epidemiology
Myocardial infarction is a common presentation of ischemic heart disease. The WHO estimated in 2002, that 12.6 percent of worldwide deaths were from ischemic heart disease[4] with it the leading cause of death in developed countries, and third to AIDS and lower respiratory infections in developing countries.[90] Worldwide more than 3 million people have STEMIs and 4 million have NSTEMIs a year.[91]
Coronary heart disease is responsible for 1 in 5 deaths in the United States. It is becoming more common in the developing world such that in India, cardiovascular disease (CVD) is the leading cause of death.[92] The deaths due to CVD in India were 32% of all deaths in 2007 and are expected to rise from 1.17 million in 1990 and 1.59 million in 2000 to 2.03 million in 2010.[93] Although a relatively new epidemic in India, it has quickly become a major health issue with deaths due to CVD expected to double during 1985–2015.[94][95] Mortality estimates due to CVD vary widely by state, ranging from 10% in Meghalaya to 49% in Punjab (percentage of all deaths). Punjab (49%), Goa (42%), Tamil Nadu (36%) and Andhra Pradesh (31%) have the highest CVD related mortality estimates.[96] State-wise differences are correlated with prevalence of specific dietary risk factors in the states. Moderate physical exercise is associated with reduced incidence of CVD in India (those who exercise have less than half the risk of those who don't).[94]
Legal implications
At common law, a myocardial infarction is generally a disease, but may sometimes be an injury. This has implications for no-fault insurance schemes such as workers' compensation. A heart attack is generally not covered;[97] however, it may be a work-related injury if it results, for example, from unusual emotional stress or unusual exertion.[98] Additionally, in some jurisdictions, heart attacks suffered by persons in particular occupations such as police officers may be classified as line-of-duty injuries by statute or policy. In some countries or states, a person who has suffered from a myocardial infarction may be prevented from participating in activity that puts other people's lives at risk, for example driving a car or flying an airplane.[99]
Research
Patients who receive stem cell treatment by coronary artery injections of stem cells derived from their own bone marrow after a myocardial infarction (MI) show improvements in left ventricular ejection fraction and end-diastolic volume not seen with placebo. The larger the initial infarct size, the greater the effect of the infusion. Clinical trials of progenitor cell infusion as a treatment approach to ST elevation MI are proceeding.[100]
There are currently 3 biomaterial and tissue engineering approaches for the treatment of MI, but these are in an even earlier stage of medical research, so many questions and issues need to be addressed before they can be applied to patients. The first involves polymeric left ventricular restraints in the prevention of heart failure. The second utilizes in vitro engineered cardiac tissue, which is subsequently implanted in vivo. The final approach entails injecting cells and/or a scaffold into the myocardium to create in situ engineered cardiac tissue.[101]
References
- ^ a b Mallinson, T (2010). "Myocardial Infarction". Focus on First Aid (15): 15. http://www.focusonfirstaid.co.uk/Magazine/issue15/index.aspx. Retrieved 2010-06-08.
- ^ Kosuge, M; Kimura K, Ishikawa T et al. (March 2006). "Differences between men and women in terms of clinical features of ST-segment elevation acute myocardial infarction". Circulation Journal 70 (3): 222–226. doi:10.1253/circj.70.222. PMID 16501283. http://www.jstage.jst.go.jp/article/circj/70/3/222/_pdf. Retrieved 2008-05-31.
- ^ Erhardt L, Herlitz J, Bossaert L, et al. (2002). "Task force on the management of chest pain" (PDF). Eur. Heart J. 23 (15): 1153–76. doi:10.1053/euhj.2002.3194. PMID 12206127. http://eurheartj.oxfordjournals.org/cgi/reprint/23/15/1153.
- ^ a b Robert Beaglehole, et al. (2004) (PDF). The World Health Report 2004 – Changing History. World Health Organization. pp. 120–4. ISBN 92-4-156265-X. http://www.who.int/entity/whr/2004/en/report04_en.pdf.
- ^ Bax L, Algra A, Mali WP, Edlinger M, Beutler JJ, van der Graaf Y (2008). "Renal function as a risk indicator for cardiovascular events in 3216 patients with manifest arterial disease". Atherosclerosis 200 (1): 184–90. doi:10.1016/j.atherosclerosis.2007.12.006. PMID 18241872. http://linkinghub.elsevier.com/retrieve/pii/S0021-9150(07)00768-X.
