- Hypermobility
-
Hypermobility Classification and external resources [[File:  |frameless|upright=1.06|alt=]]
|frameless|upright=1.06|alt=]]
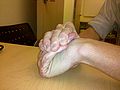
Hypermobile fingers and thumbICD-10 M35.7 ICD-9 728.5 OMIM 147900 DiseasesDB 31101 MeSH D007593 Hypermobility (also called "double jointedness" or hypermobility syndrome, benign joint hypermobility syndrome, or hyperlaxity) describes joints that stretch farther than is normal. For example, some hypermobile people can bend their thumbs backwards to their wrists, bend their knee joints backwards, put their leg behind the head or other contortionist performances. It can affect a single joint or multiple joints throughout the body.
Contents
Causes
Hypermobility generally results from one or more of the following:
- Misaligned joints
- Abnormally shaped ends of one or more bones at a joint
- A Type 1 collagen or other connective tissue defect (found in Ehlers-Danlos syndrome, Marfan syndrome) resulting in weakened ligaments/ligamentous laxity, muscles and tendons. This same defect also results in weakened bones, which may result in osteoporosis and fractures
- Abnormal joint proprioception (an impaired ability to determine where in space parts of the body are, and how stretched a joint is)
These abnormalities cause abnormal distribution of wear and tear on joints, meaning that the joints wear out and can lead to osteoarthritis.
The condition tends to run in families, suggesting that there may be a genetic basis for at least some forms of hypermobility. The term double jointed is often used to describe hypermobility; however, the name is a misnomer and should not to be taken literally, as an individual with hypermobility in a joint does not actually have two separate joints where others would have just one.
-
Dip.jpg
Hypermobile knee
The picture of Hypermobile knee can be viewed by clicking on this link : https://fbcdn-sphotos-a.akamaihd.net/hphotos-ak-ash4/223251_2073393431673_1150026333_32606870_6850469_n.jpg
Some people have hypermobility with no other symptoms or medical conditions. However, people with hypermobility syndrome may experience many difficulties. For example, their joints may be easily injured, be more prone to complete dislocation due to the weakly stabilized joint and they may develop problems from muscle fatigue (as muscles must work harder to compensate for the excessive weakness in the ligaments that support the joints). Hypermobility syndrome can also lead to chronic pain.
Hypermobility may also be symptomatic of a serious medical condition, such as Ehlers-Danlos syndrome, Marfan syndrome, rheumatoid arthritis, osteogenesis imperfecta, lupus, polio, Down syndrome, morquio syndrome, cleidocranial dysostosis or myotonia congenita.
In addition, hypermobility has been associated with chronic fatigue syndrome and fibromyalgia. During pregnancy certain hormones alter the physiology of ligaments making them able to stretch to accommodate the birthing process. For some women with hypermobility pregnancy-related pelvic girdle pain can be debilitating due to these two converging factors, and prohibits her from standing up or walking. Use of a bedpan and wheelchair may be necessary, or even permanent in some cases due to hip stretching.
Symptoms of hypermobility include a dull but intense pain around the knee and ankle joints and the soles of the feet. The condition affecting these parts can be alleviated by using insoles in the footwear that have been specially made for the individual after assessment by an orthopaedic surgeon and orthotist.
Anxiety and joint hypermobility
In 1998, a study was done concerning the link between panic disorder with joint hypermobility. The prevalence of panic disorder among patients with joint hypermobility syndrome was 67.7% compared to the control psychiatric group (10.1%). Women and subjects who were younger were found to be over 20 times more likely to have the hypermobile joints than their counterparts in the control group. In the study, there was also a higher prevalence for mitral valve prolapse (8%). The study does not determine whether hypermobility is associated in any way with psychiatric dysfunction or dysautonomia; many factors could explain the relation, and hypermobility's unwelcome gift of chronic pain may very well cause many people anxiety or depression. [1]
Hypermobility syndrome
Hypermobility syndrome is generally considered to comprise hypermobility together with other symptoms, such as myalgia and arthralgia. It is relatively common among children and affects more females than males.
Causes
Current thinking suggests that there are four factors: These four factors affect different people to varying degrees.
