- Chlortalidone
-
Chlortalidone 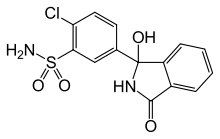
Systematic (IUPAC) name (RS)-2-chloro-5-(1-hydroxy-3-oxo-2,3-dihydro-1H-isoindol-1-yl)benzene-1-sulfonamide Clinical data Trade names Hygroton, Tenoretic AHFS/Drugs.com Consumer Drug Information MedlinePlus a682342 Pregnancy cat. C (Au), B (U.S.) Legal status POM (UK) Routes Oral Pharmacokinetic data Protein binding 75% Half-life 40 hours Excretion Renal Identifiers CAS number 77-36-1 ATC code C03BA04 PubChem CID 2732 DrugBank APRD00127 ChemSpider 2631 
UNII Q0MQD1073Q 
KEGG D00272 
ChEBI CHEBI:3654 
ChEMBL CHEMBL1055 
Chemical data Formula C14H11ClN2O4S Mol. mass 338.766 g/mol SMILES eMolecules & PubChem  (what is this?) (verify)
(what is this?) (verify)Chlortalidone (INN/BAN) or chlorthalidone (USAN) is a diuretic drug used to treat hypertension, originally marketed as Hygroton in the USA. It is described as a thiazide diuretic (or, rather, a thiazide-like diuretic because it acts similarly to the thiazides but does not contain the benzothiadiazine molecular structure). Compared with other medications of the thiazide class, chlorthalidone has the longest duration of action, but a similar diuretic effect at maximal therapeutic doses. It is often used in the management of hypertension and edema.
Unlike loop diuretics, chlorthalidone efficacy is diminished in patients with certain renal diseaes (e.g. Chronic Renal Disease). A clinical trial (ALLHAT) in 2002 compared chlorthalidone to doxazosin in the treatment of high-risk hypertensive patients. In this study, only chlorthalidone significantly reduced the risk of combined cardiovascular disease events, especially heart failure, when compared with drugs such as doxazosin.[1] Chlorthalidone was approved by the FDA in 1960. The ALLHAT study conclusions showed that there was no significant difference in all-cause mortality, fatal heart disease, or non-fatal myocardial infarction when chlorthalidone was compared with lisinopril or amlodipine but did show decrease rates of heart failure after 6 years when compared with amlodipine and decreased rates of cerebrovascular disease after 6 years when compared with lisinopril leading the study conclusions to say that thiazide-type diuretics are preferred first-step in antihypertensive therapy.
Mechanism of action
Chlorthalidone increases the excretion of sodium, chloride, and water into the renal lumen by inhibiting sodium ion transport across the renal tubular epithelium. Its primary site of action is in the cortical diluting segment of the ascending limb of the loop of Henle. Thiazides and related compounds also decrease the glomerular filtration rate, which further reduces the drug's efficacy in patients with renal impairment (e.g. renal insufficiency). By increasing the delivery of sodium to the distal renal tubule, chlorthalidone indirectly increases potassium excretion via the sodium-potassium exchange mechanism (i.e. apical ROMK/Na channels coupled with basolateral NKATPases). This can result in hypokalemia and hypochloremia as well as a mild metabolic alkalosis; however, the diuretic efficacy of chlorthalidone is not affected by the acid-base balance of the patient being treated.
Initially, diuretics lower blood pressure by decreasing cardiac output and reducing plasma and extracellular fluid volume. Eventually, cardiac output returns to normal, and plasma and extracellular fluid volume return to slightly less than normal, but a reduction in peripheral vascular resistance is maintained, thus resulting in an overall lower blood pressure. The reduction in intravascular volume induces an elevation in plasma renin activity and aldosterone secretion, further contributing to the potassium loss associated with thiazide diuretic therapy.
Combination products
It is also available as a combination product with the beta blocker atenolol, marketed in the UK as Co-tenidone and in the US as Tenoretic.
References
- ^ ALLHAT Officers and Coordinators for the ALLHAT Collaborative Research Group (December 18 2002). "Major outcomes in high-risk hypertensive patients randomized to angiotensin-converting enzyme inhibitor or calcium channel blocker vs diuretic: The Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial (ALLHAT)". JAMA 288 (23): 2981–97. doi:10.1001/jama.288.23.2981. PMID 12479763. http://jama.ama-assn.org/cgi/content/full/288/23/2981.
Symporter inhibitors Sodium chloride thiazide: Bendroflumethiazide • Chlorothiazide • Cyclopenthiazide • Cyclothiazide • Hydrochlorothiazide • Hydroflumethiazide • Methyclothiazide • Polythiazide • Trichlormethiazide
other: Chlorthalidone • MetolazoneSodium, potassium, chloride Antihypertensives: diuretics (C03) Sulfonamides
(except EA)CA inhibitors (at PT)Thiazide-likes (primarily DCT)Quinethazone • Clopamide • Chlortalidone • Mefruside • Clofenamide • Metolazone • Meticrane • Xipamide • Indapamide • Clorexolone • FenquizonePotassium-sparing (at CD) ESC blockersOsmotic diuretics (PT, DL) VAs (DCT and CD) vaptans: Conivaptan • Mozavaptan • Satavaptan • Tolvaptan
tetracyclines: DemeclocyclineOther Categories:- Diuretics
- Sulfonamides
- Isoindolines
- Organochlorides
- Lactams
Wikimedia Foundation. 2010.
