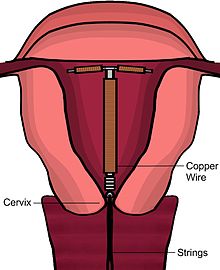
- IUD with copper
-
This article is about non-hormonally-based intrauterine contraceptives. For hormonally-based intrauterine contraceptives such as Mirena, see Hormonal IUD.
IUD with copper 
Photo of a common IUD (Paragard T 380A)Background Birth control type Intra-uterine First use 1909–1929 Failure rates (first year) Perfect use 0.6% Typical use 0.8% Usage Duration effect 5–12+ years Reversibility Immediate User reminders Check thread position after each period. Have removed shortly after menopause, if not before. Clinic review Annually Advantages and disadvantages STD protection No Periods May be heavier and more painful Benefits Unnecessary to take any daily action.
Emergency contraception if inserted within 5 daysRisks Small transient risk of PID in first 20 days following insertion.
Rarely, uterine perforation.Intrauterine device Intervention ICD-9-CM 69.7 A copper IUD (ATC G02BA) (also intrauterine device, IUD, copper-T, or coil) is a type of intrauterine device. Most IUDs have a plastic T- or U-shaped frame which is wrapped in copper wire, with the exception of Gynefix, which is a plastic string with several copper beads, affixed to the fundus of the uterus. The device has to be fitted inside and removed from the uterus by a doctor or qualified medical practitioner. It remains in place the entire time pregnancy is not desired.
The IUD is a long acting reversible contraceptive, with different IUDs intended to last for different lengths of time, between 3 and 10 years. Trials have demonstrated the copper T 380A to be effective for at least 12 years.[1] The length of time that the device lasts depends mainly on the amount of exposed copper, which is indicated, in square millimeters, by a number in the name of each device (i.e., the Paragard T-380A has 380 square millimeters of exposed copper).
The IUD is the world's most widely used method of reversible birth control,[2] currently used by nearly 160 million women (just over two-thirds of whom are in China where it is the most widely used birth control method, surpassing sterilization).[3]
Contents
History
According to popular legend, Arab traders inserted small stones into the uteruses of their camels to prevent pregnancy during long desert treks. The story was originally a tall tale to entertain delegates at a scientific conference on family planning; although it was later repeated as truth, it has no known historical basis.[4]
Precursors to IUDs were first marketed in 1902. Developed from stem pessaries (where the stem held the pessary in place over the cervix), the 'stem' on these devices actually extended into the uterus itself. Because they occupied both the vagina and the uterus, this type of stem pessary was also known as an intrauterine device. Use of intrauterine devices was associated with high rates of infection; for this reason, they were condemned by the medical community.[5]
The first intrauterine device (contained entirely in the uterus) was described in a German publication in 1909, although the author appears to have never marketed his product.[6]
In 1929, Dr. Ernst Gräfenberg of Germany published a report on an IUD made of silk suture. He had found a 3% pregnancy rate among 1,100 women using his ring. In 1930, Dr. Gräfenberg reported a lower pregnancy rate of 1.6% among 600 women using an improved ring wrapped in silver wire. Unbeknownst to Dr. Gräfenberg, the silver wire was contaminated with 26% copper. Copper's role in increasing IUD efficacy would not be recognized until nearly 40 years later.
In 1934, Japanese physician Tenrei Ota developed a variation of the Gräfenberg ring that contained a supportive structure in the center. The addition of this central disc lowered the IUD's expulsion rate. These devices still had high rates of infection, and their use and development was further stifled by World War II politics: contraception was forbidden in both Nazi Germany and Axis-allied Japan. The Western world did not learn of the work by Gräfenberg and Ota until well after the war ended.[6]
The first plastic IUD, the Margulies Coil or Margulies Spiral, was introduced in 1958. This device was somewhat large, causing discomfort to a large proportion of women users, and had a hard plastic tail, causing discomfort to their male partners. The modern colloquialism "coil" is based on the coil-shaped design of early IUDs.