- ^ Pearte CA, Furberg CD, O'Meara ES, et al. (2006). "Characteristics and baseline clinical predictors of future fatal versus nonfatal coronary heart disease events in older adults: the Cardiovascular Health Study". Circulation 113 (18): 2177–85. doi:10.1161/CIRCULATIONAHA.105.610352. PMID 16651468. http://circ.ahajournals.org/cgi/content/full/113/18/2177.
- ^ a b Reznik, AG (2010). "[Morphology of acute myocardial infarction at prenecrotic stage]" (in Russian). Kardiologiia 50 (1): 4–8. PMID 20144151.
- ^ a b Moe KT, Wong P (March 2010). "Current trends in diagnostic biomarkers of acute coronary syndrome". Ann. Acad. Med. Singap. 39 (3): 210–5. PMID 20372757. http://www.annals.edu.sg/pdf/39VolNo3Mar2010/V39N3p210.pdf.
- ^ Thygesen K, Alpert JS, White HD (October 2007). "Universal definition of myocardial infarction". Eur. Heart J. 28 (20): 2525–38. doi:10.1093/eurheartj/ehm355. PMID 17951287. http://eurheartj.oxfordjournals.org/content/28/20/2525.full.
- ^ National Heart, Lung and Blood Institute. Heart Attack Warning Signs. Retrieved November 22, 2006.
- ^ Marcus GM, Cohen J, Varosy PD, et al. (2007). "The utility of gestures in patients with chest discomfort". Am. J. Med. 120 (1): 83–9. doi:10.1016/j.amjmed.2006.05.045. PMID 17208083. http://linkinghub.elsevier.com/retrieve/pii/S0002-9343(06)00668-1.
- ^ Little RA, Frayn KN, Randall PE, et al. (1986). "Plasma catecholamines in the acute phase of the response to myocardial infarction". Arch Emerg Med 3 (1): 20–7. PMC 1285314. PMID 3524599. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=1285314.
- ^ a b Canto JG, Goldberg RJ, Hand MM, et al. (December 2007). "Symptom presentation of women with acute coronary syndromes: myth vs reality". Arch. Intern. Med. 167 (22): 2405–13. doi:10.1001/archinte.167.22.2405. PMID 18071161. http://archinte.ama-assn.org/cgi/pmidlookup?view=long&pmid=18071161.
- ^ McSweeney JC, Cody M, O'Sullivan P, Elberson K, Moser DK, Garvin BJ (2003). "Women's early warning symptoms of acute myocardial infarction". Circulation 108 (21): 2619–23. doi:10.1161/01.CIR.0000097116.29625.7C. PMID 14597589.
- ^ Kannel WB. (1986). "Silent myocardial ischemia and infarction: insights from the Framingham Study". Cardiol Clin 4 (4): 583–91. PMID 3779719.
- ^ a b Davis TM, Fortun P, Mulder J, Davis WA, Bruce DG (2004). "Silent myocardial infarction and its prognosis in a community-based cohort of Type 2 diabetic patients: the Fremantle Diabetes Study". Diabetologia 47 (3): 395–9. doi:10.1007/s00125-004-1344-4. PMID 14963648.
- ^ Rubin's Pathology — Clinicopathological Foundations of Medicine. Maryland: Lippincott Williams & Wilkins. 2001. pp. 549. ISBN 0-7817-4733-3.
- ^ Acute Coronary Syndrome. American Heart Association. Retrieved November 25, 2006.
- ^ Boie ET (2005). "Initial evaluation of chest pain". Emerg. Med. Clin. North Am. 23 (4): 937–57. doi:10.1016/j.emc.2005.07.007. PMID 16199332. http://linkinghub.elsevier.com/retrieve/pii/S0733-8627(05)00059-3.
- ^ a b c d e f Wilson PW, D'Agostino RB, Levy D, Belanger AM, Silbershatz H, Kannel WB. (1998). "Prediction of coronary heart disease using risk factor categories" (PDF). Circulation 97 (18): 1837–47. PMID 9603539. http://circ.ahajournals.org/cgi/reprint/97/18/1837.pdf.
- ^ a b Saikku P, Leinonen M, Tenkanen L, Linnanmaki E, Ekman MR, Manninen V, Manttari M, Frick MH, Huttunen JK. (1992). "Chronic Chlamydia pneumoniae infection as a risk factor for coronary heart disease in the Helsinki Heart Study". Ann Intern Med 116 (4): 273–8. PMID 1733381.
- ^ Andraws R, Berger JS, Brown DL. (2005). "Effects of antibiotic therapy on outcomes of patients with coronary artery disease: a meta-analysis of randomized controlled trials". JAMA 293 (21): 2641–7. doi:10.1001/jama.293.21.2641. PMID 15928286.
