- Norepinephrine transporter
-
Solute carrier family 6 (neurotransmitter transporter, noradrenalin), member 2 Identifiers Symbols SLC6A2; NAT1; NET; NET1; SLC6A5 External IDs OMIM: 163970 MGI: 1270850 HomoloGene: 816 GeneCards: SLC6A2 Gene Gene Ontology Molecular function • norepinephrine:sodium symporter activity
• monoamine transmembrane transporter activity
• symporter activityCellular component • membrane fraction
• plasma membrane
• integral to plasma membraneBiological process • transport
• neurotransmitter transport
• synaptic transmission
• monoamine transport
• transmembrane transportSources: Amigo / QuickGO RNA expression pattern 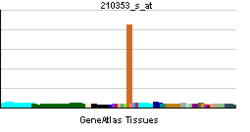
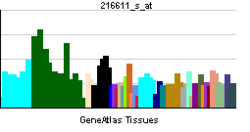
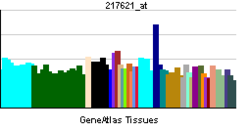
More reference expression data Orthologs Species Human Mouse Entrez 6530 20538 Ensembl ENSG00000103546 ENSMUSG00000055368 UniProt P23975 Q6NZB4 RefSeq (mRNA) NM_001043.3 NM_009209.3 RefSeq (protein) NP_001034.1 NP_033235.3 Location (UCSC) Chr 16:
55.67 – 55.74 MbChr 8:
95.48 – 95.53 MbPubMed search [1] [2] The norepinephrine transporter (NET), also known as solute carrier family 6 member 2 (SLC6A2), is a protein that in humans is encoded by the SLC6A2 gene.[1]
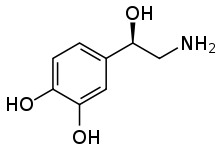
NET is a monoamine transporter and is responsible for the Na+/Cl–-dependent reuptake of extracellular norepinephrine (NE). NET can also reuptake extracellular dopamine (DA). The reuptake of these two neurotransmitters is essential in regulating concentrations in the synaptic cleft. NETs, along with the other monoamine transporters, are the targets of many antidepressants and recreational drugs. In addition, a deficiency of NET is associated with many affective and autonomic disorders such as orthostatic intolerance and ADHD.[2][3] There is evidence that single-nucleotide polymorphisms in the NET gene (SLC6A2) may be an underlying factor in some of these disorders.[3]
Contents
Gene
The norepinephrine transporter gene, SLC6A2 is located on human chromosome 16 locus 16q12.2. This gene is encoded by 14 exons.[3] Based on the nucleotide and amino acid sequence, the NET transporter consists of 617 amino acids with 12 membrane-spanning domains. The structural organization of NET is highly homologous to other members of a sodium/chloride-dependent family of neurotransmitter transporters, including dopamine, epinephrine, serotonin and GABA transporters.[3]
Single nucleotide polymorphisms
A single-nucleotide polymorphism (SNP) is a genetic variation in which a genome sequence is altered by a single nucleotide (A, T, C or G). NET proteins with an altered amino acid sequence (more specifically, a missense mutation) could potentially be associated with various diseases that involve abnormally high or low plasma levels of norepinephrine due to altered NET function. NET SNPs and possible associations with various diseases are an area of focus for many research projects. There is evidence suggesting a relationship between NET SNPs and various disorders such as ADHD[4][3] psychiatric disorders,[3] postural tachycardia[3][5] and orthostatic intolerance.[3][5] The SNPs rs3785143 and rs11568324 have been related to attention-deficit hyperactivity disorder.[6] Thus far, however, the only confirmed direct association between a SNP and a clinical condition is that of the SNP, Ala457Pro, and orthostatic intolerance.[3] Thirteen NET missense mutations have been discovered so far.[3]
Missense Mutations in the NET Gene[3][7] Location Amino Acid Variant Related Disease Exon 2 Val69Ile None Exon 3 Thr99Ile None Exon 5 Val245Ile None Exon 6 Asn292Thr None Exon 8 Val356Leu None Exon 8 Ala369Pro None Exon 8 Asn375Ser None Exon 10 Val449Ile None Exon 10 Ala457Pro Orthostatic intolerance Exon 10 Lys463Arg None Exon 11 Gly478Ser None Exon 12 Phe528Cys None Exon 13 Tyr548His None For the table above, refer to this table of standard amino acid abbreviations. This notation
for missense mutations, take Val69Ile for example, indicates that amino acid Val69 was changed to Ile.Genetic variations
An epigenetic mechanism (hypermethylation of CpG islands in the NET gene promoter region) that results in reduced expression of the noradrenaline transporter and consequently a phenotype of impaired neuronal reuptake of norepinephrine has been implicated in both postural orthostatic tachycardia syndrome and panic disorder.[8]