- The shape of the ends of the bones: Some joints normally have a large range of movement, like the shoulder and hip. Both these joints are ball in sockets. If a shallow rather than a deep socket is inherited, a relatively large range of movement will be possible at the affected joints. If the hip socket is particularly shallow, then the hip may dislocate easily.
- Weak or stretched ligaments caused by protein or hormone problems: ligaments are made up of several types of protein fibre. These proteins include elastin, which gives elasticity, which may be altered in some people. Also, the female sex hormones alter the collagen proteins. Women are generally more supple just before a period, and even more so in the latter stages of pregnancy, because of the effect of a hormone called relaxin. This hormone allows the pelvis to expand so the head of the baby can pass through. Different races have differences in their joint mobility, which may reflect differences in the structure of the collagen proteins. People from the Indian sub-continent, for example, often have much more supple hands than Europeans. [2]
- The tone of the muscles: The tone (or stiffness) of the muscles is controlled by your nervous system, and influences the range of movement in the joints. Some people use special techniques to change their muscle tone and increase their flexibility. Yoga, for example, can help to relax the muscles and make the joints more supple. Gymnasts and athletes can sometimes acquire hypermobility in at least some of their joints through the exercises they do in training.
- The sense of joint movement (proprioception): if it is difficult to detect the exact position of the joints with closed eyes, then it is possible to develop hypermobile joints because of over-stretching.[3]
Symptoms
People with hypermobility syndrome may develop other conditions caused by their unstable joints. These conditions include:
- Joint instability causing frequent sprains, tendinitis, or bursitis when doing activities that would not affect the normal individual
- Early-onset osteoarthritis
- Subluxations or dislocations, especially in the shoulder
- Knee pain
- Back pain, prolapsed discs or spondylolisthesis
- Joints that make clicking noises
- Susceptibility to whiplash
- Temporomandibular Joint Syndrome also known as TMJ
- Increased nerve compression disorders (e.g. carpal tunnel syndrome)
- The ability of Finger Locking
- Do not respond well to normal doses of anaesthetic or pain medication
- "Growing pains" as described in children in late afternoon or night
Diagnosis
Joint hypermobility syndrome needs to be distinguished from other disorders that share many common features, such as Marfan syndrome, Ehlers-Danlos Syndrome, and osteogenesis imperfecta. In the last couple of years collaborations of experts in connective tissue disorders formally agreed that there was little distinction between Hypermobility Syndrome and Ehlers Danlos Syndrome and that they are in fact the same disorder. Information on this can be found in an article titled "The lack of clinical distinction between the hypermobility type of Ehlers–Danlos syndrome and the joint hypermobility syndrome (a.k.a. hypermobility syndrome)"[4]
Generalized hypermobility is a common feature in all these hereditary connective tissue disorders and many features overlap, but often distinguishing features are present that enable differentiating these disorders.[5]
Brighton criteria
As of July 2000, hypermobility is diagnosed using the Brighton criteria[6]. The Brighton criteria will not replace the Beighton score but instead will use the previous criteria in conjunction with other symptoms. HMS will be diagnosed in the presence of either two major criteria, one major and two minor criteria, or four minor criteria. The criteria are as follows:
Major criteria
- A Beighton score of 4/9 or more (either current or historic)
- Arthralgia for more than three months in four or more joints
Minor criteria
- A Beighton score of 1, 2 or 3/9 (0, 1, 2 or 3 if aged 50+)
- Arthralgia (> 3 months) in one to three joints or back pain (> 3 months), spondylosis, spondylolysis/spondylolisthesis.
- Dislocation/subluxation in more than one joint, or in one joint on more than one occasion.
- Soft tissue rheumatism. > 3 lesions (e.g. epicondylitis, tenosynovitis, bursitis).
- Marfanoid habitus (tall, slim, span/height ratio >1.03, upper: lower segment ratio less than 0.89, arachnodactyly (positive Steinberg thumb / Walker wrist signs).
- Abnormal skin: striae, hyperextensibility, thin skin, papyraceous scarring.
- Eye signs: drooping eyelids or myopia or antimongoloid slant.