- ^ Muller JE, Stone PH, Turi ZG, et al. (1985). "Circadian variation in the frequency of onset of acute myocardial infarction". N. Engl. J. Med. 313 (21): 1315–22. doi:10.1056/NEJM198511213132103. PMID 2865677.
- ^ Beamer AD, Lee TH, Cook EF, et al. (1987). "Diagnostic implications for myocardial ischemia of the circadian variation of the onset of chest pain". Am. J. Cardiol. 60 (13): 998–1002. doi:10.1016/0002-9149(87)90340-7. PMID 3673917.
- ^ Cannon CP, McCabe CH, Stone PH, et al.; McCabe; Stone; Schactman; Thompson; Theroux; Gibson; Feldman et al. (1997). "Circadian variation in the onset of unstable angina and non-Q-wave acute myocardial infarction (the TIMI III Registry and TIMI IIIB)". Am. J. Cardiol. 79 (3): 253–8. doi:10.1016/S0002-9149(97)00743-1. PMID 9036740. http://linkinghub.elsevier.com/retrieve/pii/S0002914997007431.
- ^ Tofler GH, Brezinski D, Schafer AI, et al. (1987). "Concurrent morning increase in platelet aggregability and the risk of myocardial infarction and sudden cardiac death". N. Engl. J. Med. 316 (24): 1514–8. doi:10.1056/NEJM198706113162405. PMID 3587281.
- ^ Peters A, von Klot S, Heier M, Trentinaglia I, Hormann A, Wichmann HE, et al. 2004. Exposure to traffic and the onset of myocardial infarction. N Engl J Med 351:1721–1730
- ^ Yusuf S, Hawken S, Ounpuu S, Bautista L, Franzosi MG, Commerford P, Lang CC, Rumboldt Z, Onen CL, Lisheng L, Tanomsup S, Wangai P Jr, Razak F, Sharma AM, Anand SS; INTERHEART Study Investigators. (2005). "Obesity and the risk of myocardial infarction in 27,000 participants from 52 countries: a case-control study". Lancet 366 (9497): 1640–9. doi:10.1016/S0140-6736(05)67663-5. PMID 16271645.
- ^ Jensen G, Nyboe J, Appleyard M, Schnohr P. (1991). "Risk factors for acute myocardial infarction in Copenhagen, II: Smoking, alcohol intake, physical activity, obesity, oral contraception, diabetes, lipids, and blood pressure". Eur Heart J 12 (3): 298–308. PMID 2040311.
- ^ a b Nyboe J, Jensen G, Appleyard M, Schnohr P. (1989). "Risk factors for acute myocardial infarction in Copenhagen. I: Hereditary, educational and socioeconomic factors. Copenhagen City Heart Study". Eur Heart J 10 (10): 910–6. PMID 2598948.
- ^ Khader YS, Rice J, John L, Abueita O. (2003). "Oral contraceptives use and the risk of myocardial infarction: a meta-analysis". Contraception 68 (1): 11–7. doi:10.1016/S0010-7824(03)00073-8. PMID 12878281.
- ^ a b c d Wilson AM, Ryan MC, Boyle AJ. (2006). "The novel role of C-reactive protein in cardiovascular disease: risk marker or pathogen". Int J Cardiol 106 (3): 291–7. doi:10.1016/j.ijcard.2005.01.068. PMID 16337036.
- ^ Pearson TA, Mensah GA, Alexander RW, Anderson JL, Cannon RO 3rd, Criqui M, Fadl YY, Fortmann SP, Hong Y, Myers GL, Rifai N, Smith SC Jr, Taubert K, Tracy RP, Vinicor F; Centers for Disease Control and Prevention; American Heart Association. (2003). "Markers of inflammation and cardiovascular disease: application to clinical and public health practice: A statement for healthcare professionals from the Centers for Disease Control and Prevention and the American Heart Association" (PDF). Circulation 107 (3): 499–511. doi:10.1161/01.CIR.0000052939.59093.45. PMID 12551878. http://circ.ahajournals.org/cgi/reprint/107/3/499.pdf.
- ^ Janket SJ, Baird AE, Chuang SK, Jones JA. (2003). "Meta-analysis of periodontal disease and risk of coronary heart disease and stroke". Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 95 (5): 559–69. doi:10.1038/sj.ebd.6400272. PMID 12738947.
- ^ Pihlstrom BL, Michalowicz BS, Johnson NW. (2005). "Periodontal diseases". Lancet 366 (9499): 1809–20. doi:10.1016/S0140-6736(05)67728-8. PMID 16298220.
