- Primary biliary cirrhosis
-
Primary biliary cirrhosis Classification and external resources 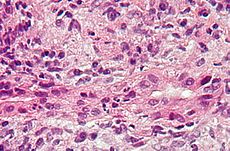
Micrograph of primary biliary cirrhosis showing bile duct inflammation and injury. H&E stain.ICD-10 K74.3 ICD-9 571.6 OMIM 109720 DiseasesDB 10615 eMedicine med/223 MeSH D008105 Primary biliary cirrhosis, often abbreviated PBC, is an autoimmune disease of the liver[1] marked by the slow progressive destruction of the small bile ducts (bile canaliculi) within the liver. When these ducts are damaged, bile builds up in the liver (cholestasis) and over time damages the tissue. This can lead to scarring, fibrosis and cirrhosis. It was previously thought to be a rare disease, but more recent studies have shown that it may affect up to 1 in 3-4,000 people; the sex ratio is at least 9:1 (female to male).[2]
Contents
Signs and symptoms
The following signs may present in PBC:
- Fatigue
- Pruritus (itchy skin)
- Jaundice (yellowing of the eyes and skin), due to increased bilirubin in the blood.
- Xanthoma (local collections of cholesterol in the skin, especially around the eyes (Xanthelasma))
- Complications of cirrhosis and portal hypertension:
- Fluid retention in the abdomen (ascites)
- Hypersplenism
- Esophageal varices
- Hepatic encephalopathy, up to coma, in extreme cases.
- Association with an extrahepatic autoimmune disorder such as Rheumatoid arthritis or Sjögren's syndrome (up to 80% incidence).
Diagnosis
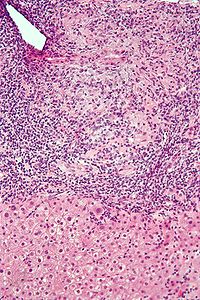 Intermediate magnification micrograph of PBC showing bile duct inflammation and periductal granulomas. Liver biopsy. H&E stain.
Intermediate magnification micrograph of PBC showing bile duct inflammation and periductal granulomas. Liver biopsy. H&E stain.
To diagnose PBC, distinctions should be established from other conditions with similar symptoms, such as autoimmune hepatitis or primary sclerosing cholangitis (PSC).
Diagnostic blood tests include:
- Deranged liver function tests (elevated gamma-glutamyl transferase and alkaline phosphatase)
- Presence of certain antibodies: antimitochondrial antibody(AMA), antinuclear antibody(ANA)
Abdominal ultrasound or a CT scan is usually performed to rule out blockage to the bile ducts. Previously most suspected sufferers underwent a liver biopsy, and - if uncertainty remained - endoscopic retrograde cholangiopancreatography (ERCP, an endoscopic investigation of the bile duct). Now most patients are diagnosed without invasive investigation since the combination of anti-mitochondrial antibodies (see below) and typical (cholestatic) liver function tests are considered diagnostic. However, a liver biopsy is necessary to determine the stage of disease.
Anti-nuclear antibodies appear to be prognostic agents in PBC. Anti-glycoprotein-210 antibodies, and to a lesser degree anti-p62 antibodies correlate with progression toward end stage liver failure. Anti-centromere antibodies correlate with developing portal hypertension.[3] Anti-np62[4] and anti-sp100 are also found in association with PBC.
Biopsy
Primary biliary cirrhosis is characterized by interlobular bile duct destruction. Histopathologic findings of primary biliary cirrhosis include:[5]
- Inflammation of the bile ducts, characterized by intraepithelial lymphocytes, and
- Periductal epithelioid granulomata.
Summary of stages
- Stage 1 - Portal Stage: Normal sized triads; portal inflammation, subtle bile duct damage. Granulomas are often detected in this stage.
- Stage 2 - Periportal Stage: Enlarged triads; periportal fibrosis and/or inflammation. Typically characterized by the finding of a proliferation of small bile ducts.
- Stage 3 - Septal Stage: Active and/or passive fibrous septa.
- Stage 4 - Biliary Cirrhosis: Nodules present; garland
Etiology
The cause of the disease is unknown at this time, but research indicates that there is an immunological basis for the disease, making it an autoimmune disorder. Most of the patients (>90%) seem to have anti-mitochondrial antibodies (AMAs) against pyruvate dehydrogenase complex (PDC-E2), an enzyme complex that is found in the mitochondria. In addition, a more specific test to confirm this disease from a bone disorder such as Paget's disease which also has increases in Alkaline phosphatase is the Gamma-glutamyl transpeptidase test (GGT). An increase in GGT could indicate presence of Primary Biliary Cirrhosis. 57% of patients with acute liver failure have anti-transglutaminase antibodies[6] suggesting a role of gluten sensitivity in primary biliary cirrhosis, and primary biliary cirrhosis is considerably more common in gluten sensitive enteropathy than the normal population.[7][8] In some cases of disease protein expression may cause an immune tolerance failure, as might be the case with gp210 and p62, nuclear pore proteins. Gp210 has increased expression in the bile duct of anti-gp210 positive patients.[9] Both proteins appear to be prognostic of liver failure relative to anti-mitochondrial antibodies.
A genetic predisposition to disease has been thought important for some time, as evident by cases of PBC in family members, concordance in identical twins, and clustering of autoimmune diseases. In 2009 a Canadian led group of investigators reported in the New England Journal of Medicine results from the first genome scan of PBC patients.[10][11] This research revealed parts of the IL12 signaling cascade, particularly IL12A and IL12RB2 polymorphisms, to be important in the etiology of the disease in addition to the HLA region, suggesting future therapeutic targets.