The Lippes Loop, a slightly smaller device with a monofilament tail, was introduced in 1962 and gained in popularity over the Margulies device.[5]
The stainless steel single-ring IUD was developed in the 1970s[7] and widely used in China because of low manufacturing costs. The Chinese government banned production of steel IUDs in 1993 due to high failure rates (up to 10% per year).[8][9]
Dr. Howard Tatum, in the USA, conceived the plastic T-shaped IUD in 1968. Shortly thereafter Dr. Jaime Zipper, in Chile, introduced the idea of adding copper to the devices to improve their contraceptive effectiveness.[5][10] It was found that copper-containing devices could be made in smaller sizes without compromising effectiveness, resulting in fewer side effects such as pain and bleeding.[11] T-shaped devices had lower rates of expulsion due to their greater similarity to the shape of the uterus.[6]
The poorly designed Dalkon Shield plastic IUD (which had a multifilament tail) was manufactured by the A. H. Robins Company and sold by Robins in the United States for three and a half years from January 1971 through June 1974, before sales were suspended by Robins on June 28, 1974 at the request of the FDA because of safety concerns following reports of 110 septic spontaneous abortions in women with the Dalkon Shield in place, seven of whom had died.[12][13] Robins stopped international sales of the Dalkon Shield in April 1975.[14]
Second-generation copper-T IUDs were also introduced in the 1970s. These devices had higher surface areas of copper, and for the first time consistently achieved effectiveness rates of greater than 99%.[11] In addition to T-shaped IUDs, there are also U-shaped IUDs (such as the Multiload) and 7-shaped Gravigard Copper 7 (with a mini version for nulliparous women introduced in the 1980s). More recently, a frameless IUD called Gynefix was introduced.
Mechanism of contraception and effectiveness
The mechanism of IUDs is not well understood. It is known however that the presence of a device in the uterus prompts the release of leukocytes and prostaglandins by the endometrium. These substances are hostile to both sperm and eggs; the presence of copper increases the spermicidal effect.[15][16] The general medical consensus is that spermicidal and ovicidal mechanisms are the only way in which IUDs work.[17] Some physicians and medical texts have suggested they may have a secondary effect of interfering with the development of pre-implanted embryos;[18] this secondary effect is considered more plausible when the IUD is used as emergency contraception.[19]
Second-generation copper-T IUDs have failure rates of less than 1% per year, and cumulative 10-year failure rates of 2-6%.[9] A copper IUD may also be used as emergency contraception. If an IUD is inserted within five days of unprotected intercourse, a woman's chance of pregnancy is reduced to that of ongoing IUD users.[20] A large World Health Organization trial reported a cumulative 12-year failure rate of 2.2% for the T 380A (ParaGard) (an average failure rate of 0.18% per year over 12 years), equivalent to a cumulative 10-year failure rate of 1.8% following tubal ligation.[1] The frameless GyneFix also has a failure rate of less than 1% per year.[21] Worldwide, older IUD models with lower effectiveness rates are no longer produced.[11]
Insertion
Both insertion and removal is performed by a medical professional, and informed consent may be required. Before placement of an IUD, a medical history and physical examination by a medical professional is useful to check for any contraindications or concerns.[22]
A copper IUD can be inserted at any phase of the menstrual cycle, but the optimal time is right after the menstrual period, when the cervix is softest and the woman is least likely to be pregnant.[22] Uterine sounding may be used to measure the length and direction of the cervical canal and uterus in order to decrease the risk of uterine perforation.[23] A speculum is used to hold the vagina open, a tenaculum is used to steady the cervix and uterus, and a tube is used to place the IUD.[22]
After the insertion is finished, normal activities such as sex, exercise, and swimming can be performed as soon as it feels comfortable.[22] Strenuous physical activity does not affect the position of the IUD.[22]
Contraindications