- ^ Scannapieco FA, Bush RB, Paju S. (2003). "Associations between periodontal disease and risk for atherosclerosis, cardiovascular disease, and stroke. A systematic review". Ann Periodontol 8 (1): 38–53. doi:10.1902/annals.2003.8.1.38. PMID 14971247.
- ^ D'Aiuto F, Parkar M, Nibali L, Suvan J, Lessem J, Tonetti MS. (2006). "Periodontal infections cause changes in traditional and novel cardiovascular risk factors: results from a randomized controlled clinical trial". Am Heart J 151 (5): 977–84. doi:10.1016/j.ahj.2005.06.018. PMID 16644317.
- ^ Lourbakos A, Yuan YP, Jenkins AL, Travis J, Andrade-Gordon P, Santulli R, Potempa J, Pike RN. (2001). "Activation of protease-activated receptors by gingipains from Porphyromonas gingivalis leads to platelet aggregation: a new trait in microbial pathogenicity" (PDF). Blood 97 (12): 3790–7. doi:10.1182/blood.V97.12.3790. PMID 11389018. http://bloodjournal.hematologylibrary.org/cgi/reprint/97/12/3790.pdf.
- ^ Qi M, Miyakawa H, Kuramitsu HK. (2003). "Porphyromonas gingivalis induces murine macrophage foam cell formation". Microb Pathog 35 (6): 259–67. doi:10.1016/j.micpath.2003.07.002. PMID 14580389.
- ^ Spahr A, Klein E, Khuseyinova N, Boeckh C, Muche R, Kunze M, Rothenbacher D, Pezeshki G, Hoffmeister A, Koenig W. (2006). "Periodontal infections and coronary heart disease: role of periodontal bacteria and importance of total pathogen burden in the Coronary Event and Periodontal Disease (CORODONT) study". Arch Intern Med 166 (5): 554–9. doi:10.1001/archinte.166.5.554. PMID 16534043.
- ^ Warren-Gash C, Smeeth L, Hayward AC (2009). "Influenza as a trigger for acute myocardial infarction or death from cardiovascular disease: a systematic review". Lancet Infect Dis 9 (10): 601–610. doi:10.1016/S1473-3099(09)70233-6. PMID 19778762.
- ^ Davis TM, Balme M, Jackson D, Stuccio G, Bruce DG (October 2000). "The diagonal ear lobe crease (Frank's sign) is not associated with coronary artery disease or retinopathy in type 2 diabetes: the Fremantle Diabetes Study". Aust N Z J Med 30 (5): 573–7. doi:10.1111/j.1445-5994.2000.tb00858.x. PMID 11108067.
- ^ Lichstein E, Chadda KD, Naik D, Gupta PK. (1974). "Diagonal ear-lobe crease: prevalence and implications as a coronary risk factor". N Engl J Med 290 (11): 615–6. doi:10.1056/NEJM197403142901109. PMID 4812503.
- ^ Miric D, Fabijanic D, Giunio L, Eterovic D, Culic V, Bozic I, Hozo I. (1998). "Dermatological indicators of coronary risk: a case-control study". Int J Cardiol 67 (3): 251–5. doi:10.1016/S0167-5273(98)00313-1. PMID 9894707.
- ^ Greenland P, LaBree L, Azen SP, Doherty TM, Detrano RC (2004). "Coronary artery calcium score combined with Framingham score for risk prediction in asymptomatic individuals". JAMA 291 (2): 210–5. doi:10.1001/jama.291.2.210. PMID 14722147. http://jama.ama-assn.org/cgi/pmidlookup?view=long&pmid=14722147.
- ^ Detrano R, Guerci AD, Carr JJ, et al. (2008). "Coronary calcium as a predictor of coronary events in four racial or ethnic groups". N. Engl. J. Med. 358 (13): 1336–45. doi:10.1056/NEJMoa072100. PMID 18367736. http://content.nejm.org/cgi/pmidlookup?view=short&pmid=18367736&promo=ONFLNS19.
- ^ Arad Y, Goodman KJ, Roth M, Newstein D, Guerci AD (2005). "Coronary calcification, coronary disease risk factors, C-reactive protein, and atherosclerotic cardiovascular disease events: the St. Francis Heart Study". J. Am. Coll. Cardiol. 46 (1): 158–65. doi:10.1016/j.jacc.2005.02.088. PMID 15992651. http://linkinghub.elsevier.com/retrieve/pii/S0735-1097(05)01031-4.
- ^ http://www.heartscore.org
- ^ a b Tsujita K, Kaikita K, Soejima H, Sugiyama S, Ogawa H (April 2010). "[Acute coronary syndrome-initiating factors]" (in Japanese). Nippon Rinsho 68 (4): 607–14. PMID 20387549.
