- Oropharyngeal cancer
-
Oropharyngeal cancer 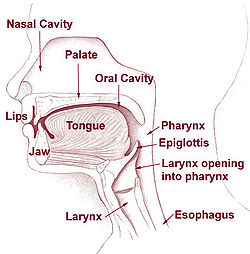
Head and neck. 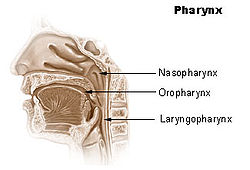
Pharynx Gray's subject #244 1141 Artery pharyngeal branches of ascending pharyngeal artery, ascending palatine, descending palatine, pharyngeal branches of inferior thyroid Vein pharyngeal veins Nerve pharyngeal plexus MeSH Pharynx Oropharyngeal cancer is a disease which malignant cells form in the tissue of oropharynx. Oropharynx is a middle part of the throat which includes the base of the tongue, the tonsils, the soft palate, and the walls of the pharynx.[1]
Contents
Studies
For patients with advanced oropharyngeal cancer the combination of radiotherapy and chemotherapy appears to be as efficient as surgical management. Shiley et al compared the maintenance of swallowing function with the two approaches. They studied 27 patients who underwent the advanced stage (III and IV) of oropharyngeal cancer. Among those patients, 67% had base of tongue lesions and 82% of them used gastrostomy tube either before or during the treatment. Three months after the chemoradiation, 33% of the patients were consuming all nutrition orally, 45% had some oral intake but still had the tube feeding, and 22% had no oral intake at all. The results showed that the short-term incidence of gastrostomy tube dependence after chemo radiation was similar to that after surgical management of oropharyngeal cancer at their institution.[2]
Symptoms
Following are the possible signs of oropharyngeal cancer. [3][1]
- A sore throat that persists
- Pain or difficulty with swallowing
- Unexplained weight loss
- Voice changes
- Ear pain
- A lump in the back of the throat or mouth
- A lump in the neck
- A dull pain behind the sternum
- Cough
Risk factors
Following are the risk factors that can increase the risk of developing oropharyngeal cancer. [3]
- Smoking and chewing tobacco.
- Heavy alcohol use.
- A diet low in fruits and vegetables.
- Chewing betel quid, a stimulant commonly used in parts of Asia.
- Being infected with human papilloma virus (HPV).
- EBV infection.
- plummer-Vinson syndrome.
- poor nutrition.
- P53 mutation
CONDITIONS ASSOCIATED WITH MALIGNANT TRANSFORMATION HIGH-risk lesions
- Erythroplakia
- speckled Erythroplakia
- Chronic hyperplastic candidiasis
Medium- risk lesions.
- oral submucosal fibrosis
- syphilitic glossitis
- sideropenic dysphagia (or paterson-kelly-brown syndrome)
low-risk lesions.
- oral lichen planus
- discoid lupus erythematosus
- discoid keratosis congenita.
Prognosis
The prognosis for people with oropharyngeal cancer depends on the age and health of the person and the stage of the disease. It is important for people with oropharyngeal cancer to have follow-up exams for the rest of their lives as cancer can occur in nearby areas. In addition, it is important to eliminate risk factors such as smoking and drinking alcohol, which increase the risk for second cancers.[1]
Spread
There are three ways of cancer spreading in the body.[3]
- Cancer invades the surrounding normal tissues.
- Cancer invades the lymph system and travels through the lymph vessels to other places in the body.
- Cancer invades the veins and capillaries and travels through the blood to other places in the body.
Stages
Stage 0 carcinoma in situ
Abnormal cells are found in the lining of the oropharynx, These may become cancer and spread into nearby normal tissue.
Stage 1
Cancer has formed and is 2 centimeters or smaller and has not spread outside the oropharynx.
Stage 2
Cancer has formed and is larger than 2 centimeters, but not larger than 4 centimeters. Also it has not yet spread outside the oropharynx.
Stage 3
- Cancer is larger than 4 centimeters and has not spread outside the oropharynx
- Any size and has spread to only one lymph node on the same side of the neck as the cancer. The lymph node with cancer is 3 centimeters or smaller.
Stage 4A
- Cancer has spread to tissues near the oropharynx, including the voice box, roof of the mouth, lower jaw, muscle of the tongue, or central muscles of the jaw, and may have spread to one or more nearby lymph nodes, none larger than 6 centimeters.
- Cancer is any size and has spread to one lymph node that is larger than 3 centimeters but not larger than 6 centimeters on the same side of the neck as the cancer, or to more than one lymph node, none larger than 6 centimeters, on one of both sides of the neck.
