- Negative pressure ventilator
-
This article is about the medical device. For the band, see Iron Lung (band).
Negative pressure ventilator Intervention 
An Emerson iron lung. The patient lies within the chamber, which when sealed provides an effectively oscillating atmospheric pressure. This particular machine was donated to the Centers for Disease Control and Prevention Museum by the family of poliomyelitis patient Barton Hebert of Covington, Louisiana, who had used the device from the late 1950s until his death in 2003.ICD-9-CM 93.99 MeSH D015919 A negative pressure ventilator (often referred to colloquially as an iron lung) is a form of medical ventilator that enables a person to breathe when normal muscle control has been lost or the work of breathing exceeds the person's ability.
Contents
Method and use
Humans, like most other animals, breathe by negative pressure breathing:[1] the rib cage expands and the diaphragm relaxes, expanding the chest cavity. This causes the pressure in the chest cavity to decrease, and the lungs expand to fill the space. This, in turn, causes the pressure of the air inside the lungs to decrease (it becomes negative, relative to the atmosphere), and air flows into the lungs from the atmosphere: inhalation. When the chest cavity is contracted, the reverse happens and the person exhales. If a person loses part or all of the ability to control the muscles involved, breathing becomes difficult or impossible.
The person using the iron lung is placed into the central chamber, a cylindrical steel drum. A door allowing the head and neck to remain free is then closed, forming a sealed, air-tight compartment enclosing the rest of the person's body. Pumps that control airflow periodically decrease and increase the air pressure within the chamber, and particularly, on the chest. When the pressure is below that within the lungs, the lungs expand and atmospheric pressure pushes air from outside the chamber in via the person's nose and airways to keep the lungs filled; when the pressure goes above that within the lungs, the reverse occurs, and air is expelled. In this manner, the iron lung mimics the physiological action of breathing: by periodically altering intrathoracic pressure, it causes air to flow in and out of the lungs. The iron lung is a form of non-invasive therapy.
Invention and early use
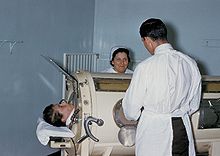 Staff in a Rhode Island hospital are examining a patient in an iron lung tank respirator during the 1960 polio epidemic. The iron lung encased the thoracic cavity in an air-tight chamber. The chamber was used to create a negative pressure around the thoracic cavity, thereby causing air to enter the lungs to equalize intrapulmonary pressure.
Staff in a Rhode Island hospital are examining a patient in an iron lung tank respirator during the 1960 polio epidemic. The iron lung encased the thoracic cavity in an air-tight chamber. The chamber was used to create a negative pressure around the thoracic cavity, thereby causing air to enter the lungs to equalize intrapulmonary pressure.
The first negative pressure ventilator was described by Scottish physician John Dalziel in 1832. Successful use of similar devices was described a few years later. The first of these devices to be widely used however was developed by Drinker and Shaw in 1928.[2] The iron lung, often referred to in the early days as the "Drinker respirator", was invented by Phillip Drinker (1894 – 1972) and Louis Agassiz Shaw Junior, professors of industrial hygiene at the Harvard School of Public Health.[3][4][5][6] The machine was powered by an electric motor with air pumps from two vacuum cleaners. The air pumps changed the pressure inside a rectangular, airtight metal box, pulling air in and out of the lungs.[7]
The first clinical use of the Drinker respirator on a human was on October 12, 1928 at the Children's Hospital in Boston.[4][8] The subject was an eight-year-old girl who was nearly dead as a result of respiratory failure due to poliomyelitis (often called polio or infantile paralysis).[6] Her dramatic recovery, within less than a minute of being placed in the chamber, helped popularize the new device.[5]
Boston manufacturer Warren E. Collins began production of the iron lung that year.[9][10] Although it was initially developed for the treatment of victims of coal gas poisoning, it was most famously used in the mid-20th century for the treatment of respiratory failure caused by poliomyelitis.[3]
In 1931, John Haven Emerson (February 5, 1906 – February 4, 1997) introduced an improved and less expensive iron lung.[11][12] The Emerson iron lung had a bed that could slide in and out of the cylinder as needed, and the tank had portal windows which allowed attendants to reach in and adjust limbs, sheets, or hot packs.[7] Drinker and Harvard University sued Emerson, claiming he had infringed on patent rights. Emerson defended himself by making the case that such lifesaving devices should be freely available to all.[7] Emerson also demonstrated that every aspect of Drinker's patents had been patented by others at earlier times. Emerson won the case, and Drinker's patents were declared invalid.
