- Pancreas
-
For other uses, see Pancreas (disambiguation).
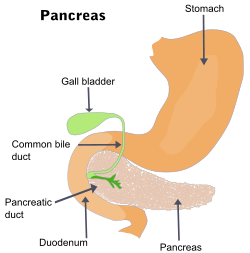
The pancreas /ˈpæŋkriəs/ is a gland organ in the digestive and endocrine system of vertebrates. It is both an endocrine gland producing several important hormones, including insulin, glucagon, and somatostatin, as well as a digestive organ, secreting pancreatic juice containing digestive enzymes that assist the absorption of nutrients and the digestion in the small intestine. These enzymes help to further break down the carbohydrates, proteins, and lipids in the chyme.
Contents
Histology
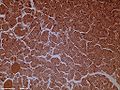
Under a microscope, stained sections of the pancreas reveal two different types of parenchymal tissue.[2] Lightly staining clusters of cells are called islets of Langerhans, which produce hormones that underlie the endocrine functions of the pancreas. Darker staining cells form acini connected to ducts. Acinar cells belong to the exocrine pancreas and secrete digestive enzymes into the gut via a system of ducts.
Structure Appearance Function Islets of Langerhans Lightly staining, large, spherical clusters Hormone production and secretion (endocrine pancreas) Pancreatic acini Darker staining, small, berry-like clusters Digestive enzyme production and secretion (exocrine pancreas) Function
See also: endocrine pancreas and exocrine pancreasThe pancreas is a dual-function gland, having features of both endocrine and exocrine glands.
The part of the pancreas with endocrine function is made up of approximately a million[3] cell clusters called islets of Langerhans. Four main cell types exist in the islets. They are relatively difficult to distinguish using standard staining techniques, but they can be classified by their secretion: α cells secrete glucagon (increase glucose in blood), β cells secrete insulin (decrease glucose in blood), δ cells secrete somatostatin (regulates/stops α and β cells), and PP cells secrete pancreatic polypeptide.[4]
The islets are a compact collection of endocrine cells arranged in clusters and cords and are crisscrossed by a dense network of capillaries. The capillaries of the islets are lined by layers of endocrine cells in direct contact with vessels, and most endocrine cells are in direct contact with blood vessels, by either cytoplasmic processes or by direct apposition. According to the volume The Body, by Alan E. Nourse,[5] the islets are "busily manufacturing their hormone and generally disregarding the pancreatic cells all around them, as though they were located in some completely different part of the body." The islet of Langerhans plays an imperative role in glucose metabolism and regulation of blood glucose concentration.
The pancreas as an exocrine gland helps out the digestive system. It secretes pancreatic fluid that contains digestive enzymes that pass to the small intestine. These enzymes help to further break down the carbohydrates, proteins, and lipids (fats) in the chyme.
In humans, the secretory activity of the pancreas is regulated directly via the effect of hormones in the blood on the islets of Langerhans and indirectly through the effect of the autonomic nervous system on the blood flow.[6]
- Sympathetic (adrenergic)
- α2: decreases secretion from beta cells, increases secretion from alpha cells, β2: increases secretion from beta cells
- Parasympathetic (muscarinic)
- M3: increases stimulation of alpha cells and beta cells[7]
Anatomy
 Surface projections of the organs of the trunk, showing pancreas at the transpyloric plane
Surface projections of the organs of the trunk, showing pancreas at the transpyloric plane
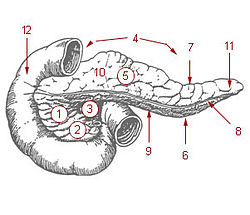
 1. Bile ducts: 2. Intrahepatic bile ducts, 3. Left and right hepatic ducts, 4. Common hepatic duct, 5. Cystic duct, 6. Common bile duct, 7. Ampulla of Vater, 8. Major duodenal papilla
1. Bile ducts: 2. Intrahepatic bile ducts, 3. Left and right hepatic ducts, 4. Common hepatic duct, 5. Cystic duct, 6. Common bile duct, 7. Ampulla of Vater, 8. Major duodenal papilla
9. Gallbladder, 10-11. Right and left lobes of liver. 12. Spleen.
13. Esophagus. 14. Stomach. Small intestine: 15. Duodenum, 16. Jejunum
17. Pancreas: 18: Accessory pancreatic duct, 19: Pancreatic duct.
20-21: Right and left kidneys (silhouette).
