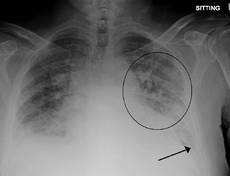
- Pulmonary edema
-
Pulmonary edema Classification and external resources
Pulmonary edema with small pleural effusions on both sides.ICD-10 J81 ICD-9 514 518.4 DiseasesDB 11017 MedlinePlus 000140 eMedicine med/1955 radio/581 MeSH D011654 Pulmonary edema (American English), or oedema (British English; both words from the Greek οἴδημα), is fluid accumulation in the air spaces and parenchyma of the lungs.[1] It leads to impaired gas exchange and may cause respiratory failure. It is due to either failure of the left ventricle of the heart to adequately remove blood from the pulmonary circulation ("cardiogenic pulmonary edema"), see below, or an injury to the lung parenchyma or vasculature of the lung ("noncardiogenic pulmonary edema"), see below.[2] Whilst the range of causes are manifold the treatment options are limited, and to a large extent, the most effective therapies are used whatever the cause. Treatment is focused on three aspects, firstly improving respiratory function, secondly, treating the underlying cause, and thirdly avoiding further damage to the lung. Pulmonary edema, especially in the acute setting, can lead to respiratory failure, cardiac arrest due to hypoxia and death.
Contents
Symptoms and signs
The overwhelming symptom of pulmonary edema is difficulty breathing, but may also include coughing up blood (classically seen as pink, frothy sputum), excessive sweating, anxiety, and pale skin. Shortness of breath can manifest as orthopnea (inability to lie down flat due to breathlessness) and/or paroxysmal nocturnal dyspnea (episodes of severe sudden breathlessness at night), indeed these are common presenting symptoms of chronic pulmonary edema due to left ventricular failure. The chronic development of pulmonary edema may be associated with symptoms and signs of "fluid overload", this is a non specific term to describe the manifestations of left ventricular failure on the rest of the body and includes peripheral edema (swelling of the legs, in general, of the "pitting" variety, wherein the skin is slow to return to normal when pressed upon), raised jugular venous pressure and hepatomegaly, where the liver is enlarged and may be tender or even pulsatile. Other signs include end-inspiratory crackles (sounds heard at the end of a deep breath) on auscultation and the presence of a third heart sound.[2]
Diagnosis
There is no one single test which confirms that breathlessness is caused by pulmonary edema, indeed in many cases the causes of shortness of breath are probably multifactorial.
Low oxygen saturation and disturbed arterial blood gas readings support the proposed diagnosis by suggesting a pulmonary shunt. Chest X-ray will show fluid in the alveolar walls, Kerley B lines, increased vascular shadowing in a classical batwing peri-hilum pattern, upper lobe diversion (increased blood flow to the superior parts of the lung), and possibly pleural effusions.In contrast patchy alveolar infiltrates are more typically associated with noncardiogenic edema[2]
Urgent echocardiography, if available, may strengthen the diagnosis especially in cardiogenic pulmonary edema by demonstrating impaired left ventricular function, high central venous pressures and high pulmonary artery pressures. In certain circumstances insertion of a Swan-Ganz catheter may be required to aid diagnosis.
Blood tests are performed for electrolytes (sodium, potassium) and markers of renal function (creatinine, urea). Liver enzymes, inflammatory markers (usually C-reactive protein) and a complete blood count as well as coagulation studies (PT, aPTT) are typically requested. B-type natriuretic peptide (BNP) is available in many hospitals, sometimes even as a point-of-care test. Low levels of BNP (<100 pg/ml) suggest a cardiac cause is unlikely.[2]
Causes
Pulmonary edema is an accumulation of fluid within the parenchyma and air spaces of the lungs. Classically it is cardiogenic (left ventricular) but fluid may also accumulate due to damage to the lung. This damage may be direct injury or injury mediated by high pressures within the pulmonary circulation. When directly or indirectly caused by increased left ventricular pressure pulmonary edema may form when mean pulmonary pressure rises from the normal of 15 mmHg[3] to above 25 mmHg.[4] Broadly, the causes of pulmonary oedema can be divided into cardiogenic and non-cardiogenic. By convention cardiogenic refers to left ventricular causes.