Modern usage
Rows of irons lungs filled hospital wards at the height of the polio outbreaks of the 1940s and 1950s. Polio vaccination programs have virtually eradicated new cases of poliomyelitis in the United States. Because of this, and also the development of modern ventilators and widespread use of tracheal intubation and tracheotomy, the iron lung has virtually disappeared from modern medicine. For example, in 1959, there were 1,200 people using tank respirators in the United States, but by 2004 there were only 39.[7]
Positive pressure ventilation systems are now more common than negative pressure systems. Positive pressure ventilators work by blowing air into the patient's lungs via intubation through the airway; they were used for the first time in Blegdams Hospital, Copenhagen, Denmark during a polio outbreak in 1952.[13][14] It proved a success and soon superseded the iron lung throughout Europe.
The iron lung now has a marginal place in modern respiratory therapy. Most patients with paralysis of the breathing muscles use modern mechanical ventilators that push air into the airway with positive pressure. These are generally efficacious and have the advantage of not restricting patients' movements or caregivers' ability to examine the patients as significantly as an iron lung does. However, negative pressure ventilation is a truer approximation of normal physiological breathing and results in more normal distribution of air in the lungs. It may also be preferable in certain rare conditions, such as Ondine's curse, in which failure of the medullary respiratory centers at the base of the brain result in patients having no autonomic control of breathing. At least one reported polio patient, Dianne Odell, had a spinal deformity that caused the use of mechanical ventilators to be contraindicated.[15] There are patients who today still use the older machines, often in their homes, despite the occasional difficulty of finding the various replacement parts. Joan Headley of Post-Polio Health International stated to CNN that there are approximately 30 patients in the USA still using an iron lung.[16] That figure may be inaccurately low; Houston alone had 19 iron lung patients living at home in 2008.[17] Martha Mason of Lattimore, North Carolina died on May 4, 2009, after spending 60 of her 72 years in an iron lung.[18]
On the 30th of October 2009, June Middleton of Melbourne, Australia, who had been entered in the Guinness Book of Records as the person who spent the longest time in an iron lung, died aged 83, having spent more than 60 years in her iron lung.[19]
Biphasic Cuirass Ventilation is a modern development of the iron lung, consisting of a wearable rigid upper-body shell (a cuirass) which functions as a negative pressure ventilator.
See also
- Both Respirator
References
- ^ "Gas Exchange in Humans". http://www.stemnet.nf.ca/~dpower/resp/exchange.htm. Retrieved 2011-07-01.
- ^ Laurie, Gini (2002). "Ventilator users, home care, and independent living: a historical perspective". In Gilgoff, Irene S.. Breath of Life: The Role of the Ventilator in Managing Life-Threatening Illnesses. Lanham, Maryland: Scarecrow Press, Inc.. pp. 161–201. ISBN 081083488X. http://books.google.com/books?id=ngA1izcCrFQC&pg=PA161&lpg=PA161&dq=%22Ventilator+users,+home+care,+and+independent+living:+a+historical+perspective%22&source=bl&ots=mpAz4WBI8A&sig=BCn90LxY7ISgXP6LegX9eQU91FA&hl=en&ei=-nEWTsCNPI2osAKqirEv&sa=X&oi=book_result&ct=result&resnum=2&ved=0CB4Q6AEwAQ#v=onepage&q=%22Ventilator%20users%2C%20home%20care%2C%20and%20independent%20living%3A%20a%20historical%20perspective%22&f=false.
- ^ a b Sherwood, RJ (1973). "Obituaries: Philip Drinker 1894–1972". The Annals of Occupational Hygiene 16 (1): 93–4. doi:10.1093/annhyg/16.1.93. http://annhyg.oxfordjournals.org/content/16/1/93.extract. Retrieved 2011-07-01.
- ^ a b Gorham, J (1979). "A medical triumph: the iron lung". Respiratory Therapy 9 (1): 71–3. PMID 10297356.
- ^ a b The Harvard Education and Research Center for Occupational Safety and Health (2010). "2010-2011 Student Handbook". Cambridge, Massachusetts: The Harvard Education and Research Center for Occupational Safety and Health. http://www.hsph.harvard.edu/research/erc/files/no_whoswho_editsept10updates.pdf. Retrieved 2011-07-02.
- ^ a b P.C. Rossin College of Engineering and Applied Science (2011). "Philip Drinker '17". Distinguished Alumni: Great Talents & Bright Minds. Bethlehem, Pennsylvania: Lehigh University. http://www3.lehigh.edu/engineering/about/drinker.asp. Retrieved 2011-07-01.
- ^ a b c d Kenneth E. Behring Center (2011). "The iron lung and other equipment". Whatever happened to polio?. Washington, DC: National Museum of American History. http://americanhistory.si.edu/polio/howpolio/ironlung.htm. Retrieved 2011-07-02.
