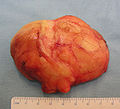
- Lipoma
-
Lipoma Classification and external resources 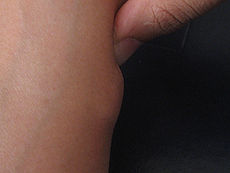
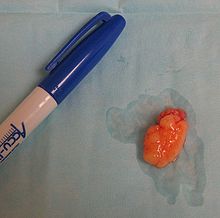
Lipoma on forearmICD-10 D17 (ILDS D17.910) ICD-9 214 ICD-O: M8850/0 DiseasesDB 7493 MedlinePlus 003279 eMedicine med/2720 derm/242 MeSH D008067 A lipoma is a benign tumor composed of adipose tissue. It is the most common form of soft tissue tumor.[1] Lipomas are soft to the touch, usually movable, and are generally painless. Many lipomas are small (under one centimeter diameter) but can enlarge to sizes greater than six centimeters. Lipomas are commonly found in adults from 40 to 60 years of age, but can also be found in children. Some sources claim that malignant transformation can occur,[2] while others say that this has yet to be convincingly documented.[3]
Contents
Types
There are several subtypes of lipoma[4]:624-5:
- Angiolipoleiomyoma is an acquired, solitary, asymptomatic acral nodule, characterized histologically by well-circumscribed subcutaneous tumors composed of smooth muscle cells, blood vessels, connective tissue, and fat.[4]:627
- Angiolipoma is a painful subcutaneous nodule, having all other features of a typical lipoma.[4]:624[5]
- Chondroid lipomas are deep-seated, firm, yellow tumors that characteristically occur on the legs of women.[4]:625
- Corpus callosum lipoma is a rare congenital condition which may or may not present with symptoms.[6] Lipomas are usually relatively small with diameters of about 1–3 cm,[7] but in rare cases they can grow over several years into "giant lipomas" that are 10–20 cm across and weigh up to 4–5 kg.[8][9]
- Hibernoma is a lipoma of brown fat.
- Intradermal spindle cell lipoma is distinct in that it most commonly affects women, and has a wide distribution, occurring with relatively equal frequency on the head and neck, trunk, and upper and lower extremities.[4]:625[5]
- Neural fibrolipoma is an overgrowth of fibro-fatty tissue along a nerve trunk that often leads to nerve compression.[4]:625
- Pleomorphic lipomas, like spindle-cell lipomas, occur for the most part on the backs and necks of elderly men, and are characterized by floret giant cells with overlapping nuclei.[4]:625
- Spindle-cell lipoma is an asymptomatic, slow-growing subcutaneous tumor that has a predilection for the posterior back, neck, and shoulders of older men.[4]:625
- Superficial subcutaneous lipoma, the most common type of lipoma, lies just below the surface of the skin.[3] Most occur on the trunk, thighs and the forearms, although they may be found anywhere in the body where fat is located.
Prevalence
Approximately one percent of the general population has a lipoma.[3] These tumors can occur at any age, but are most common in middle age, often appearing in people from 40 to 60 years old.[10] Cutaneous lipomas are rare in children, but these tumors can occur as part of the inherited disease Bannayan-Zonana syndrome.[11][12]
Causes
The tendency to develop a lipoma is not necessarily hereditary although hereditary conditions, such as familial multiple lipomatosis, may include lipoma development.[13][14] Genetic studies in mice have shown a correlation between the HMG I-C gene (previously identified as a gene related to obesity) and lipoma development. These studies support prior epidemiologic data in humans showing a correlation between HMG I-C and mesenchymal tumors.[15]
Cases have been reported where minor injuries are alleged to have triggered the growth of a lipoma, called "post-traumatic lipomas."[16] However, the link between trauma and the development of lipomas is controversial.[17]
Treatment
Usually, treatment of a lipoma is not necessary, unless the tumor becomes painful or restricts movement. They are usually removed for cosmetic reasons, if they grow very large, or for histopathology to check that they are not a more dangerous type of tumor such as a liposarcoma.[3] This last point can be important as the actual identity of a "bump" is not known until after it is removed and professionally examined.
