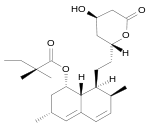
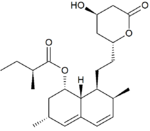- Statin
-
This article is about the group of cholesterol lowering drugs. For the amino acid, see Statine.
Statins (or HMG-CoA reductase inhibitors) are a class of drugs used to lower cholesterol levels by inhibiting the enzyme HMG-CoA reductase, which plays a central role in the production of cholesterol in the liver. Increased cholesterol levels have been associated with cardiovascular diseases (CVD),[1] and statins are therefore used in the prevention of these diseases. Randomized controlled trials have shown that they are most effective in those with cardiovascular disease (secondary prevention), with questionable benefit in those without previous CVD but with elevated cholesterol levels.[2][3] Statins have rare but severe adverse effects, particularly muscle damage, and some doctors believe they are overprescribed.
The best-selling of the statins is atorvastatin, marketed as Lipitor and manufactured by Pfizer. By 2003 it had become the best-selling pharmaceutical in history,[4] with Pfizer reporting sales of US$12.4 billion in 2008.[5] As of 2010, a number of statins are on the market: atorvastatin (Lipitor and Torvast), fluvastatin (Lescol), lovastatin (Mevacor, Altocor, Altoprev), pitavastatin (Livalo, Pitava), pravastatin (Pravachol, Selektine, Lipostat), rosuvastatin (Crestor) and simvastatin (Zocor, Lipex).[6] Several combination preparations of a statin and another agent—such as ezetimibe/simvastatin, sold as Vytorin—are also available.
Contents
Medical uses
Clinical practice guidelines generally recommend that the people have tried "lifestyle modification", including a cholesterol-lowering diet and physical exercise, before statin use is considered; statins or other pharmacologic agents may then be recommended for those who do not meet their lipid-lowering goals through diet and lifestyle approaches.[7][8]
Primary prevention
A 2010 meta-analysis of studies found no benefit in terms of all-cause mortality when statins were used as a high-risk primary prevention intervention[9] and a 2011 review found little evidence of improved quality of life and questionable cost effectiveness when used for primary prevention.[3]
Secondary prevention
Statins are effective in decreasing mortality in people with preexisting cardiovascular disease. They are also currently advocated for use in patients at high risk of developing heart disease.[2] On average, statins can lower LDL cholesterol by 1.8 mmol/l (70 mg/dl), which translates into a 60% decrease in the number of cardiac events (heart attack, sudden cardiac death) and a 17% reduced risk of stroke after long-term treatment.[10] They have less effect than the fibrates or niacin in reducing triglycerides and raising HDL-cholesterol ("good cholesterol").
Comparative effectiveness
No large scale comparison exists that examines the relative effectiveness of the various statins against one another for preventing hard cardiovascular outcomes, such as death or myocardial infarction.
An independent analysis has been done to compare atorvastatin, pravastatin and simvastatin, based on their effectiveness against placebos. It found that, at commonly prescribed doses, there are no statistically significant differences amongst statins in reducing cardiovascular morbidity and mortality.[11] The CURVES study, which compared the efficacy of different doses of atorvastatin, simvastatin, pravastatin, lovastatin, and fluvastatin for reducing LDL and total cholesterol in patients with hypercholesterolemia, found that atorvastatin was more effective without increasing adverse events.[12]
Statins differ in their ability to reduce cholesterol levels. Doses should be individualized according to patient characteristics such as goal of therapy and response. After initiation and/or dose changes, lipid levels should be analyzed within 1–3 months and dosage adjusted accordingly, then every 6–12 months afterwards. [13] [14] [15] [16]
Statin Equivalent Dosages % LDL Reduction (approx.) Atorvastatin Fluvastatin Lovastatin Pravastatin Rosuvastatin Simvastatin 10-20% -- 20 mg 10 mg 10 mg -- 5 mg 20-30% -- 40 mg 20 mg 20 mg -- 10 mg 30-40% 10 mg 80 mg* 40 mg 40 mg 5 mg 20 mg 40-45% 20 mg -- 80 mg* 80 mg* 5–10 mg 40 mg 46-50% 40 mg -- -- -- 10–20 mg 80 mg* 50-55% 80 mg -- -- -- 20 mg -- 56-60% -- -- -- -- 40 mg -- * 80mg dose no longer recommended due to increased risk of rhabdomyolysis Starting dose Starting dose 10–20 mg 20 mg 10–20 mg 40 mg 10 mg; 5 mg if hypothyroid, >65 yo, Asian 20 mg If higher LDL reduction goal 40 mg if >45% 40 mg if >25% 20 mg if >20% -- 20 mg if LDL >190 mg/dL (4.87 mmol/L) 40 mg if >45% Optimal timing Anytime Evening With evening meals Anytime Anytime Evening Adverse effects
