- Carpal tunnel syndrome
-
Carpal tunnel syndrome Classification and external resources 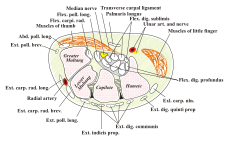
Transverse section at the wrist. The median nerve is colored yellow. The carpal tunnel consists of the bones and flexor retinaculum.ICD-10 G56.0 ICD-9 354.0 OMIM 115430 DiseasesDB 2156 MedlinePlus 000433 eMedicine orthoped/455 pmr/21 emerg/83 radio/135 MeSH D002349 This article is about the medical condition. For the anatomical structure, see Carpal tunnel. For the Fall Out Boy song, see The Carpal Tunnel of Love. For the Kid Koala album, see Carpal Tunnel Syndrome (album).Carpal Tunnel Syndrome (CTS) is an entrapment idiopathic median neuropathy, causing paresthesia, pain, and other symptoms in the distribution of the median nerve due to its compression at the wrist in the carpal tunnel. The pathophysiology is not completely understood but can be considered compression of the median nerve traveling through the carpal tunnel.[1] The National Center for Biotechnology Information and highly cited older literature[2] say the most common cause of CTS is typing.[3] More recent research by Lozano-Calderón has cited genetics as a larger factor than use,[4] and has encouraged caution in ascribing causality.[5]
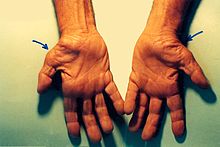
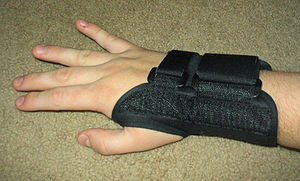
The main symptom of CTS is intermittent numbness of the thumb, index, long and radial half of the ring finger.[6] The numbness usually occurs at night, as humans tend to sleep with flexed wrists. It can be relieved by wearing a wrist splint that prevents flexion.[7] Long-standing CTS leads to permanent nerve damage with constant numbness, atrophy of some of the muscles of the thenar eminence, and weakness of palmar abduction.[8]
Pain in carpal tunnel syndrome is primarily numbness that is so intense that it wakes one from sleep. Pain in electrophysiologically verified CTS is associated with misinterpretation of nociception and depression.[9]
Palliative treatments for CTS include use of night splints and corticosteroid injection. The only scientifically established disease modifying treatment is surgery to cut the transverse carpal ligament.[10]
Contents
Signs and symptoms
Patients with CTS experience numbness, tingling, or burning sensations in the thumb and fingers, in particular the index, middle fingers, and radial half of the ring fingers, which are innervated by the median nerve. Less-specific symptoms may include pain in the hands or wrists and loss of grip strength[11] (both of which are more characteristic of painful conditions such as arthritis). Before the median nerve enters the carpal tunnel it passes first through the thoracic outlet and then the two heads of the pronator teres muscle of the forearm.[12] As a consequence, inflammation, edema, or hypertrophy in the thoracic outlet or the forearm can impinge the median nerve, mimicking the effects of carpal tunnel syndrome, and patients may also report pain in the arm and shoulder.[13]
Numbness and paresthesias in the median nerve distribution are the hallmark neuropathic symptoms (NS) of carpal tunnel entrapment syndrome. Weakness and atrophy of the thenar muscles may occur if the condition remains untreated.[14]
Causes
Most cases of CTS are of unknown causes, or idiopathic.[15] Carpal Tunnel Syndrome can be associated with any condition that causes pressure on the median nerve at the wrist. Some common conditions that can lead to CTS include obesity, oral contraceptives, hypothyroidism, arthritis, diabetes, and trauma.[16] Carpal tunnel is also a feature of a form of Charcot-Marie-Tooth syndrome type 1 called hereditary neuropathy with liability to pressure palsies.
Other causes of this condition include intrinsic factors that exert pressure within the tunnel, and extrinsic factors (pressure exerted from outside the tunnel), which include benign tumors such as lipomas, ganglion, and vascular malformation.[17]
The international debate regarding the relationship between CTS and repetitive motion in work is ongoing. The Occupational Safety and Health Administration (OSHA) has adopted rules and regulations regarding cumulative trauma disorders. Occupational risk factors of repetitive tasks, force, posture, and vibration have been cited. However, the American Society for Surgery of the Hand (ASSH) has issued a statement claiming that the current literature does not support a causal relationship between specific work activities and the development of diseases such as CTS.[18]
The relationship between work and CTS is controversial; in many locations, workers diagnosed with carpal tunnel syndrome are entitled to time off and compensation.[19] In the USA, Carpal tunnel syndrome results in an average of $30,000 in lifetime costs (medical bills and lost time from work).[20]
Some speculate that carpal tunnel syndrome is provoked by repetitive movement and manipulating activities and that the exposure can be cumulative. It has also been stated that symptoms are commonly exacerbated by forceful and repetitive use of the hand and wrists in industrial occupations,[21] but it is unclear as to whether this refers to pain (which may not be due to carpal tunnel syndrome) or the more typical numbness symptoms.[22]
A review of available scientific data by the National Institute for Occupational Safety and Health (NIOSH) indicated that job tasks that involve highly repetitive manual acts or specific wrist postures were associated with incidents of CTS, but causation was not established, and the distinction from work-related arm pains that are not carpal tunnel syndrome was not clear. It has been proposed that repetitive use of the arm can affect the biomechanics of the upper limb or cause damage to tissues. It has also been proposed that postural and spinal assessment along with ergonomic assessments should be included in the overall determination of the condition. While addressing these factors has been found to improve comfort in some studies,[23]
The speculation or rationale that CTS is work-related is based on debatable points such as: 1. CTS is found mostly in the working adult population. This may depend on how CTS is defined and diagnosed, but this seems untrue. For instance, in one recent representative series of a consecutive experience, most patients were older and not working.[24] Based on the claimed increased incidence in the workplace, arm use is implicated, but the weight of evidence suggests that this is an inherent, genetic, slowly but inevitably progressive idiopathic peripheral mononeuropathy.[25]
Associated with other diseases
A variety of patient factors can lead to CTS, including heredity, size of the carpal tunnel, associated local and systematic diseases, and certain habits.[1] Non-traumatic causes generally happen over a period of time, and are not triggered by one certain event. Many of these factors are manifestations of physiologic aging.[26]
Examples include:
- Rheumatoid arthritis and other diseases that cause inflammation of the flexor tendons.