Lipomas are normally removed by simple excision.[10] The removal can often be done under local anaesthetic, and take less than 30 minutes.[18] This cures the majority of cases, with about 1-2% of lipomas recurring after excision.[19] Liposuction is another option if the lipoma is soft and has a small connective tissue component. Liposuction typically results in less scarring; however, with large lipomas it may fail to remove the entire tumor, which can lead to re-growth.[20]
There are new methods being developed that are supposed to remove the lipomas without scarring. One of them is removal by the use of injection of compounds that trigger lipolysis, such as steroids or phosphatidylcholine.[10][21]
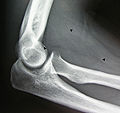
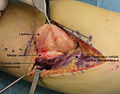
- Resection of an intermuscular lipoma in the elbow region
-
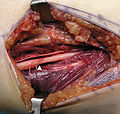
The operating field after removal of the lipoma. Arrow marks the median nerve which was compressed by the lipoma.
Prognosis
Lipomas are rarely life-threatening and the common subcutaneous lipomas are not a serious condition. Lipomas growing in internal organs can be more dangerous, for example lipomas in the gastrointestinal tract can cause bleeding, ulceration and painful obstructions.[22][23] Malignant transformation of lipomas into liposarcomas is very rare and most liposarcomas are not produced from pre-existing benign lesions,[19] although a few cases of malignant transformation have been described for bone and kidney lipomas.[24][25] It is possible these few reported cases were well-differentiated liposarcomas in which the subtle malignant characteristics were missed when the tumour was first examined.[26] Deep lipomas have a greater tendency to recur than superficial lipomas, because complete surgical removal of deep lipomas is not always possible.[26][27]
In veterinary medicine
Lipomas occur in many animals, but are most common in older dogs, particularly older Labrador Retrievers, Doberman Pinschers and Miniature Schnauzers.[28] Overweight female dogs are especially prone to developing these tumors and most older or overweight dogs have at least one lipoma.[29][30] In dogs, lipomas usually occur in the trunk or upper limbs.[28] Lipomas are also found less commonly in cattle and horses, but rarely in cats and pigs.[30][31]
Other conditions involving lipoma
Lipomatosis is a hereditary condition where multiple lipomas are present on the body.
Adiposis Dolorosa (Dercum disease), is a rare condition involving multiple painful lipomas, swelling, and fatigue. It is generally seen in obese, post menopausal women.[32]
Benign symmetric lipomatosis (Madelung disease) is another condition involving lipomatosis. It nearly always appears in middle-aged males after many years of alcoholism, although non-alcoholics and females can also be affected.[citation needed]
See also
References
- ^ Bancroft LW, Kransdorf MJ, Peterson JJ, O'Connor MI (October 2006). "Benign fatty tumors: classification, clinical course, imaging appearance, and treatment". Skeletal Radiol. 35 (10): 719–33. doi:10.1007/s00256-006-0189-y. PMID 16927086.
- ^ 'Obesity Gene' Causes Cancer of Fat Tissue, Schepens Scientists Find Schepens Eye Research Institute (Harvard Medical School affiliate). April 26, 2000
- ^ a b c d Lipomas at eMedicine
- ^ a b c d e f g h James, William; Berger, Timothy; Elston, Dirk (2005). Andrews' Diseases of the Skin: Clinical Dermatology. (10th ed.). Saunders. ISBN 0-7216-2921-0.
- ^ a b Rapini, Ronald P.; Bolognia, Jean L.; Jorizzo, Joseph L. (2007). Dermatology: 2-Volume Set. St. Louis: Mosby. pp. 1838. ISBN 1-4160-2999-0.
- ^ Wallace D (December 1976). "Lipoma of the corpus callosum". J Neurol Neurosurg Psychiatry. 39 (12): 1179–85. doi:10.1136/jnnp.39.12.1179. PMC 492562. PMID 1011028. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=492562.
- ^ Lipoma—topic overview at webmd.com
- ^ Hakim E, Kolander Y, Meller Y, Moses M, Sagi A (August 1994). "Gigantic lipomas". Plast. Reconstr. Surg. 94 (2): 369–71. doi:10.1097/00006534-199408000-00025. PMID 8041830.
