- Dual-energy X-ray absorptiometry
-
Not to be confused with Bone scan.
Dual-energy X-ray absorptiometry Intervention 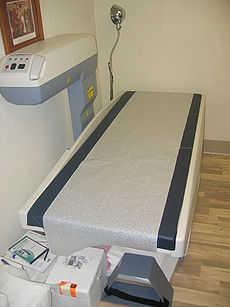
A scanner used to measure bone density with dual-energy X-ray absorptiometry.ICD-9-CM 88.98 OPS-301 code: 3-900 Dual-emission X-ray absorptiometry (DXA, previously DEXA) is a means of measuring bone mineral density (BMD). Two X-ray beams with differing energy levels are aimed at the patient's bones. When soft tissue absorption is subtracted out, the BMD can be determined from the absorption of each beam by bone. Dual-energy X-ray absorptiometry is the most widely used and most thoroughly studied bone density measurement technology.
The DXA scan is typically used to diagnose and follow osteoporosis. It is not to be confused with the nuclear bone scan, which is sensitive to certain metabolic diseases of bones in which bones are attempting to heal from infections, fractures, or tumors.
Contents
Uses
DXA scans are used primarily to evaluate bone mineral density. DXA scans can also be used to measure total body composition and fat content with a high degree of accuracy comparable to hydrostatic weighing with a few important caveats.[1][nb 1] However, it has been suggested that, while very accurately measuring minerals and lean soft tissue (LST), DXA may provide skewed results as a result of its method of indirectly calculating fat mass by subtracting it from the LST and/or body cell mass (BCM) that DXA actually measures.[2][nb 2]
Recommendations
Women over the age of 65 should get a DXA scan.[3] At risk women should consider getting a scan at age 60. 'At risk' includes many different clinical risk factors including: prior fragility fracture, use of glucocorticoids, heavy smoking, excess alcohol intake, rheumatoid arthritis, history of parental hip fracture, chronic renal and liver disease, chronic respiratory disease, long-term use of phenobarbitone or phenytoin, celiac disease, inflammatory bowel disease, and other risks. Clinical evidence on use of bone density scans in men is at present insufficient[3].
Scoring
The World Health Organization has defined the following categories based on bone density in white women:
Normal bone T-score greater than -1 Osteopenia T-score between -1 and -2.5 Osteoporosis T-score less than -2.5 Severe (established) osteoporosis T-score less than -2.5 and 1+ osteoporotic fractures The WHO committee did not have enough data to create definitions for men or other ethnic groups.[4] This test is very reliable.
Special considerations are involved in the use of DXA to assess bone mass in children. Specifically, comparing the bone mineral density of children to the reference data of adults (to calculate a T-score) will underestimate the BMD of children, because children have less bone mass than fully developed adults. This would lead to an over-diagnosis of osteopenia for children. To avoid an overestimation of bone mineral deficits, BMD scores are commonly compared to reference data for the same gender and age (by calculating a Z-score).
Also, there are other variables in addition to age that are suggested to confound the interpretation of BMD as measured by DXA. One important confounding variable is bone size. DXA has been shown to overestimate the bone mineral density of taller subjects and underestimate the bone mineral density of smaller subjects. This error is due to the way by which DXA calculates BMD. In DXA, bone mineral content (measured as the attenuation of the X-ray by the bones being scanned) is divided by the area (also measured by the machine) of the site being scanned.
Because DXA calculates BMD using area (aBMD: areal Bone Mineral Density), it is not an accurate measurement of true bone mineral density, which is mass divided by a volume. In order to distinguish DXA BMD from volumetric bone-mineral density, researchers sometimes refer to DXA BMD as an areal bone mineral density (aBMD). The confounding effect of differences in bone size is due to the missing depth value in the calculation of bone mineral density. Despite DXA technology's problems with estimating volume, it is still a fairly accurate measure of bone mineral content. Methods to correct for this shortcoming include the calculation of a volume that is approximated from the projected area measure by DXA. DXA BMD results adjusted in this manner are referred to as the bone mineral apparent density (BMAD) and are a ratio of the bone mineral content versus a cuboidal estimation of the volume of bone. Like the results for aBMD, BMAD results do not accurately represent true bone mineral density, since they use approximations of the bone's volume. BMAD is used primarily for research purposes and is not yet used in clinical settings.