- With pregnancy and hypothyroidism, fluid is retained in tissues, which swells the tenosynovium.
- During pregnancy women experience CTS due to hormonal changes (high progesterone levels) and water retention, which is common during pregnancy.
- Previous injuries including fractures of the wrist.
- Medical disorders that lead to fluid retention or are associated with inflammation such as: inflammatory arthritis, Colles' fracture, amyloidosis, hypothyroidism, diabetes mellitus, acromegaly, and use of corticosteroids and estrogens.
- Carpal tunnel syndrome is also associated with repetitive activities of the hand and wrist, in particular with a combination of forceful and repetitive activities[16]
- Acromegaly, causes excessive growth hormones. This causes the soft tissues and bones around the carpel tunnel to grow causes compression of the median nerve.[27]
- Tumors (usually benign), such as a ganglion or a lipoma, can protrude into the carpal tunnel, reducing the amount of space. This is exceedingly rare (less than 1%).
- Obesity also increases the risk of CTS: individuals classified as obese (BMI > 29) are 2.5 times more likely than slender individuals (BMI < 20) to be diagnosed with CTS.[28]
- Double-crush syndrome is a debated hypothesis that compression or irritation of nerve branches contributing to the median nerve in the neck, or anywhere above the wrist, increases sensitivity of the nerve to compression in the wrist. There is little evidence, however, that this syndrome really exists.[29]
- Heterozygous mutations in the gene SH3TC2, associated with Charcot-Marie-Tooth, confer susceptibility to neuropathy, including the carpal tunnel syndrome.[30]
- Parvovirus b19 has been associated with carpel tunnel syndrome [31]
Diagnosis
The reference standard for the diagnosis of carpal tunnel syndrome is electrophysiological testing. Patients with intermittent numbness in the distribution of the median nerve along with positive Phalen's, Durkan's, and eletrophysiological tests have, at worst, a very mild case of carpal tunnel syndrome. A predominance of pain rather than numbness is unlikely to be caused by carpal tunnel syndrome no matter what the result of electrophysiological testing.
Clinical assessment by history taking and physical examination can support a diagnosis of CTS.
- Phalen's maneuver is performed by flexing the wrist gently as far as possible, then holding this position and awaiting symptoms.[32] A positive test is one that results in numbness in the median nerve distribution when holding the wrist in acute flexion position within 60 seconds. The quicker the numbness starts, the more advanced the condition. Phalen's sign is defined as pain and/or paresthesias in the median-innervated fingers with one minute of wrist flexion. Only this test has been shown to correlate with CTS severity when studied prospectively.[1]
- Tinel's sign, a classic — though less sensitive - test is a way to detect irritated nerves. Tinel's is performed by lightly tapping the skin over the flexor retinaculum to elicit a sensation of tingling or "pins and needles" in the nerve distribution. Tinel's sign (pain and/or paresthesias of the median-innervated fingers with percussion over the median nerve) is less sensitive, but slightly more specific than Phalen’s sign.[1]
- Durkan test, carpal compression test, or applying firm pressure to the palm over the nerve for up to 30 seconds to elicit symptoms has also been proposed.[33][34]
As a note, a patient with true carpal tunnel syndrome (entrapment of the median nerve within the carpal tunnel) will not have any sensory loss over the thenar eminence (bulge of muscles in the palm of hand and at the base of the thumb). This is because the palmer branch of the median nerve, which innervates that area of the palm, branches off of the median nerve and passes over the carpal tunnel.[35] This feature of the median nerve can help separate carpal tunnel syndrome from thoracic outlet syndrome, or pronator teres syndrome.
Other conditions may also be misdiagnosed as carpal tunnel syndrome. Thus, if history and physical examination suggest CTS, patients will sometimes be tested electrodiagnostically with nerve conduction studies and electromyography. The goal of electrodiagnostic testing is to compare the speed of conduction in the median nerve with conduction in other nerves supplying the hand. When the median nerve is compressed, as in CTS, it will conduct more slowly than normal and more slowly than other nerves. There are many electrodiagnostic tests used to make a diagnosis of CTS, but the most sensitive, specific, and reliable test is the Combined Sensory Index (also known as Robinson index).[36]
Nerve conduction studies (NCS) are a sensitive measure of detecting compression of the median nerve. Electrodiagnosis rests upon demonstrating impaired median nerve conduction across the carpal tunnel in context of normal conduction elsewhere. Compression results in damage to the myelin sheath and manifests as delayed latencies and slowed conduction velocities [1]
The role of MRI or ultrasound imaging in the diagnosis of carpal tunnel syndrome is unclear.[37][38][39]
Differential diagnosis
There are some who believe that carpal tunnel syndrome is simply a universal label applied to anyone suffering from pain, numbness, swelling, and/or burning in the radial side of the hands and/or wrists. When pain is the primary symptom, carpal tunnel syndrome is unlikely to be the source of the symptoms.[22] As a whole, the medical community is not currently embracing or accepting trigger point theories due to lack of scientific evidence supporting their effectiveness.[40]
Pathophysiology
The carpal tunnel is an anatomical compartment located at the base of the wrist. Nine flexor tendons and the median nerve pass through the carpal tunnel that is surrounded on three sides by the carpal bones that form an arch. The nerve and the tendons provide function, feeling, and movement to some of the fingers. The finger and wrist flexor muscles including their tendons originate in the forearm at the medial epicondyle of the elbow joint and attach to the Metaphalangeal (MP), Proximal Interphalangeal (PIP), and Distal Interphalangeal bones of the fingers and thumb (BSI). The carpal tunnel is approximately as wide as the thumb and its boundary lies at the distal wrist skin crease and extends distally into the palm for approximately 2 cm.[citation needed]
The median nerve can be compressed by a decrease in the size of the canal, an increase in the size of the contents (such as the swelling of lubrication tissue around the flexor tendons), or both.[41] Simply flexing the wrist to 90 degrees will decrease the size of the canal.
Compression of the median nerve as it runs deep to the transverse carpal ligament (TCL) causes atrophy of the thenar eminence, weakness of the flexor pollicis brevis, opponens pollicis, abductor pollicis brevis, as well as sensory loss in the distribution of the median nerve distal to the transverse carpal ligament. There is a superficial sensory branch of the median nerve, which branches proximal to the TCL and travels superficial to it. Therefore, this branch is spared, and it innervates the palm toward the thumb.[42]
Prevention
A 2007 study, conducted by Lozano-Calderon et al. in the Department of Orthopaedic Surgery at Massachusetts General Hospital, states that carpal tunnel syndrome is determined primarily by genetics and structure.[43] It is presumed, therefore, that carpal tunnel syndrome is not preventable.[original research?]