- Varicose veins or hernia or uterine/rectal prolapse.
Beighton score
The Beighton score is an edited version of the Carter & Wilkinson scoring system which has been used for many years as an indicator of widespread hyper-mobility. However medical professionals varied in their interpretations of the results; some accepting as low as 1/9 and some 4/9 as a diagnosis of HMS. Therefore it was incorporated, with clearer guidelines, into the Brighton Criteria. The Beighton score is measured by adding 1 point for each of the following:
- Placing flat hands on the floor with straight legs
- Left knee bending backward
- Right knee bending backward
- Left elbow bending backward
- Right elbow bending backward
- Left thumb touching the forearm
- Right thumb touching the forearm
- Left little finger bending backward past 90 degrees
- Right little finger bending backward past 90 degrees
Treatments
Physical therapy
It is important that the individual with hypermobility remain extremely fit - even more so than the average individual - to prevent recurrent injuries. Regular exercise and physical therapy or hydrotherapy can reduce symptoms of hypermobility, because strong muscles help to stabilise joints. These treatments can also help by stretching tight, overused muscles and ensuring the person uses joints within the ideal ranges of motion, avoiding hyperextension or hyperflexion. Low-impact exercise such as Pilates or T'ai chi is usually recommended for hypermobile people as it is less likely to cause injury than high-impact exercise or contact sports.
Moist hot packs can relieve the pain of aching joints and muscles. For some patients, ice packs also help to relieve pain.
Medication
Medications frequently used to reduce pain and inflammation caused by hypermobility include analgesics, anti-inflammatory drugs (though these have been linked with an increase in pain and joint instability for some sufferers), and tricyclic antidepressants. Some people with hypermobility may benefit from other medications such as steroid injections or gabapentin, a drug originally used for treating epilepsy. Europe is far ahead of the United States in terms of HMS recognition and its knowledge of how to treat it{{www.hypermobility.org}}. Tramadol, a non-narcotic yet opioid pain reliever that is nearly as effective as narcotics, has been used in England to treat HMS joint pain, and it is available either by prescription from a doctor in the United States or from Mexico. Benzodiazapines are also used in HMS sufferers who experience painful muscles spasms around loose joints.
Lifestyle modification
For some people with hypermobility, lifestyle changes decrease the severity of symptoms. For example:
- If writing is painful, people may be able to reduce the pain by typing.
- If typing is painful, they may try voice control software for their computer or a more ergonomic keyboard.
- If standing is painful, keep a bend in the knees or use a wheelchair.
- Avoid activities that can bring on symptoms. These include standing, stretching the joints (such as in some forms of yoga), and lifting heavy objects or weights.
- A decrease in heavy exercise, such as lifting heavy weights or running with wrist weights, which can be jarring to many joints, can be replaced with a more gentle run on an elliptical machine. Swimming fans could try using a kickboard to exercise in a pool (careful not to hyperextend knees while kicking the water and keep a bend in your elbows if you swim; if you have weak shoulders then avoid "arms-only" "pull" exercises in the water and try to focus on kicking without hyperextension while keeping a relaxed pace with your arms.)
- Posture should be closely monitored. Weakened ligaments and muscles contribute to poor posture, which may result in numerous other medical conditions. Isometric exercises and attention to where joints are (avoid crossing legs for example if you have hip problems) are helpful to keep posture from leading to more pain.
- Remember to ask for help when needed, as to not risk excessive strain when extra assistance can be acquired.
Other treatments
- Bracing to support weak joints may be helpful when joints are injured or painful, but caution must be used not to weaken the joints further.
- Prolotherapy injections work for some, according to testimonies. Though not a typical route to take, it may be preferable to steroid injections for some. Prolotherapy supposedly works by strengthening weak ligaments by injecting saline. It takes the strain off the overworked muscles, which tweak due to over-compensation. Injured areas, coupled with HMS, take more injections sessions to improve.