Structure
The norepinephrine transporter is composed of 12 transmembrane domains (TMDs). The intracellular portion contains an amino (-NH2) group and carboxyl (-COOH) group. In addition, there is a large extracellular loop located between TMD 3 and 4.[9][10][11] The protein is composed of 617 amino acids.[9]
Function
NET functions to transport synaptically released norepinephrine back into the presynaptic neuron. As much as 90% of the norepinephrine released will be taken back up in the cell by NET. NET functions by coupling the influx of Na+ and Cl– with the transport of norepinephrine. This occurs at a fixed ratio of 1:1:1.[12] Both NET and DAT can transport norepinephrine and dopamine. The reuptake of norepinephrine and dopamine is essential in regulating the concentration of monoamine neurotransmitters in the synaptic cleft. The transporter also helps maintain homeostatic balances of the presynaptic neuron.[13]
Norepinephrine (NE) is released from noradrenergic neurons that innervate both the CNS and PNS. NE, or noradrenaline (NA), has an important role in controlling mood, arousal, memory, learning, and pain perception. NE is a part of the sympathetic nervous system.[10][14] Dysregulation of the removal of norepinephrine by NET is associated with many neuropsychiatric diseases. In addition, any antidepressants and recreational drugs compete for the binding of NET with NE.[9]
Transport mechanisms
The transport of norepinephrine back into presynaptic cell is made possible by the cotransport with Na&2B and Cl%2B. The sequential binding of the ions results in the eventual reuptake of norepinephrine. The ion gradients of Na%2B and Cl%2B make this reuptake energetically favorable. The gradient is generated by the Na+/K+-ATPase which transports three sodium ions out and two potassium ions into the cell.[13] NETs have conductances similar to those of ligand gated ion channels. The expression of NET results in a leak-channel activity.[12][13]
Location in the nervous system
NETs are restricted to the noradrenergic neurons and are not present on neurons that release dopamine or epinephrine.[11][10][13] The transporters can be found along the cell body, axons, and dendrites of the neuron.[10] NETs are located away from the synapse, where norepinephrine is released, closer to the plasma membrane of the cell. This requires norepinephrine to diffuse from the site it is released to the transporter for reuptake.[13] Norepinephrine transporters are confined to the nerves of the sympathetic system, and those innervating the adrenal medulla, lung, and placenta.[13]
Regulation
Regulation of NET function is complex and a focus of current research. NETs are regulated at both the cellular and molecular level post-translation. The most understood mechanisms include phosphorylation by the second messenger protein kinase C (PKC).[11] PKC has been shown to inhibit NET function by sequestration of the transporter from the plasma membrane.[15] The amino acid sequence of NET has shown multiple sites related to protein kinase phosphorylation.[13] Post-translational modifications can have a wide range of effects on the function of the NET, including the rate of fusion of NET-containing vesicles with the plasma membrane, and transporter turnover.[15]
Clinical significance
Orthostatic intolerance
Main article: Orthostatic intoleranceOrthostatic intolerance (OI) is a disorder of the autonomic nervous system (a subcategory of dysautonomia) characterized by the onset of symptoms upon standing. Symptoms include fatigue, lightheadedness, headache, weakness, increased heart rate/heart palpitations, anxiety, and altered vision.[3] Oftentimes, patients have high plasma norepinephrine (NE) concentrations (at least 600 pg/ml) in relation to sympathetic outflow upon standing, suggesting OI is a hyperadrenergic condition.[3][5] The discovery of identical twin sisters both suffering from OI suggested a genetic basis for the disorder.[3][5] A missense mutation on the NET gene (SLC62A) was discovered in which an alanine residue was replaced with a proline residue (Ala457Pro) in a highly conserved region of the transporter.[3] The patients’ defective NET had only 2% of the activity of the wild-type version of the gene.[3] The genetic defect in the NET protein results in decreased NET activity that could account for abnormally high NE plasma levels in OI. However, 40 other OI patients did not have the same missense mutation, indicating other factors contributed to the phenotype in the identical twins.[3] This discovery of the linkage with NET mutations that results in decreased norepinephrine reuptake activity and orthostatic intolerance suggests faulty NE uptake mechanisms can contribute to cardiovascular disease.[16]