The WHO Medical Eligibility Criteria for Contraceptive Use and RCOG Faculty of Family Planning & Reproductive Health Care (FFPRHC) UK Medical Eligibility Criteria for Contraceptive Use list the following as conditions where insertion of a copper IUD is not usually recommended (category 3) or conditions where a copper IUD should not be inserted (category 4):[24][25]
Category 3. Conditions where the theoretical or proven risks usually outweigh the advantages of inserting a copper IUD:
- Postpartum between 48 hours and 4 weeks (increased IUD expulsion rate with delayed postpartum insertion)
- Benign gestational trophoblastic disease
- Ovarian cancer
- Very high individual likelihood of exposure to gonorrhea or chlamydial STIs
- AIDS (unless clinically well on anti-retroviral therapy)
Category 4. Conditions which represent an unacceptable health risk if a copper IUD is inserted:
- Pregnancy
- Postpartum puerperal sepsis
- Immediately after a septic abortion
- Before evaluation of unexplained vaginal bleeding suspected of being a serious condition
- Malignant gestational trophoblastic disease
- Cervical cancer (awaiting treatment)
- Endometrial cancer
- Distortions of the uterine cavity by uterine fibroids or anatomical abnormalities
- Current pelvic inflammatory disease
- Current purulent cervicitis, chlamydial infection, or gonorrheal STIs
- Known pelvic tuberculosis
Some concern has been expressed that women with metal sensitivities to copper or nickel may experience adverse reactions from an IUD. The metal used in IUDs is 99.99% copper, with one study finding a maximum nickel content of 0.001%. Because nickel has a relatively high sensitizing potential, a few researchers suggested even this tiny amount might be problematic. A few case reports have attributed eczematous dermatitis and urticaria in a handful of users of copper-releasing IUDs to systemic copper or nickel allergic contact dermatitis. However, the daily metal absorption from an IUD is only a fraction of the normal daily absorption from food, and many dermatologists are skeptical that the symptoms described in the case reports were actually caused by metal sensitivity.[26][27][28]
While nulliparous women (women who have never given birth) are somewhat more likely to have side effects, this is not a contraindication for IUD use. Overall, IUDs are safe and acceptable also in young nulliparous women.[29] The same is likely the case for virgin women, unless there is a microperforate hymen that obstructs any insertion of the IUD.
Some doctors prefer to insert the IUD during menstruation to verify that the woman is not pregnant at the time of insertion. However, IUDs may safely be inserted at any time during the menstrual cycle as long as it is reasonably certain the woman is not pregnant.[30] Insertion may be more comfortable if done midcycle, when the cervix is naturally dilated.[31]
Side effects and complications
During insertion
Insertion of the IUD may introduce bacteria into the uterus. The insertion process carries an increased risk of pelvic inflammatory disease in the first 20 days following insertion,[32] but the risk is still low, and is attributable to preexisting gonorrhea or chlamydia infection present in the cervix at the time of insertion, and not to the IUD itself.[33] Proper infection prevention procedures have little or no effect on the course of gonorrhea or chlamydia infections, but is important in helping protect both clients and providers from infection in general.[33] Such infection prevention practices include washing hands and then putting on gloves, cleaning the cervix and vagina, making minimal contact with non-sterile surfaces (using a "no touch insertion technique") and, after the procedure, washing hands again and then processing instruments.[34] Antibiotics should be given before insertion to women at high risk for endocarditis (infection of the valves within the heart), but should not be used routinely.[35]
The cervix is dilated in order to sound (measure) the uterus and insert the IUD. Cervix dilation can be uncomfortable and, for some women, painful. Taking NSAIDS before the procedure can reduce discomfort,[36] as can the use of a local anaesthetic. Misoprostol 6 to 12 hrs before insertion can help with cervical dilatation.[36]
Uterine sounding is performed in order to measure the length and direction of the cervical canal and uterus. This reduces the risk of perforating the uterus with the IUD. This may occur when the IUD is inserted too deeply or at the wrong angle.[37] Uterine perforation is generally caused by an inexperienced provider and is very rare.
