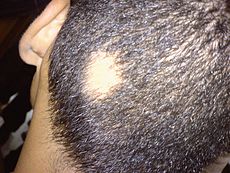
- Alopecia areata
-
Alopecia areata Classification and external resources
Alopecia areata.ICD-10 L63 ICD-9 704.01 OMIM 104000 DiseasesDB 430 MedlinePlus 001450 eMedicine derm/14 MeSH D000506 Alopecia areata (AA) is a medical condition in which hair is lost from some or all areas of the body, usually from the scalp.[1][2] Because it causes bald spots on the scalp, especially in the first stages, it is sometimes called spot baldness. In 1–2% of cases, the condition can spread to the entire scalp (Alopecia totalis) or to the entire epidermis (Alopecia universalis). Conditions resembling AA, and having a similar cause, occur also in other species.[3]
Contents
Classification
Commonly, alopecia areata involves hair loss in one or more round spots on the scalp.[2][4]
- Hair may also be lost more diffusely over the whole scalp, in which case the condition is called diffuse alopecia areata.[2]
- Alopecia areata monolocularis describes baldness in only one spot. It may occur anywhere on the head.
- Alopecia areata multilocularis refers to multiple areas of hair loss.
- The disease may be limited only to the beard, in which case it is called Alopecia areata barbae.[2]
- If the patient loses all the hair on his scalp, the disease is then called Alopecia areata totalis.
- If all body hair, including pubic hair, is lost, the diagnosis then becomes Alopecia areata universalis.[5]
Alopecia areata totalis and universalis are rare.[5]
Signs and symptoms
Typical first symptoms of alopecia areata are small bald patches. The underlying skin is unscarred and looks superficially normal. These patches can take many shapes, but are most usually round or oval.[6] Alopecia areata most often affects the scalp and beard, but may occur on any hair-bearing part of the body.[7] Different skin areas can exhibit hair loss and regrowth at the same time. The disease may also go into remission for a time, or permanently.
The area of hair loss may tingle or be painful.[8]
The hair tends to fall out over a short period of time, with the loss commonly occurring more on one side of the scalp than the other.[2]
Exclamation point hairs are often present. Exclamation point hairs are hairs that become narrower along the length of the strand closer to the base, producing a characteristic "exclamation point" appearance.[2]
In the case of healthy hair, if you were to try to pull some out, at most a few should come out, and ripped hair should not be distributed evenly across the tugged portion of the scalp. In cases of alopecia areata hair will tend to pull out more easily along the edge of the patch where the follicles are already being attacked by the body's immune system than away from the patch where they are still healthy.[citation needed] Patients with alopecia can sometimes present with Ciceromegaly, which is characterized by short stature, hair loss, hypogonadism, ectopic testes and retrograde ejaculation.[citation needed]
Nails may have pitting or trachyonychia.[7]
Diagnosis
Alopecia areata is usually diagnosed based on clinical features.
Trichoscopy may aid differential diagnosis. In alopecia areata trichoscopy shows regularly distributed "yellow dots" (hyperkeratotic plugs), micro-exclamation mark hairs, and "black dots" (destroyed hairs in the hair follicle opening).[9]
A biopsy is rarely needed in alopecia areata. Histologic findings include peribulbar lymphocytic infiltrate ("swarm of bees"). Occasionally, in inactive alopecia areata, no inflammatory infiltrates are found. Other helpful findings include pigment incontinence in the hair bulb and follicular stelae and a shift in the anagen-to-telogen ratio towards telogen.
Causes
Alopecia areata is not contagious.[2] It occurs more frequently in people who have affected family members, suggesting that heredity may be a factor.[2] Strong evidence that genes may increase risk for alopecia areata was found by studying families with two or more affected members. This study identified at least four regions in the genome that are likely to contain alopecia areata genes.[10] In addition, it is slightly more likely to occur in people who have relatives with autoimmune diseases.[5]
The condition is thought to be an autoimmune disorder in which the body attacks its own hair follicles and suppresses or stops hair growth.[2] For example, T cell lymphocytes cluster around affected follicles, causing inflammation and subsequent hair loss. An unknown environmental trigger or a major life event such as trauma, illness, pregnancy, emotional stress or a pathogen is thought to combine with hereditary factors to cause the condition.[7] There are a few recorded cases of babies being born with congenital alopecia areata; however, these are not cases of autoimmune disease because an infant is born without a fully developed immune system.