- ^ a b Dohi T, Daida H (April 2010). "[Change of concept and pathophysiology in acute coronary syndrome]" (in Japanese). Nippon Rinsho 68 (4): 592–6. PMID 20387546.
- ^ Woollard KJ, Geissmann F (February 2010). "Monocytes in atherosclerosis: subsets and functions". Nat Rev Cardiol 7 (2): 77–86. doi:10.1038/nrcardio.2009.228. PMC 2813241. PMID 20065951. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=2813241.
- ^ Spaan J, Kolyva C, van den Wijngaard J, et al. (September 2008). "Coronary structure and perfusion in health and disease". Philos Transact a Math Phys Eng Sci 366 (1878): 3137–53. doi:10.1098/rsta.2008.0075. PMID 18559321. http://rsta.royalsocietypublishing.org/cgi/pmidlookup?view=long&pmid=18559321.
- ^ Krijnen PA, Nijmeijer R, Meijer CJ, Visser CA, Hack CE, Niessen HW. (2002). "Apoptosis in myocardial ischaemia and infarction". J Clin Pathol 55 (11): 801–11. doi:10.1136/jcp.55.11.801. PMC 1769793. PMID 12401816. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=1769793.
- ^ Sudheer, MD. "Vessel localisation and Prognostication". LifeHugger. LifeHugger.com. http://www.lifehugger.com/doc/2016/Vessel_localisation_and_prognostication_in_MI. Retrieved 21 January 2011.
- ^ a b DE Fenton et al. Myocardial infarction – eMedicine, retrieved November 27, 2006.
- ^ HEART SCAN – Patient information from University College London. Retrieved November 27, 2006.
- ^ Skoufis E, McGhie AI (1998). "Radionuclide techniques for the assessment of myocardial viability". Tex Heart Inst J 25 (4): 272–9. PMC 325572. PMID 9885104. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=325572.
- ^ Anonymous (March 1979). "Nomenclature and criteria for diagnosis of ischemic heart disease. Report of the Joint International Society and Federation of Cardiology/World Health Organization task force on standardization of clinical nomenclature". Circulation 59 (3): 607–9. PMID 761341.
- ^ Alpert JS, Thygesen K, Antman E, Bassand JP. (2000). "Myocardial infarction redefined—a consensus document of The Joint European Society of Cardiology/American College of Cardiology Committee for the redefinition of myocardial infarction". J Am Coll Cardiol 36 (3): 959–69. doi:10.1016/S0735-1097(00)00804-4. PMID 10987628.
- ^ Rossi S, editor. Australian Medicines Handbook 2006. Adelaide: Australian Medicines Handbook; 2006. ISBN 0-9757919-2-3.
- ^ Smith A, Aylward P, Campbell T, et al. Therapeutic Guidelines: Cardiovascular, 4th edition. North Melbourne: Therapeutic Guidelines; 2003. ISSN 1327-9513
- ^ Peters RJ, Mehta SR, Fox KA, Zhao F, Lewis BS, Kopecky SL, Diaz R, Commerford PJ, Valentin V, Yusuf S; Clopidogrel in Unstable angina to prevent Recurrent Events (CURE) Trial Investigators. (2003). "Effects of aspirin dose when used alone or in combination with clopidogrel in patients with acute coronary syndromes: observations from the Clopidogrel in Unstable angina to prevent Recurrent Events (CURE) study". Circulation 108 (14): 1682–7. doi:10.1161/01.CIR.0000091201.39590.CB. PMID 14504182.
- ^ Yusuf S, Peto R, Lewis J, Collins R, Sleight P (1985). "Beta blockade during and after myocardial infarction: an overview of the randomized trials". Prog Cardiovasc Dis 27 (5): 335–71. doi:10.1016/S0033-0620(85)80003-7. PMID 2858114.
- ^ Dargie HJ. (2001). "Effect of carvedilol on outcome after myocardial infarction in patients with left-ventricular dysfunction: the CAPRICORN randomised trial". Lancet 357 (9266): 1385–90. doi:10.1016/S0140-6736(00)04560-8. PMID 11356434.
- ^ Pfeffer MA, Braunwald E, Moye LA, Basta L, Brown EJ Jr, Cuddy TE, Davis BR, Geltman EM, Goldman S, Flaker GC, et al. (1992). "Effect of captopril on mortality and morbidity in patients with left ventricular dysfunction after myocardial infarction. Results of the survival and ventricular enlargement trial. The SAVE Investigators". N Engl J Med. 327 (10): 669–77. doi:10.1056/NEJM199209033271001. PMID 1386652.