Therapy
There is no known cure, but medication may slow the progression so that a normal lifespan and quality of life may be attainable for many patients. However, specific treatment for fatigue, which may be debilitating in some patients, is unavailable.
- Ursodeoxycholic acid (Ursodiol) is the most frequently used treatment. This helps reduce the cholestasis and improves blood test results (liver function tests). It has a minimal effect on symptoms and whether it improves prognosis is controversial.
- To relieve itching caused by bile acids in circulation, which would normally be removed by the liver, cholestyramine (a bile acid sequestrant) may be prescribed to absorb bile acids in the gut and be eliminated, rather than re-enter the blood stream.
- Patients with PBC have poor lipid-dependent absorption of Vitamins A, D, E, K.[12] Multivitamins (esp. Vitamin D) and calcium are recommended.[citation needed]
As in all liver diseases, alcoholic beverages are contraindicated.
In advanced cases, a liver transplant, if successful, results in a favourable prognosis.
Obeticholic acid is in phase III clinical trials for PBC.[13]
Epidemiology
The female:male ratio is at least 9:1. In some areas of the US and UK the prevalence is estimated to be as high as 1 in 4000. This is much more common than in South America or Africa, which may be due to better recognition in the US and UK. First-degree relatives may have as much as a 500 times increase in prevalence, but there is debate if this risk is greater in the same generation relatives or the one that follows.[2]
Prognosis
The serum bilirubin level is an indicator of the prognosis of primary biliary cirrhosis, with levels of 2–6 mg/dL having a mean survival time of 4.1 years, 6–10 mg/dL having 2.1 years and those above 10 mg/dL having a mean survival time of 1.4 years.[14]
After liver transplant, the recurrence rate may be as high as 18% at 5 years, and up to 30% at 10 years. There is no consensus on risk factors for recurrence of the disease.[15]
Patients with primary biliary cirrhosis have an increased risk of hepatocellular carcinoma.
Additional images
-
Low magnification micrograph of PBC. H&E stain.
References
- ^ Henryk Dancygier (1 January 2010). Clinical Hepatology Principles and Practice of. Springer. pp. 895–. ISBN 9783642045097. http://books.google.com/?id=lrPX8C4p90QC&pg=PA895. Retrieved 29 June 2010.
- ^ a b Clavien, Pierre-Alain; Killenberg, Paul G. (2006). Medical Care of the Liver Transplant Patient: Total Pre-, Intra- and Post-Operative Management. Wiley-Blackwell. pp. 155. ISBN 1-4051-3032-6.
- ^ Nakamura M, Kondo H, Mori T, et al. (2007). "Anti-gp210 and anti-centromere antibodies are different risk factors for the progression of primary biliary cirrhosis". Hepatology 45 (1): 118–127. doi:10.1002/hep.21472. PMID 17187436.
- ^ Nesher G, Margalit R, Ashkenazi YJ (2001). "Anti-nuclear envelope antibodies: Clinical associations". Semin. Arthritis Rheum. 30 (5): 313–320. doi:10.1053/sarh.2001.20266. PMID 11303304.
- ^ Nakanuma Y, Tsuneyama K, Sasaki M, Harada K. Destruction of bile ducts in primary biliary cirrhosis. Baillieres Best Pract Res Clin Gastroenterol. 2000 Aug;14(4):549-70. Review. PMID 10976014.
- ^ Leung PS, Rossaro L, Davis PA, et al. (2007). "Antimitochondrial antibodies in acute liver failure: Implications for primary biliary cirrhosis". Hepatology 46 (5): 1436–42. doi:10.1002/hep.21828. PMID 17657817.
- ^ Logan RF, Ferguson A, Finlayson ND, Weir DG (1978). "Primary biliary cirrhosis and coeliac disease: an association?". Lancet 1 (8058): 230–3. doi:10.1016/S0140-6736(78)90480-4. PMID 74661.
- ^ Volta U, Rodrigo L, Granito A, et al. (2002). "Celiac disease in autoimmune cholestatic liver disorders". Am. J. Gastroenterol. 97 (10): 2609–13. doi:10.1111/j.1572-0241.2002.06031.x. PMID 12385447.
- ^ Nakamura M, Takii Y, Ito M, et al. (2006). "Increased expression of nuclear envelope gp210 antigen in small bile ducts in primary biliary cirrhosis". J. Autoimmun. 26 (2): 138–45. doi:10.1016/j.jaut.2005.10.007. PMID 16337775.
- ^ http://content.nejm.org/cgi/content/full/NEJMoa0810440
- ^ http://www.torontoliver.ca
- ^ Bruce R. Bacon; John G. O'Grady (2006). Comprehensive clinical hepatology. Elsevier Health Sciences. pp. 283–. ISBN 9780323036757. http://books.google.com/?id=ec0G9HGiR8MC&pg=PA283. Retrieved 29 June 2010.
- ^ http://www.genengnews.com/gen-news-highlights/dainippon-sumitomo-pays-intercept-15m-for-phase-iii-liver-disease-drug/81244901/
- ^ eMedicine > Primary Biliary Cirrhosis: Follow-up Author: Nikolaos T Pyrsopoulos. Coauthor: K Rajender Reddy. Updated: Dec 23, 2009
- ^ Killenberg & Clavien (2006), p. 429.
External links
- Primary Biliary Cirrhosis page from the National Digestive Diseases Information Clearinghouse
- Primary Biliary Cirrhosis page from the American Liver Foundation
- PBCers.org - patients' organisation
- PBC-Society.ca - Canadian PBC patient and research support
- PBC Foundation UK
Categories:- Diseases of liver
- Hepatology
- Autoimmune diseases
Wikimedia Foundation. 2010.