Cardiogenic
- Left ventricular failure which may be termed Congestive heart failure and may be due to a heart attack leading to left ventricular failure, arrhythmias (tachycardia/fast heartbeat or bradycardia/slow heartbeat) and fluid overload, e.g., from kidney failure or intravenous therapy which may cause dilatation and failure of the left ventricle or may cause pulmonary edema in the absence of heart failure.
Non-cardiogenic
- Hypertensive crisis. The cause of pulmonary edema in the presence of a hypertensive crisis is probably due to a combination of increased pressures in the right ventricle and pulmonary circulation and also increased systemic vascular resistance and left ventricle contractility increasing the hydrostatic pressure within the pulmonary capillaries leading to extravasation of fluid and edema.
- Upper airway obstruction (negative pressure pulmonary edema[5] )
- Neurogenic causes[6] (seizures, head trauma, strangulation, electrocution).
Other/unknown
Injury to the lung may also cause pulmonary oedema through injury to the vasculature and parenchyma of the lung. The acute lung injury-adult respiratory distress syndrome (ALI-ARDS) covers many of these causes, but they may include:
- Inhalation of hot or toxic gases
- Pulmonary contusion, i.e., high-energy trauma
- Aspiration, e.g., gastric fluid
- Reexpansion, i.e. post large volume thoracentesis, resolution of pneumothorax, post decortication, removal of endobronchial obstruction, effectively a form of negative pressure pulmonary oedema.
- Reperfusion injury, i.e. postpulmonary thromboendartectomy or lung transplantation
- Immersion pulmonary edema[7][8]
- Multiple blood transfusions
- Severe infection or inflammation which may be local or systemic. This is the classical form of ALI-ARDS.
There are also a range of causes of pulmonary edema which are less well characterised and arguably represent specific instances of the broader classifications above.
- Arteriovenous malformation
- Hantavirus pulmonary syndrome
- High altitude pulmonary edema (HAPE), probably a manifestation of neurogenic pulmonary edema[9][10]
- Envenomation, such as with the venom of Atrax robustus[11]
Management
Focus is initially on maintaining adequate oxygenation. The patient is given high-flow oxygen, noninvasive ventilation (either continuous positive airway pressure (CPAP) or variable positive airway pressure (VPAP)[12][13]) or mechanical ventilation and positive end-expiratory pressure (PEEP) in very severe cases.
When circulatory causes have led to pulmonary edema, treatment with intravenous nitrates (glyceryl trinitrate), and loop diuretics, such as furosemide or bumetanide, is the mainstay of therapy. These improve both preload and afterload, and aid in improving cardiac function.
Sildenafil is used as a preventative treatment for altitude-induced pulmonary edema and pulmonary hypertension,[14][15] the mechanism of action is via phosphodiesterase inhibition which raises cGMP, resulting in pulmonary arterial vasodialtion and inhibition of smooth muscle cell proliferation.[16] While this effect has only recently been discovered, sildenafil is already becoming an accepted treatment for this condition, in particular in situations where the standard treatment of rapid descent has been delayed for some reason.[17]
See also
- High Altitude Pulmonary Edema
- Flash pulmonary edema
- Swimming Induced Pulmonary Edema
References
- ^ "pulmonary edema" at Dorland's Medical Dictionary
- ^ a b c d Ware LB, Matthay MA. Acute pulmonary edema. N Engl J Med 2005;353:2788-96. PMID 16382065.
- ^ What Is Pulmonary Hypertension? From Diseases and Conditions Index (DCI). National Heart, Lung, and Blood Institute. Last updated September 2008. Retrieved on 6 April 2009.
- ^ Chapter 41, page 210 in: Cardiology secrets By Olivia Vynn Adair Edition: 2, illustrated Published by Elsevier Health Sciences, 2001 ISBN 1560534206, 9781560534204
- ^ Papaioannou, V.; Terzi, I.; Dragoumanis, C.; Pneumatikos, I. (2009). "Negative-pressure acute tracheobronchial hemorrhage and pulmonary edema". Journal of Anesthesia 23 (3): 417–420. doi:10.1007/s00540-009-0757-0. http://www.springerlink.com/content/r7256106w24031lr/.