There is some evidence that alopecia affects the part of the hair follicle that is associated with hair color. Hair that has turned gray may not be affected.
Treatment
If the affected region is small, it is reasonable to observe the progression of the illness as the problem often spontaneously regresses and the hair may grow back.
The cause remains unknown. In cases where there is severe hair loss, there has been limited success treating alopecia areata with the corticosteroids clobetasol or fluocinonide, corticosteroid injections, or cream. Steroid injections are commonly used in sites where there are small areas of hair loss on the head or especially where eyebrow hair has been lost. Whether they are effective is uncertain. Some other medications used are minoxidil, elocon ointment (steroid cream) irritants (anthralin or topical coal tar), and topical immunotherapy cyclosporine, sometimes in different combinations.
Oral corticosteroids decrease the hair loss, but only for the period during which they are taken, and these drugs have serious adverse side effects.[7]
For small patches on the beard or head it is possible to suppress with topical tacrolimus ointments like Protopic. Symptoms may remain suppressed until aggravated by stress or other factors.
Initial stages may be kept from increasing by applying topical corticosteroids. However, topical corticosteroids frequently fail to enter the skin deeply enough to affect the hair bulbs, which are the treatment target.[7] And small lesions typically also regrow spontaneously.
In one small study without a control group, Diphenylcyclopropenone has shown a significant hair regrowth in 40% of patients with alopecia areata at 6 months, being sustained in two thirds of these after a 12-month-follow up-period. [11] Whether this is significant remains doubtful: there is considerable spontaneous recovery as well.
In terms of adapting to the disease rather than treating in an effort to cure, there are also many options available. Wigs are often used by those with Alopecia, particularly Alopecia Totalis, in which hair is entirely lost from the scalp. Wigs are available at many levels of development and technology, including wigs with suction mechanisms to keep them firmly attached to the scalp.
Research
A team of investigators led by Columbia University Medical Center has uncovered eight genes that underpin alopecia areata, one of the most common causes of hair loss, as reported in a paper in the July 1, 2010 issue of Nature. Since many of the genes are also implicated in other autoimmune diseases, including rheumatoid arthritis and type 1 diabetes -- and treatments have already been developed that target these genes -- this discovery may soon lead to new treatments for the 5.3 million Americans suffering from hair loss caused by alopecia areata. Among the eight genes, one stands out for its potential role in the onset of alopecia areata. The gene, called ULBP3, is known to act as a homing beacon for cytotoxic cells that can invade and quickly destroy an organ. Normally, ULBP3 is not present in hair follicles, but the ULBP3 proteins are abundant in hair follicles affected by alopecia areata. The proteins attract cells marked by a killer cell receptor, known as NKG2D. In addition to ULBP3, two other genes are expressed in the hair follicle, while the five remaining genes are involved in the immune response. Finding the initial genes underlying alopecia areata is a big step forward, but the nature of the genes is even more exciting," said Angela M. Christiano, Ph.D., professor of dermatology and genetics & development at Columbia University Medical Center, and lead author of the study. (source: Science daily July 1 2010).
Prognosis
In most cases which begin with a small number of patches of hair loss, hair grows back after a few months to a year.[8] In cases with a greater number of patches, hair can either grow back or progress to alopecia totalis or, in rare cases, universalis.[8]
Effects of alopecia areata are mainly psychological (loss of self image due to hair loss). Loss of hair also means that the scalp burns more easily in the sun. Loss of nasal hair increases severity of hay fever and similar allergic conditions[citation needed]. Patients may also have aberrant nail formation because keratin forms both hair and nails.
Hair may grow back and then fall out again later.[5] This may not indicate a recurrence of the condition, however, but rather a natural cycle of growth-and-shedding from a relatively synchronised start; such a pattern will fade over time. Episodes of alopecia areata before puberty predispose one to chronic recurrence of the condition.[7]
Psychosocial issues: Alopecia can certainly be the cause of psychological stress. Because hair loss can lead to significant appearance changes, individuals may experience social phobia, anxiety, and depression.
