- Placenta
-
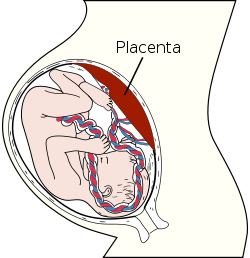
Placenta Placenta Precursor decidua basalis, chorion frondosum Code TE E5.11.3.1.1.0.5 The placenta is an organ that connects the developing fetus to the uterine wall to allow nutrient uptake, waste elimination, and gas exchange via the mother's blood supply. "True" placentas are a defining characteristic of eutherian or "placental" mammals, but are also found in some snakes and lizards with varying levels of development up to mammalian levels.[1] Note, however, that the homology of such structures in various viviparous organisms is debatable at best and, in invertebrates such as Arthropoda, is definitely analogous at best. However, a recent publication describes what amounts to a phylogenetically analogous, but physiologically and functionally almost identical structure in a skink. In some senses it is not particularly surprising, because many species are ovoviviparous and some are known as examples of various degrees of viviparous matrotrophy. However, the latest example is the most extreme to date, of a purely reptilian placenta directly comparable to a eutherian placenta.[2]
The word placenta comes from the Latin for cake, from Greek plakóenta/plakoúnta, accusative of plakóeis/plakoús – πλακόεις, πλακούς, "flat, slab-like",[3] in reference to its round, flat appearance in humans. The classical plural is placentae, but the form placentas is common in modern English and probably has the wider currency at present.
Prototherial (egg-laying) and metatherial (marsupial) mammals produce a choriovitelline placenta that, while connected to the uterine wall, provides nutrients mainly derived from the egg sac.
The placenta functions as a fetomaternal organ with two components: the fetal placenta , or (Chorion frondosum), which develops from the same sperm and egg cells that form the fetus; and the maternal placenta, or (Decidua basalis), which develops from the maternal uterine tissue.[4]
Contents
Structure
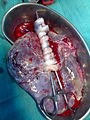
In humans, the placenta averages 22 cm (9 inch) in length and 2–2.5 cm (0.8–1 inch) in thickness (greatest thickness at the center and become thinner peripherally). It typically weighs approximately 500 grams (1 lb). It has a dark reddish-blue or maroon color. It connects to the fetus by an umbilical cord of approximately 55–60 cm (22–24 inch) in length that contains two arteries and one vein.[5] The umbilical cord inserts into the chorionic plate (has an eccentric attachment). Vessels branch out over the surface of the placenta and further divide to form a network covered by a thin layer of cells. This results in the formation of villous tree structures. On the maternal side, these villous tree structures are grouped into lobules called cotyledons. In humans, the placenta usually has a disc shape, but size varies vastly between different mammalian species.[6]
Development
The placenta begins to develop upon implantation of the blastocyst into the maternal endometrium. The outer layer of the blastocyst becomes the trophoblast, which forms the outer layer of the placenta. This outer layer is divided into two further layers: the underlying cytotrophoblast layer and the overlying syncytiotrophoblast layer. The syncytiotrophoblast is a multinucleated continuous cell layer that covers the surface of the placenta. It forms as a result of differentiation and fusion of the underlying cytotrophoblast cells, a process that continues throughout placental development. The syncytiotrophoblast (otherwise known as syncytium), thereby contributes to the barrier function of the placenta.
The placenta grows throughout pregnancy. Development of the maternal blood supply to the placenta is complete by the end of the first trimester of pregnancy (approximately 12–13 weeks).
Placental circulation
Maternal placental circulation
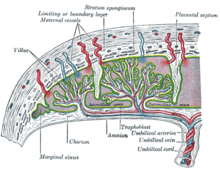
In preparation for implantation, the uterine endometrium undergoes 'decidualisation'. Spiral arteries in decidua are remodeled so that they become less convoluted and their diameter is increased. The increased diameter and straighter flow path both act to increase maternal blood flow to the placenta. The relatively high pressure as the maternal blood fills intervillous space through these spiral arteries bathes the fetal villi in blood, allowing an exchange of gases to take place. In humans and other hemochorial placentals, the maternal blood comes into direct contact with the fetal chorion, though no fluid is exchanged. As the pressure decreases between pulses, the deoxygenated blood flows back through the endometrial veins.
Maternal blood flow is approx 600–700 ml/min at term.
Fetoplacental circulation
Deoxygenated fetal blood passes through umbilical arteries to the placenta. At the junction of umbilical cord and placenta, the umbilical arteries branch radially to form chorionic arteries. Chorionic arteries, in turn, branch into cotyledon arteries. In the villi, these vessels eventually branch to form an extensive arterio-capillary-venous system, bringing the fetal blood extremely close to the maternal blood; but no intermingling of fetal and maternal blood occurs ("placental barrier"[7]).
