- Trophoblast
-
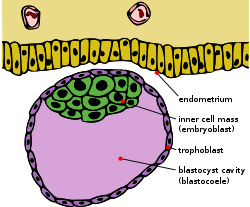
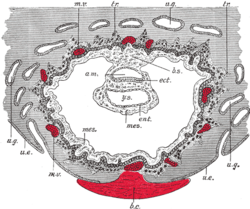
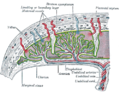
Trophoblast Blastocyst with an inner cell mass and trophoblast. Section through ovum imbedded in the uterine decidua. Semidiagrammatic.
am. Amniotic cavity.
b.c. Blood-clot.
b.s. Body-stalk.
ect. Embryonic ectoderm.
ent. Entoderm.
mes. Mesoderm.
m.v. Maternal vessels.
tr. Trophoblast.
u.e. Uterine epithelium.
u.g. Uterine glands.
y.s. Yolk-sac.Latin trophoblastus; massa cellularis externa Gray's subject #6 46 Days 6 Gives rise to caul Code TE E6.0.1.1.2.0.2 MeSH Trophoblasts Trophoblasts (from Greek trephein: to feed, and blastos: germinator) are cells forming the outer layer of a blastocyst, which provide nutrients to the embryo and develop into a large part of the placenta. They are formed during the first stage of pregnancy and are the first cells to differentiate from the fertilized egg. This layer of trophoblasts is also collectively referred to as "the trophoblast",[1] or, after gastrulation,[2] the trophectoderm, as it is then contiguous with the ectoderm of the embryo.
Contents
Function
Trophoblasts are specialised cells of the placenta that play an important role in embryo implantation and interaction with the decidualised maternal uterus. The core of placental villi contain mesenchymal cells and placental blood vessels that are directly connected to the fetal circulation via the umbilical cord. This core is surrounded by two layers of trophoblast; a single layer of mononuclear cytotrophoblast that fuse together to form the overlying multinucleated syncytiotrophoblast layer that covers the entire surface of the placenta. It is this syncytiotrophoblast that is in direct contact with the maternal blood that reaches the placental surface, and thus facilitates the exchange of nutrients, wastes and gases between the maternal and fetal systems.[citation needed]
In addition, cytotrophoblast in the tips of villi can differentiate into another type of trophoblast called the extravillous trophoblast. Extravillous trophoblast grow out from the placenta and penetrate into the decidualised uterus. This process is essential not only for physically attaching the placenta to the mother, but also for altering the vasculature in the uterus to allow it to provide an adequate blood supply to the growing fetus as pregnancy progresses. Some of these trophoblast even replace the endothelial cells in the uterine spiral arteries as they remodel these vessels into wide bore conduits that are independent of maternal vasoconstriction. This ensures the fetus receives a steady supply of blood, and the placenta is not subjected to fluctuations in oxygen that could cause it damage.[citation needed]
Differentiation
The trophoblast proliferates and differentiates into 2 cell layers at approximately 6 days after fertilization for humans:
Layer Location Description cytotrophoblast inner layer Single celled, inner layer of the trophoblast. syncytiotrophoblast outer layer Thick layer that lacks cell boundaries and grows into the endometrial stroma. It secretes hCG in order to maintain progesterone secretion and sustain a pregnancy. intermediate trophoblast (IT) implantation site, chorion, villi (dependent on subtype) anchor placenta (implanation site IT), unknown (chorionic & villus IT) Pathology
The invasion of a specific type of trophoblast (extravillous trophoblast) into the maternal uterus is a vital stage in the establishment of pregnancy:
- Failure of the trophoblast to invade sufficiently is important in the development of some cases of pre-eclampsia.
- Too firm an attachment may lead to placenta accreta.
Gestational trophoblastic disease represents a form of proliferation.
Additional images
-
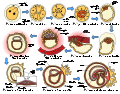
The initial stages of human embryogenesis
See also
References
External links
- Swiss embryology (from UL, UB, and UF) iperiodembry/carnegie02
- Oklahoma State
- University of Illinois
Embryonic adnexa Trophoblast (Cytotrophoblast, Syncytiotrophoblast, Intermediate trophoblast)
Chorionic villi/Intervillous space · Amnion/Amniotic sac/Amniotic cavity
rostral embryonic ligament · caudal embryonic ligamentFetal membranes Circulatory Ungrouped Categories:
Wikimedia Foundation. 2010.