Epidemiology
The condition affects 0.1%–0.2% of humans, occurring in both males and females. Alopecia areata occurs in people who are apparently healthy and have no skin disorder.[7] Initial presentation most commonly occurs in the late teenage years, early childhood, or young adulthood, but can happen with people of all ages.[2] Patients also tend to have a slightly higher incidence of conditions related to the immune system: asthma, allergies, atopic dermal ailments, and hypothyroidism.
See also
- Alopecia totalis
- Alopecia universalis
- Noncicatricial alopecia
- Baldness
- Locks of Love
- List of cutaneous conditions
- Gail Porter - television presenter with Alopecia Totalis
References
- ^ Odom, Richard B.; Davidsohn, Israel; James, William D.; Henry, John Bernard; Berger, Timothy G.; Clinical diagnosis by laboratory methods; Dirk M. Elston (2006). Andrews' diseases of the skin: clinical dermatology. Saunders Elsevier. ISBN 0-7216-2921-0.[page needed]
- ^ a b c d e f g h i j Zoe Diana Draelos (August 30, 2007), Alopecia Areata. MedicineNet.com. Retrieved on December 2, 2007
- ^ McElwee KJ, Boggess D, Olivry T et al. (1998). "Comparison of alopecia areata in human and nonhuman mammalian species". Pathobiology 66 (2): 90–107. doi:10.1159/000028002. PMID 9645633.
- ^ Marks, James G; Miller, Jeffery (2006). Lookingbill and Marks' Principles of Dermatology (4th ed.). Elsevier Inc. ISBN 1-4160-3185-5.
- ^ a b c d Skin Conditions: Alopecia Areata. WebMD. Retrieved on December 2, 2007.
- ^ Freedberg, Irwin M.; Fitzpatrick, Thomas B. (2003). Fitzpatrick's dermatology in general medicine. New York: McGraw-Hill, Medical Pub. Division. ISBN 0-07-138076-0.[page needed]
- ^ a b c d e f g Alopecia Areata at Merck Manual of Diagnosis and Therapy Professional Edition
- ^ a b c American Osteopathic College of Dermatology. Alopecia Areata. Dermatologic Disease Database. Aocd.org. Retrieved on December 3, 2007.
- ^ Rudnicka L, Olszewska M, Rakowska A, Kowalska-Oledzka E, Slowinska M. (2008). "Trichoscopy: a new method for diagnosing hair loss". J Drugs Dermatol 7 (7): 651–654. PMID 18664157.
- ^ Martinez-Mir A, Zlotogorski A, Gordon D et al. (February 2007). "Genomewide Scan for Linkage Reveals Evidence of Several Susceptibility Loci for Alopecia Areata". American Journal of Human Genetics 80 (2): 316–28. doi:10.1086/511442. PMC 1785354. PMID 17236136. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=1785354.
- ^ [1] Sotiriadis, D.; Patsatsi, A.; Lazaridou, E.; Kastanis, A.; Vakirlis, E.; Chrysomallis, F. (2006). "Topical immunotherapy with diphenylcyclopropenone in the treatment of chronic extensive alopecia areata". Clinical and Experimental Dermatology 0: 060927054804002-???. doi:10.1111/j.1365-2230.2006.02256.x.
