- Urticaria pigmentosa
-
Urticaria pigmentosa Classification and external resources 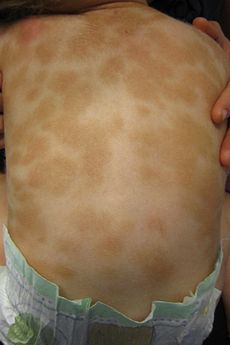
The back of a child with uriticaria pigmentosaICD-10 Q82.2 ICD-9 757.33 DiseasesDB 7864 MeSH D014582 Urticaria pigmentosa (also known as "Generalized eruption of cutaneous mastocytosis (childhood type)"[1]:616 ) is the most common form of cutaneous mastocytosis. It is a rare disease caused by excessive numbers of mast cells in the skin that produce hives or lesions on the skin when irritated.
Contents
Signs and symptoms
Urticaria Pigmentosa is characterized by excessive amounts of mast cells in the skin. Red or brown spots are often seen on the skin, typically around the chest and forehead. These mast cells, when irritated (e.g. by rubbing the skin, heat exposure), produce too much histamine, triggering an allergic reaction that leads to hives localized to the area of irritation, sometimes referred to as Darier's sign. Severe itching usually follows, and scratching the area only serves to further symptoms. Symptoms can range from very mild (flushing, hives, no treatment needed) to life-threatening (vascular collapse).
Cause
The majority of urticaria pigmentosa cases are caused by a point mutation at amino acid 816 of the proto-oncogene c-kit[2]. c-kit is a transmembrane protein which, when bound to Mast Cell Growth Factor (MCGF), signals the cell to divide. Mutations in position 816 of c-kit can result in a constant division signal being sent to the mast cells, resulting in abnormal proliferation. Different mutations have been linked to different onset times of the disease. For example, the Asp816Phe and Asp816Val mutations (the aspartate normally at position 816 in the c-kit protein has been replaced with phenylalanine or valine respectively) have been associated with early manifestation of the disease (mean age of onset: 1.3 and 5.9 months respectively). [3][4]
Irritants
The following can worsen the symptoms of urticaria pigmentosa:
- Emotional stress
- Physical stimuli such as heat, friction, and excessive exercise
- Bacterial toxins
- Venom
- Eye drops containing dextran
- NSAIDs
- Alcohol
- Morphine
The classification of NSAIDs can be disputed. Aspirin, for example, causes the mast cells to degranulate, releasing histamines and causing symptoms to flare. However, daily intake of 81 mg aspirin may keep the mast cells degranulated. Thus, while symptoms may be worsened at first, they can get better as the mast cells are unable to recharge with histamine.
Diagnosis
The disease is most often diagnosed as an infant, when parents take their baby in for what appears to be bug bites. The bug bites are actually the clumps of mast cells. Doctors can confirm the presence of mast cells by rubbing the baby's skin. If hives appear, it most likely signifies the presence of urticaria pigmentosa.
Treatments
There are no permanent cures for urticaria pigmentosa. However, treatments are possible. Most treatments for mastocytosis can be used to treat urticaria pigmentosa. Many common anti-allergy medications are useful because they reduce the mast cell's ability to react to histamine.[1]
At least one clinical study suggested that nifedipine, a calcium channel blocker used to treat high blood pressure, may reduce mast cell degranulation in patients with urticaria pigmentosa. A 1984 study by Fairly et al. included a patient with symptomatic urticaria pigmentosa who responded to nifedipine at dose of 10 mg po tid.[5] However, nifedipine has never been approved by the FDA for treatment of urticaria pigmentosa.
Another Mast cell stabilizer Gastrocrom, a form of Cromoglicic acid has also been used to reduce mast cell degranulation.
Epidemiology
Urticaria pigmentosa is an orphan disease, affecting fewer than 200,000 people in the United States.
See also
- Mastocytosis
- Mast Cells
- Urticaria
- Dermatographic urticaria
- Generalized eruption of cutaneous mastocytosis (adult type)
References
- ^ James, William; Berger, Timothy; Elston, Dirk (2005). Andrews' Diseases of the Skin: Clinical Dermatology. (10th ed.). Saunders. ISBN 0-7216-2921-0.
- ^ Akin C (2006). "Molecular Diagnosis of Mast Cell Disorders : A Paper from the 2005 William Beaumont Hospital Symposium on Molecular Pathology". J Mol Diagn 8 (4): 412–9. doi:10.2353/jmoldx.2006.060022. PMC 1867614. PMID 16931579. http://jmd.amjpathol.org/cgi/reprint/8/4/412.
- ^ Yanagihori H, Oyama N, Nakamura K, Kaneko F (2005). "c-kit Mutations in Patients with Childhood-Onset Mastocytosis and Genotype-Phenotype Correlation". J Mol Diagn 7 (2): 252–7. doi:10.1016/S1525-1578(10)60552-1. PMC 1867517. PMID 15858149. http://jmd.amjpathol.org/cgi/pmidlookup?view=long&pmid=15858149.
- ^ Sotlar K, Escribano L, Landt O, et al. (2003). "One-Step Detection of c-kit Point Mutations Using Peptide Nucleic Acid-Mediated Polymerase Chain Reaction Clamping and Hybridization Probes". Am. J. Pathol. 162 (3): 737–46. doi:10.1016/S0002-9440(10)63870-9. PMC 1868096. PMID 12598308. http://ajp.amjpathol.org/cgi/pmidlookup?view=long&pmid=12598308.
