- Cholecystectomy
-
Cholecystectomy Intervention ICD-9-CM 51.2 MeSH D002763 Cholecystectomy (
 /ˌkɒləsɪsˈtɛktəmi/; plural: cholecystectomies) is the surgical removal of the gallbladder. It is the most common method for treating symptomatic gallstones.[citation needed] Surgical options include the standard procedure, called laparoscopic cholecystectomy, and an older more invasive procedure, called open cholecystectomy.
/ˌkɒləsɪsˈtɛktəmi/; plural: cholecystectomies) is the surgical removal of the gallbladder. It is the most common method for treating symptomatic gallstones.[citation needed] Surgical options include the standard procedure, called laparoscopic cholecystectomy, and an older more invasive procedure, called open cholecystectomy.Contents
Open surgery
A traditional open cholecystectomy is a major abdominal surgery in which the surgeon removes the gallbladder through a 5- to 7-inch incision. Patients usually remain in the hospital at least 2 to 3 days and may require several additional weeks to recover at home. This procedure will therefore leave a right-sided subcostal scar.
Laparoscopic surgery
Laparoscopic cholecystectomy has now replaced open cholecystectomy as the first-choice of treatment for gallstones and inflammation of the gallbladder unless there are contraindications to the laparoscopic approach. This is because open surgery leaves the patient more prone to infection.[1] Sometimes, a laparoscopic cholecystectomy will be converted to an open cholecystectomy for technical reasons or safety.
 A US Navy general surgeon and an operating room nurse discuss proper procedures while performing a laparoscopic cholecystectomy surgery.
A US Navy general surgeon and an operating room nurse discuss proper procedures while performing a laparoscopic cholecystectomy surgery.
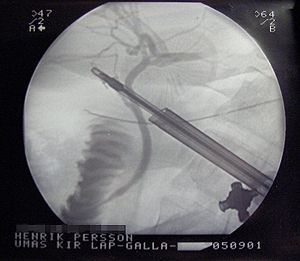
Laparoscopic cholecystectomy requires several small incisions in the abdomen to allow the insertion of operating ports, small cylindrical tubes approximately 5 to 10 mm in diameter, through which surgical instruments and a video camera are placed into the abdominal cavity. The camera illuminates the surgical field and sends a magnified image from inside the body to a video monitor, giving the surgeon a close-up view of the organs and tissues. The surgeon watches the monitor and performs the operation by manipulating the surgical instruments through the operating ports.
To begin the operation, the patient is placed in the supine position on the operating table and anesthetized. A scalpel is used to make a small incision at the umbilicus. Using either a Veress needle or Hasson technique the abdominal cavity is entered. The surgeon inflates the abdominal cavity with carbon dioxide to create a working space. The camera is placed through the umbilical port and the abdominal cavity is inspected. Additional ports are opened inferior to the ribs at the epigastric, midclavicular, and anterior axillary positions. The gallbladder fundus is identified, grasped, and retracted superiorly. With a second grasper, the gallbladder infundibulum is retracted laterally to expose and open Calot's Triangle (the area bound by the cystic artery, cystic duct, and common hepatic duct). The triangle is gently dissected to clear the peritoneal covering and obtain a view of the underlying structures. The cystic duct and the cystic artery are identified, clipped with tiny titanium clips and cut. Then the gallbladder is dissected away from the liver bed and removed through one of the ports. This type of surgery requires meticulous surgical skill, but in straightforward cases can be done in about an hour.
Recently, this procedure is performed through a single incision in the patient's umbilicus. This advanced technique is called Laparoendoscopic Single Site Surgery or "LESS".
Procedural risks and complications
Laparoscopic cholecystectomy does not require the abdominal muscles to be cut, resulting in less pain, quicker healing, improved cosmetic results, and fewer complications such as infection and adhesions. Most patients can be discharged on the same or following day as the surgery, and can return to any type of occupation in about a week. Furthermore, flexible instruments are being used in laparoscopic surgery by some surgeons. Using the SPIDER surgical system, they can perform the cholestectomy through a single incision through the navel. These patients often recover faster than traditional methods, and have an almost invisible scar.
An uncommon but potentially serious complication is injury to the common bile duct, which connects the gallbladder and liver. An injured bile duct can leak bile and cause a painful and potentially dangerous infection. Many cases of minor injury to the common bile duct can be managed non-surgically. Major injury to the bile duct, however, is a very serious problem and may require corrective surgery. This surgery should be performed by an experienced biliary surgeon.[2]
Abdominal peritoneal adhesions, gangrenous gallbladders, and other problems that obscure vision are discovered during about 5% of laparoscopic surgeries, forcing surgeons to switch to the standard cholecystectomy for safe removal of the gallbladder. Adhesions and gangrene, of course, can be quite serious, but converting to open surgery does not equate to a complication.
