- Mitochondrial disease
-
Mitochondrial disease Classification and external resources 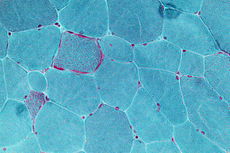
Micrograph showing ragged red fibres, a finding seen in mitochondrial diseases. Muscle biopsy. Gomori trichrome stain.ICD-9 277.87 DiseasesDB 28840 MeSH D028361 Mitochondrial diseases are a group of disorders caused by dysfunctional mitochondria, the organelles that are the "powerhouses" of the cell. Mitochondria are found in every cell of the human body except red blood cells. Mitochondria convert the energy of food molecules into the ATP that powers most cell functions.
Mitochondrial diseases are often caused by genetics or mutations to the mitochondrial DNA that affect mitochondria function. Mitochondrial diseases take on unique characteristics both because of the way the diseases are often inherited and because mitochondria are so critical to cell function. The subclass of these diseases that have neuromuscular disease symptoms are often called a mitochondrial myopathy.
There is some evidence for mitochondrial dysfunction as the molecular basis of bipolar disorder. In addition, classical mitochondrial diseases occur in a subset of individuals with autism and are usually caused by genetic anomalies or mitochondrial respiratory pathway deficits.
Contents
Classification
In addition to the mitochondrial myopathies, other examples include:
- Diabetes mellitus and deafness (DAD)
- this combination at an early age can be due to mitochondrial disease
- Diabetes mellitus and deafness can also be found together for other reasons
- Leber's hereditary optic neuropathy (LHON)
- visual loss beginning in young adulthood
- eye disorder characterized by progressive loss of central vision due to degeneration of the optic nerves and retina
- Wolff-Parkinson-White syndrome
- multiple sclerosis-type disease
- affects 1 in 50,000 people in Finland
- Leigh syndrome, subacute sclerosing encephalopathy
- after normal development the disease usually begins late in the first year of life, although onset may occur in adulthood
- a rapid decline in function occurs and is marked by seizures, altered states of consciousness, dementia, ventilatory failure
- Neuropathy, ataxia, retinitis pigmentosa, and ptosis (NARP)
- progressive symptoms as described in the acronym
- dementia
- Myoneurogenic gastrointestinal encephalopathy (MNGIE)
- gastrointestinal pseudo-obstruction
- neuropathy
- Myoclonic Epilepsy with Ragged Red Fibers (MERRF)
- progressive myoclonic epilepsy
- "Ragged Red Fibers" – clumps of diseased mitochondria accumulate in the subsarcolemmal region of the muscle fiber and appear as "Ragged Red Fibers" when muscle is stained with modified Gömöri trichrome stain
- short stature
- hearing loss
- lactic acidosis
- exercise intolerance
- Mitochondrial myopathy, encephalomyopathy, lactic acidosis, stroke-like symptoms (MELAS)
- mtDNA depletion
- mitochondrial neurogastrointestinal encephalomyopathy (MNGIE)
Nota bene: Conditions such as Friedreich's ataxia can affect the mitochondria, but are not associated with mitochondrial proteins.
Symptoms
Symptoms include poor growth, loss of muscle coordination, muscle weakness, visual problems, hearing problems, learning disabilities, heart disease, liver disease, kidney disease, gastrointestinal disorders, respiratory disorders, neurological problems, autonomic dysfunction, and dementia.
Characteristics
The effects of mitochondrial disease can be quite varied. Since the distribution of the defective mitochondrial DNA may vary from organ to organ within the body, and each mutation is modulated by other genome variants, the mutation that in one individual may cause liver disease might in another person cause a brain disorder. The severity of the specific defect may also be great or small. Some minor defects cause only "exercise intolerance", with no serious illness or disability. Defects often affect the operation of the mitochondria and multiple tissues more severely, leading to multi-system diseases.
Mitochondrial diseases as a rule are worse when the defective mitochondria are present in the muscles, cerebrum, or nerves,[1] because these cells use more energy than most other cells in the body.