The most common adverse side effects are raised liver enzymes and muscle problems. In randomized clinical trials, reported adverse effects are low; but they are "higher in studies of real world use", and more varied.[17] In randomized trials statins increased the risk of an adverse effect by 39% compared to placebo (odds ratios 1.4); two-thirds of these were myalgia or raised liver enzymes with serious adverse effects similar to placebo.[18] However, reliance on clinical trials can be misleading indications of real-world adverse effects – for example, the statin cerivastatin was withdrawn from the market in 2001 due to cases of rhabdomyolysis (muscle breakdown), although rhabdomyolysis did not occur in a meta-analysis of cerivastatin clinical trials.[17] Other possible adverse effects include cognitive loss, neuropathy, pancreatic and hepatic dysfunction, and sexual dysfunction.[17]
Some patients on statin therapy report myalgias,[19] muscle cramps,[19] or, less frequently, gastrointestinal or other symptoms. Liver enzyme derangements may also occur, typically in about 0.5%,[citation needed] are also seen at similar rates with placebo use and repeated enzyme testing, and generally return to normal either without discontinuance over time or after briefly discontinuing the drug. Multiple other side-effects occur rarely; typically also at similar rates with only placebo in the large statin safety/efficacy trials. Two randomized clinical trials found cognitive issues while two did not; recurrence upon reintroduction suggests that these are causally related to statins in some individuals.[20] A Danish case-control study published in 2002 suggested a relation between long term statin use and increased risk of nerve damage or polyneuropathy[21] but suggested this side effect is "rare, but it does occur";[22] other researchers have pointed to studies of the effectiveness of statins in trials involving 50,000 people which have not shown nerve damage as a significant side effect.[23]
Rare reactions include myositis and myopathy, with the potential for rhabdomyolysis (the pathological breakdown of skeletal muscle) leading to acute renal failure. Coenzyme Q10 (ubiquinone) levels are decreased in statin use;[24] Q10 supplements are sometimes used to treat statin-associated myopathy, though there was no evidence of their effectiveness as of 2007[update].[25] A common variation in the SLCO1B1 gene, which participates in the absorption of statins, has been shown to significantly increase the risk of myopathy.[26]
Graham et al. (2004) reviewed records of over 250,000 patients treated from 1998 to 2001 with the statin drugs atorvastatin, cerivastatin, fluvastatin, lovastatin, pravastatin, and simvastatin.[27] The incidence of rhabdomyolyis was 0.44 per 10,000 patients treated with statins other than cerivastatin. However, the risk was over tenfold greater if cerivastatin was used, or if the standard statins (atorvastatin, fluvastatin, lovastatin, pravastatin, simvastatin) were combined with fibrate (fenofibrate or gemfibrozil) treatment. Cerivastatin was withdrawn by its manufacturer in 2001.
All commonly used statins show somewhat similar results, however the newer statins, characterized by longer pharmacological half-lives and more cellular specificity, have had a better ratio of efficacy to lower adverse effect rates.[citation needed] Some researchers have suggested that hydrophilic statins such as fluvastatin, rosuvastatin, and pravastatin are less toxic than lipophilic statins such as atorvastatin, lovastatin, and simvastatin, but other studies have not found a connection;[28] it is suggested that the risk of myopathy is lowest with pravastatin and fluvastatin probably because they are more hydrophillic and as a result have less muscle penetration.[citation needed] Lovastatin induces the expression of gene atrogin-1, which is believed to be responsible in promoting muscle fiber damage.[28]
Although there have been concerns that statins might increase cancer, several meta-analyses have found no relationship to cancer, the largest of which as of 2006 included nearly 87,000 participants.[29] However, in 2007 a meta-analysis of 23 statin treatment arms with 309,506 person-years of follow-up found that the risk of cancer was significantly associated with lower achieved LDL-C levels; the authors say that this requires further investigation.[30]
Several case-control studies have found that statins reduce cancer incidence,[29] including one[31] which showed that patients taking statins for over 5 years reduced their risk of colorectal cancer by 50%; this effect was not exhibited by fibrates although the trialists warned that the number needed to treat would approximate 5000, making statins unlikely tools for primary prevention.[31]
Drug interactions
Combining any statin with a fibrate or niacin, another category of lipid-lowering drugs, increases the risks for rhabdomyolysis to almost 6.0 per 10,000 person-years.[27] Most physicians have now abandoned routine monitoring of liver enzymes and creatine kinase, although they still consider this prudent in those on high-dose statins or in those on statin/fibrate combinations, and mandatory in the case of muscle cramps or of deterioration in renal function.