After insertion
After IUD insertion, menstrual periods are often heavier, more painful, or both - especially for the first few months after they are inserted. On average, menstrual blood loss increases by 20–50% after insertion of a copper-T IUD; increased menstrual discomfort is the most common medical reason for IUD removal.[38]
Expulsion is more common in younger women, women who have not had children, and when an IUD is inserted immediately after childbirth or abortion. Women should check the string of the IUD at least once per menstrual cycle to verify that it is still in place.
The string(s) may be felt by some men during intercourse. If this is problematic, the provider may cut the strings even down to the cervix, so they cannot be felt. Shortening the strings does prevent the woman from checking for expulsion, however.
The risk of ectopic pregnancy to a woman using an IUD is lower than the risk of ectopic pregnancy to a woman using no form of birth control. However, of pregnancies that do occur during IUD use, a higher than expected percentage (3–4%) are ectopic.[39]
The pregnancy rate during IUD use is very low (less than 1% per year). If pregnancy does occur, the IUD should be removed. Although IUDs are not teratogenic,[17] presence of the IUD increases the risk of miscarriage, particularly during the second trimester. It also increases the risk of premature delivery. Although the Dalkon Shield IUD was associated with septic abortions (infections associated with miscarriage), other brands of IUD are not. IUDs are also not associated with birth defects.[40]
Non-hormonal (copper) IUDs are considered safe to use while breastfeeding.[41]
Some barrier contraceptives protect against STDs. Hormonal contraceptives reduce the risk of developing pelvic inflammatory disease (PID), a serious complication of certain STDs. IUDs, by contrast, do not protect against STDs or PID.[32]
Use as emergency contraception
Intrauterine devices can be used as emergency contraception to prevent pregnancy up to 5 days after unprotected sexual intercourse, or sexual intercourse during which the primary contraception is believed to have failed (e.g. a condom was used, but it broke). Insertion of a copper-T IUD as emergency contraception is more than 99% effective, making it more effective than emergency contraceptive pills (ECP or 'morning-after pill').[20]
Prevalence
 A sign in Futu, Hubei, suggests getting an IUD after the first childbirth, and a tubal ligation after the second
A sign in Futu, Hubei, suggests getting an IUD after the first childbirth, and a tubal ligation after the second
The IUD is the world's most widely used method of reversible birth control,[2] currently used by nearly 160 million women (just over two-thirds of whom are in China where it is the most widely used birth control method, surpassing sterilization).[3] Usage in many countries has been measured by surveys of married women of reproductive age. In this population in the 1990s, IUD use ranged from 1.5% in North America, to 18% in Scandinavia, 33% in Russia and China, and 40% in Kazakhstan.[42] Use in China increased to 45% of married women by 2002.[3]
Among women who recently had sex and are not trying to become pregnant, 1.9% use IUDs in the United States, 6% in the United Kingdom and 20% in France.[43]
In the U.S., the ParaGard T 380A was approved by the FDA in 1984 and became available for use in 1988. and was used by 1.3% of women of reproductive age in a 2002 U.S. survey.[44]
Types of IUDs available
Many different types of copper IUDs are currently manufactured worldwide, but availability varies widely by country. For example, in the United States, only one type of copper IUD is approved for use,[44] while in the United Kingdom, over ten varieties are available.[45] One company, Mona Lisa N.V. offers generic versions of many existing IUDs.[46]