However, others[who?] think it can be prevented by developing healthy habits like avoiding repetitive stress, practicing healthy work habits like using ergonomic equipment (wrist rest, mouse pad), taking proper breaks, using keyboard alternatives (digital pen, voice recognition, and dictation), and employing early passive treatment like taking turmeric (anti-inflammatory), omega-3 fatty acids, and B vitamins. Scientists have long abandoned the potential role of B-vitamins in carpal tunnel syndrome.[44][45]
Those favoring activity as a cause of carpal tunnel syndrome speculate that activity-limitation might limit the risk of developing carpal tunnel syndrome, but there is little or no data to support these concepts.[43] and they stigmatize arm use in ways that risks increasing illness.[46][47]
Treatment
There have been numerous scientific papers evaluating treatment efficacy in CTS. It is important to distinguish treatments that are supported in the scientific literature from those that are advocated by any particular device manufacturer or any other party with a vested financial interest. Generally accepted treatments, as described below, may include splinting or bracing, steroid injection, activity modification, physiotherapy, regular massage therapy treatments, chiropractic, medications, and surgical release of the transverse carpal ligament.
According to the 2007 guidelines by the American Academy of Orthopaedic Surgeons,[48] early surgery with carpal tunnel release is indicated where there is clinical evidence of median nerve denervation or the patient elects to proceed directly to surgical treatment. Otherwise, the main recommended treatments are local corticosteroid injection, splinting (immobilizing braces), oral corticosteroids and ultrasound treatment. The treatment should be switched when the current treatment fails to resolve the symptoms within 2 to 7 weeks. However, these recommendations have sufficient evidence for carpal tunnel syndrome when found in association with the following conditions: diabetes mellitus, coexistent cervical radiculopathy, hypothyroidism, polyneuropathy, pregnancy, rheumatoid arthritis, and carpal tunnel syndrome in the workplace.[48]
Immobilizing braces
The importance of wrist braces and splints in the carpal tunnel syndrome therapy is known, but many people are unwilling to use braces. In 1993, The American Academy of Neurology recommend a non-invasive treatment for the CTS at the beginning (except for sensitive or motor deficit or grave report at EMG/ENG): a therapy using splints was indicated for light and moderate pathology.[49] Current recommendations generally don't suggest immobilizing braces, but instead activity modification and non-steroidal anti-inflammatory drugs as initial therapy, followed by more aggressive options or specialist referral if symptoms do not improve.[50][51][52]
Many health professionals suggest that, for best results, one should wear braces at night and, if possible, during the activity primarily causing stress on the wrists.[53][54]
Localized corticosteroid injections
Corticosteroid injections can be quite effective for temporary relief from symptoms of CTS for a short time-frame while a patient develops a longterm strategy that fits with his/her lifestyle.[55] In certain patients, an injection may also be of diagnostic value. This treatment is not appropriate for extended periods, however. In general, medical professionals prescribe local steroid injections only until other treatment options can be identified. For most patients, surgery is the only option that will provide permanent relief.[56]
Other medication
A more aggressive pharmaceutical option is an injection of cortisone, to reduce swelling and nerve pressure within the carpal tunnel. Methylcobalamin (vitamin B12) has been helpful in some cases of CTS. [57]
Carpal tunnel release surgery
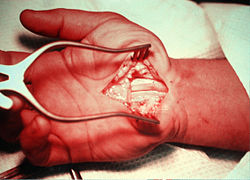
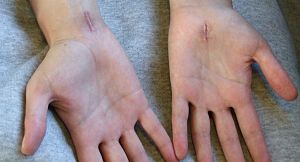 Scars from carpal tunnel release surgery. Two different techniques were used. The left scar is 6 weeks old, the right scar is 2 weeks old. Also note the muscular atrophy of the thenar eminence in the left hand, a common sign of advanced CTS
Scars from carpal tunnel release surgery. Two different techniques were used. The left scar is 6 weeks old, the right scar is 2 weeks old. Also note the muscular atrophy of the thenar eminence in the left hand, a common sign of advanced CTS
Release of the transverse carpal ligament is known as "carpal tunnel release" surgery. It is recommended when there is static (constant, not just intermittent) numbness, muscle weakness, or atrophy, and when night-splinting no longer controls intermittent symptoms.[58] In general, milder cases can be controlled for months to years, but severe cases are unrelenting symptomatically and are likely to result in surgical treatment.[59]
Procedure
In carpal tunnel release surgery, the goal is to divide the transverse carpal ligament in two. This is a wide ligament that runs across the hand, from the scaphoid bone to the hamate bone and pisiform. It forms the roof of the carpal tunnel, and when the surgeon cuts across it (i.e., in a line with the ring finger) it no longer presses down on the nerve inside, relieving the pressure.[60]
There are several carpal tunnel release surgery variations: Each surgeon has differences of preference based on his or her personal beliefs and experience. All techniques have several things in common, involving brief outpatient procedures, palm or wrist incision(s), and cutting of the transverse carpal ligament.[citation needed]
The two major types of surgery are open carpal tunnel release and endoscopic carpal tunnel release. Most surgeons historically have performed the open procedure, widely considered to be the gold standard. However, since the 1990s, a growing number of surgeons now offer endoscopic carpal tunnel release.[citation needed]
Open surgery involves an incision on the palm about an inch or two in length. Through this incision, the skin and subcutaneous tissue is divided, followed by the palmar fascia, and ultimately the transverse carpal ligament.[citation needed]
Endoscopic techniques involve one or two smaller incisions (less than half inch each) through which instrumentation is introduced including a synovial elevator, probes, knives, and an endoscope used to visualize the underside of the transverse carpal ligament.[61] The endoscopic methods do not divide the subcutaneous tissues or the palmar fascia to the same degree as the open method does.[citation needed]
Many studies have been done to determine whether perceived benefits of a limited endoscopic or arthroscopic release are significant. Brown et al. conducted a prospective, randomized, multi-center study and found no significant differences between the two groups with regard to secondary quantitative outcome measurements.[62] However, the open technique resulted in more tenderness of the scar than the endoscopic method. A prospective randomized study done in 2002 by Trumble revealed that good clinical outcomes and patient satisfaction are achieved more quickly with the endoscopic method. Single-portal endoscopic surgery is a safe and effective method of treating carpal tunnel syndrome. There was no significant difference in the rate of complications or the cost of surgery between the two groups. However, the open technique caused greater scar tenderness during the first three months after surgery, and a longer time before the patients could return to work.[63]
Many surgeons have embraced limited incision methods. It is considered to be the procedure of choice for many of these surgeons with respect to idiopathic carpal tunnel syndrome. Supporting this are the results of some of the previously mentioned series that cite no difference in the rate of complications for either method of surgery. Thus, there has been broad support for either surgical procedure using a variety of devices or incisions. The primary goal of any carpal tunnel release surgery is to divide the transverse carpal ligament and the distal aspect of the volar ante brachial fascia, thereby decompressing the median nerve.[64] Despite these views, some surgeons have suggested that in their own hands endoscopic carpal tunnel release has been associated with a higher incidence of median nerve injury, and for this reason it has been abandoned at several centers in the United States. At the 2007 meeting of the American Society for Surgery of the Hand, a former advocate of endoscopic carpal tunnel release, Thomas J. Fischer, MD, retracted his advocacy of the technique, based on his assessment that the benefit of the procedure (slightly faster recovery) did not outweigh the risk of injury to the median nerve.