Therapeutic uses
"The involvement of the norepinephrine transporter (NET) in the pathophysiology and treatment of attention deficit hyperactivity disorder (ADHD), substance abuse, neurodegenerative disorders (e.g., Alzheimer's disease (AD) and Parkinson's disease (PD)) and clinical depression has long been recognized. [2006]"[17]
Depression
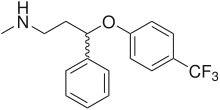
Main article: DepressionCertain antidepressant medications act to raise noradrenaline, such as serotonin-norepinephrine reuptake inhibitors (SNRIs), norepinephrine-dopamine reuptake inhibitors (NDRIs), norepinephrine reuptake inhibitors (NRIs or NERIs) and the tricyclic antidepressants (TCAs). These medications prevent NET from functioning normally, resulting in higher extracellular concentrations of NE. Noradrenaline therefore remains in the synapse longer, allowing it to reach more normal levels. Since the noradrenaline transporter is responsible for most of the dopamine clearance in the prefrontal cortex,[18] SNRIs would also raise dopamine levels in synapses there. However, dopamine in most brain regions is cleared primarily by the dopamine transporter, which works roughly ten times faster.[19] For many years, the number one choice in treating mood disorders like depression was through the uptake of TCAs, such as desipramine (Norpramin), nortriptyline (Arentyl, Pamelor), protriptyline (Vivactil) and amoxapine (Asendin).[20] However, currently far more potent drugs have been developed in the US, most notably the discovery of selective serotonin reuptake inhibitors (SSRIs). SSRIs affect the communication between chemical messengers in the brain by regulating how much of a certain chemical messenger enters the brain.[20] SSRIs regulate serotonin levels in the brain, which seems to aid the brain in exchanging messages more efficiently and in turn livens mood.[21] Drugs such as fluoxetine and paroxetine are both very impelling in treating mood disorders because they reduce many of the side effects one receives compared to using TCAs to treat such mood disorders.[21]
ADHD
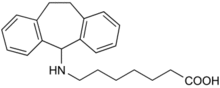
Main article: ADHD Atomoxetine, an NET inhibitor marketed as Strattera
Atomoxetine, an NET inhibitor marketed as Strattera
The strong NET inhibitor atomoxetine (Strattera) has been approved by the FDA to treat ADHD in adults.[22][23] It works to increase one's ability to focus, decrease any impulsiveness, and lessen hyperactivity in both children and adults who suffer from ADHD.[24] It is the first ADHD drug to be developed that reduces any risk of substance abuse for patients who continually take atomoxetine for their ADHD. The FDA approved another drug called Vyvanse specifically prescribed to children between the ages of 6 and 12 to treat ADHD. Both drugs for adults and children had common side effects similar to decreased appetite, bad sleeping habits, stomachaches and headaches.[22] Other common drugs that have been previously prescribed to treat ADHD in adults and children include Methylphenidate (Ritalin, Metadate, Concerta, Daytrana), Amphetamine (Adderall) and Dextroamphetamine (Dexadrine, Detrostat).[22]
Schizophrenia
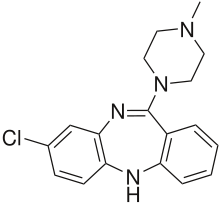