IUD Type Copper (mg2) Life (years) Manufacturer Distinguishing characteristics Multiload Cu375 U-shaped 375 5 Multilan Multiload Cu250 U-shaped 250 3 Multilan Multi-Safe 375 U-shaped 375 5 Williams Medical Supplies Multi-Safe 375 Short Loop U-shaped 375 5 Williams Medical Supplies Load 375 U-shaped 375 5 7-MED Industrie Nova-T 380 T-shaped (plain) 380 5 Bayer Neo-Safe T 380 T-shaped (plain) 380 5 Durbin UT 380 T-shaped (plain) 380 5 7-MED Industrie UT 380 Short T-shaped (plain) 380 5 7-MED Industrie Flexi-T 300 T-shaped (plain) 300 5 Prosan Flexi-T + 300 T-shaped (plain) 300 5 Prosan Wider arms than Flexi-T 300 T-safe CU 380A T-shaped (banded) 380 8 Durbin Flexi-T + 380 T-shaped (banded) 380 5 Prosan TT 380 Slimline T-shaped (banded) 380 10 7-MED Industrie Paragard T-shaped (banded) 380 10 Duramed Gynefix 330 (standard) Frameless 330 5 Contrel Only frameless IUD brand available Gynefix 200 (mini) Frameless 200 3 Contrel Only frameless IUD brand available IUD Type Copper (mg2) Life (years) Manufacturer Distinguishing characteristics See also
References
- ^ a b World Health Organization (1997). "Long-term reversible contraception. Twelve years of experience with the TCu380A and TCu220C". Contraception 56 (6): 341–52. PMID 9494767.
- ^ a b "What are the most widely used contraceptive methods across the world?". Births / Birth control. Institut national d'études démographiques (INED). 2006. http://www.ined.fr/en/everything_about_population/faq/naissances_natalite/bdd/q_text/what_are_the_most_widely_used_contraceptive_methods_across_the_world_/question/80/. Retrieved 2006-11-16.
- ^ a b c World Health Organization (2002). "The intrauterine device (IUD)-worth singing about". Progress in Reproductive Health Research (60): 1–8. http://www.who.int/reproductive-health/hrp/progress/60/news60.html.
- ^ "A History of Birth Control Methods". Planned Parenthood. June 2002. Archived from the original on 2008-05-17. http://web.archive.org/web/20080517045452/http://www.plannedparenthood.org/resources/research-papers/bc-history-6547.htm. Retrieved 2007-10-14., which cites:
- Thomas, Patricia (1988-03-14). "Contraceptives". Medical World News 29 (5): 48.
- Bullough, Vern L.; Bullough, Bonnie (1990). Contraception: A Guide to Birth Control Methods. Buffalo, NY: Prometheus Books.
- ^ a b c Lynch, Catherine M.. "History of the IUD". Contraception Online. Baylor College of Medicine. Archived from the original on 2006-01-27. http://web.archive.org/web/20060127085615/http://www.contraceptiononline.org/meetings/IUD/lynch/presentation_text.cfm?cme_activityid=47&showmenu=1. Retrieved 2006-07-09.
- ^ a b c "Evolution and Revolution: The Past, Present, and Future of Contraception". Contraception Online (Baylor College of Medicine) 10 (6). February 2000. http://www.contraceptiononline.org/contrareport/article01.cfm?art=93.
- ^ Bradley, Jeff (August 1998). "Ultrasound Interactive Case Study: Ring IUD". OBGYN.net. http://www.obgyn.net/us/us.asp?page=/us/present/9808/bradley. Retrieved 2006-07-09. (Has pictures of various IUD designs.)
- ^ Kaufman, J. (1993 May-Jun). "The cost of IUD failure in China". Studies in Family Planning 24 (3): 194–6. doi:10.2307/2939234. JSTOR 2939234. PMID 8351700.
- ^ a b IUDs-An Update. Chapter 2.3: Effectiveness.
- ^ Van Kets, H.E.; Editors C. Coll Capdevila, L. Iglesias Cortit and G. Creatsas (1997). "Importance of intrauterine contraception". Contraception Today, Proceedings of the 4th Congress of the European Society of Contraception. The Parthenon Publishing Group. pp. 112–116. http://www.contrel.be/IUD%20GENERAL/Mhistory.htm. Retrieved 2006-07-09. (Has pictures of many IUD designs, both historic and modern.)