Balloon Carpal Tunnelplasty is a technique that uses a minimally invasive balloon catheter director to access the carpal tunnel. The director protects the median nerve and contents of the carpal tunnel. As with a traditional tissue elevator/expander with Balloon Carpal Tunnelplasty, the carpal ligament is elevated increasing the space in the carpal tunnel. The Balloon Carpal Tunnelplasty technique is performed through a one-centimeter incision at the distal wrist crease. It is monitored and expansion is confirmed by direct or endoscopic visualization. The purpose of Balloon Carpal Tunnelplasty is to avoid an incision in the palm of the hand, avoid cutting the transverse carpal ligament, and maintain the biomechanics of the hand. [65]
Efficacy
Surgery to correct carpal tunnel syndrome has a high success rate. Up to 90% of patients were able to return to their same jobs after surgery.[66][67][68] In general, endoscopic techniques are as effective as traditional open carpal surgeries,[69][70] though the faster recovery time typically noted in endoscopic procedures is felt by some to possibly be offset by higher complication rates.[71][72] Success is greatest in patients with the most typical symptoms. The most common cause of failure is incorrect diagnosis, and it should be noted that this surgery will only mitigate carpal tunnel syndrome, and will not relieve symptoms with alternative causes. Recurrence is rare, and apparent recurrence usually results from a misdiagnosis of another problem.[citation needed] Complications can occur, but serious ones are infrequent to rare.[citation needed]
Carpal tunnel surgery is usually performed by a hand surgeon, orthopaedic surgeon, or plastic surgeon. Some neurosurgeons and general surgeons also perform the procedure.[citation needed]
Ultrasound treatment
Some claim that Ultrasound to the wrist gives significant improvement of symptoms in people with CTS.[73] A treatment process may consist of 20 sessions of 15 minutes of ultrasound applied to the area over the carpal tunnel at a frequency of 1 MHz, and a power of 1.0 W/cm2.[73]
However, many studies have shown no effect.[74][75] Given these inconsistencies, the role of ultrasound in the treatment of CTS is debatable and it should be considered an experimental treatment.
Physiotherapy
One review of the evidence for possible symptom reduction found good evidence (level B recommendations) for splinting, ultrasound, nerve gliding exercises, carpal bone mobilization, magnetic therapy, and yoga for people with carpal tunnel syndrome.[76] However, a recent evidence based guideline produced by the American Academy of Orthopedic Surgeons assigned lower grades to most of these treatments.[77]
Again, some claim that pro-active ways to reduce stress on the wrists, which alleviates wrist pain and strain, involve adopting a more ergonomic work and life environment. For example, some have claimed that switching from a QWERTY computer keyboard layout to a more optimised ergonomic layout such as Dvorak was commonly cited as beneficial in early CTS studies, however some meta-analyses of these studies claim that the evidence that they present is limited.[78][79]
Occupational therapy
OTs are involved in the assessment and intervention process with clients with CTS. Within the area of intervention, OTs provide education; symptom management techniques such as splinting; and modification of specific tasks, equipment and environment .
Prognosis
Most people relieved of their carpal tunnel symptoms with conservative or surgical management find minimal residual or "nerve damage".[80] Long-term chronic carpal tunnel syndrome (typically seen in the elderly) can result in permanent "nerve damage", i.e. irreversible numbness, muscle wasting, and weakness.
While outcomes are generally good, certain factors can contribute to poorer results that have little to do with nerves, anatomy, or surgery type. One study showed that mental status parameters or alcohol use yields much poorer overall results of treatment.[81]
Recurrence of carpal tunnel syndrome after successful surgery is rare.[82] If a person has hand pain after surgery, it is most likely not caused by carpal tunnel syndrome. It may be the case that the illness of a person with hand pain after carpal tunnel release was diagnosed incorrectly, such that the carpal tunnel release has had no positive effect upon the patient's symptoms.[citation needed]
Epidemiology
Carpal tunnel syndrome can affect anyone. In the U.S., roughly 1 out of 20 people will suffer from the effects of carpal tunnel syndrome. Caucasians have the highest risk of CTS compared with other races such as non-white South Africans.[83] Women suffer more from CTS than men with a ratio of 3:1 between the ages of 45–60 years. Only 10% of reported cases of CTS are younger than 30 years.[83] Increasing age is a risk factor. CTS is also common in pregnancy.
History
The condition known as Carpal Tunnel Syndrome had major appearances throughout the years but it was most commonly heard of in the years following World War II.[84]Individuals who had suffered from this condition have been depicted in surgical literature for the mid-19th century.[84]In 1854, Sir James Paget was the first to report median nerve compression at the wrist in a distal radius fracture.[85] Following the early 20th century there were various cases of median nerve compression underneath the transverse carpal ligament.[85] Carpal Tunnel Syndrome was most commonly noted in medical literature in the early 20th century but the first use of the term was noted 1939. Physician Dr. George S. Phalen of the Cleveland Clinic identified the pathology after working with a group of patients in the 1950s and 1960s.