Stage 4B
- Cancer surrounds the main artery in the neck or has spread to bones in the jaw or skull, to muscle in the side of the jaw, or to the upper part of the throat behind the nose, and may have spread to nearby lymph nodes
- Cancer has spread to a lymph node that is larger than 6 centimeters and may have spread to tissues around the oropharynx.
Stage 4C
Cancer has spread to other parts of the body; the tumor may be any size and may have spread to lymph nodes.
- Glossary
Further information: List of oncology-related termsSociety and culture
In 2010 American actor Michael Douglas reported to have oropharyngeal cancer.[4]
See also
- HPV-positive oropharyngeal cancer
- Cancer
- Head and neck cancer
- Cancer of the larynx
- Thyroid cancer
- Oropharynx
- Larynx
- Human pharynx
References
- ^ a b c "Oropharyngeal Cancer Overview". Cleveland Clinic. 9/7/2007. http://my.clevelandclinic.org/disorders/Oropharyngeal_Cancer/hic_Oropharyngeal_Cancer.aspx. Retrieved 2011-04-18.
- ^ Shiley SG; Hargunani CA; Skoner JM; Holland JM; Wax MK (March 2006). "Swallowing Function after Chemoradiation for Advanced Stage Oropharyngeal Cancer". Otolaryngol Head Neck Surgery 134 (3): 455–9. PMID 16500444.
- ^ a b c d "Oropharyngeal Cancer Treatment (PDQ®)". National Cancer Institute. http://www.cancer.gov/cancertopics/pdq/treatment/oropharyngeal/patient/. Retrieved 2011-04-18.
- ^ DeNoon, Daniel J. (September 1, 2010). "Michael Douglas and Throat Cancer FAQ". WebMD Health News. WebMD. http://www.webmd.com/cancer/news/20100901/throat-cancer-faq. Retrieved 2011-04-18.
Further reading
Pathology: Tumor, Neoplasm, Cancer, and Oncology (C00–D48, 140–239) Conditions Malignant progressionTopographyHead/Neck (Oral, Nasopharyngeal) · Digestive system · Respiratory system · Bone · Skin · Blood · Urogenital · Nervous system · Endocrine systemHistologyOtherPrecancerous condition · Paraneoplastic syndromeStaging/grading Carcinogenesis Misc. M: NEO
tsoc, mrkr
tumr, epon, para
drug (L1i/1e/V03)
Tumors of lip, oral cavity and pharynx / head and neck cancer (C00–C14/D10–D11, 140–149/210) Oral cancer malignant epithelial tumors (Acinic cell carcinoma, Mucoepidermoid carcinoma, Adenoid cystic carcinoma, Salivary duct carcinoma, Epithelial-myoepithelial carcinoma)benign epithelial tumors (Pleomorphic adenoma, Warthin's tumor)Head and neck, upper RT: Nose (TA A06.1, TH H3.05.01, GA 10.992) External nose Ala of nose
nasal cartilages (of the septum, Greater alar, Lesser alar, Lateral nasal, Accessory nasal, Vomeronasal)Nasal cavity OpeningsLateral wallNasal concha/meati: Superior nasal concha · Middle nasal concha · Inferior nasal concha · Superior nasal meatus · Middle nasal meatus · Inferior nasal meatus
Sphenoethmoidal recess · Ethmoid bulla · Agger nasi · Ethmoidal infundibulum · Semilunar hiatus · Maxillary hiatusMedial wallParanasal sinuses Naso-pharynx Head and neck anatomy, digestive system: Mouth anatomy (TA A05.1–2, TH H3.04.01, GA 11.1110–2, 1125–1141) Mouth Lip (Upper, Lower, Vermilion border, Frenulum of lower lip, Labial commissure of mouth, Philtrum)
Cheek (Buccal fat pad)Interdental papilla · Gingival sulcus · Gingival margin · Free gingival margin · Gingival fibers · Junctional epithelium · Mucogingival junction · Sulcular epithelium · Stippling
Periodontium: Cementum · Gingiva · Periodontal ligamentTeethsee tooth anatomydorsum (Taste bud, Median sulcus, Terminal sulcus, Foramen cecum, Lingual tonsils) · underside (Frenulum, Fimbriated fold, Sublingual caruncle) · Anterior · Posterior · Glossoepiglottic folds · Lingual septumOro-pharynx/
faucesCategories:
Wikimedia Foundation. 2010.