- ^ a b c IUDs—An Update. Chapter 1: Background.
- ^ Sivin I (1993). "Another look at the Dalkon Shield: meta-analysis underscores its problems". Contraception 48 (1): 1–12. doi:10.1016/0010-7824(93)90060-K. PMID 8403900.
- ^ Mintz, Morton (January 15, 1986). "A Crime Against Women. A. H. Robins and the Dalkon Shield". Multinational Monitor 7 (1). http://multinationalmonitor.org/hyper/issues/1986/0115/index.html.
- ^ Salem R (February 2006). "New Attention to the IUD: Expanding Women’s Contraceptive Options To Meet Their Needs". Popul Rep B (7). http://www.infoforhealth.org/pr/b7/chap1.shtml#outdated.
- ^ "Mechanisms of the Contraceptive Action of Hormonal Methods and Intrauterine Devices (IUDs)". Family Health International. 2006. http://www.fhi.org/en/RH/Pubs/booksReports/methodaction.htm. Retrieved 2006-07-05.
- ^ Keller, Sarah (Winter 1996, Vol. 16, No. 2). "IUDs Block Fertilization". Network. Family Health International. http://www.fhi.org/en/RH/Pubs/Network/v16_2/nt1623.htm. Retrieved 2006-07-05.
- ^ a b Grimes, David (2007). "Intrauterine Devices (IUDs)". In Hatcher, Robert A., et al.. Contraceptive Technology (19th rev. ed.). New York: Ardent Media. pp. 120. ISBN 0-9664902-0-7.
- ^ Stanford J, Mikolajczyk R (2002). "Mechanisms of action of intrauterine devices: update and estimation of postfertilization effects". Am J Obstet Gynecol 187 (6): 1699–708. doi:10.1067/mob.2002.128091. PMID 12501086., which cites:
- Smart Y, Fraser I, Clancy R, Roberts T, Cripps A (1982). "Early pregnancy factor as a monitor for fertilization in women wearing intrauterine devices". Fertil Steril 37 (2): 201–4. PMID 6174375.
- ^ Trussell, James; Elizabeth G. Raymond (April 2008) (PDF). Emergency Contraception: A Last Chance to Prevent Unintended Pregnancy. The Office of Population Research at Princeton University and the Association of Reproductive Health Professionals. http://ec.princeton.edu/questions/ec-review.pdf. Retrieved 2008-05--08.
- ^ a b Gottardi G, Spreafico A, de Orchi L (1986). "The postcoital IUD as an effective continuing contraceptive method.". Contraception 34 (6): 549–58. doi:10.1016/S0010-7824(86)80011-7. PMID 3549140.
- ^ O'Brien, PA; Marfleet C (January 25, 2005). "Frameless versus classical intrauterine device for contraception". Cochrane Database of Systematic Reviews (1). doi:10.1002/14651858.CD003282. PMID 11687184.
- ^ a b c d e Birth Control Intrauterine Devices (IUDs) Author: Omnia M Samra. Last Editorial Review: 5/18/2006
- ^ about.com > What To Expect During an IUD Insertion (ParaGard IUD or Mirena IUD) By Dawn Stacey M.Ed. Updated April 30, 2010
- ^ WHO (2004). "Intrauterine devices (IUDs)". Medical Eligibility Criteria for Contraceptive Use (3rd ed.). Geneva: Reproductive Health and Research, WHO. ISBN 92-4-156266-8. http://www.who.int/reproductive-health/publications/mec/iuds.html.
- ^ FFPRHC (2006). "The UK Medical Eligibility Criteria for Contraceptive Use (2005/2006)" (PDF). Archived from the original on 2007-06-19. http://web.archive.org/web/20070619230102/http://www.ffprhc.org.uk/admin/uploads/UKMEC200506.pdf. Retrieved 2007-01-11.