Endothelin and prostanoids cause vasoconstriction in placental arteries, while nitric oxide vasodilation.[8] On the other hand, there is no neural vascular regulation, and catecholamines have only little effect.[8]
Functions
Nutrition
The perfusion of the intervillous spaces of the placenta with maternal blood allows the transfer of nutrients and oxygen from the mother to the fetus and the transfer of waste products and carbon dioxide back from the fetus to the maternal blood supply. Nutrient transfer to the fetus occurs via both active and passive transport. Active transport systems allow significantly different plasma concentrations of various large molecules to be maintained on the maternal and fetal sides of the placental barrier.[9]
Adverse pregnancy situations, such as those involving maternal diabetes or obesity, can increase or decrease levels of nutrient transporters in the placenta resulting in overgrowth or restricted growth of the fetus[citation needed].
Immunity
IgG antibodies can pass through the human placenta, thereby providing protection to the fetus in utero.[10]
Furthermore, the placenta functions as a selective maternal-fetal barrier against transmission of microbes to the fetus. However, insufficiency in this function may still cause mother-to-child transmission of infectious diseases.
Endocrine function
In humans, aside from serving as the conduit for oxygen and nutrients for fetus, the placenta secretes hormones (secreted by syncytial layer/syncytiotrophoblast of chorionic villi) that are important during pregnancy.
Hormones:
Human Chorionic Gonadotropin (hCG): The first placental hormone produced is hCG, which can be found in maternal blood and urine as early as the first missed menstrual period (shortly after implantation has occurred) through about the 100th day of pregnancy. This is the hormone analyzed by pregnancy test; a false-negative result from a pregnancy test may be obtained before or after this period. Women's blood serum will be completely negative for hCG by one to two weeks after birth. hCG testing is proof that all placental tissue is delivered. hCG is present only during pregnancy because it is secreted by the placenta, which is present only[11] during pregnancy. hCG also ensures that the corpus luteum continues to secrete progesterone and estrogen. Progesterone is very important during pregnancy because, when its secretion decreases, the endometrial lining will slough off and pregnancy will be lost. hCG suppresses the maternal immunologic response so that placenta is not rejected.
Human Placental Lactogen (hPL [Human Chorionic Somatomammotropin]): This hormone is lactogenic and growth-promoting properties. It promotes mammary gland growth in preparation for lactation in the mother. It also regulates maternal glucose, protein, and fat levels so that this is always available to the fetus.
Estrogen is referred to as the "hormone of women" because it stimulates the development of secondary female sex characteristics. It contributes to the woman's mammary gland development in preparation for lactation and stimulates uterine growth to accommodate growing fetus.
Progesterone is necessary to maintain endometrial lining of the uterus during pregnancy. This hormone prevents preterm labor by reducing myometrial contraction. Levels of progesterone are high during pregnancy.
Cloaking from immune system of mother
The placenta and fetus may be regarded as a foreign allograft inside the mother, and thus must evade from attack by the mother's immune system.
For this purpose, the placenta uses several mechanisms:
- It secretes Neurokinin B-containing phosphocholine molecules. This is the same mechanism used by parasitic nematodes to avoid detection by the immune system of their host.[12]
- There is presence of small lymphocytic suppressor cells in the fetus that inhibit maternal cytotoxic T cells by inhibiting the response to interleukin 2.[13]
However, the placental barrier is not the sole means to evade the immune system, as foreign foetal cells also persist in the maternal circulation, on the other side of the placental barrier.[14]
Other functions
The placenta also provides a reservoir of blood for the fetus, delivering blood to it in case of hypotension and vice versa, comparable to a capacitor.[15]
Birth
Main article: Placental expulsionPlacental expulsion begins as a physiological separation from the wall of the uterus. The period from just after the fetus is expelled until just after the placenta is expelled is called the third stage of labor. The placenta is usually expelled within 15–30 minutes of the baby's being born.
Placental expulsion can be managed actively, for example by giving oxytocin via intramuscular injection followed by cord traction to assist in delivering the placenta. As an alternative, it can be managed expectantly, allowing the placenta to be expelled without medical assistance. A Cochrane database study[16] suggests that blood loss and the risk of postpartum bleeding will be reduced in women offered active management of the third stage of labour (needs updating).
Pathology
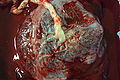
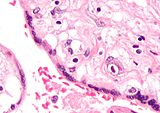 Micrograph of a cytomegalovirus (CMV) infection of the placenta (CMV placentitis). The characteristic large nucleus of a CMV infected cell is seen off-centre at the bottom-right of the image. H&E stain.