Main article: SchizophreniaThe role of NE in schizophrenia has not been fully understood, but has stimulated research into this topic.[25] The only relationship that has been understood between researchers is that there is a positive correlation between increased NE levels in the brain and activity of schizophrenia.[25] Before the age of modern treatment of schizophrenia, patients that were mentally ill were not treated and instead that were hidden away in their homes.[25] Old treatments often included sedatives, electroconvulsive therapy (ECT), artificially induced comas and frontal lobotomies.[25] Unfortunately, the side effects of these treatments usually outweighed the therapeutic benefits of these treatments.[25] The first breakthrough for schizophrenia treatment was the discovery of the antipsychotic drug called Chlorpromazine (CPZ) in 1979, which is still in common use today.[25] Another drug developed from the class of atypical antipsychotic drug called Clozapine.[26] This drug works to help patients who have tried to injure/kill themselves before from getting no prior treatment. It works similarly to SSRIs by regulating the concentrations of certain chemical messengers in the brain.[26]
Psychostimulants
Cocaine
Main article: CocaineCocaine is a powerful psychostimulant and known to be one of the most widely abused substances.[27] Cocaine is a nonselective, competitive antagonist of norepinephrine, serotonin, and dopamine transport. This thwarts the absorption of these chemicals into the presynaptic terminal[27] and allows a large concentration of dopamine, serotonin and norepinephrine to build up in the cell. The potential for cocaine addiction is thought to be a result of its effects on dopamine transporters in the CNS, while it has been suggested that the life-threatening cardiovascular effects of cocaine may involve the inhibition of NETs at sympathetic and CNS autonomic synapses.[28]
Amphetamines
Main article: AmphetamineAmphetamines have a similar effect on norepinephrine levels compared to that of cocaine in that they both increase NE levels in the brain.[29] Amphetamine-like drugs are substrates for monoamine transporters, include NET, that cause a reversal in the direction of neurotransmitter transport.[13][30] Amphetamines cause a large accumulation of extracellular NE.[29] High levels of NE in the brain account for most of the profound effects of amphetamines, including alertness, anorectic, locomotor and sympathomimetic effects.[29] However, the effects that amphetamines have on the brain are slower but last longer than the effects cocaine has on the brain.[29] MDMA (3,4-Methylenedioxymethamphetamine or "ecstacy") is an amphetamine with wide recreational use. A study reported that the NET inhibitor Reboxetine reduced the stimulant effects of MDMA in humans, demonstrating the crucial role NET has in the cardiovascular and stimulant-like effects of MDMA.[31]
Further research
NETs role in many brain disorders underlies the importance of understanding the (dys)regulation of the transporter. A complete model of the proteins that associate with the transporter will be useful in designing drug therapies for diseases such as schizophrenia, affective disorder, and autonomic disorders. Recently discovered mechanisms of the NET, including the ability to act reversibly and as an ion channel, provide other areas of research.[13][11]
See also
- Neurotransmitter transporter
- Sodium:neurotransmitter symporter
- Solute carrier family
- Norepinephrine
- Monoamine transporter
- Orthostatic intolerance
- Single-nucleotide polymorphisms
References
- ^ Pacholczyk T, Blakely RD, Amara SG (March 1991). "Expression cloning of a cocaine- and antidepressant-sensitive human noradrenaline transporter". Nature 350 (6316): 350–4. doi:10.1038/350350a0. PMID 2008212.
- ^ S. Schroeter, S. Apparsundaram, R. G. Wiley, L. H. Miner, S. R. Sesack & R. D. Blakely (May 2000). "Immunolocalization of the cocaine- and antidepressant-sensitive l-norepinephrine transporter". The Journal of comparative neurology 420 (2): 211–232. PMID 10753308.
- ^ a b c d e f g h i j k l m n o p q Tellioglu T, Robertson D (November 2001). "Genetic or acquired deficits in the norepinephrine transporter: current understanding of clinical implications". Expert Rev Mol Med 2001 (29): 1–10. doi:10.1017/S1462399401003878. PMID 14987367.
- ^ Kim CH, Hahn MK, Joung Y, Anderson SL, Steele AH, Mazei-Robinson MS, Gizer I, Teicher MH, Cohen BM, Robertson D, Waldman ID, Blakely RD, Kim KS (December 2006). "A polymorphism in the norepinephrine transporter gene alters promoter activity and is associated with attention-deficit hyperactivity disorder". Proc. Natl. Acad. Sci. U.S.A. 103 (50): 19164–9. doi:10.1073/pnas.0510836103. PMC 1748193. PMID 17146058. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=1748193.