- ^ Jouppila P, Niinimäki A, Mikkonen M (1979). "Copper allergy and copper IUD". Contraception 19 (6): 631–7. doi:10.1016/0010-7824(79)90009-X. PMID 487812.
- ^ Frentz G, Teilum D (1980). "Cutaneous eruptions and intrauterine contraceptive copper device". Acta Derm Venereol 60 (1): 69–71. PMID 6153839.
- ^ Wohrl S, Hemmer W, Focke M, Gotz M, Jarisch R (2001). "Copper allergy revisited". J Am Acad Dermatol 45 (6): 863–70. doi:10.1067/mjd.2001.117729. PMID 11712031.
- ^ Forthofer KV (2009). "A clinical review of the intrauterine device as an effective method of contraception". J Obstet Gynecol Neonatal Nurs 38 (6): 693–8. doi:10.1111/j.1552-6909.2009.01067.x. PMID 19930283.
- ^ IUDs-An Update. Chapter 3: Insertion.
- ^ control methods/pub-contraception-iud.xml#1103415754536::8998200633989168060 "Understanding IUDs". Planned Parenthood Federation of America. July 2005. http://www.plannedparenthood.org/pp2/portal/files/portal/medicalinfo/Birth control methods/pub-contraception-iud.xml#1103415754536::8998200633989168060. Retrieved 2006-07-22.
- ^ a b Farley TM, Rosenberg MJ, Rowe PJ, Chen JH, Meirik O (1992). "Intrauterine devices and pelvic inflammatory disease: an international perspective". Lancet 339 (8796): 785–8. doi:10.1016/0140-6736(92)91904-M. PMID 1347812.
Grimes DA (2000). "Intrauterine device and upper-genital-tract infection". Lancet 356 (9234): 1013–9. doi:10.1016/S0140-6736(00)02699-4. PMID 11041414.
Mishell Jr., Daniel R. (2004). "Contraception". In in Strauss III, Jerome F.; Barbieri, Robert L. (eds.). Yen and Jaffe's Reproductive Endocrinology (5th ed.). Philadelphia: Elsevier Saunders. pp. 899–938. ISBN 0-7216-9546-9.
Grimes, David A. (2004). "Intrauterine Devices (IUDs)". In in Hatcher, Robert A.; Trussell, James; Stewart, Felicia H.; Nelson, Anita L.; Cates Jr., Willard; Guest, Felicia; Kowal, Deborah (eds.). Contraceptive Technology (18th rev. ed.). New York: Ardent Media. pp. 495–530. ISBN 0-9664902-5-8.
Speroff, Leon; Darney, Philip D. (2005). "Intauterine Contraception: The IUD". A Clinical Guide for Contraception (4th ed.). Philadelphia: Lippincott Williams & Wilkins. pp. 221–257. ISBN 0-7817-6488-2.
Hall, Janet E. (2005). "Infertility and Fertility Control". In in Kasper Dennis L.; Braunwald, Eugene; Fauci, Anthony S.; Hauser, Stephen L.; Longo, Dan L.; Jameson, J. Larry (eds.). Harrison's Principles of Internal Medicine (16th ed.). New York: McGraw-Hill. pp. 279–83. ISBN 0-07-139140-1.
Soper, David E.; Mead, Philip B. (2005). "Infections of the Female Pelvis". In in Mandell, Gerald L.; Bennett, John E.; Dolin, Raphael (eds.). Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases (6th ed.). Philadelphia: Elsevier Chuchill Livingston. pp. 1372–81. ISBN 0-443-06643-4.