A Consensus Development Conference panel, convened by the National Institutes of Health in September 1992, endorsed laparoscopic cholecystectomy as a safe and effective surgical treatment for gallbladder removal, equal in efficacy to the traditional open surgery. The panel noted, however, that laparoscopic cholecystectomy should be performed only by experienced surgeons and only on patients who have symptoms of gallstones.
In addition, the panel noted that the outcome of laparoscopic cholecystectomy is greatly influenced by the training, experience, skill, and judgment of the surgeon performing the procedure. Therefore, the panel recommended that strict guidelines be developed for training and granting credentials in laparoscopic surgery, determining competence, and monitoring quality. According to the panel, efforts should continue toward developing a noninvasive approach to gallstone treatment that will not only eliminate existing stones, but also prevent their formation or recurrence.
One common complication of cholecystectomy is inadvertent injury to analogous bile ducts known as Ducts of Luschka, occurring in 33% of the population. It is non-problematic until the gall bladder is removed, and the tiny supravesicular ducts may be incompletely cauterized or remain unobserved, leading to biliary leak post-operatively. The patient will develop biliary peritonitis within 5 to 7 days following surgery, and will require a temporary biliary stent. It is important that the clinician recognize the possibility of bile peritonitis early and confirm diagnosis via HIDA scan to lower morbidity rate. Aggressive pain management and antibiotic therapy should be initiated as soon as diagnosed.
Biopsy
After removal, the gallbladder should be sent for pathological examination to confirm the diagnosis and look for an incidental cancer. If cancer is present, a reoperation to remove part of the liver and lymph nodes will be required in most cases.[3]
Long-term prognosis
A minority of the population, from 5% to 40%, develop a condition called postcholecystectomy syndrome, or PCS.[4] Symptoms can include gastrointestinal distress and persistent pain in the upper right abdomen.
As many as twenty percent of patients develop chronic diarrhea. The cause is unclear, but is presumed to involve the disturbance to the bile system. Most cases clear up within weeks, though in rare cases the condition may last for many years. It can be controlled with drugs.[5]
References
- ^ Soper NJ, Stockmann PT, Dunnegan DL, Ashley SW (August 1992). "Laparoscopic cholecystectomy. The new 'gold standard'?". Arch Surg 127 (8): 917–21; discussion 921–3. PMID 1386505.
- ^ Kapoor VK. "Bile duct injury repair – When? What? Who?" Journal of HBP Surgery 2007; 14: 476-9.
- ^ Kapoor VK. Incidental gall bladder cancer. American Journal of Gastroenterology 2001; 96: 627-629.
- ^ "Postcholecystectomy syndrome". WebMD. http://www.webmd.com/hw-popup/Postcholecystectomy-syndrome. Retrieved 2007-08-25.
- ^ Chronic diarrhea: A concern after g - MayoClinic.com
External links
Surgery: surgical procedures (including Ectomy, stomy, and otomy) Ectomy Genital♀: Cervicectomy · Clitoridectomy · Oophorectomy · Salpingoophorectomy · Salpingectomy · Hysterectomy · Vaginectomy · Vulvectomy
♂: Vasectomy · Penectomy · Orchidectomy · Prostatectomy · Posthectomy · GonadectomyMusculoskeletalcns (Decompressive craniectomy, Hemispherectomy, Anterior temporal lobectomy, Hypophysectomy, Amygdalohippocampectomy, Laminectomy, Corpectomy, Facetectomy) · pns (Ganglionectomy, Sympathectomy/Endoscopic thoracic sympathectomy, Neurectomy) · ear (Stapedectomy, Mastoidectomy) · eye (Photorefractive keratectomy, Trabeculectomy, Iridectomy, Vitrectomy)GastrointestinalGingivectomy · Glossectomy · Esophagectomy · Gastrectomy · Appendectomy · Proctocolectomy · Colectomy · Hepatectomy · Cholecystectomy · Pancreatectomy/PancreaticoduodenectomyRespiratoryEndocrineRenalLymphaticUngroupedEmbolectomy · Endarterectomy · Frenectomy · Ganglionectomy · Lobectomy · Myomectomy · Panniculectomy · PericardiectomyStomy GastrointestinalGastrostomy (Percutaneous endoscopic gastrostomy) · Gastroduodenostomy · Gastroenterostomy · Ileostomy · Jejunostomy · Colostomy · Cholecystostomy · HepatoportoenterostomyUrogenitalNervous systemOtomy UrogenitalNervous systemcns (Craniotomy, Pallidotomy, Thalamotomy, Lobotomy, Bilateral cingulotomy, Cordotomy, Rhizotomy, Laminotomy, Foraminotomy) · pns (Axotomy, Vagotomy) · ear (Myringotomy) · eye (Radial keratotomy)MusculoskeletalGastrointestinalRespiratoryCardiovascularUngroupedCategories:- Surgical removal procedures
- Accessory digestive gland surgery
Wikimedia Foundation. 2010.