Other imaging technologies such as Computed Quantitative Computer Tomography (QCT) are capable of measuring the bone's volume, and are, therefore, not susceptible to the confounding effect of bone-size in the way that DXA results are susceptible.
DXA uses X-rays to assess bone mineral density. However, the radiation dose is approximately 1/10 that of a standard chest X-ray.[5]
The quality of DXA operators varies widely. DXA is not regulated like other radiation based imaging techniques because of its low dosage. Each state has a different policy as to what certifications are needed to operate a DXA machine. California, for example, requires coursework and a state-run test, whereas Maryland has no requirements for DXA technicians. Many states require a training course and certificate from the International Society of Clinical Densitometry (ISCD). Because BMD testing with DXA is very susceptible to operator error, it is important to find out what qualifies the technician to operate the machine.[citation needed]
It is important for patients to get repeat BMD measurements done on the same machine each time, or at least a machine from the same manufacturer. Error between machines, or trying to convert measurements from one manufacturer's standard to another can introduce errors large enough to wipe out the sensitivity of the measurements.[citation needed]
DXA results need to be adjusted if the patient is taking strontium supplements [6][7]
Current clinical practice in paediatrics
DXA is, by far, the most widely used technique for bone measurements, since it is considered to be cheap, accessible, easy to use, and able to provide an accurate estimation of bone mineral density in adults.[8]
The official position of the International Society for Clinical Densitometry (ISCD) is that a patient may be tested for BMD if he suffers from a condition that could precipitate bone loss, is going to be prescribed pharmaceuticals known to cause bone loss, or is being treated and needs to be monitored. The ISCD states that there is no clearly understood correlation between BMD and the risk of a child's suffering a fracture; the diagnosis of osteoporosis in children cannot be made using the basis of a densitometry criteria. T-scores are prohibited with children and should not even appear on DXA reports. Thus, the WHO classification of osteoporosis and osteopenia in adults cannot be applied to children, but Z-scores can be used to assist diagnosis.[9]
Some clinics may routinely carry out DXA scans on paediatric patients with conditions such as nutritional rickets, lupus, and Turner Syndrome.[10] DXA has been demonstrated to measure skeletal maturity[11] and body fat composition[12] and has been used to evaluate the effects of pharmaceutical therapy.[13] It may also aid paediatricians in diagnosing and monitoring treatment of disorders of bone mass acquisition in childhood.[14]
However, it seems that DXA is still in its early days in paediatrics, and there are widely acknowledged limitations and disadvantages with DXA. A view exists[15] that DXA scans for diagnostic purposes should not even be performed outside specialist centers, and, if a scan is done outside one of these centers, it should not be interpreted without consultation with an expert in the field.[15] Furthermore, most of the pharmaceuticals given to adults with low bone mass can be given to children only in strictly monitored clinical trials.
Whole-body calcium measured by DXA has been validated in adults using in-vivo neutron activation of total body calcium[16][17] but this is not suitable for paediatric subjects and studies have been carried out on paediatric-sized animals.[16][17]
Radiation exposure
The radiation received by the patient during the scan is less than that of an airline flight from California to New York and back[citation needed] ].
Notes
- ^ In a different study, St-Onge explains "While DXA can be considered a major advance in body composition methodology [BCM], our findings show the limitation of LST [Lean Soft Tissue Mass] estimates as a marker of age-related changes in BCM and thus potentially functional outcomes. Although disease is also likely to alter the relationship of BCM to LST, our findings suggest BCM/LST in otherwise healthy participants might be a useful biomarker) basically explaining age and sex differences skew the results so that proper approximations must be made
- ^ Manninen cites the problem with DXA by explaining that "It should be noted, however, that DXA provides a measure of lean soft tissue (LST), and the original notion that LST hydration is constant is not correct. Rather, LST hydration varies as a function of extra- and intracellular water distribution."(p. 3) The discrepancy, he argued, was more likely to skew results in low-carbohydrate dieters as a result of hydration differences when compared to medium- and high-carbohydrate dieters and electrolyte supplementation, so that low hydration reduces LST mass, further reducing the ratio of LST to adipose mass (increasing bodyfat %)
References
- ^ St-Onge, Marie-Pierre; Jack Wang, Wei Shen, ZiMian Wang, David B. Allison, Stanley Heshka, Richard N. Pierson jr., Steven B. Heymsfield (March 2004). "Dual-Energy X-Ray Absorptiometry-Measured Lean Soft Tissue Mass: Differing Relation to Body Cell Mass Across the Adult Life Span". The Journals of Gerontology: Series A 59 (8): B796–B800. doi:10.1093/gerona/59.8.B796. PMID 15238354. http://biomedgerontology.oxfordjournals.org/content/59/8/B796.full. Retrieved 2010-04-02.