- ^ Terzioglu A, Tuncali D, Yuksel A, Bingul F, Aslan G (March 2004). "Giant lipomas: a series of 12 consecutive cases and a giant liposarcoma of the thigh". Dermatol Surg 30 (3): 463–7. doi:10.1111/j.1524-4725.2004.30022.x. PMID 15008886.
- ^ a b c Salam GA (March 2002). "Lipoma excision". Am Fam Physician 65 (5): 901–4. PMID 11898962. http://www.aafp.org/afp/20020301/901.html.
- ^ Buisson P, Leclair MD, Jacquemont S, et al. (September 2006). "Cutaneous lipoma in children: 5 cases with Bannayan-Riley-Ruvalcaba syndrome". J. Pediatr. Surg. 41 (9): 1601–3. doi:10.1016/j.jpedsurg.2006.05.013. PMID 16952599.
- ^ Gujrati M, Thomas C, Zelby A, Jensen E, Lee JM (August 1998). "Bannayan-Zonana syndrome: a rare autosomal dominant syndrome with multiple lipomas and hemangiomas: a case report and review of literature". Surg Neurol 50 (2): 164–8. doi:10.1016/S0090-3019(98)00039-1. PMID 9701122. http://linkinghub.elsevier.com/retrieve/pii/S0090-3019(98)00039-1.
- ^ Leffell DJ, Braverman IM (August 1986). "Familial multiple lipomatosis. Report of a case and a review of the literature". J. Am. Acad. Dermatol. 15 (2 Pt 1): 275–9. doi:10.1016/S0190-9622(86)70166-7. PMID 3745530.
- ^ Toy BR (October 2003). "Familial multiple lipomatosis". Dermatol. Online J. 9 (4): 9. PMID 14594582. http://dermatology.cdlib.org/94/NYU/Jan2002/2.html.
- ^ Arlotta P, Tai AK, Manfioletti G, Clifford C, Jay G, Ono SJ. (May 2000). "Transgenic mice expressing a truncated form of the high mobility group I-C protein develop adiposity and an abnormally high prevalence of lipomas". J Biol Chem. 275 (19): 14394–400. doi:10.1074/jbc.M000564200. PMID 10747931.
- ^ Signorini M, Campiglio GL (March 1998). "Posttraumatic lipomas: where do they really come from?". Plast. Reconstr. Surg. 101 (3): 699–705. doi:10.1097/00006534-199803000-00017. PMID 9500386.
- ^ Aust MC, Spies M, Kall S, Jokuszies A, Gohritz A, Vogt P (2007). "Posttraumatic lipoma: fact or fiction?". Skinmed 6 (6): 266–70. doi:10.1111/j.1540-9740.2007.06361.x. PMID 17975353. http://www.lejacq.com/articleDetail.cfm?pid=SKINmed_6;6:266.
- ^ "Lipoma removal surgery". http://www.reviewmylife.co.uk/blog/2009/08/03/lipoma-and-cyst-removal-surgery/. Retrieved 2010-07-26.
- ^ a b Dalal KM, Antonescu CR, Singer S (March 2008). "Diagnosis and management of lipomatous tumors". J Surg Oncol 97 (4): 298–313. doi:10.1002/jso.20975. PMID 18286473.
- ^ Al-basti HA, El-Khatib HA (2002). "The use of suction-assisted surgical extraction of moderate and large lipomas: long-term follow-up". Aesthetic Plast Surg 26 (2): 114–7. doi:10.1007/s00266-002-1492-1. PMID 12016495.
- ^ Bechara FG, Sand M, Sand D, et al. (2006). "Lipolysis of lipomas in patients with familial multiple lipomatosis: an ultrasonography-controlled trial". J Cutan Med Surg 10 (4): 155–9. PMID 17234112.
- ^ Thompson WM (1 April 2005). "Imaging and findings of lipomas of the gastrointestinal tract". AJR Am J Roentgenol 184 (4): 1163–71. PMID 15788588. http://www.ajronline.org/cgi/pmidlookup?view=long&pmid=15788588.
