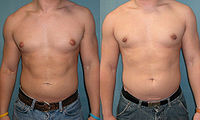
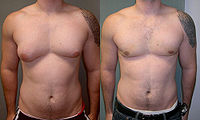
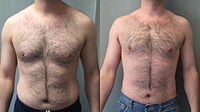
- Gynecomastia
-
Gynecomastia Classification and external resources 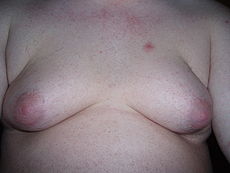
Male with severe gynecomastia and pseudogynecomastiaICD-10 N62 ICD-9 611.1 MedlinePlus 003165 Gynecomastia or Gynaecomastia, pronounced /ˌɡaɪnɨkɵˈmæstiə/, is the abnormal development of large mammary glands in males resulting in breast enlargement. The term comes from the Greek γυνή gyné (stem gynaik-) meaning "woman" and μαστός mastós meaning "breast". The condition can occur physiologically in neonates (due to female hormones from the mother), in adolescence, and in the elderly (Both in adolescence and elderly it is an abnormal condition associated with disease or metabolic disorders). In adolescent boys the condition is often a source of distress, but for the large majority of boys whose pubescent gynecomastia is not due to obesity, the breast development shrinks or disappears within a couple of years.[1]
The causes of common gynecomastia remain uncertain, although it has generally been attributed to an imbalance of sex hormones or the tissue responsiveness to them; a root cause is rarely determined for individual cases. The condition may also be caused by an imbalance of estrogenic and androgenic effects on the breast, resulting in an increased or unopposed estrogen action on breast tissue. Approximately 4 to 10% cases of gynecomastia are due to drugs. Spironolactone (Aldactone) is a common cause, inducing gynecomastia in 10% of those receiving it as a treatment for heart failure.[2][3] Both Digoxin and Furosemide are also reported to cause the same condition. Although, chances of gynecomastia could be more if these two drugs are coadministered.[4] Breast prominence can result from hypertrophy of breast tissue, chest adipose tissue (fat) and skin, and is typically a combination. Breast prominence due solely to excessive adipose is often termed pseudogynecomastia[5] or sometimes lipomastia.[6]
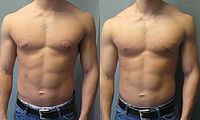
Gynecomastia should be distinguished from muscle hypertrophy of the pectoralis muscles caused by exercise (e.g., swimming, bench press, etc.).
Contents
Classification
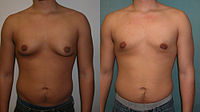
"Puffy nipples" is among the most common forms of gynecomastia. This glandular tissue accumulation is concentrated under and typically confined to the areola, or can be slightly extended outside the areola forming a dome shaped appearance to the areola.
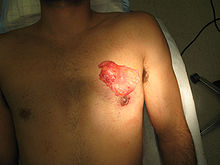
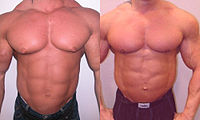
Pure glandular gynecomastia is common in bodybuilders and is thought to be a result of the use of anabolic steroids.[7] In this case it is known as anabolic-androgenic steroid (AAS) induced gynecomastia.[7] Due to excess testosterone levels from steroids, which is converted to estrogen, bodybuilders and other athletes are sometimes afflicted with gynecomastia in its purest form. Gynecomastia in lean men is usually only a breast tissue gland with little to no adipose tissue. Proper treatment of pure gynecomastia can be done only by excision of the breast tissue, which in the case of bodybuilders is by itself sufficient to achieve a flat nipple-areola complex. Liposuction is only rarely necessary.
Congenital or hereditary gynecomastia is typically evident by the ages of 12 to 18 in boys.[8] Thirty percent to sixty percent of young boys suffer from large male breasts.[8] As many as thirty percent may live with enlarged male breasts for the rest of their lives, but in other cases the gynecomastia will recede with age. However, severe forms of adolescent gynecomastia may require an intervention, in consultation with the patient, the parents, and child development professionals.
Related conditions
Pseudogynecomastia[5] is typical of enlarged diameter and or excessive areola projection. However, it is not composed of glandular tissue, but of adipose tissue. It looks much like typical gynecomastia but requires different treatment. Exercise and diet may be effective in combating pseudogynecomastia. Only if this regimen is unsuccessful should surgery be considered. This is generally the only type of gynecomastia which can be improved with liposuction, but excision may be indicated in some cases.
Unilateral / asymmetrical gynecomastia occurs when only one breast is larger due to gynecomastia, the other breast is typically normal in both size and shape. Bilateral asymmetry occurs when gynecomastia is present in both breasts, each to a different degree.
As older persons suffering from gynecomastia tend to have less skin elasticity and thus will have a greater abundance of excess skin related to gynecomastia.[9]
Health conditions
Several health conditions can cause gynecomastia by affecting hormone levels:
- Hypogonadism
- Any of the conditions that interfere with normal testosterone production, such as Klinefelter syndrome or pituitary insufficiency, can be associated with gynecomastia.
- Aging
- Hormone changes that occur with normal aging can cause gynecomastia, especially in men who are overweight.
- Tumors
- Some tumors, such as those involving the testes, adrenal glands or pituitary gland, can produce hormones that alter the male-female hormone balance.
- Hyperthyroidism
- In this condition, the thyroid gland produces too much of the hormone thyroxine.
- Kidney failure
- About half the people being treated with regular hemodialysis experience gynecomastia due to hormonal changes.
- Liver failure and cirrhosis
- Hormonal fluctuations related to liver problems as well as medications taken for cirrhosis are associated with gynecomastia.
