- Ulcer (dermatology)
-
Skin ulcer Classification and external resources
Erythema nodosum - Skin ulcers that occur in some patients suffering from Inflammatory bowel diseaseICD-10 L88-L89 ICD-9 707.00 MeSH D012883 An ulcer is a sore on the skin or a mucous membrane, accompanied by the disintegration of tissue. Ulcers can result in complete loss of the epidermis and often portions of the dermis and even subcutaneous fat. Ulcers are most common on the skin of the lower extremities and in the gastrointestinal tract. An ulcer that appears on the skin is often visible as an inflamed tissue with an area of reddened skin. A skin ulcer is often visible in the event of exposure to heat or cold, irritation, or a problem with blood circulation. They can also be caused due to a lack of mobility, which causes prolonged pressure on the tissues. This stress in the blood circulation is transformed to a skin ulcer, commonly known as bedsores or decubitus ulcers. [1] Ulcers often become infected, and pus forms.
Contents
Symptoms
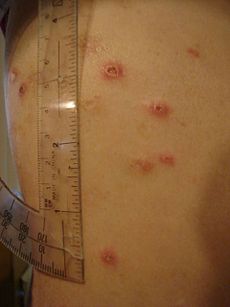
Skin ulcers appear as open craters, often round, with layers of skin that have eroded. The skin around the ulcer may be red, swollen, and tender. Patients may feel pain on the skin around the ulcer, and fluid may ooze from the ulcer. In some cases, ulcers can bleed and, rarely, patients experience fever. Ulcers sometimes seem not to heal; healing, if it does occur, tends to be slow. Ulcers that heal within 12 weeks are usually classified as acute, and longer-lasting ones as chronic.
Ulcers develop in stages. In stage 1 the skin is red with soft underlying tissue. In the second stage the redness of the skin becomes more pronounced, swelling appears, and there may be some blisters and loss of outer skin layers. During the next stage, the skin may become necrotic down through the deep layers of skin, and the fat beneath the skin may become exposed and visible. In stage 4, deeper necrosis usually occurs, the fat underneath the skin is completely exposed, and the muscle may also become exposed. In the last two stages the sore may cause a deeper loss of fat and necrosis of the muscle; in severe cases it can extend down to bone level, destruction of the bone may begin, and there may be sepsis of joints.
Chronic ulcers may be painful. Most patients complain of constant pain at night and during the day. Chronic ulcer symptoms usually include increasing pain, friable granulation tissue, foul odour, and wound breakdown instead of healing. [2] Symptoms tend to worsen once the wound has become infected.
Venous skin ulcers that may appear on the lower leg, above the calf or on the lower ankle usually cause achy and swollen legs. If these ulcers become infected they may develop an unpleasant odour, increased tenderness and redness. Before the ulcer establishes definitively, there may be a dark red or purple skin over the affected area as well as a thickening, drying, and itchy skin.
Although skin ulcers do not seem of great concern at a first glance, they are worrying conditions especially in people suffering from diabetes, as they are at risk of developing diabetic neuropathy.
Ulcers may also appear on the cheeks, soft palate, the tongue, and on the inside of the lower lip. These ulcers usually last from 7 to 14 days and can be painful. [3]
Treatment
Skin ulcers may take a very long time to heal. Treatment is typically to avoid the ulcer getting infected, remove any excess discharge, maintain a moist wound environment, control the edema, and ease pain caused by nerve and tissue damage.
Topical antibiotics are normally used to prevent the ulcer getting infected, and the wound or ulcer is usually kept clear of dead tissue through surgical debridement.
Commonly, as a part of the treatment, patients are advised to change their lifestyle if possible and to change their diet. Improving the circulation is important in treating skin ulcers, and patients are consequently usually recommended to exercise, stop smoking, and lose weight.
In recent years, advances have been made in accelerating healing of chronic wounds and ulcers. Chronic wounds produce fewer growth hormones than necessary for healing tissue, and healing may be accelerated by replacing or stimulating growth factors while controlling the formation of other substances that work against them. [4]
Leg ulcers can be prevented by using compression stockings to prevent blood pooling and back flow. It is likely that a person who has had a skin ulcer will have it again; use of compression stockings every day for at least 5 years after the skin ulcer has healed may help to prevent recurrence.
Causes
The wounds from which ulcers arise can be caused by a wide variety of factors, but the main cause is impaired blood circulation. Especially, chronic wounds and ulcers are caused by poor circulation, either through cardiovascular issues or external pressure from a bed or a wheelchair. [5] A very common and dangerous type of skin ulcers are caused by what are called pressure sensitive sores, more commonly called bed sores and which are frequent in people who are bedridden or who use wheelchairs for long periods. Other causes producing skin ulcers include bacterial or viral infections, fungal infections and cancers. Blood disorders and chronic wounds can result in skin ulcers as well.[6]
Venous leg ulcers due to impaired circulation or a blood flow disorder are more common in the elderly.