Notable cases
- HRH Prince Philip, husband of Queen Elizabeth II[86]
- Mike Dirnt, bassist with the band Green Day[87]
- Michael Einziger, guitarist with the band Incubus
References
- ^ a b c d e Scott, Kevin R.; Kothari, Milind J. (October 5, 2009). "Treatment of carpal tunnel syndrome". UpToDate. http://www.uptodate.com/patients/content/topic.do?topicKey=~wx2xecoDuYz0gp.
- ^ Silverstein, B; Fine, L; Armstrong, T (1987). "Occupational factors and carpal tunnel syndrome". American Journal of Industrial Medicine 11 (3): 343-358. doi:10.1002/ajim.4700110310.
- ^ http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0001469/
- ^ Lozano-Calderón, S; Anthony, S; Ring, D (2008). "The quality and strength of evidence for etiology: example of carpal tunnel syndrome". The Journal of hand surgery 33 (4): 525–38. doi:10.1016/j.jhsa.2008.01.004. PMID 18406957.
- ^ Scangas, G; Lozano-Calderón, S; Ring, D (2008). "Disparity between popular (Internet) and scientific illness concepts of carpal tunnel syndrome causation". The Journal of hand surgery 33 (7): 1076–80. doi:10.1016/j.jhsa.2008.03.001. PMID 18762100.
- ^ Walker, Jennie A. (2010). "Management of patients with carpal tunnel syndrome". Nursing Standard 24 (19): 44–8. PMID 20175360.
- ^ Shiel, William C.. "Carpal Tunnel Syndrome & Tarsal Tunnel Syndrome". MedicineNet. http://www.medicinenet.com/carpal_tunnel_syndrome/article.htm.
- ^ Uemura, T; Hidaka N, Nakamura H. (28). "Clinical outcome of carpal tunnel release with and without opposition transfer.". J Hand Surg Eur Vol. 35 (8): 632–6. doi:10.1177/1753193410369988. PMID 20427406. http://www.ncbi.nlm.nih.gov/pubmed/20427406. Retrieved 26 February 2011.
- ^ Nunez, F; Vranceanu, AM; Ring, D (2010). "Determinants of pain in patients with carpal tunnel syndrome". Clinical orthopaedics and related research 468 (12): 3328–32. doi:10.1007/s11999-010-1551-x. PMC 2974864. PMID 20811788. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=2974864.
- ^ Bickel, Kyle D (January 2010). "Carpal Tunnel Syndrome". Journal of Hand Surgery 35 (1): 147–152. doi:10.1016/j.jhsa.2009.11.003. PMID 20117319. http://www.jhandsurg.org/article/S0363-5023%2809%2900949-6/fulltext. Retrieved 26 February 2011.
- ^ Atroshi, I.; Gummesson, C; Johnsson, R; Ornstein, E; Ranstam, J; Ros�n, I (1999). "Prevalence of Carpal Tunnel Syndrome in a General Population". JAMA 282 (2): 153–158. doi:10.1001/jama.282.2.153. PMID 10411196.
- ^ Netter, Frank (2011). Atlas of Human Anatomy (5th ed.). Philadelphia, PA: Saunders Elsevier. pp. 412, 417, 435. ISBN 9780808924234.
- ^ "Carpal Tunnel Syndrome Information Page". National Institute of Neurological Disorders and Stroke. December 28, 2010. http://www.ninds.nih.gov/disorders/carpal_tunnel/carpal_tunnel.htm.
- ^ Lazaro, R (1997). "Neuropathic symptoms and musculoskeletal pain in carpal tunnel syndrome: Prognostic and therapeutic implications". Surgical Neurology 47 (2): 115–7; discussion 117–9. doi:10.1016/S0090-3019(95)00457-2.
- ^ Sternbach, G (1999). "The carpal tunnel syndrome". Journal of Emergency Medicine 17 (3): 519–23. doi:10.1016/S0736-4679(99)00030-X. PMID 10338251.
- ^ a b Katz, Jeffrey N.; Simmons, Barry P. (2002). "Carpal Tunnel Syndrome". New England Journal of Medicine 346 (23): 1807–12. doi:10.1056/NEJMcp013018. PMID 12050342.
- ^ Tiong, W. H. C.; Ismael, T.; Regan, P. J. (2005). "Two rare causes of carpal tunnel syndrome". Irish Journal of Medical Science 174 (3): 70–8. doi:10.1007/BF03170208. PMID 16285343.
- ^ "Carpal Tunnel Syndrome". Assh.org. http://www.assh.org/Public/HandConditions/Pages/CarpalTunnelSyndrome.aspx. Retrieved 2011-10-05.
- ^ . pp. 353–67, viii. doi:10.1016/j.coem.2005.11.014.
- ^ Office of Communications and Public Liaison (December 18, 2009). "National Institute of Neurological Disorders and Stroke". http://www.ninds.nih.gov/disorders/carpal_tunnel/detail_carpal_tunnel.htm.
- ^ Werner, Robert A. (2006). "Evaluation of Work-Related Carpal Tunnel Syndrome". Journal of Occupational Rehabilitation 16 (2): 201. doi:10.1007/s10926-006-9026-3. PMID 16705490.
- ^ a b Graham, B. (1 December 2008). "The Value Added by Electrodiagnostic Testing in the Diagnosis of Carpal Tunnel Syndrome". The Journal of Bone and Joint Surgery 90 (12): 2587–2593. doi:10.2106/JBJS.G.01362. PMID 19047703.
- ^ Cole, Donald C.; Hogg-Johnson, Sheilah; Manno, Michael; Ibrahim, Selahadin; Wells, Richard P.; Ferrier, Sue E.; Worksite Upper Extremity Research Group (2006). "Reducing musculoskeletal burden through ergonomic program implementation in a large newspaper". International Archives of Occupational and Environmental Health 80 (2): 98–108. doi:10.1007/s00420-006-0107-6. PMID 16736193.
- ^ LOZANOCALDERON, S; PAIVA, A, RING, D (1 March 2008). "Patient Satisfaction After Open Carpal Tunnel Release Correlates With Depression". The Journal of Hand Surgery 33 (3): 303–307. doi:10.1016/j.jhsa.2007.11.025. PMID 18343281.
- ^ LOZANOCALDERON, S; ANTHONY, S, RING, D (1 April 2008). "The Quality and Strength of Evidence for Etiology: Example of Carpal Tunnel Syndrome". The Journal of Hand Surgery 33 (4): 525–538. doi:10.1016/j.jhsa.2008.01.004. PMID 18406957.