Consumption of grapefruit or grapefruit juice inhibits the metabolism of statins. Bitter oranges may have a similar effect.[32] Furanocoumarins in grapefruit juice (i.e. bergamottin and dihydroxybergamottin) inhibit the cytochrome P450 enzyme CYP3A4, which is involved in the metabolism of most statins (however it is a major inhibitor of only lovastatin, simvastatin and to a lesser degree atorvastatin) and some other medications[33] (it had been thought that flavonoids (i.e. naringin) were responsible). This increases the levels of the statin, increasing the risk of dose-related adverse effects (including myopathy/rhabdomyolysis). An alternative, somewhat risky, approach is that some users take grapefruit juice to enhance the effect of lower (hence cheaper) doses of statins; this increases risk and the potential for statin toxicity.
Mechanism of action
 The HMG-CoA reductase pathway, which is blocked by statins via inhibiting the rate limiting enzyme HMG-CoA reductase.
The HMG-CoA reductase pathway, which is blocked by statins via inhibiting the rate limiting enzyme HMG-CoA reductase.
Statins act by competitively inhibiting HMG-CoA reductase, the first committed enzyme of the HMG-CoA reductase pathway. Because statins are similar to HMG-CoA on a molecular level they take the place of HMG-CoA in the enzyme and reduce the rate by which it is able to produce mevalonate, the next molecule in the cascade that eventually produces cholesterol, as well as a number of other compounds. This ultimately reduces cholesterol via several mechanisms.
Inhibiting cholesterol synthesis
By inhibiting HMG-CoA reductase, statins block the pathway for synthesizing cholesterol in the liver. This is significant because most circulating cholesterol comes from internal manufacture rather than the diet. When the liver can no longer produce cholesterol, levels of cholesterol in the blood will fall. Cholesterol synthesis appears to occur mostly at night,[34] so statins with short half-lives are usually taken at night to maximize their effect. Studies have shown greater LDL and total cholesterol reductions in the short-acting simvastatin taken at night rather than the morning,[35][36] but have shown no difference in the long-acting atorvastatin.[37]
Increasing LDL uptake
Liver cells sense the reduced levels of liver cholesterol and seek to compensate by synthesizing LDL receptors to draw cholesterol out of the circulation.[38] This is accomplished via protease enzymes that cleave a protein called "membrane-bound sterol regulatory element binding protein", which migrates to the nucleus and causes increased production of various other proteins and enzymes, including the LDL receptor. The LDL receptor then relocates to the liver cell membrane and binds to passing LDL and VLDL particles (the "bad cholesterol" linked to disease). LDL and VLDL are drawn out of circulation into the liver where the cholesterol is reprocessed into bile salts. These are excreted, and subsequently recycled mostly by an internal bile salt circulation.
Other effects
Statins exhibit action beyond lipid-lowering activity in the prevention of atherosclerosis. The ASTEROID trial showed direct ultrasound evidence of atheroma regression during statin therapy.[39] Researchers hypothesize that statins prevent cardiovascular disease via four proposed mechanisms (all subjects of a large body of biomedical research):[40]
- Improve endothelial function
- Modulate inflammatory responses
- Maintain plaque stability
- Prevent thrombus formation
Statins may even benefit those without high cholesterol. In 2008 the JUPITER study showed fewer stroke, heart attacks, and surgeries even for patients who had no history of high cholesterol or heart disease, but only elevated C-reactive protein levels. There were also 20% fewer deaths (mainly from reduction in cancer deaths) though deaths from cardiovascular causes were not reduced.[41]
Click on genes, proteins and metabolites below to link to respective articles.[42]
Pharmacogenomics
A 2004 study showed that patients with one of two common single-nucleotide polymorphisms (SNP) (small genetic variations) in the HMG-CoA reductase gene were less responsive to statins.[43] A 2008 study showed that carriers of the KIF6 genetic mutation were more responsive to statin treatment.[44]
Likewise, a 2008 study demonstrated a link between an increased risk of myopathy at higher doses of statins (40 – 80 mg) and a SNP in SLCO1B1, a gene encoding for the organic anion transporter peptide OADP1B1.[45]
History
In 1971, Akira Endo, a Japanese biochemist working for the drug company Sankyo, began the search for a cholesterol-lowering drug. Research had already shown that cholesterol is mostly manufactured by the body in the liver, using an enzyme known as HMG-CoA reductase.[4] Endo and his team reasoned that certain microorganisms may produce inhibitors of the enzyme to defend themselves against other organisms, as mevalonate is a precursor of many substances required by organisms for the maintenance of their cell wall (ergosterol) or cytoskeleton (isoprenoids).[46] The first agent they identified was mevastatin (ML-236B), a molecule produced by the fungus Penicillium citrinum.