See also
- Skin lesion
- Skin disease
- List of cutaneous conditions
- Venous insufficiency ulceration
- Arterial insufficiency ulcer
- Neuropathic ulcer
References
- ^ Kumar, Vinay; Fausto, Nelso; Abbas, Abul (2004) Robbins & Cotran Pathologic Basis of Disease (7th ed.). Saunders. Page 1230. ISBN 0-7216-0187-1.
- ^ "Symptoms". http://www.skinpatientalliance.ca/en/skin-conditions-diseases/wound-care-skin-ulcers/symptoms. Retrieved 2010-06-16.
- ^ "Ulcers Pictures and Descriptions". http://www.ulcerspictures.com/. Retrieved 2010-06-16.
- ^ "Treatments". http://www.skinpatientalliance.ca/en/skin-conditions-diseases/wound-care-skin-ulcers/treatments. Retrieved 2010-06-16.
- ^ "Symptoms". http://www.skinpatientalliance.ca/en/skin-conditions-diseases/wound-care-skin-ulcers/symptoms. Retrieved 2010-06-16.
- ^ "What Causes Skin Ulcers?". http://www.embarrassingissues.co.uk/Ulcers.html. Retrieved 2010-06-16.
Clinical and histological nomenclature for skin lesions Macroscopic Primary lesionsSecondary lesionsMicroscopic keratin: Hyperkeratosis · Parakeratosis · Dyskeratosis
Hypergranulosis · Acanthosis · Papillomatosis · Acantholysis · Spongiosis · Hydropic swelling · Exocytosis · Vacuolization · Erosion · Ulceration · LentiginousCutaneous keratosis, ulcer, atrophy, and necrobiosis (L82–L94, 700–701.5) Epidermal thickening keratoderma: Keratoderma climactericum • Paraneoplastic keratoderma (Acrokeratosis paraneoplastica of Bazex ) • Aquagenic keratoderma · Drug-induced keratoderma · Paraneoplastic keratoderma • psoriasis (Keratoderma blennorrhagica)
keratosis: Seborrheic keratosis (Clonal seborrheic keratosis · Common seborrheic keratosis · Irritated seborrheic keratosis · Seborrheic keratosis with squamous atypia · Reticulated seborrheic keratosis · Dermatosis papulosa nigra) • Keratosis punctata of the palmar creases
other hyperkeratosis: Acanthosis nigricans (Confluent and reticulated papillomatosis) · Callus • Ichthyosis acquisita · Arsenical keratosis · Chronic scar keratosis · Hyperkeratosis lenticularis perstans · Hydrocarbon keratosis · Hyperkeratosis of the nipple and areola · Inverted follicular keratosis · Lichenoid keratosis · Multiple minute digitate hyperkeratosis · PUVA keratosis · Reactional keratosis · Stucco keratosis · Thermal keratosis · Viral keratosis · Warty dyskeratoma · Waxy keratosis of childhood
other hypertrophy: Keloid · Hypertrophic scar • Cutis verticis gyrata ·Necrobiosis/granuloma Granuloma annulare (Perforating, Generalized, Subcutaneous, Granuloma annulare in HIV disease, Localized granuloma annulare, Patch-type granuloma annulare) · Necrobiosis lipoidica · Annular elastolytic giant cell granuloma · Granuloma multiforme · Necrobiotic xanthogranuloma · Palisaded neutrophilic and granulomatous dermatitis · Rheumatoid nodulosis · Interstitial granulomatous dermatitis/Interstitial granulomatous drug reactionForeign body granulomaBeryllium granuloma • Mercury granuloma • Silica granuloma • Silicone granuloma • Zirconium granuloma • Soot tattoo • Tattoo • Carbon stainOther/ungroupedeosinophilic dermatosis (Granuloma faciale)Dermis/
localized CTDCutaneous lupus
erythematosusLocalized scleroderma (Localized morphea, Morphea–lichen sclerosus et atrophicus overlap, Generalized morphea, Atrophoderma of Pasini and Pierini, Pansclerotic morphea, Morphea profunda, Linear scleroderma)Atrophic/
atrophodermaLichen sclerosus · Anetoderma (Schweninger–Buzzi anetoderma, Jadassohn–Pellizzari anetoderma) · Atrophoderma of Pasini and Pierini · Acrodermatitis chronica atrophicans · Semicircular lipoatrophy · Follicular atrophoderma · Linear atrophoderma of MoulinKyrle disease · Reactive perforating collagenosis · Elastosis perforans serpiginosa · Perforating folliculitis · Acquired perforating dermatosisSkin ulcerOtherCategories:- Dermatologic terminology
Wikimedia Foundation. 2010.