- ^ Stevens JC, Beard CM, O'Fallon WM, Kurland LT (1992). "Conditions associated with carpal tunnel syndrome". Mayo Clin Proc 67 (6): 541–548. PMID 1434881.
- ^ "Carpel Tunnel Syndrome in Acromegaly". Treatmentandsymptoms.com. http://www.treatmentandsymptoms.com/endocrine/acromegaly/. Retrieved 2011-10-05.
- ^ Werner, Robert A.; Albers, James W.; Franzblau, Alfred; Armstrong, Thomas J. (1994). "The relationship between body mass index and the diagnosis of carpal tunnel syndrome". Muscle & Nerve 17 (6): 632–6. doi:10.1002/mus.880170610.
- ^ Wilbourn AJ, Gilliatt RW (1997). "Double-crush syndrome: a critical analysis". Neurology 49 (1): 21–27. PMID 9222165.
- ^ Lupski, James R.; Reid, Jeffrey G.; Gonzaga-Jauregui, Claudia; Rio Deiros, David; Chen, David C.Y.; Nazareth, Lynne; Bainbridge, Matthew; Dinh, Huyen et al. (2010). "Whole-Genome Sequencing in a Patient with Charcot–Marie–Tooth Neuropathy". New England Journal of Medicine 362 (13): 1181–91. doi:10.1056/NEJMoa0908094. PMID 20220177.
- ^ Musiani, Monica; gallinella, Georgio (1997). "Persistent parvovirus b18 infections resulting in carpel tunnel syndrome". Clinical Pathology 49 (1): 21–27. PMID 9222165.
- ^ Cush JJ, Lipsky PE (2004). "Approach to articular and musculoskeletal disorders". Harrison's Principles of Internal Medicine (16th ed.). McGraw-Hill Professional. p. 2035. ISBN 0-07-140235-7.
- ^ Gonzalezdelpino, J; Delgadomartinez, A; Gonzalezgonzalez, I; Lovic, A (1997). "Value of the carpal compression test in the diagnosis of carpal tunnel syndrome". The Journal of Hand Surgery: Journal of the British Society for Surgery of the Hand 22: 38–41. doi:10.1016/S0266-7681(97)80012-5.
- ^ Durkan, JA (1991). "A new diagnostic test for carpal tunnel syndrome". The Journal of bone and joint surgery. American volume 73 (4): 535–8. PMID 1796937.
- ^ Netter, Frank (2011). Atlas of Human Anatomy (5th ed.). Philadelphia, PA: Saunders Elsevier. p. 447. ISBN 9780808924234.
- ^ Robinson, L (2007). "Electrodiagnosis of Carpal Tunnel Syndrome". Physical Medicine and Rehabilitation Clinics of North America 18 (4): 733–46. doi:10.1016/j.pmr.2007.07.008.
- ^ Wilder-Smith, Einar P; Seet, Raymond C S; Lim, Erle C H (2006). "Diagnosing carpal tunnel syndrome—clinical criteria and ancillary tests". Nature Clinical Practice Neurology 2 (7): 366–74. doi:10.1038/ncpneuro0216. PMID 16932587.
- ^ Bland, Jeremy DP (2005). "Carpal tunnel syndrome". Current Opinion in Neurology 18 (5): 581–5. doi:10.1097/01.wco.0000173142.58068.5a. PMID 16155444.
- ^ Jarvik, J; Yuen, E; Kliot, M (2004). "Diagnosis of carpal tunnel syndrome: electrodiagnostic and MR imaging evaluation". Neuroimaging Clinics of North America 14: 93–102, viii. doi:10.1016/j.nic.2004.02.002.
- ^ Davies, Clair; Simons, David G.; Davies, Amber (2004). The Trigger Point Therapy Workbook: Your Self-Treatment Guide for Pain Relief, Second Edition. Oakland, Calif: New Harbinger Publications. ISBN 978-1-57224-375-0.[page needed]
- ^ RH Gelberman, PT Hergenroeder, AR Hargens, GN Lundborg and WH Akeson (03/01/1981). "The carpal tunnel syndrome. A study of carpal canal pressures". The Journal of Bone and Joint Surgery 63 (3): 380–383. PMID 7204435. http://www.ejbjs.org/cgi/content/abstract/63/3/380.
- ^ Norvell, Jeffrey G.; Steele, Mark (September 10, 2009). "Carpal Tunnel Syndrome". eMedicine. http://emedicine.medscape.com/article/822792-overview.
- ^ a b Lozano-Calderón, Santiago; Shawn Anthony, David Ring (April 2008). "The Quality and Strength of Evidence for Etiology: Example of Carpal Tunnel Syndrome". The Journal of Hand Surgery 33 (4): 525–538. doi:10.1016/j.jhsa.2008.01.004. PMID 18406957.
- ^ Spooner, GR; Desai, HB, Angel, JF, Reeder, BA, Donat, JR (1993 Oct). "Using pyridoxine to treat carpal tunnel syndrome. Randomized control trial". Canadian Family Physician 39: 2122–7. PMC 2379872. PMID 8219859. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=2379872.
- ^ Scangas, G; Lozano-Calderón, S, Ring, D (2008 Sep). "Disparity between popular (Internet) and scientific illness concepts of carpal tunnel syndrome causation". The Journal of hand surgery 33 (7): 1076–80. doi:10.1016/j.jhsa.2008.03.001. PMID 18762100.
- ^ Scangas, George; Santiago Lozano-Calderón, David Ring (September 2008). "Disparity Between Popular (Internet) and Scientific Illness Concepts of Carpal Tunnel Syndrome Causation". The Journal of Hand Surgery 33 (7): 1076–1080. doi:10.1016/j.jhsa.2008.03.001. PMID 18762100.
- ^ Anthony, Shawn; Santiago Lozano-Calderón, David Ring (March 2008). "Stigmatization of Repetitive Hand Use in Newspaper Reports of Hand Illness". HAND 3 (1): 30–33. doi:10.1007/s11552-007-9052-4. PMC 2528973. PMID 18780117. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=2528973.
- ^ a b Clinical Practice Guideline on the Treatment of Carpal Tunnel Syndrome. American Academy of Orthopaedic Surgeons. September 2008. http://www.aaos.org/Research/guidelines/CTSTreatmentGuideline.pdf.[page needed]
- ^ . PMID 16557211.