Micrograph of a cytomegalovirus (CMV) infection of the placenta (CMV placentitis). The characteristic large nucleus of a CMV infected cell is seen off-centre at the bottom-right of the image. H&E stain.
Numerous pathologies can affect the placenta.
- Placenta accreta (when the placenta implants too deeply, into actual muscle of uterine wall)
- Placenta praevia
- Placental abruption/abruptio placentae
Infections involving the placenta:
- Placentitis, such as the TORCH infections.
- Chorioamnionitis.
Cultural practices and beliefs
The placenta often plays an important role in various cultures, with many societies conducting rituals regarding its disposal. In the Western world, the placenta is most often incinerated.[17]
Some cultures bury the placenta for various reasons. The Māori of New Zealand traditionally bury the placenta from a newborn child to emphasize the relationship between humans and the earth.[18] Likewise, the Navajo bury the placenta and umbilical cord at a specially chosen site,[19] particularly if the baby dies during birth.[20] In Cambodia and Costa Rica, burial of the placenta is believed to protect and ensure the health of the baby and the mother.[21] If a mother dies in childbirth, the Aymara of Bolivia bury the placenta in a secret place so that the mother's spirit will not return to claim her baby's life.[22]
The placenta is believed by some communities to have power over the lives of the baby or its parents. The Kwakiutl of British Columbia bury girls' placentas to give the girl skill in digging clams, and expose boys' placentas to ravens to encourage future prophetic visions. In Turkey, the proper disposal of the placenta and umbilical cord is believed to promote devoutness in the child later in life. In Ukraine, Transylvania, and Japan, interaction with a disposed placenta is thought to influence the parents' future fertility.
Several cultures believe the placenta to be or have been alive, often a relative of the baby. Nepalese think of the placenta as a friend of the baby; Malaysian Orang Asli regard it as the baby's older sibling. The Ibo of Nigeria consider the placenta the deceased twin of the baby, and conduct full funeral rites for it.[21] Native Hawaiians believe that the placenta is a part of the baby, and traditionally plant it with a tree that can then grow alongside the child.[17]
In some cultures, the placenta is eaten, a practice known as placentophagy. In some eastern cultures, such as China and Hong Kong, the dried placenta (紫河車) is thought to be a healthful restorative and is sometimes used in preparations of traditional Chinese medicine and various health products.[23]
Additional images
-
Micrograph of a placental infection (CMV placentitis).
See also
References
- ^ Pough et al. 1992. Herpetology: Third Edition. Pearson Prentice Hall:Pearson Education, Inc., 2002.
- ^ Blackburn, D. G. and Flemming, A. F. (2011), Invasive implantation and intimate placental associations in a placentotrophic african lizard, Trachylepis ivensi (scincidae) Journal of Morphology. doi: 10.1002/jmor.11011
- ^ Henry George Liddell, Robert Scott, "A Greek-English Lexicon", at Perseus
- ^ Definitions of placental- related terms.
- ^ Examination of the placenta
- ^ Placental Structure and Classification
- ^ Placental blood circulation
- ^ a b Kiserud, T.; Acharya, G. (2004). "The fetal circulation". Prenatal Diagnosis 24 (13): 1049–1059. doi:10.1002/pd.1062. PMID 15614842.
- ^ Wright, Caroline; Sibley, Colin P. (2011). "Placental Transfer in Health and Disease". In Helen Kay, Michael Nelson, and Yuping Wang. The Placenta: From Development to Disease. John Wiley and Sons. pp. 66. ISBN 9781444333664.
- ^ Simister, N.E., and Story, C.M. 1997. "Human placental Fc receptors and the transmission of antibodies from mother to fetus." Journal of Reproductive Immunology 37: 1-23
- ^ Pillitteri, Adele(2010). Maternal and Child Health Nursing(6th Edition[Philippine Edition]): Lippincott Williams & Wilkins
- ^ "Placenta 'fools body's defences'". BBC News. 10 November 2007. http://news.bbc.co.uk/1/hi/health/7081298.stm.
- ^ Clark DA, Chaput A, Tutton D (March 1986). "Active suppression of host-vs-graft reaction in pregnant mice. VII. Spontaneous abortion of allogeneic CBA/J x DBA/2 fetuses in the uterus of CBA/J mice correlates with deficient non-T suppressor cell activity". J. Immunol. 136 (5): 1668–75. PMID 2936806.
- ^ Williams Z, Zepf D, Longtine J, et al. (March 2008). "Foreign fetal cells persist in the maternal circulation". Fertil. Steril. 91 (6): 2593–5. doi:10.1016/j.fertnstert.2008.02.008. PMID 18384774.