- ^ a b c d Shannon JR, Flattem NL, Jordan J, Jacob G, Black BK, Biaggioni I, Blakely RD, Robertson D (February 2000). "Orthostatic intolerance and tachycardia associated with norepinephrine-transporter deficiency". N. Engl. J. Med. 342 (8): 541–9. doi:10.1056/NEJM200002243420803. PMID 10684912.
- ^ Kim JW, Biederman J, McGrath CL, Doyle AE, Mick E, Fagerness J, Purcell S, Smoller JW, Sklar P, Faraone SV (June 2008). "Further evidence of association between two NET single-nucleotide polymorphisms with ADHD". Mol. Psychiatry 13 (6): 624–30. doi:10.1038/sj.mp.4002090. PMID 17876324.
- ^ Maarten E. A. Reith (2002). Neurotransmitter transporters: structure, function, and regulation. Humana Press. p. 120. ISBN 978-0-89603-945-2. http://books.google.com/books?id=tp8vVbk-2IMC&pg=PA120. Retrieved 27 October 2011.
- ^ Esler M, Alvarenga M, Pier C, Richards J, El-Osta A, Barton D, Haikerwal D, Kaye D, Schlaich M, Guo L, Jennings G, Socratous F, Lambert G (2006). "The neuronal noradrenaline transporter, anxiety and cardiovascular disease". J Psychopharmacol 20 (4 Suppl): 60–6. doi:10.1177/1359786806066055. PMID 16785272.
- ^ a b c Stöber G, Nöthen MM, Pörzgen P, Brüss M, Bönisch H, Knapp M, Beckmann H, Propping P (November 1996). "Systematic search for variation in the human norepinephrine transporter gene: identification of five naturally occurring missense mutations and study of association with major psychiatric disorders". Am. J. Med. Genet. 67 (6): 523–32. doi:10.1002/(SICI)1096-8628(19961122)67:6<523::AID-AJMG3>3.0.CO;2-I. PMID 8950409.
- ^ a b c d Schroeter S, Apparsundaram S, Wiley RG, Miner LH, Sesack SR, Blakely RD (May 2000). "Immunolocalization of the cocaine- and antidepressant-sensitive l-norepinephrine transporter". J. Comp. Neurol. 420 (2): 211–32. PMID 10753308.
- ^ a b c d Sager JJ, Torres GE (August 2011). "Proteins interacting with monoamine transporters: current state and future challenges". Biochemistry 50 (34): 7295–310. doi:10.1021/bi200405c. PMID 21797260.
- ^ a b Galli A, DeFelice LJ, Duke BJ, Moore KR, Blakely RD (October 1995). "Sodium-dependent norepinephrine-induced currents in norepinephrine-transporter-transfected HEK-293 cells blocked by cocaine and antidepressants". J. Exp. Biol. 198 (Pt 10): 2197–212. PMID 7500004.
- ^ a b c d e f g h i Torres GE, Gainetdinov RR, Caron MG (January 2003). "Plasma membrane monoamine transporters: structure, regulation and function". Nat. Rev. Neurosci. 4 (1): 13–25. doi:10.1038/nrn1008. PMID 12511858.
- ^ Zhou J (December 2004). "Norepinephrine transporter inhibitors and their therapeutic potential". Drugs Future 29 (12): 1235–1244. PMC 1518795. PMID 16871320. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=1518795.
- ^ a b Gether U, Andersen PH, Larsson OM, Schousboe A (July 2006). "Neurotransmitter transporters: molecular function of important drug targets". Trends Pharmacol. Sci. 27 (7): 375–83. doi:10.1016/j.tips.2006.05.003. PMID 16762425.
- ^ Schroeder C, Tank J, Boschmann M, Diedrich A, Sharma AM, Biaggioni I, Luft FC, Jordan J (January 2002). "Selective norepinephrine reuptake inhibition as a human model of orthostatic intolerance". Circulation 105 (3): 347–53. doi:10.1161/hc0302.102597. PMID 11804991.