- ^ Sacks FM, Pfeffer MA, Moye LA, Rouleau JL, Rutherford JD, Cole TG, Brown L, Warnica JW, Arnold JM, Wun CC, Davis BR, Braunwald E. (1996). "The effect of pravastatin on coronary events after myocardial infarction in patients with average cholesterol levels. Cholesterol and Recurrent Events Trial investigators". N Engl J Med 335 (14): 1001–9. doi:10.1056/NEJM199610033351401. PMID 8801446.
- ^ Sacks FM, Moye LA, Davis BR, Cole TG, Rouleau JL, Nash DT, Pfeffer MA, Braunwald E. (1998). "Relationship between plasma LDL concentrations during treatment with pravastatin and recurrent coronary events in the Cholesterol and Recurrent Events trial". Circulation 97 (15): 1446–52. PMID 9576424.
- ^ Ray KK, Cannon CP (2005). "The potential relevance of the multiple lipid-independent (pleiotropic) effects of statins in the management of acute coronary syndromes". J. Am. Coll. Cardiol. 46 (8): 1425–33. doi:10.1016/j.jacc.2005.05.086. PMID 16226165. http://linkinghub.elsevier.com/retrieve/pii/S0735-1097(05)01773-0.
- ^ Keating G, Plosker G (2004). "Eplerenone: a review of its use in left ventricular systolic dysfunction and heart failure after acute myocardial infarction". Drugs 64 (23): 2689–707. doi:10.1157/13089615. PMID 15537370.
- ^ Mozaffarian D, Micha R, Wallace S (2010). Katan, Martijn B.. ed. "Effects on Coronary Heart Disease of Increasing Polyunsaturated Fat in Place of Saturated Fat: A Systematic Review and Meta-Analysis of Randomized Controlled Trials". PLoS Med. 7 (3): e1000252. doi:10.1371/journal.pmed.1000252. PMC 2843598. PMID 20351774. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=2843598.
- ^ "Dietary supplementation with n-3 polyunsaturated fatty acids and vitamin E after myocardial infarction: results of the GISSI-Prevenzione trial. Gruppo Italiano per lo Studio della Sopravvivenza nell'Infarto miocardico". Lancet 354 (9177): 447–55. 2001. doi:10.1016/S0140-6736(99)07072-5. PMID 10465168.
- ^ Leaf A, Albert C, Josephson M, Steinhaus D, Kluger J, Kang J, Cox B, Zhang H, Schoenfeld D (2005). "Prevention of fatal arrhythmias in high-risk subjects by fish oil n-3 fatty acid intake". Circulation 112 (18): 2762–8. doi:10.1161/CIRCULATIONAHA.105.549527. PMID 16267249. http://circ.ahajournals.org/cgi/content/full/112/18/2762.
- ^ Brouwer IA, Zock PL, Camm AJ, Bocker D, Hauer RN, Wever EF, Dullemeijer C, Ronden JE, Katan MB, Lubinski A, Buschler H, Schouten EG; SOFA Study Group. (2006). "Effect of fish oil on ventricular tachyarrhythmia and death in patients with implantable cardioverter defibrillators: the Study on Omega-3 Fatty Acids and Ventricular Arrhythmia (SOFA) randomized trial". JAMA 295 (22): 2613–9. doi:10.1001/jama.295.22.2613. PMID 16772624.
- ^ Raitt MH, Connor WE, Morris C, Kron J, Halperin B, Chugh SS, McClelland J, Cook J, MacMurdy K, Swenson R, Connor SL, Gerhard G, Kraemer DF, Oseran D, Marchant C, Calhoun D, Shnider R, McAnulty J. (2005). "Fish oil supplementation and risk of ventricular tachycardia and ventricular fibrillation in patients with implantable defibrillators: a randomized controlled trial". JAMA 293 (23): 2284–91. doi:10.1001/jama.293.23.2884. PMID 15956633.
- ^ Tuomainen TP, Salonen R, Nyyssönen K, Salonen JT (Mar 1997). "Cohort study of relation between donating blood and risk of myocardial infarction in 2682 men in eastern Finland". BMJ 314 (7083): 793–4. PMC 2126176. PMID 9080998. http://bmj.bmjjournals.com/cgi/content/full/314/7083/793.
- ^ Magee KD, Campbell SG, Moher D, Rowe BH (2008). Magee, Kirk. ed. "Heparin versus placebo for acute coronary syndromes". Cochrane Database Syst Rev (2): CD003462. doi:10.1002/14651858.CD003462.pub2. PMID 18425889. http://onlinelibrary.wiley.com/o/cochrane/clsysrev/articles/CD003462/frame.html.