- Malnutrition and starvation
- When the human body is deprived of adequate nutrition, testosterone levels drop, but estrogen levels remain constant, causing a hormonal imbalance. Gynecomastia can also occur once normal nutrition resumes.
Treatment
Treating the underlying cause of the gynecomastia may lead to improvement in the condition. Patients should talk with their doctor about revising any medications, such as risperidone, that are found to be causing gynecomastia. Often, an alternative medication can be found that avoids gynecomastia side-effects while still treating the primary condition (e.g., in place of taking spironolactone the alternative eplerenone can be used). Selective estrogen receptor modulator medications, such as tamoxifen and clomiphene, or androgens (typically testosterone) or aromatase inhibitors such as anastrozole are medical treatment options, although they are not universally approved for the treatment of gynecomastia. Endocrinological attention may help during the first 2–3 years. After that window, however, the breast tissue tends to remain and harden, leaving surgery (either liposuction, gland excision, skin sculpture, reduction mammoplasty, or a combination of these surgical techniques) as the only treatment option. Many American insurance companies deny coverage for surgery for gynecomastia treatment on the grounds that it is a cosmetic procedure. Radiation therapy is sometimes used to prevent gynecomastia in patients with prostate cancer prior to estrogen therapy. Compression garments can camouflage chest deformity and stabilize bouncing tissue bringing emotional relief to some. There are also many who choose to not treat the condition.
Prognosis
Gynecomastia is not physically harmful, but in some cases can be an indicator of other more serious underlying conditions, such as testicular cancer.[10][11][12] Growing glandular tissue, typically from some form of hormonal stimulation, is often tender or painful. Furthermore, it can frequently present social and psychological difficulties for the sufferer.[13] Weight loss can alter the condition in cases where it is triggered by obesity, but losing weight will not reduce the glandular component and patients cannot target areas for weight loss. Massive weight loss can result in sagging tissues about the chest, chest ptosis. The size and geometry of the fibro-glandular tissue present is unique to each patient. This results in a range of physically apparent aesthetic deformities, for which, classification systems have been devised. [14]
Gallery
See also
References
- Notes
- ^ Adolescent gynecomastia
- ^ Pitt, Bertram (1999-09-02). "The Effect of Spironolactone on Morbidity and Mortality in Patients with Severe Heart Failure". N Engl J Med. http://www.nejm.org/doi/full/10.1056/NEJM199909023411001#t=articleResults. Retrieved 2011-08-01.
- ^ Haynes, Bridgett; Mookadam, F (2009-08-01). "Male Gynecomastia". Mayo Clinic proceedings. Mayo Clinic (Mayo Clin Proc.) 84 (8): 672. doi:10.4065/84.8.672. PMC 2719518. PMID 19648382. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=2719518.
- ^ Aiman, Umme; Haseeen, MA; Rahman, SZ (Dec 2009). "Gynecomastia: An ADR due to drug interaction". Indian J Pharmacol. 41 (6): 286–7. doi:10.4103/0253-7613.59929. PMC 2846505. PMID 20407562. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=2846505.
- ^ a b Braunstein, Glenn D.; Braunstein, Glenn D. (Feb 18 1993). "Gynecomastia". New England Journal of Medicine 328 (7): 490–5. doi:10.1056/NEJM199302183280708. PMID 8421478.
- ^ Allee, Mark R (2006-11-15). "Gynecomastia". WebMD, Inc. (emedicine.com). http://www.emedicine.com/med/topic934.htm. Retrieved 2007-05-20.
- ^ a b Llewellyn, W (2009). William Llewellyn's Anabolics. pp. 43–44.
- ^ a b Bembo, SA; Carlson, HE (June 2004). "Gynecomastia: Its features, and when and how to treat it". Cleveland Clinic Journal of Medicine 71 (6): 511–517. doi:10.3949/ccjm.71.6.511. PMID 15242307.
- ^ Gerhardt, LC; Lenz, A; Spencer, ND; Münzer, T; Derler, S (Aug 2009). "Skin-textile friction and skin elasticity in young and aged persons". Skin Res Technol 15 (3): 288–98. doi:10.1111/j.1600-0846.2009.00363.x. PMID 19624425.
- ^ http://www.labtestsonline.org/understanding/conditions/testicular.html
- ^ http://emedicine.medscape.com/article/120858-overview
- ^ http://www.medhelp.org/posts/Urology/Gynecomastia-and-cancer-of-the-testies/show/912913
- ^ Wiesman IM, Lehman JA, Parker MG, Tantri MD, Wagner DS, Pedersen JC (August 2004). "Gynecomastia: an outcome analysis". Ann Plast Surg 53 (2): 97–101. PMID 15269574. http://meta.wkhealth.com/pt/pt-core/template-journal/lwwgateway/media/landingpage.htm?issn=0148-7043&volume=53&issue=2&spage=97.
- ^ Simon BE, Hoffman S, Kahn S. Classification and surgical correction of gynecomastia. Plast Reconstr Surg 1973;51:48-52.
External links
- What is gynecomastia? Children's Hospital Boston
- Excessive alcohol consumption can lead to male breasts Fitho- Health & Fitness Resource
Disorders of breast (N60–N64, 610–611) Mastitis Puerperal mastitis (Breast engorgement) · Nonpuerperal mastitis (Subareolar abscess/Zuska's disease, Granulomatous mastitis)Other Benign mammary dysplasia (Duct ectasia of breast · Chronic cystic mastitis) · Galactorrhea · Mastodynia · nipple (Nipple discharge, Inverted nipple, Fissure of the nipple) · Galactocele · Ptosis · Breast cyst · Breast lump · Fat necrosis of breast · Gynecomastia · Hypertrophy of breastCategories:- Andrology
- Medical conditions related to obesity
- Breast diseases
Wikimedia Foundation. 2010.