- Erythrocyte sedimentation rate
-
Erythrocyte sedimentation rate Diagnostics 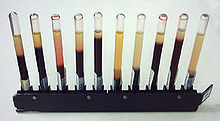
A rack of ESR tubes.MeSH D001799 LOINC 43402-7 The erythrocyte sedimentation rate (ESR), also called a sedimentation rate or Biernacki Reaction, is the rate at which red blood cells sediment in a period of 1 hour. It is a common hematology test that is a non-specific measure of inflammation. To perform the test, anticoagulated blood is placed in an upright tube, known as a Westergren tube, and the rate at which the red blood cells fall is measured and reported in mm/h.
Since the introduction of automated analyzers into the clinical laboratory, the ESR test has been automatically performed.
The ESR is governed by the balance between pro-sedimentation factors, mainly fibrinogen, and those factors resisting sedimentation, namely the negative charge of the erythrocytes (zeta potential). When an inflammatory process is present, the high proportion of fibrinogen in the blood causes red blood cells to stick to each other. The red cells form stacks called 'rouleaux,' which settle faster. Rouleaux formation can also occur in association with some lymphoproliferative disorders in which one or more immunoglobulin are secreted in high amounts. Rouleaux formation can, however, be a normal physiological finding in horses, cats, and pigs.
The ESR is increased by any cause or focus of inflammation. The ESR is increased in pregnancy or rheumatoid arthritis, and decreased in polycythemia, sickle cell anemia, hereditary spherocytosis, and congestive heart failure. The basal ESR is slightly higher in females.[1]
Contents
History
This test was invented in 1897 by the Polish doctor Edmund Biernacki.[2] In some parts of the world the test continues to be referred to as the Biernacki Test (Polish abbreviation: OB = Odczyn Biernackiego.) In 1918 the Swedish pathologist Robert Sanno Fåhræus declared the same and along with Alf Vilhelm Albertsson Westergren are eponymously remembered for the Fåhræus-Westergren test (abbreviated as FW test; in the UK, usually termed Westergren test),[3] which uses sodium citrate-coagulated specimens.[4]
Uses
Although it is frequently ordered, ESR is of limited use as a screening test in asymptomatic patients. It is useful for diagnosing diseases, such as multiple myeloma, temporal arteritis, polymyalgia rheumatica, various auto-immune diseases, systemic lupus erythematosus, rheumatoid arthritis, and chronic kidney diseases. In many of these cases, the ESR may exceed 100 mm/hour.[5]
It is commonly used for a differential diagnosis for Kawasaki's disease and it may be increased in some chronic infective conditions like tuberculosis and infective endocarditis. It is a component of the PDCAI, an index for assessment of severity of inflammatory bowel disease in children.
The clinical usefulness of ESR is limited to monitoring the response to therapy in certain inflammatory diseases such as temporal arteritis, polymyalgia rheumatica and rheumatoid arthritis. It can also be used as a crude measure of response in Hodgkin's lymphoma. Additionally, ESR levels are used to define one of the several possible adverse prognostic factors in the staging of Hodgkin's lymphoma. There is also a wintrobe method.
The use of the ESR as a screening test in asymptomatic persons is limited by its low sensitivity and specificity. When there is a moderate suspicion of disease, the ESR may have some value as a "sickness index."
Normal values
Note: mm/hr. = millimeters per hour.
Westergren's original normal values (men 3mm and women 7mm)[6] made no allowance for a person's age and in 1967 it was confirmed that ESR values tend to rise with age and to be generally higher in women.[7] Values are increased in states of anemia,[8] and in black populations.[9]
Adults
The widely used[10] rule for calculating normal maximum ESR values in adults (98% confidence limit) is given by a formula devised in 1983:[11]
ESR reference ranges from a large 1996 study with weaker confidence limits:[12]
Age 20 55 90 Men 12 20 19 Women 18 21 23 Children
Normal values of ESR have been quoted as 1[13] to 2[14] mm/hr at birth, rising to 4 mm/hr 8 days after delivery,[14] and then to 17 mm/hr by day 14.[13]
Typical normal ranges quoted are:[15]
- Newborn: 0 to 2 mm/hr
- Neonatal to puberty: 3 to 13 mm/hr, but other laboratories place an upper limit of 20.[16]
Relation to C-reactive protein
C-reactive protein is an acute phase protein produced by the liver during an inflammatory reaction. Since C-reactive protein levels in the blood rise more quickly after the inflammatory or infective process begins, ESR is often replaced with C-reactive protein measurement. There are specific drawbacks, however, for example, both tests for ESR and CRP were found to be independently associated with a diagnosis of acute maxillary sinusitis [17] so in some cases the combination of the two measurements may improve diagnostic sensitivity and specificity.