Although mitochondrial diseases vary greatly in presentation from person to person, several major clinical categories of these conditions have been defined, based on the most common phenotypic features, symptoms, and signs associated with the particular mutations that tend to cause them.
An outstanding question and area of research is whether ATP depletion or reactive oxygen species are in fact responsible for the observed phenotypic consequences.
Causes
Mitochondrial disorders may be caused by mutations, acquired or inherited, in mitochondrial DNA (mtDNA) or in nuclear genes that code for mitochondrial components. They may also be the result of acquired mitochondrial dysfunction due to adverse effects of drugs, infections, or other environmental causes (see MeSH).
Mitochondrial DNA inheritance behaves differently from autosomal and sexually-linked inheritance. Nuclear DNA has two copies per cell (except for sperm and egg cells), one copy being inherited from the father and the other from the mother. Mitochondrial DNA, however, is strictly inherited from the mother and each mitochondrial organelle typically contains multiple mtDNA copies (see Heteroplasmy). During cell division the mitochondrial DNA copies segregate randomly between the two new mitochondria, and then those new mitochondria make more copies. If only a few of the mtDNA copies inherited from the mother are defective, mitochondrial division may cause most of the defective copies to end up in just one of the new mitochondria (for more detailed inheritance patterns, see Human mitochondrial genetics). Mitochondrial disease may become clinically apparent once the number of affected mitochondria reaches a certain level; this phenomenon is called "threshold expression".
Mitochondrial DNA mutations occur frequently, due to the lack of the error checking capability that mitochondrial DNA has (see Mutation rate). This means that mitochondrial DNA disorders may occur spontaneously and relatively often. Defects in enzymes that control mitochondrial DNA replication (all of which are encoded for by genes in the nuclear DNA) may also cause mitochondrial DNA mutations.
Most mitochondrial function and biogenesis is controlled by nuclear DNA. Human mitochondrial DNA encodes only 13 proteins of the respiratory chain, while most of the estimated 1,500 proteins and components targeted to mitochondria are nuclear-encoded. Defects in nuclear-encoded mitochondrial genes are associated with hundreds of clinical disease phenotypes including anemia, dementia, hypertension, lymphoma, retinopathy, seizures, and neurodevelopmental disorders.[2]
Treatment
Although research is ongoing, treatment options are currently limited; vitamins are frequently prescribed, though the evidence for their effectiveness is limited.[3] Membrane penetrating antioxidants have the most important role in improving mitochondrial dysfunction. Pyruvate has been proposed recently as a treatment option.[4]
Spindle transfer, where the nuclear DNA is transferred to another healthy egg cell leaving the defective mitochondrial DNA behind, is a potential treatment procedure that has been successfully carried out on monkeys.[5] [6] Using a similar pronuclear transfer technique, researchers at Newcastle University successfully transplanted healthy DNA in human eggs from women with mitochondrial disease into the eggs of women donors who were unaffected.[7] [8] Human genetic engineering is already being used on a small scale to allow infertile women with genetic defects in their mitochondria to have children.[9]
Embryonic mitochondrial transplant and protofection have been proposed as a possible treatment for inherited mitochondrial disease, and allotopic expression of mitochondrial proteins as a radical treatment for mtDNA mutation load.
Statistics
About 1 in 4,000 children in the United States will develop mitochondrial disease by the age of 10 years. Up to 4,000 children per year in the US are born with a type of mitochondrial disease.[citation needed] Because mitochondrial disorders contain many variations and subsets, some particular mitochondrial disorders are very rare.