- ^ American Academy of Orthopaedic Surgeons (1996). Clinical Guideline on wrist pain. National Guideline clearinghouse.[unreliable medical source?]
- ^ Katz, Jeffrey N.; Simmons, Barry P. (2002). "Carpal Tunnel Syndrome". New England Journal of Medicine 346 (23): 1807–1812. doi:10.1056/NEJMcp013018. PMID 12050342.
- ^ Harris JS, ed (1998). Occupational Medicine Practice Guidelines: evaluation and management of common health problems and functional recovery in workers. Beverly Farms, Mass.: OEM Press. ISBN 978-1-883595-26-5.[page needed]
- ^ Premoselli, S; Sioli, P; Grossi, A; Cerri, C (2006). "Neutral wrist splinting in carpal tunnel syndrome: a 3- and 6-months clinical and neurophysiologic follow-up evaluation of night-only splint therapy". Europa medicophysica 42 (2): 121–6. PMID 16767058.
- ^ Michlovitz, SL (2004). "Conservative interventions for carpal tunnel syndrome". The Journal of orthopaedic and sports physical therapy 34 (10): 589–600. PMID 15552705.
- ^ Marshall, Shawn C; Tardif, Gaetan; Ashworth, Nigel L; Marshall, Shawn C (2007). "Local corticosteroid injection for carpal tunnel syndrome". In Marshall, Shawn C. Cochrane Database of Systematic Reviews. doi:10.1002/14651858.CD001554.pub2.
- ^ Hui, A.C.F.; Wong, S; Leung, CH; Tong, P; Mok, V; Poon, D; Li-Tsang, CW; Wong, LK et al. (2005). "A randomized controlled trial of surgery vs steroid injection for carpal tunnel syndrome". Neurology 64 (12): 2074–8. doi:10.1212/01.WNL.0000169017.79374.93. PMID 15985575.
- ^ Sato, Y; Honda, Y; Iwamoto, J; Kanoko, T; Satoh, K (2005). "Amelioration by mecobalamin of subclinical carpal tunnel syndrome involving unaffected limbs in stroke patients". Journal of the Neurological Sciences 231 (1–2): 13–8. doi:10.1016/j.jns.2004.12.005. PMID 15792815.
- ^ Hui, A.C.F.; Wong, S.M.; Tang, A.; Mok, V.; Hung, L.K.; Wong, K.S. (2004). "Long-term outcome of carpal tunnel syndrome after conservative treatment". International Journal of Clinical Practice 58 (4): 337–9. doi:10.1111/j.1368-5031.2004.00028.x. PMID 15161116.
- ^ Kouyoumdjian, JA; Morita, MP; Molina, AF; Zanetta, DM; Sato, AK; Rocha, CE; Fasanella, CC (2003). "Long-term outcomes of symptomatic electrodiagnosed carpal tunnel syndrome". Arquivos de neuro-psiquiatria 61 (2A): 194–8. doi:10.1590/S0004-282X2003000200007. PMID 12806496.
- ^ http://www.handuniversity.com/topics.asp?Topic_ID=16[dead link] A patient's guide to endoscopic carpal tunnel release[unreliable medical source?]
- ^ http://www.youtube.com/watch?v=M4hTY1vyrxg[unreliable medical source?]
- ^ Brown, RA; Gelberman, RH; Seiler Jg, 3rd; Abrahamsson, SO; Weiland, AJ; Urbaniak, JR; Schoenfeld, DA; Furcolo, D (1993). "Carpal tunnel release. A prospective, randomized assessment of open and endoscopic methods". The Journal of bone and joint surgery. American volume 75 (9): 1265–75. PMID 8408148. http://www.ejbjs.org/cgi/content/abstract/75/9/1265.
- ^ Trumble, Thomas E.; Diao, Edward; Abrams, Reid A.; Gilbert-Anderson, Mary M. (2002). "Single-portal endoscopic carpal tunnel release compared with open release : a prospective, randomized trial". The Journal of bone and joint surgery. American volume 84-A (7): 1107–15. PMID 12107308. http://www.ejbjs.org/cgi/content/abstract/84/7/1107.
- ^ "Carpal Tunnel Syndrome - Your Orthopaedic Connection - AAOS". Orthoinfo.aaos.org. 2009-12-01. http://orthoinfo.aaos.org/topic.cfm?topic=A00005. Retrieved 2011-10-05.
- ^ Berger, L. “Balloon Carpal Tunnelplasty, First Comparative Clinical Study”; The University of Pittsburgh Journal Vol 17, pg 80; 2006
- ^ Schmelzer, Rodney E.; Rocca, Gregory J. Della; Caplin, David A. (2006). "Endoscopic Carpal Tunnel Release: A Review of 753 Cases in 486 Patients". Plastic and Reconstructive Surgery 117 (1): 177–85. doi:10.1097/01.prs.0000194910.30455.16. PMID 16404264.
- ^ Quaglietta, Paolo; Corriero, G. (2005). Endoscopic carpal tunnel release surgery: retrospective study of 390 consecutive cases. "Advanced Peripheral Nerve Surgery and Minimal Invasive Spinal Surgery". Acta Neurochirurgica Supplementum. Acta Neurochirurgica 97: 41–5. doi:10.1007/3-211-27458-8_10. ISBN 3-211-23368-7.
- ^ Park, S.-H.; Cho, B. H.; Ryu, K. S.; Cho, B. M.; Oh, S. M.; Park, D. S. (2004). "Surgical Outcome of Endoscopic Carpal Tunnel Release in 100 Patients with Carpal Tunnel Syndrome". Minimally Invasive Neurosurgery 47 (5): 261–5. doi:10.1055/s-2004-830075. PMID 15578337.
- ^ Scholten, R; Bouter, LM; Gerritsen, A; Uitdehaag, BM; De Vet, HCW; Van Geldere, D; Scholten, Rob (2004). Surgical treatment options for carpal tunnel syndrome. In Scholten, Rob. "The Cochrane Database of Systematic Reviews". Cochrane Database of Systematic Reviews. doi:10.1002/14651858.CD003905.pub2.
- ^ McNally, S. A.; Hales, PF (2003). "Results of 1245 endoscopic carpal tunnel decompressions". Hand Surgery 8 (1): 111–6. doi:10.1142/S0218810403001480. PMID 12923945.