Mevastatin was never marketed, because of its adverse effects of tumors, muscle deterioration, and sometimes death in laboratory dogs. P. Roy Vagelos, chief scientist and later CEO of Merck & Co, was interested, and made several trips to Japan starting in 1975. By 1978, Merck had isolated lovastatin (mevinolin, MK803) from the fungus Aspergillus terreus, first marketed in 1987 as Mevacor.[4]
A link between cholesterol and cardiovascular disease, known as the lipid hypothesis, had already been suggested. Cholesterol is the main constituent of atheroma, the fatty lumps in the wall of arteries that occur in atherosclerosis and, when ruptured, cause the vast majority of heart attacks. Treatment consisted mainly of dietary measures such as a low-fat diet, and poorly tolerated medicines such as clofibrate, cholestyramine and nicotinic acid. Cholesterol researcher Daniel Steinberg writes that while the Coronary Primary Prevention Trial of 1984 demonstrated that cholesterol lowering could significantly reduce the risk of heart attacks and angina, physicians, including cardiologists, remained largely unconvinced.[47]
To market statins effectively, Merck had to convince the public about the dangers of high cholesterol, and doctors that statins were safe and would extend lives. As a result of public campaigns, people became familiar with their cholesterol numbers and the difference between "good" and "bad" cholesterol, and rival pharmaceutical companies began producing their own statins, such as pravastatin (Pravachol), manufactured by Sankyo and Bristol-Myers Squibb. In April 1994, the results of a Merck-sponsored study, the Scandinavian Simvastatin Survival Study or "4S", were announced. Researchers tested simvastatin, later sold by Merck as Zocor, on 4,444 patients with high cholesterol and heart disease. After five years, the study concluded that patients saw a 35-percent reduction in their cholesterol, and their chances of dying of a heart attack were reduced by 42 percent.[4][48] In 1995, Zocor and Mevacor both made Merck over US$1 billion.[4] Endo was awarded the 2006 Japan Prize, and the Lasker-DeBakey Clinical Medical Research Award in 2008.
Available forms
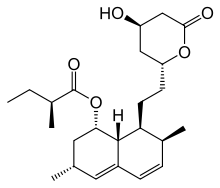
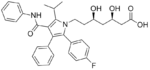
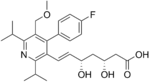
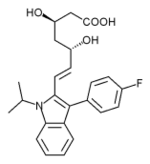
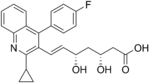
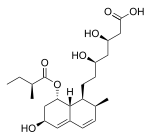
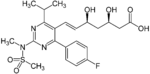
The statins are divided into two groups: fermentation-derived and synthetic. They include, along with brand names, which may vary between countries:
Statin Image Brand name Derivation Metabolism[49] Atorvastatin Lipitor, Torvast Synthetic CYP3A4 Cerivastatin Lipobay, Baycol. (Withdrawn from the market in August, 2001 due to risk of serious Rhabdomyolysis) Synthetic various CYP3A isoforms [50] Fluvastatin Lescol, Lescol XL Synthetic CYP2C9 Lovastatin Mevacor, Altocor, Altoprev Fermentation-derived. Naturally-occurring compound. Found in oyster mushrooms and red yeast rice. CYP3A4 Mevastatin Compactin Naturally-occurring compound. Found in red yeast rice. CYP3A4 Pitavastatin Livalo, Pitava Synthetic Pravastatin Pravachol, Selektine, Lipostat Fermentation-derived. (A fermentation product of bacterium Nocardia autotrophica). Non CYP[51] Rosuvastatin Crestor Synthetic CYP2C9 and CYP2C19 Simvastatin Zocor, Lipex Fermentation-derived. (Simvastatin is a synthetic derivate of a fermentation product ofAspergillus terreus.) CYP3A4 Simvastatin+Ezetimibe Vytorin Combination therapy Lovastatin+Niacin extended-release Advicor Combination therapy Atorvastatin+Amlodipine Besylate Caduet Combination therapy - Cholesterol+Blood Pressure Simvastatin+Niacin extended-release Simcor Combination therapy LDL-lowering potency varies between agents. Cerivastatin is the most potent, (withdrawn from the market in August, 2001 due to risk of serious Rhabdomyolysis) followed by (in order of decreasing potency), rosuvastatin, atorvastatin, simvastatin, lovastatin, pravastatin, and fluvastatin.[52] The relative potency of pitavastatin has not yet been fully established.
Some types of statins are naturally occurring, and can be found in such foods as oyster mushrooms and red yeast rice. Randomized controlled trials found them to be effective, but the quality of the trials was low.[53] Most of the block-buster branded statins will be generic by 2012,including atorvastatin, the largest selling branded drug.
Research
Research continues into other areas where statins also appear to have a favorable effect, including dementia,[54] lung cancer,[55]nuclear cataracts,[56] hypertension,[57] prostate cancer [58]
Controversy
Some scientists believe that statins are overused. Their use has expanded into groups with lesser benefit, and lesser evidence of benefit. The lower the risk of cardiovascular events, the lower the ratio is of benefits to costs.[59]
A smaller group of scientists, The International Network of Cholesterol Skeptics, question the lipid hypothesis and argue that elevated cholesterol has not been adequately linked to heart disease. These organizations maintain that statins are not as beneficial or safe as suggested.[60]
References
- ^ Lewington S, Whitlock G, Clarke R, et al. (December 2007). "Blood cholesterol and vascular mortality by age, sex, and blood pressure: a meta-analysis of individual data from 61 prospective studies with 55,000 vascular deaths". Lancet 370 (9602): 1829–39. doi:10.1016/S0140-6736(07)61778-4. PMID 18061058.