The anterior border of the liver is lifted upwards (brown arrow). Gallbladder with Longitudinal section, pancreas and duodenum with frontal one. Intrahepatic ducts and stomach in transparency.
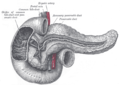
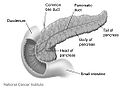
The pancreas lies in the epigastrium and left hypochondrium areas of the abdomenIt is composed of the following parts:
- The head lies within the concavity of the duodenum.
- The uncinate process emerges from the lower part of head, and lies deep to superior mesenteric vessels.
- The neck is the constricted part between the head and the body.
- The body lies behind the stomach.
- The tail is the left end of the pancreas. It lies in contact with the spleen and runs in the lienorenal ligament.
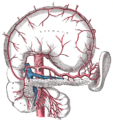
The superior pancreaticoduodenal artery from gastroduodenal artery and the inferior pancreaticoduodenal artery from superior mesenteric artery run in the groove between the pancreas and duodenum and supply the head of pancreas. The pancreatic branches of splenic artery also supply the neck, body and tail of the pancreas. The largest of those branches is called the arteria pancreatica magna; its occlusion, although rare, is fatal.
The body and neck of the pancreas drain into splenic vein; the head drains into the superior mesenteric and portal veins.
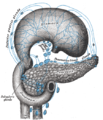
Lymph is drained via the splenic, celiac and superior mesenteric lymph nodes.
Diseases
Main article: Pancreatic diseaseBecause the pancreas is a storage depot for digestive enzymes, injury to the pancreas is potentially very dangerous. A puncture of the pancreas generally requires prompt and experienced medical intervention.
Pancreatic cancers, particularly cancer of the exocrine pancreas, remain one of the most deadly cancers, and the mortality rate is very high.
Diabetes mellitus type 1 is a chronic autoimmune disorder in which the immune system attacks the insulin-secreting cells in the pancreas.
History
The pancreas was first identified for western civilization by Herophilus (335–280 BC), a Greek anatomist and surgeon. Only a few hundred years later, Rufus of Ephesus, another Greek anatomist, gave the pancreas its name. The term "pancreas" is derived from the Greek πᾶν ("all", "whole"), and κρέας ("flesh")[8] – presumably because of its fleshy consistency.
Embryological development
 Schematic illustrating the development of the pancreas from a dorsal and a ventral bud. During maturation the ventral bud flips to the other side of the gut tube (arrow) where it typically fuses with the dorsal lobe. An additional ventral lobe which usually regress during development is omitted.
Schematic illustrating the development of the pancreas from a dorsal and a ventral bud. During maturation the ventral bud flips to the other side of the gut tube (arrow) where it typically fuses with the dorsal lobe. An additional ventral lobe which usually regress during development is omitted.
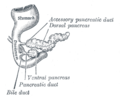
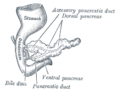
The pancreas forms from the embryonic foregut and is therefore of endodermal origin. Pancreatic development begins [with] the formation of a ventral and dorsal anlage (or buds). Each structure communicates with the foregut through a duct. The ventral pancreatic bud becomes the head and uncinate process, and comes from the hepatic diverticulum.
Differential rotation and fusion of the ventral and dorsal pancreatic buds results in the formation of the definitive pancreas.[9] As the duodenum rotates to the right, it carries with it the ventral pancreatic bud and common bile duct. Upon reaching its final destination, the ventral pancreatic bud fuses with the much larger dorsal pancreatic bud. At this point of fusion, the main ducts of the ventral and dorsal pancreatic buds fuse, forming the duct of Wirsung, the main pancreatic duct.
Differentiation of cells of the pancreas proceeds through two different pathways, corresponding to the dual endocrine and exocrine functions of the pancreas. In progenitor cells of the exocrine pancreas, important molecules that induce differentiation include follistatin, fibroblast growth factors, and activation of the Notch receptor system.[9] Development of the exocrine acini progresses through three successive stages. These include the predifferentiated, protodifferentiated, and differentiated stages, which correspond to undetectable, low, and high levels of digestive enzyme activity, respectively.