- ^ Thoma, Achilleas; Veltri, Karen; Haines, Ted; Duku, Eric (2004). "A Meta-Analysis of Randomized Controlled Trials Comparing Endoscopic and Open Carpal Tunnel Decompression". Plastic and Reconstructive Surgery: 1137–46. doi:10.1097/01.PRS.0000135850.37523.D0.
- ^ Chow, J; Hantes, M (2002). "Endoscopic carpal tunnel release: Thirteen years' experience with the chow technique". The Journal of Hand Surgery 27 (6): 1011–8. doi:10.1053/jhsu.2002.35884. PMID 12457351.
- ^ a b Ebenbichler, GR; Resch, KL; Nicolakis, P; Wiesinger, GF; Uhl, F; Ghanem, AH; Fialka, V (1998). "Ultrasound treatment for treating the carpal tunnel syndrome: randomised "sham" controlled trial". BMJ (Clinical research ed.) 316 (7133): 731–5. PMC 28476. PMID 9529407. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=28476.
- ^ Gurcay, E; Unlu, E, Gurcay, AG, Tuncay, R, Cakci, A (2010 Dec 14). "Assessment of phonophoresis and iontophoresis in the treatment of carpal tunnel syndrome: a randomized controlled trial". Rheumatology international. doi:10.1007/s00296-010-1706-9. PMID 21153642.
- ^ Yildiz, N; Atalay, NS, Gungen, GO, Sanal, E, Akkaya, N, Topuz, O (2011). "Comparison of ultrasound and ketoprofen phonophoresis in the treatment of carpal tunnel syndrome". Journal of back and musculoskeletal rehabilitation 24 (1): 39–47. doi:10.3233/BMR-2011-0273. PMID 21248399.
- ^ Muller, M; Tsui, D; Schnurr, R; Biddulph-Deisroth, L; Hard, J; MacDermid, JC (2004). "Effectiveness of hand therapy interventions in primary management of carpal tunnel syndrome: a systematic review". Journal of Hand Therapy 17 (2): 210–28. doi:10.1197/j.jht.2004.02.009. PMID 15162107.
- ^ Keith, M. W.; Masear, V., Chung, K. C., Amadio, P. C., Andary, M., Barth, R. W., Maupin, K., Graham, B., Watters, W. C., Turkelson, C. M., Haralson, R. H., Wies, J. L., McGowan, R. (4 January 2010). "American Academy of Orthopaedic Surgeons Clinical Practice Guideline on The Treatment of Carpal Tunnel Syndrome". The Journal of Bone and Joint Surgery 92 (1): 218–219. doi:10.2106/JBJS.I.00642. PMID 20048116.
- ^ Lincoln, A; Vernick, JS; Ogaitis, S; Smith, GS; Mitchell, CS; Agnew, J (2000). "Interventions for the primary prevention of work-related carpal tunnel syndrome". American Journal of Preventive Medicine 18 (4 Suppl): 37–50. doi:10.1016/S0749-3797(00)00140-9. PMID 10793280.
- ^ Verhagen, Arianne P; Karels, Celinde C; Bierma-Zeinstra, Sita MA; Burdorf, Lex L; Feleus, Anita; Dahaghin, Saede SD; De Vet, Henrica CW; Koes, Bart W et al. (2006). Ergonomic and physiotherapeutic interventions for treating work-related complaints of the arm, neck or shoulder in adults. In Verhagen, Arianne P. "Cochrane Database of Systematic Reviews". Cochrane Database of Systematic Reviews 3: CD003471. doi:10.1002/14651858.CD003471.pub3. PMID 16856010.
- ^ Olsen, K. M.; Knudson, D. V. (2001). "Change in Strength and Dexterity after Open Carpal Tunnel Release". International Journal of Sports Medicine 22 (4): 301–3. doi:10.1055/s-2001-13815. PMID 11414675.
- ^ Katz, Jeffrey N.; Losina, Elena; Amick, Benjamin C.; Fossel, Anne H.; Bessette, Louis; Keller, Robert B. (2001). "Predictors of outcomes of carpal tunnel release". Arthritis & Rheumatism 44 (5): 1184–93. doi:10.1002/1529-0131(200105)44:5<1184::AID-ANR202>3.0.CO;2-A.
- ^ Ruch, DS; Seal, CN; Bliss, MS; Smith, BP (2002). "Carpal tunnel release: efficacy and recurrence rate after a limited incision release". Journal of the Southern Orthopaedic Association 11 (3): 144–7. PMID 12539938.[unreliable medical source?]
- ^ a b Ashworth, Nigel L. (December 4, 2008). "Carpal Tunnel Syndrome". eMedicine. http://emedicine.medscape.com/article/327330-overview.
- ^ a b Amadio, Peter C. (2007). "History of carpal tunnel syndrome". In Luchetti, Riccardo; Amadio, Peter C.. Carpal Tunnel Syndrome. Berlin: Springer. pp. 3–9. ISBN 978-3-540-22387-0. http://books.google.com/books?id=LMA3dh605bgC&pg=PA3.
- ^ a b Fuller, David A. (September 22, 2010). "Carpal Tunnel Syndrome". eMedicine. http://emedicine.medscape.com/article/1243192-overview.
- ^ Prince Philip undergoes minor surgery on hand. BBC News. June 8, 2010. http://www.bbc.co.uk/news/10268511.
- ^ Rosen, Steven (Autumn 2004). "Green Day". Total Guitar: 24–30. http://www.greendayauthority.com/TheBand/articles/totalbass_pg2.jpg.
External links
- Carpal Tunnel Syndrome : Anatomy, Pathology, Causes, Clinical features, Diagnostic Tests and Treatment | Medchrome
- Carpal Tunnel Syndrome Fact Sheet (National Institute of Neurological Disorders and Stroke)
- Non-Surgical Treatment of Carpal Tunnel Syndrome
- Surgical Treatment of Carpal Tunnel Syndrome
- Carpal Tunnel Syndrome
- Carpal Tunnel Syndrome, information, diagnostic tool
Nervous system pathology, PNS, somatic (G50–G64, 350–357) Nerve, nerve root, plexus V (Trigeminal neuralgia, Anesthesia dolorosa) · VII (Facial nerve paralysis, Bell's palsy, Melkersson–Rosenthal syndrome, Parry–Romberg syndrome, Central seven) · XI (Accessory nerve disorder)Lower limbGeneralPolyneuropathies/Polyradiculoneuropathy OtherCategories:- Syndromes
Wikimedia Foundation. 2010.