- ^ a b National Institute for Health and Clinical Excellence (May 2008, reissued March 2010). "Lipid modification - Cardiovascular risk assessment and the modification of blood lipids for the primary and secondary prevention of cardiovascular disease - Quick reference guide" (PDF). http://www.nice.org.uk/nicemedia/live/11982/40675/40675.pdf. Retrieved 2010-08-25.
- ^ a b Taylor, F; Ward, K, Moore, TH, Burke, M, Davey Smith, G, Casas, JP, Ebrahim, S (2011 Jan 19). "Statins for the primary prevention of cardiovascular disease.". Cochrane database of systematic reviews (Online) (1): CD004816. doi:10.1002/14651858.CD004816.pub4. PMID 21249663.
- ^ a b c d e Simons, John. "The $10 billion pill", Fortune magazine, January 20, 2003.
- ^ "Doing Things Differently", Pfizer 2008 Annual Review, April 23, 2009, p. 15.
- ^ Sweetman, Sean C., ed (2009). "Cardiovascular drugs". Martindale: the complete drug reference (36th ed.). London: Pharmaceutical Press. pp. 1155–434. ISBN 978-0-85369-840-1.
- ^ National Cholesterol Education Program (2001). Third Report of the National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III): Executive Summary. Bethesda, MD: National Institutes of Health. National Heart, Lung, and Blood Institute.. pp. 40. NIH Publication No. 01-3670.
- ^ National Collaborating Centre for Primary Care (2010) (PDF). NICE clinical guideline 67: Lipid modification. London: National Institute for Health and Clinical Excellence. pp. 38. http://www.nice.org.uk/nicemedia/live/11982/40689/40689.pdf.
- ^ Ray KK, Seshasai SR, Erqou S, et al. (June 2010). "Statins and all-cause mortality in high-risk primary prevention: a meta-analysis of 11 randomized controlled trials involving 65,229 participants". Arch Intern Med 170 (12): 1024–31. doi:10.1001/archinternmed.2010.182. PMID 20585067.
- ^ Law MR, Wald NJ, Rudnicka AR (June 2003). "Quantifying effect of statins on low density lipoprotein cholesterol, ischaemic heart disease, and stroke: systematic review and meta-analysis". BMJ 326 (7404): 1423. doi:10.1136/bmj.326.7404.1423. PMC 162260. PMID 12829554. http://www.bmj.com/cgi/content/full/326/7404/1423.
- ^ Zhou Z, Rahme E, Pilote L (2006). "Are statins created equal? Evidence from randomized trials of pravastatin, simvastatin, and atorvastatin for cardiovascular disease prevention". Am. Heart J. 151 (2): 273–81. doi:10.1016/j.ahj.2005.04.003. PMID 16442888.
- ^ Jones P, Kafonek S, Laurora I, Hunninghake D (1998). "Comparative dose efficacy study of atorvastatin versus simvastatin, pravastatin, lovastatin, and fluvastatin in patients with hypercholesterolemia (the CURVES study)". Am J Cardiol 81 (5): 582–7. doi:10.1016/S0002-9149(97)00965-X. PMID 9514454.
- ^ Ryan Oftebro, PharmD. HMG-CoA Reductase Inhibitors (“Statins”): Clinical Pearls for Washington Rx Therapeutic Interchange Program (TIP). Accessed 2009-11-22.
- ^ Common Medication Conversions (Equivalents): Statins (HMG-CoA Reductase Inhibitors) GlobalRPh.com. Accessed 2009-11-22.
- ^ Treating Elevated Cholesterol and Heart Disease: The Statins. Consumer Reports Health Best Buy Drugs. February 2007
- ^ Dosage information including FDA approved labels (package inserts) from DailyMed United States National Library of Medicine.
- ^ a b c Golomb BA, Evans MA (2008). "Statin adverse effects : a review of the literature and evidence for a mitochondrial mechanism". Am J Cardiovasc Drugs 8 (6): 373–418. doi:10.2165/0129784-200808060-00004. PMC 2849981. PMID 19159124. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=2849981.
- ^ Silva MA, Swanson AC, Gandhi PJ, Tataronis GR (January 2006). "Statin-related adverse events: a meta-analysis". Clin Ther 28 (1): 26–35. doi:10.1016/j.clinthera.2006.01.005. PMID 16490577.