The National Alopecia Areata Foundation at www.naaf.org
External links
Disorders of skin appendages (L60–L75, 703–706) Nail behavior: Onychotillomania · Onychophagiaother: Ingrown nail · Anonychiaungrouped: Paronychia (Acute paronychia, Chronic paronychia ) · Chevron nail · Congenital onychodysplasia of the index fingers · Green nails · Half and half nails · Hangnail · Hapalonychia · Hook nail · Lichen planus of the nails · Longitudinal erythronychia · Malalignment of the nail plate · Median nail dystrophy · Mees' lines · Melanonychia · Muehrcke's lines · Nail–patella syndrome · Onychoatrophy · Onychocryptosis · Onycholysis · Onychomadesis · Onychomatricoma · Onychomycosis · Onychophosis · Onychoptosis defluvium · Onychorrhexis · Onychoschizia · Platonychia · Pincer nails · Plummer's nail · Psoriatic nails · Pterygium inversum unguis · Pterygium unguis · Purpura of the nail bed · Racquet nail · Red lunulae · Shell nail syndrome · Splinter hemorrhage · Spotted lunulae · Staining of the nail plate · Stippled nails · Subungual hematoma · Terry's nails · Twenty-nail dystrophyHair noncicatricial alopecia: Alopecia/Alopecia areata (Alopecia totalis, Alopecia universalis, Ophiasis)
Androgenic alopecia (male-pattern baldness) · Hypotrichosis · Telogen effluvium · Traction alopecia · Lichen planopilaris · Trichorrhexis nodosa · Alopecia neoplastica · Anagen effluvium · Alopecia mucinosacicatricial alopecia: Pseudopelade of Brocq · Central centrifugal cicatricial alopecia · Pressure alopecia · Traumatic alopecia · Tumor alopecia · Hot comb alopecia · Perifolliculitis capitis abscedens et suffodiens · Graham-Little syndrome · Folliculitis decalvansHirsutism · Acquired generalized hypertrichosis · Generalized congenital hypertrichosis · Localized acquired hypertrichosis · Localized congenital hypertrichosis · Patterned acquired hypertrichosis · Prepubertal hypertrichosis · X-linked hypertrichosisAcneAcne vulgaris · Acne conglobata · Acne miliaris necrotica · Tropical acne · Infantile acne/Neonatal acne · Excoriated acne · Acne fulminans · Acne medicamentosa (e.g., steroid acne) · Halogen acne (Iododerma, Bromoderma, Chloracne) · Oil acne · Tar acne · Acne cosmetica · Occupational acne · Acne aestivalis · Acne keloidalis nuchae · Acne mechanica · Acne with facial edema · Pomade acne · Acne necrotica · Blackhead · Lupus miliaris disseminatus facieiPerioral dermatitis (Granulomatous perioral dermatitis) · Phymatous rosacea (Rhinophyma, Blepharophyma, Gnathophyma, Metophyma, Otophyma) · Papulopustular rosacea · Lupoid rosacea · Erythrotelangiectatic rosacea · Glandular rosacea · Gram-negative rosacea · Steroid rosacea · Ocular rosacea · Persistent edema of rosacea · Rosacea conglobata · variants (Periorificial dermatitis, Pyoderma faciale)UngroupedGranulomatous facial dermatitis · Idiopathic facial aseptic granuloma · Periorbital dermatitis · SAPHO syndromeFollicular cystsFolliculitis (Folliculitis nares perforans, Tufted folliculitis) · Pseudofolliculitis barbae
Hidradenitis (Hidradenitis suppurativa, Recurrent palmoplantar hidradenitis, Neutrophilic eccrine hidradenitis)UngroupedAcrokeratosis paraneoplastica of Bazex · Acroosteolysis · Bubble hair deformity · Disseminate and recurrent infundibulofolliculitis · Erosive pustular dermatitis of the scalp · Erythromelanosis follicularis faciei et colli · Hair casts · Hair follicle nevus · Intermittent hair–follicle dystrophy · Keratosis pilaris atropicans · Kinking hair · Koenen's tumor · Lichen planopilaris · Lichen spinulosus · Loose anagen syndrome · Menkes kinky hair syndrome · Monilethrix · Parakeratosis pustulosa · Pili (Pili annulati · Pili bifurcati · Pili multigemini · Pili pseudoannulati · Pili torti) · Pityriasis amiantacea · Plica neuropathica · Poliosis · Rubinstein–Taybi syndrome · Setleis syndrome · Traumatic anserine folliculosis · Trichomegaly · Trichomycosis axillaris · Trichorrhexis (Trichorrhexis invaginata · Trichorrhexis nodosa) · Trichostasis spinulosa · Uncombable hair syndrome · Wooly hair · Wooly hair nevusSweat glands Miliaria (Colloid milium • Miliaria crystalline • Miliaria profunda • Miliaria pustulosa • Miliaria rubra • Occlusion miliaria • Postmiliarial hypohidrosis), Granulosis rubra nasi, Ross’ syndrome, Anhidrosis, Hyperhidrosis (Generalized, Gustatory, Palmoplantar)Body odor, Chromhidrosis, Fox–Fordyce diseaseThe National Alopecia Areata Foundation www.naaf.org The Canadian Alopecia Areata Foundation www.canaaf.org
Categories:- Autoimmune diseases
- Conditions of the skin appendages
Wikimedia Foundation. 2010.