References
Grahame R. The revised (Brighton 1998) criteria for the diagnosis of benign joint hypermobility syndrome (BJHS). J Rheumatol. 2000;27:1777 –1779
- ^ Martin-Santos R, Bulbena A, Porta M, Gago J, Molina L, Duró JC (November 1998). "Association Between Joint Hypermobility Syndrome and Panic Disorder". American Journal of Psychiatry 155 (11): 1578–1583. PMID 9812121. http://ajp.psychiatryonline.org/cgi/content/full/155/11/1578.
- ^ Keer, Rosemary; Rodney Grahame (2003). Hypermobility syndrome : recognition and management for physiotherapists. Edinburgh: Butterworth-Heinemann. pp. 71. ISBN 0750653906. http://books.google.com/books?id=Z3tLOlyeuI4C&printsec=frontcover. "Asian Indians were found by Wordsworth et al. (1987) to be significantly more mobile than English Caucasians."
- ^ "Joint hypermobility". Arthritis Research UK. http://www.arc.org.uk/arthinfo/patpubs/6019/6019.asp.
- ^ "Rare illnesses and disabilities". http://www.rid-alliance.org/index.php?option=com_content&view=article&id=10:the-lack-of-clinical-distinction-between-the-hypermobility-type-of-ehlersdanlos-syndrome-and-the-joint-hypermobility-syndrome-aka-hypermobility-syndrome&catid=13:hypermobility-syndromeehlers-danlos-syndrome-type&Itemid=7.
- ^ Zweers MC, Kucharekova M, Schalkwijk J (March 2005). "Tenascin-X: a candidate gene for benign joint hypermobility syndrome and hypermobility type Ehlers-Danlos syndrome?". Ann. Rheum. Dis. 64 (3): 504–5. doi:10.1136/ard.2004.026559. PMC 1755395. PMID 15708907. http://ard.bmj.com/cgi/content/extract/64/3/504.
- ^ Grahame R. The revised (Brighton 1998) criteria for the diagnosis of benign joint hypermobility syndrome (BJHS). J Rheumatol. 2000;27:1777 –1779
External links
- Gurley-Green S (May 2001). "Living with the hypermobility syndrome". Rheumatology (Oxford) 40 (5): 487–9. doi:10.1093/rheumatology/40.5.487. PMID 11371654. http://rheumatology.oxfordjournals.org/cgi/content/full/40/5/487/.
- "Joint hypermobility syndrome". Indian Journal of Rheumatology 5 (4): 150. http://medind.nic.in/jaa/t05/i4/jaat05i4p150g.pdf.
- The Disability Handbook on Arthritis
- Martín-Santos R, Bulbena A, Porta M, Gago J, Molina L, Duró JC (November 1998). "Association between joint hypermobility syndrome and panic disorder". Am J Psychiatry 155 (11): 1578–83. PMID 9812121.
- The Hypermobility Syndrome Association (HMSA) is a charity run by and for people diagnosed with the Hypermobility Syndrome (HMS)
Systemic CT disorders (M32–M36, 710) General Other hypersensitivity/autoimmune Other Soft tissue disorders / Rheumatism / Connective tissue arthropathy (M65–M79, 725–728) Capsular joint Synovitis/Tenosynovitis (Calcific tendinitis, Stenosing tenosynovitis, Trigger finger, DeQuervain's syndrome) · Transient synovitis · Ganglion cystvillonodular synovitis (Giant cell tumor of the tendon sheath)BursopathyBursitis (Olecranon, Prepatellar, Trochanteric, Subacromial) · Synovial cyst (Baker's cyst) · Calcific bursitisNoncapsular joint Ligamentous laxity · Hypermobilityupper limb (Adhesive capsulitis of shoulder, Impingement syndrome Rotator cuff tear, Golfer's elbow, Tennis elbow)lower limb (Iliotibial band syndrome, Patellar tendinitis, Achilles tendinitis, Calcaneal spur, Metatarsalgia) · Bone spurNonjoint M: JNT
anat(h/c, u, t, l)/phys
noco(arth/defr/back/soft)/cong, sysi/epon, injr
proc, drug(M01C, M4)
Categories:- Diseases involving the fasciae
- Syndromes
- Arthritis
- Skeletal disorders
- Rheumatology
- Contortion
Wikimedia Foundation. 2010.