- ^ TIME IS MUSCLE TIME WASTED IS MUSCLE LOST[dead link]. Early Heart Attack Care, St. Agnes Healthcare. Retrieved November 29, 2006.
- ^ Meine TJ, Roe MT, Chen AY, et al. (2005). "Association of intravenous morphine use and outcomes in acute coronary syndromes: results from the CRUSADE Quality Improvement Initiative". Am Heart J 149 (6): 1043–9. doi:10.1016/j.ahj.2005.02.010. PMID 15976786. http://linkinghub.elsevier.com/retrieve/pii/S0002870305001493.
- ^ "Routine use of oxygen in the treatment of myocardial infarction: systematic review – Wijesinghe et al. 95 (3): 198 – Heart". http://heart.bmj.com/cgi/content/full/95/3/198.
- ^ Cabello JB, Burls A, Emparanza JI, Bayliss S, Quinn T (2010). Cabello, Juan B. ed. "Oxygen therapy for acute myocardial infarction". Cochrane Database Syst Rev 6 (6): CD007160. doi:10.1002/14651858.CD007160.pub2. PMID 20556775.
- ^ O'Connor RE, Brady W, Brooks SC, et al. (November 2010). "Part 10: acute coronary syndromes: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care". Circulation 122 (18 Suppl 3): S787–817. doi:10.1161/CIRCULATIONAHA.110.971028. PMID 20956226.
- ^ Krumholz H et al (2009). "Patterns of hospital performance in acute myocardial infarction and heart failure – 30-day mortality and readmission". Circulation: Cardiovascular Quality and Outcomes 2 (5): 407–13. doi:10.1161/CIRCOUTCOMES.109.883256. PMID 20031870. http://circoutcomes.ahajournals.org/cgi/content/abstract/CIRCOUTCOMES.109.883256v1.
- ^ a b López de Sá E, López-Sendón J, Anguera I, Bethencourt A, Bosch X (November 2002). "Prognostic value of clinical variables at presentation in patients with non-ST-segment elevation acute coronary syndromes: results of the Proyecto de Estudio del Pronóstico de la Angina (PEPA)". Medicine (Baltimore) 81 (6): 434–42. doi:10.1097/00005792-200211000-00004. PMID 12441900.
- ^ Fox KA, Dabbous OH, Goldberg RJ, et al. (November 2006). "Prediction of risk of death and myocardial infarction in the six months after presentation with acute coronary syndrome: prospective multinational observational study (GRACE)". BMJ 333 (7578): 1091. doi:10.1136/bmj.38985.646481.55. PMC 1661748. PMID 17032691. http://www.bmj.com/cgi/content/full/333/7578/1091.
- ^ Weir RA, McMurray JJ, Velazquez EJ. (2006). "Epidemiology of heart failure and left ventricular systolic dysfunction after acute myocardial infarction: prevalence, clinical characteristics, and prognostic importance". Am J Cardiol 97 (10A): 13F–25F. doi:10.1016/j.amjcard.2006.03.005. PMID 16698331.
- ^ Bosch X, Theroux P. (2005). "Left ventricular ejection fraction to predict early mortality in patients with non-ST-segment elevation acute coronary syndromes". Am Heart J 150 (2): 215–20. doi:10.1016/j.ahj.2004.09.027. PMID 16086920.
- ^ Nicod P, Gilpin E, Dittrich H, Polikar R, Hjalmarson A, Blacky A, Henning H, Ross J (1989). "Short- and long-term clinical outcome after Q wave and non-Q wave myocardial infarction in a large patient population". Circulation 79 (3): 528–36. doi:10.1161/01.CIR.79.3.528. PMID 2645061.
- ^ Becker RC, Gore JM, Lambrew C, Weaver WD, Rubison RM, French WJ, Tiefenbrunn AJ, Bowlby LJ, Rogers WJ. (1996). "A composite view of cardiac rupture in the United States National Registry of Myocardial Infarction". J Am Coll Cardiol 27 (6): 1321–6. doi:10.1016/0735-1097(96)00008-3. PMID 8626938.
- ^ Liew R, Sulfi S, Ranjadayalan K, Cooper J, Timmis AD. (2006). "Declining case fatality rates for acute myocardial infarction in South Asian and white patients in the past 15 years". Heart 92 (8): 1030–4. doi:10.1136/hrt.2005.078634. PMC 1861115. PMID 16387823. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=1861115.
