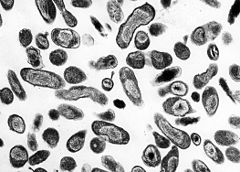
- Coxiella burnetii
-
Coxiella burnetii C. burnetii, the causative agent of Q fever Scientific classification Kingdom: Bacteria Phylum: Proteobacteria Class: Gammaproteobacteria Order: Legionellales Family: Coxiellaceae Genus: Coxiella Species: C. burnetii Binomial name Coxiella burnetii
(Derrick 1939)
Philip 1948Coxiella burnetii is an obligate intracellular bacterial pathogen, and is the causative agent of Q fever. The genus Coxiella is morphologically similar to Rickettsia, but with a variety of genetic and physiological differences. C. burnetii are small Gram-negative bacteria that are highly resistant to environmental stresses such as high temperature, osmotic pressure, and ultraviolet light. These characteristics are attributed to a small cell variant (SCV) form of the organism that is part of a biphasic developmental cycle including a more metabolically and replicatively active large cell variant (LCV) form.[1] It can survive standard disinfectants, and is resistant to many other environmental changes like those presented in the phagolysosome.[2]
Contents
History and naming
Research in the 1920s and 1930s identified what appeared to be a new type of Rickettsia, isolated from ticks, that was able to pass through filters. The first description of what may have been Coxiella burnetii was published in 1925 by Hideyo Noguchi, but, since his samples did not survive, it remains unclear as to whether it was the same organism. The definitive descriptions were published in the late 1930s as part of research into the cause of Q fever, by Edward Holbrook Derrick and Macfarlane Burnet in Australia, and Herald Rea Cox and Gordon Davis at the Rocky Mountain Laboratory (RML) in the United States.[3]
The RML team proposed the name Rickettsia diaporica, derived from the Greek word for having the ability to pass through filter pores, to avoid naming it after either Cox or Davis if indeed Noguchi's description had priority. Around the same time, Derrick proposed the name Rickettsia burnetii, in recognition of Burnet's contribution in identifying the organism as a Rickettsia. As it became clear that the species differed significantly from other Rickettsia, it was first elevated to a subgenus named after Cox, Coxiella, and then in 1948 to its own genus of that name, proposed by Cornelius B. Philip, another RML researcher.[3]
Coxiella was difficult to study because it could not be reproduced outside a host. However, in 2009, scientists reported a technique allowing the bacteria to grow in an axenic culture and suggested the technique may be useful for study of other pathogens.[4]
This is the main target of milk pasteurization.
Pathogenesis
The ID50 (the dose needed to infect 50% of experimental subjects) is one via inhalation; i.e., inhalation of one organism will yield disease in 50% of the population. This is an extremely low infectious dose, making C. burnetii the most infectious organism known to man.[5] Disease occurs in two stages: an acute stage that presents with headaches, chills, and respiratory symptoms, and an insidious chronic stage.
While most infections clear up spontaneously, treatment with tetracycline or doxycycline appears to reduce the symptomatic duration and reduce the likelihood of chronic infection. A combination of erythromycin and rifampin is highly effective in curing and prevention of disease and so is vaccination with Q-vax vaccine (CSL).
The bacteria use a Type IVB secretion system known as Icm/Dot to inject effector proteins called Ank proteins into the host. These effectors increase the bacteria's ability to survive inside the host cell. In Legionella pneumophila, which uses the same secretion system and also injects Ank proteins, survival is enhanced because these Ank proteins interfere with fusion of the bacteria-containing vacuole with the host's degradation endosomes.[6]
Use as a biological weapon
The United States ended its biological warfare program in 1969. When it did, C. burnetii was one of seven agents it had standardized as biological weapons.[7]
References
- ^ Voth, D. E. & Heinzen (2007), "Lounging in a lysosome: The intracellular lifestyle of Coxiella burnetii", Cellular Microbiology 9 (4): 1829–840, doi:10.1111/j.1462-5822.2007.00901.x, PMID 17381428
- ^ Sankaran, Neeraja (2000). "Coxiella burnetii". Microbes and people : an A-Z of microorganisms in our lives. Phoenix, Arizona: The Oryx Press. pp. 72. ISBN 1-57356-217-3. "In contrast to other rickettsiae, which are highly sensitive and easily killed by chemical disinfectants and changes in their surroundings, C. burnetii is highly resistant" & "Q fever". Centers for Disease Control and Prevention; National Center for Infectious Diseases; Division of Viral and Rickettsial Diseases; Viral and Rickettsial Zoonoses Branch. 2003-02-13. http://www.cdc.gov/ncidod/dvrd/qfever/index.htm. Retrieved 2006-05-24. "The organisms are resistant to heat, drying, and many common disinfectants."
- ^ a b McDade, Joseph E. (1990), "Historical Aspects of Q Fever", in Marrie, Thomas J., Q Fever, Volume I: The Disease, CRC Press, pp. 5–22, ISBN 0849359848
- ^ Omsland, Anders; Cockrell, Diane C.; Howe, Dale; Fischer, Elizabeth R.; Virtaneva, Kimmo; Sturdevant, Daniel E.; Porcella; Heinzen, Robert A. (2009), "Host cell-free growth of the Q fever bacterium Coxiella burnetii", PNAS 106 (11): 4430–4434, doi:10.1073/pnas.0812074106, PMC 2657411, PMID 19246385, http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=2657411
- ^ Q fever caused by Coxiella burnetii, http://www.cdc.gov/ncidod/dvrd/qfever/
- ^ Pan, X.; Lührmann, A.; Satoh, A.; Laskowski-Arce, M. A. & Roy, C. R. (2008), "Ankyrin repeat proteins comprise a diverse family of bacterial type IV effectors", Science 320 (5883): 1651–1654, doi:10.1126/science.1158160, PMC 2514061, PMID 18566289, http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=2514061
- ^ Croddy, Eric C. and Hart, C. Perez-Armendariz J., Chemical and Biological Warfare, (Google Books), Springer, 2002, pp. 30-31, (ISBN 0387950761), accessed October 24, 2008.
External links
- Coxiella burnetii genomes and related information at PATRIC, a Bioinformatics Resource Center funded by NIAID
Categories:- Proteobacteria
- Biological weapons
- Gram negative bacteria
Wikimedia Foundation. 2010.