Progenitor cells of the endocrine pancreas arise from cells of the protodifferentiated stage of the exocrine pancreas.[9] Under the influence of neurogenin-3 and Isl-1, but in the absence of notch receptor signaling, these cells differentiate to form two lines of committed endocrine precursor cells. The first line, under the direction of Pax-0, forms α- and γ- cells, which produce glucagon and pancreatic polypeptides, respectively. The second line, influenced by Pax-6, produces β- and δ-cells, which secrete insulin and somatostatin, respectively.
Insulin and glucagon can be detected in the human fetal circulation by the fourth or fifth month of fetal development.[9]
In animals
Pancreatic tissue is present in all vertebrate species, but its precise form and arrangement vary widely. There may be up to three separate pancreases, two of which arise from ventral buds, and the other dorsally. In most species (including humans), these fuse in the adult, but there are several exceptions. Even when a single pancreas is present, two or three pancreatic ducts may persist, each draining separately into the duodenum (or equivalent part of the foregut). Birds, for example, typically have three such ducts.[10]
In teleosts, and a few other species (such as rabbits), there is no discrete pancreas at all, with pancreatic tissue being distributed diffusely across the mesentery and even within other nearby organs, such as the liver or spleen. In a few teleost species, the endocrine tissue has fused to form a distinct gland within the abdominal cavity, but otherwise it is distributed amongst the exocrine components. The most primitive arrangement, however, appears to be that of lampreys and lungfish, in which pancreatic tissue is found as a number of discrete nodules within the wall of the gut itself, with the exocrine portions being little different from other glandular structures of the intestine.[10]
Gallery
References
- ^ Physiology at MCG 6/6ch2/s6ch2_30
- ^ Histology at BU 10404loa
- ^ Hellman B, Gylfe E, Grapengiesser E, Dansk H, Salehi A (2007). "[Insulin oscillations--clinically important rhythm. Anti-diabetics should increase the pulsative component of the insulin release]" (in Swedish). Lakartidningen 104 (32–33): 2236–9. PMID 17822201.
- ^ BRS physiology 4th edition ,page 255-256, Linda S. Constanzo, Lippincott publishing
- ^ The Body, by Alan E. Nourse, in the Time-Life Science Library Series (op. cit., p. 171.)
- ^ "New Research Redraws Pancreas Anatomy". 7 July 2011. http://medicalxpress.com/news/2011-07-redraws-pancreas-anatomy.html.
- ^ Verspohl EJ, Tacke R, Mutschler E, Lambrecht G (1990). "Muscarinic receptor subtypes in rat pancreatic islets: binding and functional studies". Eur. J. Pharmacol. 178 (3): 303–311. doi:10.1016/0014-2999(90)90109-J. PMID 2187704.
- ^ Harper, Douglas. "Pancreas". Online Etymology Dictionary. http://www.etymonline.com/index.php?term=pancreas. Retrieved 2007-04-04.
- ^ a b c d Carlson, Bruce M. (2004). Human embryology and developmental biology. St. Louis: Mosby. pp. 372–4. ISBN 0-323-01487-9.
- ^ a b Romer, Alfred Sherwood; Parsons, Thomas S. (1977). The Vertebrate Body. Philadelphia, PA: Holt-Saunders International. pp. 357–359. ISBN 0-03-910284-X.
External links
Human systems and organs TA 2–4:
MSBone (Carpus · Collar bone (clavicle) · Thigh bone (femur) · Fibula · Humerus · Mandible · Metacarpus · Metatarsus · Ossicles · Patella · Phalanges · Radius · Skull (cranium) · Tarsus · Tibia · Ulna · Rib · Vertebra · Pelvis · Sternum) · CartilageTA 5–11:
splanchnic/
viscusmostly
Thoracicmostly
AbdominopelvicDigestive system+
adnexaMouth (Salivary gland, Tongue) · upper GI (Oropharynx, Laryngopharynx, Esophagus, Stomach) · lower GI (Small intestine, Appendix, Colon, Rectum, Anus) · accessory (Liver, Biliary tract, Pancreas)TA 12–16 Blood
(Non-TA)General anatomy: systems and organs, regional anatomy, planes and lines, superficial axial anatomy, superficial anatomy of limbsCategories:- Pancreas
- Organs
Wikimedia Foundation. 2010.