- ^ a b Anne Harding (August 28, 2007). "Docs often write off patient side effect concerns". Reuters. http://www.reuters.com/article/healthNews/idUSCOL86315820070828. Retrieved 2009-10-06.
- ^ Holman JR. (2007). Some Docs in Denial About Statin Side Effects. Doc News.
- ^ Gaist D, Jeppesen U, Andersen M, García Rodríguez LA, Hallas J, Sindrup SH (2002). "Statins and risk of polyneuropathy—a case-control study". Neurology 58 (9): 1333–1337. PMID 12011277. http://www.neurology.org/cgi/content/abstract/58/9/1333. Lay summary – USA Today (2002-08-20).
- ^ Sandra G. Boodman, The Washington Post (September 10, 2002). "Study links statins to nerve damage". Pittsburgh Post-Gazette. http://www.post-gazette.com/healthscience/20020910hstatins3.asp. Retrieved 2009-10-06.
- ^ Julie Appleby and Steve Sternberg (2002-08-18). "Statin side effect rare, but be aware". USA TODAY. http://www.usatoday.com/money/markets/2002-08-18-statin-effect_x.htm. Retrieved 2009-10-06.
- ^ Ghirlanda G, Oradei A, Manto A, Lippa S, Uccioli L, Caputo S, Greco A, Littarru G (1993). "Evidence of plasma CoQ10-lowering effect by HMG-CoA reductase inhibitors: a double-blind, placebo-controlled study". J Clin Pharmacol 33 (3): 226–9. PMID 8463436.
- ^ Marcoff L, Thompson PD (2007). "The role of coenzyme Q10 in statin-associated myopathy: a systematic review". J. Am. Coll. Cardiol. 49 (23): 2231–7. doi:10.1016/j.jacc.2007.02.049. PMID 17560286.
- ^ Search Collaborative, Group; Link, E; Parish, S; Armitage, J; Bowman, L; Heath, S; Matsuda, F; Gut, I et al. (July 2008). "SLCO1B1 Variants and Statin-Induced Myopathy -- A Genomewide Study". N. Engl. J. Med. Online (8): 789–99. doi:10.1056/NEJMoa0801936. PMID 18650507. http://content.nejm.org/cgi/content/full/NEJMoa0801936v1.
- ^ a b Graham DJ, Staffa JA, Shatin D, et al. (2004). "Incidence of hospitalized rhabdomyolysis in patients treated with lipid-lowering drugs". JAMA 292 (21): 2585–90. doi:10.1001/jama.292.21.2585. PMID 15572716. http://jama.ama-assn.org/cgi/content/full/292/21/2585.
- ^ a b Hanai J, Cao P, Tanksale P, et al. (2007). "The muscle-specific ubiquitin ligase atrogin-1/MAFbx mediates statin-induced muscle toxicity". J. Clin. Invest. 117 (12): 3940–51. doi:10.1172/JCI32741. PMC 2066198. PMID 17992259. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=2066198.
- ^ a b Dale KM, Coleman CI, Henyan NN, Kluger J, White CM (2006). "Statins and cancer risk: a meta-analysis". JAMA 295 (1): 74–80. doi:10.1001/jama.295.1.74. PMID 16391219. http://jama.ama-assn.org/cgi/content/full/295/1/74.
- ^ Alsheikh-Ali AA; Maddukuri, PV; Han, H; Karas, RH (2007). "Effect of the Magnitude of Lipid Lowering on Risk of Elevated Liver Enzymes, Rhabdomyolysis, and Cancer: Insights From Large Randomized Statin Trials". Journal of the American College of Cardiology 50 (5): 409–418. doi:10.1016/j.jacc.2007.02.073. PMID 17662392.
- ^ a b Poynter JN, Gruber SB, Higgins PD, et al. (2005). "Statins and the risk of colorectal cancer". N. Engl. J. Med. 352 (21): 2184–92. doi:10.1056/NEJMoa043792. PMID 15917383. http://content.nejm.org/cgi/content/full/352/21/2184.
- ^ Mayo clinic: article on interference between grapefruit and medication
- ^ Kane GC, Lipsky JJ (2000). "Drug-grapefruit juice interactions". Mayo Clin. Proc. 75 (9): 933–42. doi:10.4065/75.9.933. PMID 10994829.
- ^ Miettinen TA (March 1982). "Diurnal variation of cholesterol precursors squalene and methyl sterols in human plasma lipoproteins". Journal of Lipid Research 23 (3): 466–73. PMID 7200504. http://www.jlr.org/cgi/content/abstract/23/3/466.
- ^ Saito Y; Yoshida S; Nakaya N; Hata Y; Goto Y (Jul-Aug 1991). "Comparison between morning and evening doses of simvastatin in hyperlipidemic subjects. A double-blind comparative study". Arterioscler Thromb 11 (4): 816–26. PMID 2065035.