- ^ "Cause of Death — UC Atlas of Global Inequality". Center for Global, International and Regional Studies (CGIRS) at the University of California Santa Cruz. http://ucatlas.ucsc.edu/cause.php. Retrieved December 7, 2006.
- ^ White HD, Chew DP (August 2008). "Acute myocardial infarction". Lancet 372 (9638): 570–84. doi:10.1016/S0140-6736(08)61237-4. PMID 18707987.
- ^ Mukherjee AK. (1995). "Prediction of coronary heart disease using risk factor categories". J Indian Med Assoc 93 (8): 312–5. PMID 8713248.
- ^ Ghaffar A, Reddy KS and Singhi M (2004). "Burden of non-communicable diseases in South Asia" (PDF). BMJ 328 (7443): 807–810. doi:10.1136/bmj.328.7443.807. PMC 383378. PMID 15070638. http://www.bmj.com/cgi/reprint/328/7443/807.pdf.
- ^ a b Rastogi T, Vaz M, Spiegelman D, Reddy KS, Bharathi AV, Stampfer MJ, Willett WC and Ascherio1 A (2004). "Physical activity and risk of coronary heart disease in India" (PDF). Int. J. Epidemiol 33 (4): 1–9. doi:10.1093/ije/dyh042. PMID 15044412. http://ije.oxfordjournals.org/cgi/reprint/33/4/759.pdf.
- ^ Gupta R. (2007). "Escalating Coronary Heart Disease and Risk Factors in South Asians" (PDF). Indian Heart Journal: 214–17. http://indianheartjournal.com/editorial007.pdf.
- ^ Gupta R, Misra A, Pais P, Rastogi P and Gupta VP. (2006). "Correlation of regional cardiovascular disease mortality in India with lifestyle and nutritional factors" (PDF). International Journal of Cardiology 108 (3): 291–300. doi:10.1016/j.ijcard.2005.05.044. PMID 15978684. http://www.sciencedirect.com/science?_ob=MImg&_imagekey=B6T16-4GFV5CY-4-3&_cdi=4882&_user=209690&_orig=search&_coverDate=04%2F14%2F2006&_sk=998919996&view=c&wchp=dGLzVlz-zSkzV&md5=050edf99a813f475b985c8d590c86228&ie=/sdarticle.pdf.
- ^ Workers' Compensation FAQ. Prairie View A&M University. Retrieved November 22, 2006.
- ^ SIGNIFICANT DECISIONS Subject Index. Board of Industrial Insurance Appeals. Retrieved November 22, 2006.
- ^ "Classification of Drivers' Licenses Regulations". Nova Scotia Registry of Regulations. May 24, 2000. http://www.gov.ns.ca/just/regulations/regs/mvclasdl.htm. Retrieved April 22, 2007.
- ^ Schachinger V, Erbs S, Elsasser A, Haberbosch W, Hambrecht R, Holschermann H, Yu J, Corti R, Mathey DG, Hamm CW, Suselbeck T, Assmus B, Tonn T, Dimmeler S, Zeiher AM; REPAIR-AMI Investigators (2006). "Intracoronary bone marrow-derived progenitor cells in acute myocardial infarction". N Engl J Med 2006 355 (12): 1210–21. doi:10.1056/NEJMoa060186. PMID 16990384.
- ^ Christman KL, Lee RJ. "Biomaterials for the Treatment of Myocardial Infarction". J Am Coll Cardiol 2006; 48(5): 907–13. PMID 16949479
External links
- American Heart Association's Heart Attack web site – Information and resources for preventing, recognizing and treating heart attack.
- Heart Attack – overview of resources from MedlinePlus
Pathology: hemodynamics Decreases general: Anemic infarct · Hemorrhagic infarct
regional: Myocardial infarction · Cerebral infarction · Splenic infarction · Limb infarctionIncreases general Bruise/Hematoma: Petechia · Purpura · Ecchymosis
regional: head (Epistaxis, Hemoptysis, Intracranial hemorrhage, Hyphema, Subconjunctival hemorrhage) · torso (Hemothorax, Hemopericardium, Pulmonary hematoma) · abdomen (Gastrointestinal bleeding, Haemobilia, Hemoperitoneum, Hematocele, Hematosalpinx ) · joint (Hemarthrosis)general: Anasarca · Angioedema/Lymphedema · Exudate/Transudate
regional: Cerebral edema · Pulmonary edema · Hydrothorax · Ascites/hydroperitoneum · HydrosalpinxOtherCategories:- Aging-associated diseases
- Causes of death
- Ischemic heart diseases
- Medical emergencies
Wikimedia Foundation. 2010.