External links
- ESR Blood Test Interpretation
- ESR Blood Test Results Explained
- Erythrocyte Sedimentation Rate
- American Family Physician article on ESR
References
- ^ http://www.nlm.nih.gov/medlineplus/ency/article/003638.htm
- ^ Edmund Faustyn Biernacki and eponymously named Biernacki's test at Who Named It?
- ^ Robert (Robin) Sanno Fåhræus and Alf Vilhelm Albertsson Westergren who are eponymously named for the Fåhræus-Westergren test (aka Westergren test) at Who Named It?
- ^ International Council for Standardization in Haematology (Expert Panel on Blood Rheology) (1993). "ICSH recommendations for measurement of erythrocyte sedimentation rate. International Council for Standardization in Haematology (Expert Panel on Blood Rheology)". J. Clin. Pathol. 46 (3): 198–203. doi:10.1136/jcp.46.3.198. PMC 501169. PMID 8463411. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=501169.
- ^ "Sedimentation Rate". WebMD. 2006-06-16. http://www.webmd.com/a-to-z-guides/sedimentation-rate. Retrieved 2008-03-01.
- ^ Westergren A (1957). "Diagnostic tests: the erythrocyte sedimentation rate range and limitations of the technique". Triangle 3 (1): 20–5. PMID 13455726.
- ^ Böttiger LE, Svedberg CA (1967). "Normal erythrocyte sedimentation rate and age". Br Med J 2 (5544): 85–7. doi:10.1136/bmj.2.5544.85. PMC 1841240. PMID 6020854. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=1841240.
- ^ Kanfer EJ, Nicol BA (1997). "Haemoglobin concentration and erythrocyte sedimentation rate in primary care patients" (Scanned & PDF). Journal of the Royal Society of Medicine 90 (1): 16–8. PMC 1296109. PMID 9059375. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=1296109.
- ^ Gillum RF (1993). "A racial difference in erythrocyte sedimentation". Journal of the National Medical Association 85 (1): 47–50. PMC 2571720. PMID 8426384. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=2571720.
- ^ Reference range (ESR) at GPnotebook
- ^ Miller A, Green M, Robinson D (1983). "Simple rule for calculating normal erythrocyte sedimentation rate". Br Med J (Clin Res Ed) 286 (6361): 266. doi:10.1136/bmj.286.6361.266. PMC 1546487. PMID 6402065. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=1546487.
- ^ Wetteland P, Røger M, Solberg HE, Iversen OH (1996). "Population-based erythrocyte sedimentation rates in 3910 subjectively healthy Norwegian adults. A statistical study based on men and women from the Oslo area". J. Intern. Med. 240 (3): 125–31. doi:10.1046/j.1365-2796.1996.30295851000.x. PMID 8862121. - listing upper reference levels expected to be exceeded only by chance in 5% of subjects
- ^ a b Adler SM, Denton RL (1975). "The erythrocyte sedimentation rate in the newborn period". J. Pediatr. 86 (6): 942–8. doi:10.1016/S0022-3476(75)80233-2. PMID 1168702.
- ^ a b Ibsen KK, Nielsen M, Prag J, et al. (1980). "The value of the micromethod erythrocyte sedimentation rate in the diagnosis of infections in newborns". Scand J Infect Dis Suppl Suppl 23: 143–5. PMID 6937959.
- ^ MedlinePlus Encyclopedia ESR
- ^ Mack DR, Langton C, Markowitz J, et al. (2007). "Laboratory values for children with newly diagnosed inflammatory bowel disease". Pediatrics 119 (6): 1113–9. doi:10.1542/peds.2006-1865. PMID 17545378. - as commented on at
* Bauchner H (2007-06-13). "Lab Screening in Children with Suspected Inflammatory Bowel Disease". Journal Watch Pediatrics and Adolescent Medicine. http://pediatrics.jwatch.org/cgi/content/full/2007/613/2. Retrieved 2008-03-01. - ^ Jens Georg Hansen, Henrik Schmidt, Jorn Rosborg, Elisabeth Lund (22 July 1995). "Predicting acute maxillary sinusitis in a general practice population". BMJ 311 (6999): 233–236. PMC 2550286. PMID 7627042. http://www.bmj.com/cgi/content/full/311/6999/233.
MEP CBC (Platelet count) · Mean platelet volume · vWF: Ristocetin induced platelet agglutination
clotting factors: Prothrombin time · Partial thromboplastin time · Thrombin time
other/general coagulation: Bleeding time · animal enzyme (Reptilase time, Ecarin clotting time, Dilute Russell's viper venom time) · Thromboelastography
fibrinolysis: Euglobulin lysis time · D-dimerRed blood cell indices
(erythrocytes)CFU-GM Other Categories:- Blood tests
Wikimedia Foundation. 2010.