- ^ O'Leary, R.; McKinlay, J. (2011). "Neurogenic pulmonary oedema". Continuing Education in Anaesthesia, Critical Care & Pain 11 (3): 87–92. doi:10.1093/bjaceaccp/mkr006.
- ^ Hampson NB, Dunford RG (1997). "Pulmonary edema of scuba divers". Undersea Hyperb Med 24 (1): 29–33. PMID 9068153. http://archive.rubicon-foundation.org/2388. Retrieved 2008-09-04.
- ^ Cochard G, Arvieux J, Lacour JM, Madouas G, Mongredien H, Arvieux CC (2005). "Pulmonary edema in scuba divers: recurrence and fatal outcome". Undersea Hyperb Med 32 (1): 39–44. PMID 15796313. http://archive.rubicon-foundation.org/4032. Retrieved 2008-09-04.
- ^ Luks AM (2008). "Do we have a "best practice" for treating high altitude pulmonary edema?". High Alt. Med. Biol. 9 (2): 111–4. doi:10.1089/ham.2008.1017. PMID 18578641.
- ^ Bates, M (2007). "High altitude pulmonary edema". Altitude Physiology Expeditions. http://www.altitude.org/altitude_sickness.php#HAPE. Retrieved 2008-09-04.
- ^ White J, Gray M, Fisher M (1989). Atrax Robustus IPCS InChem
- ^ Masip J, Roque M, Sánchez B, Fernández R, Subirana M, Expósito JA (December 2005). "Noninvasive ventilation in acute cardiogenic pulmonary edema: systematic review and meta-analysis". JAMA 294 (24): 3124–30. doi:10.1001/jama.294.24.3124. PMID 16380593. http://jama.ama-assn.org/cgi/content/full/294/24/3124.
- ^ Peter JV, Moran JL, Phillips-Hughes J, Graham P, Bersten AD (April 2006). "Effect of non-invasive positive pressure ventilation (NIPPV) on mortality in patients with acute cardiogenic pulmonary oedema: a meta-analysis". Lancet 367 (9517): 1155–63. doi:10.1016/S0140-6736(06)68506-1. PMID 16616558.
- ^ Richalet JP, Gratadour P, Robach P, et al. (2005). "Sildenafil inhibits altitude-induced hypoxemia and pulmonary hypertension". Am. J. Respir. Crit. Care Med. 171 (3): 275–81. doi:10.1164/rccm.200406-804OC. PMID 15516532.
- ^ Perimenis P (2005). "Sildenafil for the treatment of altitude-induced hypoxaemia". Expert Opin Pharmacother 6 (5): 835–7. doi:10.1517/14656566.6.5.835. PMID 15934909.
- ^ Clark, Michael; Kumar, Parveen J. (2009). Kumar and Clark's clinical medicine. St. Louis, Mo: Elsevier Saunders. pp. 783. ISBN 0-7020-2993-9.
- ^ Fagenholz PJ, Gutman JA, Murray AF, Harris NS (2007). "Treatment of high altitude pulmonary edema at 4240 m in Nepal". High Alt. Med. Biol. 8 (2): 139–46. doi:10.1089/ham.2007.3055. PMID 17584008.
External links
- HeartFailureMatters.org Animation showing How Heart Failure causes Fluid Accumulation - Created by the European Heart Failure Association
Pathology: hemodynamics Decreases general: Anemic infarct · Hemorrhagic infarct
regional: Myocardial infarction · Cerebral infarction · Splenic infarction · Limb infarctionIncreases general Bruise/Hematoma: Petechia · Purpura · Ecchymosis
regional: head (Epistaxis, Hemoptysis, Intracranial hemorrhage, Hyphema, Subconjunctival hemorrhage) · torso (Hemothorax, Hemopericardium, Pulmonary hematoma) · abdomen (Gastrointestinal bleeding, Haemobilia, Hemoperitoneum, Hematocele, Hematosalpinx ) · joint (Hemarthrosis)general: Anasarca · Angioedema/Lymphedema · Exudate/Transudate
regional: Cerebral edema · Pulmonary edema · Hydrothorax · Ascites/hydroperitoneum · HydrosalpinxOtherCategories:- Respiratory diseases principally affecting the interstitium
- Medical emergencies
Wikimedia Foundation. 2010.