- ^ Today in History: Iron Lung Used for the First Time (1928)
- ^ Julie K. Silver; Daniel J. Wilson (2007). Polio Voices. Santa Barbara: Praeger Publishers. p. 141.
- ^ "Artificial Lung on Wheels Prove Life Saver" Popular Mechanics, December 1930 photo of earliest production units from Boston
- ^ Geddes, LA (2007). "The history of artificial respiration". IEEE Engineering in Medicine and Biology Magazine: the Quarterly Magazine of the Engineering in Medicine & Biology Society 26 (6): 38–41. doi:10.1109/EMB.2007.907081. PMID 18189086.
- ^ "Iron Lung". National Museum of American History. http://americanhistory.si.edu/collections/object.cfm?key=35&objkey=114. Retrieved 2011-07-01.
- ^ Louise Reisner-Sénélar (2009). "The Danish anaesthesiologist Björn Ibsen a pioneer of long-term ventilation on the upper airways". https://docs.google.com/viewer?a=v&pid=explorer&chrome=true&srcid=0B7CdB217pf6yN2QxOGI5NTUtZWIzYS00N2NhLWFhODQtOGZjMjdhZTlkZGE5&hl=de. Retrieved 2011-07-01.
- ^ Wackers, Ger (1994). "Chapter 4: Theaters of truth and competence. Intermittent positive pressure respiration during the 1952 polio-epidemic in Copenhagen". http://www.fdcw.unimaas.nl/personal/WebSitesMWT/Wackers/proefschrift.html#h4. Retrieved 2011-07-01.
- ^ "Power failure kills iron lung lady". The Sydney Morning Herald. 2008-05-29. http://www.smh.com.au/news/world/power-failure-kills-iron-lung-lady/2008/05/29/1211654160059.html. Retrieved 2011-07-01.
- ^ "Woman dies after life spent in iron lung". May 28, 2008. http://www.cnn.com/2008/US/05/28/iron.lung.death.ap/index.html. Retrieved 2011-07-01.[dead link]
- ^ Lauran Neergaard (2009-01-13). "Emergency officials struggle to find those on life-support during power outages". http://www.ems1.com/ems-products/consulting-management/articles/447100-Emergency-officials-struggle-to-find-those-on-life-support-during-power-outages. Retrieved 2011-07-01.
- ^ Fox, Margalit (2009-05-10). "Martha Mason, Who Wrote Book About Her Decades in an Iron Lung, Dies at 71". The New York Times. http://www.nytimes.com/2009/05/10/us/10mason.html?_r=1&scp=1&sq=iron%20lung&st=cse. Retrieved 2011-07-01.
- ^ "Dead after 60 years in iron lung". The Sydney Morning Herald. 2009-11-01. http://www.smh.com.au/national/dead-after-60-years-in-iron-lung-20091101-hqyy.html?autostart=1. Retrieved 2011-07-01.
Further reading
- Emerson, JH; Loynes, JA (1978). The evolution of iron lungs: respirators of the body-encasing type. Cambridge, Massachusetts: J.H. Emerson Company.
- Martha Mason, a polio survivor, penned a best-selling memoir, Breath, about her life inside an iron lung.
- Margaret Atwood mentions an iron lung in her book Cat's Eye
- Peg Kehret mentions the use of an iron lung in her autobiographical book, Small Steps: The Year I Got Polio
- Elizabeth Berg shares a fictionalization of the true story of Pat Raming, the first woman to give birth to baby while in an iron lung, in her book, We are all Welcome Here. 2006.
External links
Respiratory system surgeries and other procedures (ICD-9-CM V3 21-22, 30-34, ICD-10-PCS 0B) Upper RT nose: Rhinoplasty · Septoplasty · Rhinectomy · Rhinomanometry
larynx: Laryngoscopy · Laryngectomy · Laryngotomy (Thyrotomy)Lower RT trachea: Cricothyrotomy · Tracheoesophageal puncture · Tracheotomy
lung: Pneumonectomy · Wedge resection · Lung transplantation · Decortication of lung · Heart-lung transplantChest wall, pleura,
mediastinum, and diaphragmMedical imaging Bronchography · CT pulmonary angiogram · High resolution CT · Spiral CT · Ventilation/perfusion scanCPRs Lung function test Cytology Respiratory therapy/
intubationMechanical ventilation · Positive pressure ventilation · Artificial respiration · Nebulizer · Hyperbaric medicine · Oxygen therapy · Decompression chamber · Heliox · Negative pressure ventilator · Postural drainage · CPRCategories:- Medical pumps
- Poliomyelitis
- Respiratory therapy
- 1928 introductions
- Mechanical ventilation
Wikimedia Foundation. 2010.