- ^ Fairley JA, Pentland AP, Voorhees JJ (1984). "Urticaria pigmentosa responsive to nifedipine". J. Am. Acad. Dermatol. 11 (4 Pt 2): 740–3. doi:10.1016/S0190-9622(84)70233-7. PMID 6491000.
External links
- DermAtlas 27
- The Mastocytosis Society
- Mastokids
- The Masto Forum
- UK Mastocytosis Support
- BC Health Guide
- About.com with Pictures
- Prevalence of Urticaria Pigmentosa
- Alto WA, Clarcq L (June 1999). "Cutaneous and systemic manifestations of mastocytosis". Am Fam Physician 59 (11): 3047–54, 3059–60. PMID 10392589. http://www.aafp.org/afp/990600ap/3047.html.
- The Skin Site
Congenital malformations and deformations of integument / skin disease (Q80–Q82, 757.0–757.3) Genodermatosis Congenital ichthyosis/
erythrokeratodermiaADARUngroupedIchthyosis bullosa of Siemens · Ichthyosis follicularis · Ichthyosis prematurity syndrome · Ichthyosis–sclerosing cholangitis syndrome · Nonbullous congenital ichthyosiform erythroderma · Ichthyosis linearis circumflexa · Ichthyosis hystrixEB
and relatedJEB (JEB-H, Mitis, Generalized atrophic, JEB-PA)related: Costello syndrome · Kindler syndrome · Laryngoonychocutaneous syndrome · Skin fragility syndrome ·Naegeli syndrome/Dermatopathia pigmentosa reticularis · Hay–Wells syndrome · Hypohidrotic ectodermal dysplasia · Focal dermal hypoplasia · Ellis–van Creveld syndrome · Rapp–Hodgkin syndrome/Hay–Wells syndromeEhlers–Danlos syndrome · Cutis laxa (Gerodermia osteodysplastica) · Popliteal pterygium syndrome · Pseudoxanthoma elasticum · Van Der Woude syndromeHyperkeratosis/
keratinopathydiffuse: Diffuse epidermolytic palmoplantar keratoderma • Diffuse nonepidermolytic palmoplantar keratoderma • Palmoplantar keratoderma of Sybert • Mal de Meleda •syndromic (connexin (Bart–Pumphrey syndrome • Clouston's hidrotic ectodermal dysplasia • Vohwinkel syndrome) • Corneodermatoosseous syndrome • plakoglobin (Naxos syndrome) • Scleroatrophic syndrome of Huriez • Olmsted syndrome • Cathepsin C (Papillon–Lefèvre syndrome • Haim–Munk syndrome) • Camisa diseasefocal: Focal palmoplantar keratoderma with oral mucosal hyperkeratosis • Focal palmoplantar and gingival keratosis • Howel–Evans syndrome • Pachyonychia congenita (Pachyonychia congenita type I • Pachyonychia congenita type II) • Striate palmoplantar keratoderma • Tyrosinemia type II)punctate: Acrokeratoelastoidosis of Costa • Focal acral hyperkeratosis • Keratosis punctata palmaris et plantaris • Keratosis punctata of the palmar creases • Schöpf–Schulz–Passarge syndrome • Porokeratosis plantaris discreta • Spiny keratodermaungrouped: Palmoplantar keratoderma and spastic paraplegia • desmoplakin (Carvajal syndrome) • connexin (Erythrokeratodermia variabilis • HID/KID)OtherMeleda disease · Keratosis pilaris · ATP2A2 (Darier's disease) · Dyskeratosis congenita · Lelis syndromeDyskeratosis congenita · Keratolytic winter erythema · Keratosis follicularis spinulosa decalvans · Keratosis linearis with ichthyosis congenital and sclerosing keratoderma syndrome · Keratosis pilaris atrophicans faciei · Keratosis pilarisOthercadherin (EEM syndrome) · immune system (Hereditary lymphedema, Mastocytosis/Urticaria pigmentosa) · Hailey–Hailey
see also Template:Congenital malformations and deformations of skin appendages, Template:Phakomatoses, Template:Pigmentation disorders, Template:DNA replication and repair-deficiency disorderDevelopmental
anomaliesMidlineOther/ungroupedAplasia cutis congenita · Amniotic band syndrome · Branchial cyst · Cavernous venous malformation
Accessory nail of the fifth toe · Bronchogenic cyst · Congenital cartilaginous rest of the neck · Congenital hypertrophy of the lateral fold of the hallux · Congenital lip pit · Congenital malformations of the dermatoglyphs · Congenital preauricular fistula · Congenital smooth muscle hamartoma · Cystic lymphatic malformation · Median raphe cyst · Melanotic neuroectodermal tumor of infancy · Mongolian spot · Nasolacrimal duct cyst · Omphalomesenteric duct cyst · Poland anomaly · Rapidly involuting congenital hemangioma · Rosenthal–Kloepfer syndrome · Skin dimple · Superficial lymphatic malformation · Thyroglossal duct cyst · Verrucous vascular malformation · BirthmarkCategories:- Rare diseases
- Dermal and subcutaneous growths
Wikimedia Foundation. 2010.