- ^ Wallace A; Chinn D; Rubin G (4 October 2003). "Taking simvastatin in the morning compared with in the evening: randomised controlled trial". British Medical Journal 327 (7418): 788. doi:10.1136/bmj.327.7418.788. PMID 14525878.
- ^ Cilla DD Jr; Gibson DM; Whitfield LR; Sedman AJ (July 1996). "Pharmacodynamic effects and pharmacokinetics of atorvastatin after administration to normocholesterolemic subjects in the morning and evening". Journal of Clinical Pharmacology 36 (7): 604–9. PMID 8844442.
- ^ Ma PT, Gil G, Südhof TC, Bilheimer DW, Goldstein JL, Brown MS (1986). "Mevinolin, an inhibitor of cholesterol synthesis, induces mRNA for low density lipoprotein receptor in livers of hamsters and rabbits" (PDF). Proc. Natl. Acad. Sci. U.S.A. 83 (21): 8370–4. Bibcode 1986PNAS...83.8370M. doi:10.1073/pnas.83.21.8370. PMC 386930. PMID 3464957. http://www.pnas.org/cgi/reprint/83/21/8370.
- ^ Nissen S, Nicholls S, Sipahi I, Libby P, Raichlen J, Ballantyne C, Davignon J, Erbel R, Fruchart J, Tardif J, Schoenhagen P, Crowe T, Cain V, Wolski K, Goormastic M, Tuzcu E (2006). "Effect of very high-intensity statin therapy on regression of coronary atherosclerosis: the ASTEROID trial". JAMA 295 (13): 1556–65. doi:10.1001/jama.295.13.jpc60002. PMID 16533939. http://jama.ama-assn.org/cgi/content/full/295/13/1556.
- ^ Furberg CD (19 January 1999). "Natural Statins and Stroke Risk". Circulation 99 (2): 185–188. PMID 9892578. http://circ.ahajournals.org/cgi/content/full/99/2/185.
- ^ Ridker PM, Danielson E, Fonseca FAH, et al. (2008). "Rosuvastatin to prevent vascular events in men and women with elevated C-reactive protein". NEJM 359 (21): 2195–207. doi:10.1056/NEJMoa0807646. PMID 18997196. http://content.nejm.org/cgi/reprint/NEJMoa0807646v1.pdf.
- ^ The interactive pathway map can be edited at WikiPathways: "StatinPathway_WP430". http://www.wikipathways.org/index.php/Pathway:WP430.
- ^ Chasman DI, Posada D, Subrahmanyan L, Cook NR, Stanton VP, Ridker PM (2004). "Pharmacogenetic study of statin therapy and cholesterol reduction". JAMA 291 (23): 2821–7. doi:10.1001/jama.291.23.2821. PMID 15199031. http://jama.ama-assn.org/cgi/content/full/291/23/2821.
- ^ Iakoubova, O. A.; Sabatine, M. S.; Rowland, C. M.; Tong, C. H.; Catanese, J. J.; Ranade, K.; Simonsen, K. L.; Kirchgessner, T. G. et al. (2008). "Polymorphism in KIF6 Gene and Benefit from Statins After Acute Coronary Syndromes: Results from the PROVE IT-TIMI 22 Study". Journal of the American College of Cardiology 51 (4): 449–55. doi:10.1016/j.jacc.2007.10.017. PMID 18222355.
- ^ The SEARCH Collaborative Group (2008). "SLCO1B1 Variants and Statin-Induced Myopathy - A Genomewide Study". NEJM 359: 789–799. doi:10.1056/NEJMoa0801936. PMID 18650507. http://www.nejm.org/doi/pdf/10.1056/NEJMoa0801936.
- ^ Endo A (1 November 1992). "The discovery and development of HMG-CoA reductase inhibitors" (PDF). J. Lipid Res. 33 (11): 1569–82. PMID 1464741. http://www.jlr.org/cgi/reprint/33/11/1569.
- ^ Steinberg, Daniel. The Cholesterol Wars: The Skeptics vs. The Preponderance of Evidence. Academic Press, 2007, pp. 6–9.
- ^ "Randomised trial of cholesterol lowering in 4444 patients with coronary heart disease: the Scandinavian Simvastatin Survival Study (4S)". Lancet 344 (8934): 1383–9. November 1994. doi:10.1016/S0140-6736(94)90566-5. PMID 7968073.
- ^ Safety of Statins: Focus on Clinical Pharmacokinetics and Drug Interactions. Circulation. 2004:109:III-50-IIIi-57
- ^ Metabolism of cerivastatin by human liver microsomes in vitro. Characterization of primary metabolic pathways and of cytochrome P450 isozymes involved. Drug Metab Dispos. 1997 Mar;25(3):321-31.