- ^ Information Hyperlinked Over Proteins (IHOP)
- ^ Morón JA, Brockington A, Wise RA, Rocha BA, Hope BT (January 2002). "Dopamine uptake through the norepinephrine transporter in brain regions with low levels of the dopamine transporter: evidence from knock-out mouse lines". J. Neurosci. 22 (2): 389–95. PMID 11784783.
- ^ Yavich L, Forsberg MM, Karayiorgou M, Gogos JA, Männistö PT (September 2007). "Site-specific role of catechol-O-methyltransferase in dopamine overflow within prefrontal cortex and dorsal striatum". J. Neurosci. 27 (38): 10196–209. doi:10.1523/JNEUROSCI.0665-07.2007. PMID 17881525.
- ^ a b Zhou J (December 2004). "Norepinephrine transporter inhibitors and their therapeutic potential". Drugs Future 29 (12): 1235–1244. PMC 1518795. PMID 16871320. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=1518795.
- ^ a b Mayo Clinic Staff, Selective serotonin reuptake inhibitors (SSRIs), http://www.mayoclinic.com/health/ssris/MH00066, retrieved 1 November 2011
- ^ a b c "What medications are used to treat ADHD?". National Institutes of Mental Health. http://www.nimh.nih.gov/health/publications/mental-health-medications/what-medications-are-used-to-treat-adhd.shtml.
- ^ Simpson D, Plosker GL (2004). "Atomoxetine: a review of its use in adults with attention deficit hyperactivity disorder". Drugs 64 (2): 205–22. PMID 14717619.
- ^ "Atomoxetine -". PubMed Health. http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0000222/.
- ^ a b c d e f Decaire, Michael, The neurophysiology of schizophrenia: Etiology and Psychopharmacological treatment, http://www.uplink.com.au/lawlibrary/Documents/Docs/Doc25.html, retrieved 1 November 2011
- ^ a b AHFS Consumer Medication Information, Clozapine, http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0000893/, retrieved 1 November 2011
- ^ a b Macey DJ, Smith HR, Nader MA, Porrino LJ (January 2003). "Chronic cocaine self-administration upregulates the norepinephrine transporter and alters functional activity in the bed nucleus of the stria terminalis of the rhesus monkey". J. Neurosci. 23 (1): 12–6. PMID 12514195.
- ^ Barker EL, Blakely RD (1995). "Norepinephrine and Serotonin Transporters". In Kupfer DJ, Bloom FE. Psychopharmacology: the fourth generation of progress. New York: Raven Press. ISBN 0-7817-0166-X. http://www.acnp.org/g4/GN401000029/CH029.html. Retrieved 2011-11-02.
- ^ a b c d Drug and Human Performance Fact Sheets, Methamphetamine (And Amphetamine), http://www.nhtsa.gov/people/injury/research/job185drugs/methamphetamine.htm, retrieved 1 November 2011
- ^ Sulzer D, Chen TK, Lau YY, Kristensen H, Rayport S, Ewing A (May 1995). "Amphetamine redistributes dopamine from synaptic vesicles to the cytosol and promotes reverse transport". J. Neurosci. 15 (5 Pt 2): 4102–8. PMID 7751968.
- ^ Hysek CM, Simmler LD, Ineichen M, Grouzmann E, Hoener MC, Brenneisen R, Huwyler J, Liechti ME (August 2011). "The norepinephrine transporter inhibitor reboxetine reduces stimulant effects of MDMA ("ecstasy") in humans". Clin. Pharmacol. Ther. 90 (2): 246–55. doi:10.1038/clpt.2011.78. PMID 21677639.