- ^ Assad, R. S.; Lee, F. Y.; Hanley, F. L. (2001). "Placental compliance during fetal extracorporeal circulation". Journal of applied physiology (Bethesda, Md. : 1985) 90 (5): 1882–1886. PMID 11299282.
- ^ Prendiville, W. J.; Elbourne, D.; McDonald, S. J.; Begley, C. M. (2000). Active versus expectant management in the third stage of labour. In Begley, Cecily M. "Cochrane Database of Systematic Reviews". Cochrane Database of Systematic Reviews (3). doi:10.1002/14651858.CD000007.
- ^ a b "Why eat a placenta?". BBC. 18 April 2006. http://news.bbc.co.uk/2/hi/uk_news/magazine/4918290.stm. Retrieved 8 January 2008.
- ^ Metge, Joan. 2005. "Working in/Playing with three languages: English, Te Reo Maori, and Maori Bod Language." In Sites N.S vol. 2, No 2:83-90.
- ^ Francisco, Edna (3 December 2004). "Bridging the Cultural Divide in Medicine". Minority Scientists Network. http://sciencecareers.sciencemag.org/career_development/previous_issues/articles/3360/bridging_the_cultural_divide_in_medicine/. Retrieved 7 January 2008.
- ^ Shepardson, Mary (1978). "Changes in Navajo Mortuary Practices and Beliefs". American Indian Quarterly. University of Nebraska Press. JSTOR 0095182x.[dead link]
- ^ a b Buckley, Sarah J.. "Placenta Rituals and Folklore from around the World". Mothering. Archived from the original on 6 January 2008. http://web.archive.org/web/20080106075807/http://www.mothering.com/articles/pregnancy_birth/birth_preparation/amazing_placenta_side.html. Retrieved 7 January 2008.
- ^ Davenport, Ann (June 2005). "The Love Offer". Johns Hopkins Magazine. http://www.jhu.edu/~jhumag/0605web/ruminate.html. Retrieved 7 January 2008.
- ^ Falcao, Ronnie. "Medicinal Uses of the Placenta". http://www.gentlebirth.org/archives/eatplcnt.html. Retrieved 25 November 2008.
External links
- Additional Human placenta photography
- The Placenta, gynob.com, with quotes from Williams Obstetrics, 18th Edition, F. Gary Cunningham, M.D., Paul C. MacDonald, M.D., Norman F. Grant, M.D., Appleton & Lange, Publishers.
Human systems and organs TA 2–4:
MSBone (Carpus · Collar bone (clavicle) · Thigh bone (femur) · Fibula · Humerus · Mandible · Metacarpus · Metatarsus · Ossicles · Patella · Phalanges · Radius · Skull (cranium) · Tarsus · Tibia · Ulna · Rib · Vertebra · Pelvis · Sternum) · CartilageTA 5–11:
splanchnic/
viscusMouth (Salivary gland, Tongue) · upper GI (Oropharynx, Laryngopharynx, Esophagus, Stomach) · lower GI (Small intestine, Appendix, Colon, Rectum, Anus) · accessory (Liver, Biliary tract, Pancreas)TA 12–16 Blood
(Non-TA)General anatomy: systems and organs, regional anatomy, planes and lines, superficial axial anatomy, superficial anatomy of limbsEmbryonic adnexa Trophoblast (Cytotrophoblast, Syncytiotrophoblast, Intermediate trophoblast)
Chorionic villi/Intervillous space · Amnion/Amniotic sac/Amniotic cavity
rostral embryonic ligament · caudal embryonic ligamentFetal membranes Circulatory Ungrouped Prenatal development/Mammalian development of circulatory system (GA 5, TE E5.11) Heart development Tubular heartSepta/ostiaAtrioventricular cushions/Septum intermedium · Primary interatrial foramen · Septum primum (Foramen secundum) · Septum secundum (Foramen ovale) · Aorticopulmonary septumOtherAtrioventricular canal · Primary interventricular foramenVasculogenesis,
angiogenesis,
and lymphangiogenesisBlood island of umbilical vesicle
Development of arteriesDevelopment of veinsDevelopment of lymph vesselsLymph sacsDevelopment of circulatory system about teeth near childrenanuli: Anulus sanguineus perienameleus · lacunae: Lacuna sanguinea supraenamelea (Ductus sanguineus mesialis · Ductus sanguineus distalis · Ductus sanguineus lingualis · Ductus sanguineus palatinus · Ductus sanguineus buccalis · Ductus sanguineus labialis), Lacuna sanguinea apicalis, Lacuna sanguinea periodontalis, Lacuna sanguinea parodontalis, Lacuna sanguinea gingivalisExtraembryonic
hemangiogenesisFetal circulation Categories:- Developmental biology
- Embryology of cardiovascular system
- Organs
- Greek loanwords
Wikimedia Foundation. 2010.