- ^ Comparison of Cytochrome P-450-Dependent Metabolism and Drug Interactions of the 3-Hydroxy-3-methylglutaryl-CoA Reductase Inhibitors Lovastatin and Pravastatin in the Liver. DMD February 1, 1999 vol. 27 no. 2 173-179
- ^ Shepherd J, Hunninghake DB, Barter P, McKenney JM, Hutchinson HG (2003). "Guidelines for lowering lipids to reduce coronary artery disease risk: a comparison of rosuvastatin with atorvastatin, pravastatin, and simvastatin for achieving lipid-lowering goals". Am. J. Cardiol. 91 (5A): 11C–17C; discussion 17C–19C. doi:10.1016/S0002-9149(03)00004-3. PMID 12646338.
- ^ Liu J, Zhang J, Shi Y, Grimsgaard S, Alraek T, Fønnebø V (2006). "Chinese red yeast rice (Monascus purpureus) for primary hyperlipidemia: a meta-analysis of randomized controlled trials". Chin Med 1: 4. doi:10.1186/1749-8546-1-4. PMC 1761143. PMID 17302963. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=1761143.
- ^ Wolozin, B; Wang SW, Li NC, Lee A, Lee TA, Kazis LE (July 19, 2007). "Simvastatin is associated with a reduced incidence of dementia and Parkinson's disease". BMC Medicine 5: 20. doi:10.1186/1741-7015-5-20. PMC 1955446. PMID 17640385. http://www.biomedcentral.com/1741-7015/5/20.
- ^ Khurana V, Bejjanki HR, Caldito G, Owens MW (May 2007). "Statins reduce the risk of lung cancer in humans: a large case-control study of US veterans". Chest 131 (5): 1282–1288. doi:10.1378/chest.06-0931. PMID 17494779. http://www.chestjournal.org/cgi/content/full/131/5/1282.
- ^ Klein BE, Klein R, Lee KE, Grady LM (June 2006). "Statin use and incident nuclear cataract". JAMA 295 (23): 2752–8. doi:10.1001/jama.295.23.2752. PMID 16788130. http://jama.ama-assn.org/cgi/content/full/295/23/2752.
- ^ Golomb BA, Dimsdale JE, White HL, Ritchie JB, Criqui MH (April 2008). "Reduction in blood pressure with statins: results from the UCSD Statin Study, a randomized trial". Arch. Intern. Med. 168 (7): 721–7. doi:10.1001/archinte.168.7.721. PMID 18413554.
- ^ Mondul AM, Han M, Humphreys EB, Meinhold CL, Walsh PC, Platz EA (February 2011). "Association of statin use with pathological tumor characteristics and prostate cancer recurrence after surgery". Journal of Urology 185 (4): 1268–1273. doi:10.1016/j.juro.2010.11.089. PMID 21334020.
- ^ Abramson J, Wright J (2007). "Are lipid-lowering guidelines evidence-based?". Lancet 369 (9557): 168–9. doi:10.1016/S0140-6736(07)60084-1. PMID 17240267.
- ^ Ravnskov U, Rosch P, Sutter M, Houston M (2006). "Should we lower cholesterol as much as possible?". BMJ 332 (7553): 1330–2. doi:10.1136/bmj.332.7553.1330. PMC 1473073. PMID 16740566. http://www.bmj.com/cgi/content/full/332/7553/1330.
External links
- Statin page at Bandolier, an evidence-based medicine journal (little content after 2004)
Lipid modifying agents (C10) GI tract Liver Simvastatin# • Atorvastatin • Fluvastatin • Lovastatin • Mevastatin • Pitavastatin • Pravastatin • Rosuvastatin • Cerivastatin‡Blood vessels Combinations Other Dextrothyroxine • Probucol • Tiadenol • Benfluorex • Meglutol • Omega-3-triglycerides • Magnesium pyridoxal 5-phosphate glutamate • Policosanol • Lapaquistat§ • Alipogene tiparvovecPharmacology: enzyme inhibition Class Substrate 1.1 Aldose reductase · HMG-CoA reductase
1.13 Lipoxygenase
1.17 Xanthine oxidase · Ribonucleotide reductase2.1 COMT · Thymidylate synthase
2.4 PARP
2.5 Dihydropteroate synthetase · Farnesyltransferase
2.6 GABA transaminase
2.7 Nucleotidyltransferase (Integrase, Reverse transcriptase) · Protein kinase (Tyrosine-kinase (Janus kinase))3.1 Phosphodiesterase · Acetylcholinesterase · Ribonuclease
3.2 Polygalacturonase · Neuraminidase · Alpha-glucosidase
3.4 Protease: Exopeptidase (Dipeptidyl peptidase-4, ACE) · Endopeptidase (Trypsin, Renin, Matrix metalloproteinase)
3.5 Histone deacetylase · Beta-lactamase4.1 Dopa decarboxylase
4.2 Carbonic anhydraseCategories:- Statins
Wikimedia Foundation. 2010.