- ^ Manninen, Anssi (11 January 2006). "Very-low-carbohydrate diets and preservation of muscle mass". Nutrition & Metabolism 3: 9. doi:10.1186/1743-7075-3-9. PMC 1373635. PMID 16448570. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=1373635.
- ^ a b http://www.ahrq.gov/clinic/uspstf/uspsoste.htm
- ^ http://courses.washington.edu/bonephys/opbmd.html#tz
- ^ Radiology Info - DXA
- ^ http://www.osteopenia3.com/Strontium-dexa-scan.html
- ^ http://www.clinicaldensitometry.com/article/S1094-6950(06)00263-0/abstract "Effect of Bone Strontium on BMD Measurements" JCD Jan 2007
- ^ Gilsanz V, Eur J Radiol 1998, 26 177-182.
- ^ 2007 ISCD Official Positions, last accessed 19/05/2008.
- ^ Larry A.Binkovitz, Maria J.Henwood, Pediatr Radiol. 2006.
- ^ Pludowski P, Lebiedowski M, Lorenc RS, Osteoporos Int 2004, 14 317-322.
- ^ T Sung et al., Arch Dis Child 2001, 85 263-287.
- ^ Chris Barnes et al. Pediatric Research 2005, 52 578-581.
- ^ van der Sluis et al. Arch Dis Child 2002, 87 341-347.
- ^ a b Picaud et al. J Clin Densitom 2003, 6 17-23.
- ^ a b Margulies et al., J Clin Densitom 205, 8 298-304.
- ^ a b Horlick et al. J Bone Miner Res 2000, 15 1393-1397.
External links
- Non-invasive testing of bone density explained
- Information for patients, from RSNA
- Bone Densitometry explained
Medical testing : Medical imaging · Radiology · (ICD-9-CM V3 87-88, ICD-10-PCS B, CPT 70010-79999) X-ray/
medical radiography/
Industrial radiographyMedical: Pneumoencephalography · Dental radiography · Sialography · Myelography · CXR (Bronchography) · AXR / KUB · DXA/DXR · Upper gastrointestinal series/Small bowel follow-through/Lower gastrointestinal series · Cholangiography/Cholecystography · Mammography · Pyelogram · Cystography · Arthrogram · Hysterosalpingography · Skeletal survey · Angiography (Angiocardiography, Aortography) · Venography · Lymphogram
Industrial: Radiographic testingMedical: CT pulmonary angiogram · Cardiac CT · Abdominal and pelvic CT (Virtual colonoscopy) · CT angiography · CT head · pQCT · Spiral computed tomography · High resolution CT · Whole body imaging (Full-body CT scan) · Electron beam tomography
Industrial: Industrial CT ScanningOtherMRI MRI of brain and brain stem · MR neurography · Cardiac MRI/Cardiac MRI perfusion · MR angiography · MR cholangiopancreatography · Breast MRI
Functional MRI · Diffusion MRIUltrasound Echocardiography / Doppler echocardiography (TTE · TEE) · Intravascular · Gynecologic · Obstetric · Echoencephalography · Transcranial doppler · Abdominal ultrasonography · Transrectal · Breast ultrasound · Transscrotal ultrasound · Carotid ultrasonography
Contrast-enhanced · 3D ultrasound · Endoscopic ultrasound · Emergency ultrasound (FAST) · DuplexRadionuclide 2D / scintigraphyCholescintigraphy · Scintimammography · Ventilation/perfusion scan · Radionuclide ventriculography · Radionuclide angiography · Radioisotope renography · Sestamibi parathyroid scintigraphy · Radioactive iodine uptake test · Bone scintigraphy · Immunoscintigraphy
full body: Octreotide scan · Gallium 67 scan · Indium 111 WBC scan3D / ECTSPECT (gamma ray): SPECT of brain, Myocardial perfusion imaging
PET (positron): Brain PET, Cardiac PET, PET mammography, PET-CTOptical laser Thermography Breast thermographyCategories:- Radiology
- Measuring instruments
Wikimedia Foundation. 2010.