External links
By group SLC1–10 - (6) sodium- and chloride- dependent sodium:neurotransmitter symporters (SLC6A1, SLC6A2, SLC6A3, SLC6A4, SLC6A5, SLC6A6, SLC6A7, SLC6A8, SLC6A9, SLC6A10, SLC6A11, SLC6A12, SLC6A13, SLC6A14, SLC6A15, SLC6A16, SLC6A17, SLC6A18, SLC6A19, SLC6A20)
- (7) cationic amino-acid transporter/glycoprotein-associated (SLC7A1, SLC7A2, SLC7A3, SLC7A4) glycoprotein-associated/light or catalytic subunits of heterodimeric amino-acid transporters (SLC7A5, SLC7A6, SLC7A7, SLC7A8, SLC7A9, SLC7A10, SLC7A11, SLC7A13, SLC7A14)
- (8) Na+/Ca2+ exchanger (SLC8A1, SLC8A2, SLC8A3)
SLC11–20 - (12) electroneutral cation-Cl cotransporter (SLC12A1, SLC12A1, SLC12A2, SLC12A3, SLC12A4, SLC12A5, SLC12A6, SLC12A7, SLC12A8, SLC12A9)
- (14) urea transporter (SLC14A1, SLC14A2)
- (15) proton oligopeptide cotransporter (SLC15A1, SLC15A2, SLC15A3, SLC15A4)
- (16) monocarboxylate transporter (SLC16A1, SLC16A2, SLC16A3, SLC16A4, SLC16A5, SLC16A6, SLC16A7, SLC16A8, SLC16A9, SLC16A10, SLC16A11, SLC16A12, SLC16A13, SLC16A14)
SLC21–30 - (21) organic anion transporting (SLCO1A2, SLCO1B1, SLCO1B3, SLCO1B4, SLCO1C1) (SLCO2A1, SLCO2B1) (SLCO3A1) (SLCO4A1, SLCO4C1) (SLCO5A1) (SLCO6A1)
- (22) organic cation/anion/zwitterion transporter (SLC22A1, SLC22A2, SLC22A3, SLC22A4, SLC22A5, SLC22A6, SLC22A7, SLC22A8, SLC22A9, SLC22A10, SLC22A11, SLC22A12, SLC22A13, SLC22A14, SLC22A15, SLC22A16, SLC22A17, SLC22A18, SLC22A19, SLC22A20)
- (24) Na+/(Ca2+-K+) exchanger (SLC24A1, SLC24A2, SLC24A3, SLC24A4, SLC24A5, SLC24A6)
- (25) mitochondrial carrier (SLC25A1, SLC25A2, SLC25A3, SLC25A4, SLC25A5, SLC25A6, SLC25A7, SLC25A8, SLC25A9, SLC25A10, SLC25A11, SLC25A12, SLC25A13, SLC25A14, SLC25A15, SLC25A16, SLC25A17, SLC25A18, SLC25A19, SLC25A20, SLC25A21, SLC25A22, SLC25A23, SLC25A24, SLC25A25, SLC25A26, SLC25A27, SLC25A28, SLC25A29, SLC25A30, SLC25A31, SLC25A32, SLC25A33, SLC25A34, SLC25A35, SLC25A36, SLC25A37, SLC25A38, SLC25A39, SLC25A40, SLC25A41, SLC25A42, SLC25A43, SLC25A44, SLC25A45, SLC25A46)
SLC31–40 - (32) vesicular inhibitory amino-acid transporter (SLC32A1)
- (33) Acetyl-CoA transporter (SLC33A1)
- (35) nucleoside-sugar transporter (SLC35A1, SLC35A2, SLC35A3, SLC35A4, SLC35A5) (SLC35B1, SLC35B2, SLC35B3, SLC35B4) (SLC35C1, SLC35C2) (SLC35D1, SLC35D2, SLC35D3) (SLC35E1, SLC35E2, SLC35E3, SLC35E4)
- (36) proton-coupled amino-acid transporter (SLC36A1, SLC36A2, SLC36A3, SLC36A4)36A2 ·
- (37) sugar-phosphate/phosphate exchanger (SLC37A1, SLC37A2, SLC37A3, SLC37A4)
- (38) System A & N, sodium-coupled neutral amino-acid transporter (SLC38A1, SLC38A2, SLC38A3, SLC38A4, SLC38A5, SLC38A6, SLC38A10)
- (39) metal ion transporter (SLC39A1, SLC39A2, SLC39A3, SLC39A4, SLC39A5, SLC39A6, SLC39A7, SLC39A8, SLC39A9, SLC39A10, SLC39A11, SLC39A12, SLC39A13, SLC39A14)
- (40) basolateral iron transporter (SLC40A1)
SLC41–48 SLCO1–4 Ion pumps Vesicular Other Categories:- Human proteins
- Membrane biology
- Neurotransmitter transporters
- Solute carrier family
Wikimedia Foundation. 2010.