Glasier, Anna (2006). "Contraception". In in DeGroot, Leslie J.; Jameson, J. Larry (eds.). Endocrinology (5th ed.). Philadelphia: Elsevier Saunders. pp. 2993–3003. ISBN 0-7216-0376-9.Stubblefield, Phillip G.; Carr-Ellis, Sacheen; Kapp, Nathalie (2007). "Family Planning". In in Berek, Jonathan A. (ed.). Berek & Novak's Gynecology (14th ed.). Philadelphia: Lippincott Williams & Wilkins. pp. 247–311. ISBN 0-7817-6805-5. - ^ a b maqweb.org > Infection Prevention Practices for IUD Insertion and Removal By the United States Agency for International Development (USAID). Retrieved on Feb 14, 2010
- ^ IUDs—An Update. Sidebar: Infection Prevention for IUD Insertion and Removal.
- ^ IUDs—An Update. Sidebar: Procedures for Providing IUDs.
- ^ a b Hutten-Czapski P, Goertzen J (2008). "The occasional intrauterine contraceptive device insertion". Can J Rural Med 13 (1): 31–5. PMID 18208650. http://www.cma.ca/multimedia/staticContent/HTML/N0/l2/cjrm/vol-13/issue-1/pdf/pg31.pdf.
- ^ About.com > What To Expect During an IUD Insertion (ParaGard IUD or Mirena IUD) By Dawn Stacey M.Ed. Updated December 22, 2009
- ^ IUDs-An Update. Chapter 2.5: Bleeding and Pain.
- ^ IUDs-An Update. Chapter 2.9:Ectopic Pregnancies.
- ^ IUDs-An Update. Chapter 2.8: Intrauterine Pregnancy.
- ^ Can I use the copper IUD while nursing?
- ^ IUDs—An Update. Worldwide Use - Developed Countries. Table 2: Worldwide Use of IUDs.
- ^ "Reducing unintended pregnancy in the United States". Contraception. January 2008. http://www.arhp.org/editorials/january2008.cfm.
- ^ a b Chandra, A; Martinez GM, Mosher WD, Abma JC, Jones J. (2005). "Fertility, Family Planning, and Reproductive Health of U.S. Women: Data From the 2002 National Survey of Family Growth" (PDF). Vital Health Stat (National Center for Health Statistics) 23 (25). http://www.cdc.gov/nchs/data/series/sr_23/sr23_025.pdf. Retrieved 2007-05-20. See Table 56.
- ^ "Contraceptive coils (IUDs)". NetDoctor.co.uk. 2006. http://www.netdoctor.co.uk/sex_relationships/facts/contraceptivecoil.htm. Retrieved 2006-07-05.
- ^ Mona Lisa N.V., a manufacturer of generic IUDs
- Long-acting reversible contraception: the effective and appropriate use of long-acting reversible contraception, by the National Collaborating Centre for Women’s and Children’s Health, commissioned by the National Institute for Health and Clinical Excellence, October 2005
External links
- Association of Reproductive Health Professionals' Clinical Proceedings: New Developments in Intrauterine Contraception
- Population Reports: New Attention to the IUD—Johns Hopkins INFO Project, 2006
- IUD Toolkit—USAID's Maximizing Access & Quality Project
- Family Planning: A Global Handbook for Providers - CHAPTER 9 Copper-Bearing Intrauterine Device
- An IntraUterine Device (IUD) Insertion Video
Birth control methods (G02B, G03A) Comparison Behavioral Avoiding vaginal intercourse: Abstinence • Anal sex • Masturbation • Non-penetrative sex • Oral sex
Including vaginal intercourse: Breastfeeding infertility (LAM) • Calendar-based methods (rhythm, etc.) • Fertility awareness • WithdrawalBarrier or
spermicidalHormonal
(formulations)Progestogen-onlyAnti-estrogen Ormeloxifene (Centchroman)Post-intercourse Emergency contraception (pills or copper IUD) (Yuzpe regimen, Ulipristal acetate)Intrauterine device IUD with copper (Paragard) • IUD with progestogen (Mirena)Abortion Sterilization Categories:- Intrauterine contraception
Wikimedia Foundation. 2010.