Many diseases of aging are caused by defects in mitochondrial function. Since the mitochondria are responsible for processing oxygen and converting substances from the foods we eat into energy for essential cellular functions, if there are problems with the mitochondria, it can lead to many defects for adults. These include Type 2 diabetes, Parkinson's disease, atherosclerotic heart disease, stroke, Alzheimer's disease, and cancer. Many medicines can also injure the mitochondria.[citation needed]
"Inside the Cell" in Dr. Neal Barnard's Program for Reversing Diabetes, Rodale Press, 2007, pp. 22 – 27, which references the Feb 12, 2004 issue of the New England Journal of Medicine, an article by Yale University researchers. Dr. Barnard also references other studies in his explanation of how, in Type 2 diabetes, the mitochondria signaling process is interrupted by fats in body cells (intramyocellular lipids) which have not been properly treated. A study at Pennington Biomedical Research Cernter in Baton Brouge, LA (Diabetes 54, 2005 1926-33) showed that this in turn partially disables the genes that produce mitochondria.
People
Notable people who suffered from mitochondrial disease include:
- Rocco Baldelli (diagnosis later replaced by channelopathy)
- Mattie Stepanek (dysautonomic mitochondrial myopathy)
- Colby Wren
References
- ^ Finsterer J (2007). "Hematological manifestations of primary mitochondrial disorders". Acta Haematol. 118 (2): 88–98. doi:10.1159/000105676. PMID 17637511.
- ^ Scharfe C, Lu HH, Neuenburg JK, Allen EA, Li GC, Klopstock T, Cowan TM, Enns GM, Davis RW (2009). Rzhetsky, Andrey. ed. "Mapping gene associations in human mitochondria using clinical disease phenotypes". PLoS Comput Biol 5 (4): e1000374. doi:10.1371/journal.pcbi.1000374. PMC 2668170. PMID 19390613. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=2668170.
- ^ Marriage B, Clandinin MT, Glerum DM (2003). "Nutritional cofactor treatment in mitochondrial disorders". J Am Diet Assoc 103 (8): 1029–38. doi:10.1053/jada.2003.50196. PMID 12891154.
- ^ Tanaka M, Nishigaki Y, Fuku N, Ibi T, Sahashi K, Koga Y (2007). "Therapeutic potential of pyruvate therapy for mitochondrial diseases". Mitochondrion 7 (6): 399–401. doi:10.1016/j.mito.2007.07.002. PMID 17881297.
- ^ Genetic advance raises IVF hopes By Pallab Ghosh. BBC News, science correspondent. Page last updated at 17:04 GMT, Wednesday, 26 August 2009 18:04 UK
- ^ Tachibana M, Sparman M, Sritanaudomchai H, Ma H, Clepper L, Woodward J, Li Y, Ramsey C, Kolotushkina O, Mitalipov S (September 2009). "Mitochondrial gene replacement in primate offspring and embryonic stem cells". Nature 461 (7262): 367–372. doi:10.1038/nature08368. PMC 2774772. PMID 19710649. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=2774772.
- ^ Boseley, Sarah (2010-04-14). "Scientists reveal gene-swapping technique to thwart inherited diseases". Guardian. http://www.guardian.co.uk/science/2010/apr/14/scientists-gene-swap-technique-disease.
- ^ Craven L, Tuppen HA, Greggains GD, Harbottle SJ, Murphy JL, Cree LM, Murdoch AP, Chinnery PF, Taylor RW, Lightowlers RN, Herbert M, Turnbull DM (May 2010). "Pronuclear transfer in human embryos to prevent transmission of mitochondrial DNA disease". Nature 465 (7294): 82–85. doi:10.1038/nature08958. PMC 2875160. PMID 20393463. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=2875160.
- ^ "Genetically altered babies born". BBC News. 2001-05-04. http://news.bbc.co.uk/1/hi/sci/tech/1312708.stm. Retrieved 2008-04-26.
External links
- Mitochondrial disease at the Open Directory Project
- Seahorse Bioscience
- United Mitochondrial Disease Foundation
Non-Mendelian inheritance: Mitochondrial diseases (277.87) Carbohydrate metabolism Primarily nervous system Myopathies No primary system Chromosomal Categories:- Mitochondrial diseases
- Diabetes mellitus and deafness (DAD)
Wikimedia Foundation. 2010.