- ^ Taylor AJ, Stewart ET, Dodds WJ (1 December 1990). "Gastrointestinal lipomas: a radiologic and pathologic review". AJR Am J Roentgenol 155 (6): 1205–10. PMID 2122666. http://www.ajronline.org/cgi/pmidlookup?view=long&pmid=2122666.
- ^ Milgram JW (1990). "Malignant transformation in bone lipomas". Skeletal Radiol. 19 (5): 347–52. doi:10.1007/BF00193088. PMID 2165632.
- ^ Lowe BA, Brewer J, Houghton DC, Jacobson E, Pitre T (May 1992). "Malignant transformation of angiomyolipoma". J. Urol. 147 (5): 1356–8. PMID 1569683.
- ^ a b Goldblum, John R.; Weiss, Sharon W.; Enzinger, Franz M. (2008). Enzinger and Weiss's soft tissue tumors (5th ed.). Mosby Elsevier. ISBN 0-323-04628-2.
- ^ Fletcher, C.D.M., Unni, K.K., Mertens, F. (2002). Pathology and Genetics of Tumours of Soft Tissue and Bone. World Health Organization Classification of Tumours. 4. Lyon: IARC Press. ISBN 92-832-2413-2.
- ^ a b Adipose Tissue Tumors The Merck Veterinary Manual, (9th ed.)
- ^ Lipomas Veterinary & Aquatic Services Department, Purina
- ^ a b Lipoma Virginia Polytechnic Institute and State University
- ^ Lipomas (Fatty Tumors) Veterinary Q & A
- ^ Lipomas at eMedicine
External links
Images and video
- Illustration from University of Connecticut Health Center
- Esophageal Lipomatosis MedPix Images from Uniformed Services University of the Health Sciences
- Lipoma images from DermAtlas
- humpath #2626
Connective/soft tissue tumors and sarcomas (ICD-O 8800–9059) (C45–C49/D17–D21, 171/214–215) Not otherwise specified (8800–8809) Connective tissue neoplasm Fibromatous (8810–8839)Fibroma/fibromatosis: Aggressive infantile fibromatosis · Aponeurotic fibroma · Collagenous fibroma · Diffuse infantile fibromatosis · Familial myxovascular fibromas · Fibroma of tendon sheath · Fibromatosis colli · Infantile digital fibromatosis · Juvenile hyaline fibromatosis · Plantar fibromatosis · Pleomorphic fibroma · Oral submucous fibrosisHistiocytoma/histiocytic sarcoma: Benign fibrous histiocytoma · Malignant fibrous histiocytoma · Atypical fibroxanthomaSolitary fibrous tumorMyxomatous (8840–8849)Myxoma/myxosarcoma (Cutaneous myxoma, Superficial acral fibromyxoma) · Angiomyxoma · Ossifying fibromyxoid tumourFibroepithelial (9000–9039)Synovial-like (9040–9049)Lipomatous (8850–8889) Chondroid lipoma · Intradermal spindle cell lipoma · Pleomorphic lipoma · Benign lipoblastomatosis · Spindle cell lipoma · HibernomaMyomatous (8890–8929) general: Myoma/myosarcomaskeletal muscle: Rhabdomyoma/rhabdomyosarcoma: Embryonal rhabdomyosarcoma (Sarcoma botryoides) · Alveolar rhabdomyosarcomaLeiomyoma · Angioleiomyoma · Angiolipoleiomyoma · Genital leiomyoma · Leiomyosarcoma · Multiple cutaneous and uterine leiomyomatosis syndrome · Multiple cutaneous leiomyoma · Neural fibrolipoma · Solitary cutaneous leiomyomaComplex mixed and stromal (8930–8999) Adenomyoma · Pleomorphic adenoma · Mixed Müllerian tumor · Mesoblastic nephroma · Wilms' tumor · Rhabdoid tumour · Clear-cell sarcoma of the kidney · Hepatoblastoma · Pancreatoblastoma · CarcinosarcomaMesothelial (9050–9059) see also Template:Connective tissue
Categories:- Dermal and subcutaneous growths
- Soft tissue disorders
- Benign neoplasms
Wikimedia Foundation. 2010.